The Signs And Symptoms of Eating Disorders
With the current hysteria over the "Obesity Epidemic" sweeping Western industrialized countries, one gets the impression that the only health problems eating create stem from overweight. But the mirror has two faces. There is another world, sensationalized by a celebrity-obsessed media, and too often overlooked in our own lives: an existence dominated by life-threatening eating disorders.
As many as ten million women and one million men are fighting a life-and-death battle with anorexia or bulimia every day. One out of every four anorexics will die of complications from her disease. Yet, the amount of misinformation about eating disorders continues to grow with their prevalence. Eating disorders can be prevented and treated. The signs and symptoms are easy to recognize; it's just a matter of knowing where to look.
What is Anorexia?
Anorexia is probably the easiest eating disorder to identify. It has a clear definition in the Diagnostic and Statistical Manual of Mental Disorders (DSM). To be diagnosed, a person must exhibit all of the following symptoms:
- Refusal to maintain body weight at or above a minimally normal weight for age and height (e.g., weight loss leading to maintenance of body weight less than 85% of that expected; or failure to make expected weight gain during period of growth, leading to body weight less than 85% of that expected).
- Intense fear of gaining weight or becoming fat.
- Disturbance in the way in which one's body weight or shape is experienced, undue influence of body weight or shape on self-evaluation, or denial of the seriousness of the current low body weight.
- In postmenarcheal, premenopausal females (women who have had their first menstrual period but have not yet gone through menopause), amennorhea(the absence of at least three consecutive menstrual cycles).
However, it is little known that there are actually two types of the disease. The Restricting Type is what one commonly associates with the word "anorexic:" the person who simply eats very little, or only certain "safe" foods, or engages in periods of fasting. The second kind of anorexic is the Binge-Eating or Purging Type, who regularly binge-eats and/or compensates for intake by over-exercising, vomitting, or laxative abuse.
Signs and Symptoms of Anorexia
If you suspect someone you know suffers from anorexia, here are a few things to look for.
Behavioral Signs:
- Sensitivity to comments about weight or appearance
- Frequent excuses for not eating, such as a large meal earlier or lack of hunger
- Obsessive talk about diet, exercise, and food
- Possible self-harm, suicide attempts, or substance abuse
Physical Symptoms:
- Rapid or extreme weight loss
- Slow or abnormal heart rate
- Loss of menstrual period
- Constipation
- Thinning hair
- Malnutrition headaches
- Dehydration and mineral deficiency
- Brittle nails and dry skin
- Lowered immunity leading to frequent illness
- Growth of fur-like hair (lanugo) on face and torso
What is Bulimia Nervosa?
Bulimia nervosa is less widely understood, and much harder to identify, than anorexia. Most bulimics are at or even above a healthy weight, and often eat very normally in front of other people, keeping their disordered behaviors successfully hidden from the outside world. One common misconception about bulimia is that anyone who throws up her food merits the diagnosis, but as we saw with the purging-type anorexic, this is not, in fact, the case.
The DSM gives the following diagnostic criteria for bulimia nervosa:
Recurrent episodes of binge eating. An episode of binge eating is characterized by both of the following:
- Eating, in a fixed period of time (e.g., within any two-hour period), an amount of food that is definitely larger than most people would eat during a similar period of time and under similar circumstances.
- A sense of lack of control over eating during the episode (e.g., a feeling that one cannot stop eating or control what or how much one is eating).
- Recurrent inappropriate compensatory behavior in order to prevent weight gain, such as self-induced vomiting; misuse of laxatives, diuretics or other medications; fasting; or excessive exercise.
- The binge eating and inappropriate compensatory behaviors both occur, on average, at least once a week for three months.
- Self-evaluation is unduly influenced by body shape and weight.
- The disturbance does not occur exclusively during episodes of anorexia nervosa.
Once again, we find two main sub-groups under our umbrella diagnosis. The Purging Type involves the use of self-induced vomiting, enemas, laxatives, or ipecac to rapidly rid the body of the calories just consumed. The less-common Non-Purging Type bulimic instead turns to fasting or excessive exercise to compensate for intake over time.
Signs and Symptoms of Bulimia
It can be hard to tell for sure whether or not someone is bulimic, since so many of the disordered behaviors occur in private, but there are several signs that, when seen together, are a fairly good indicator.
Behavioral Signs
- Fluctuations in weight
- Frequent "failed" diet attempts
- Large quantities of missing food
- Consistantly going to the bathroom just after eating
- Compulsive exercise
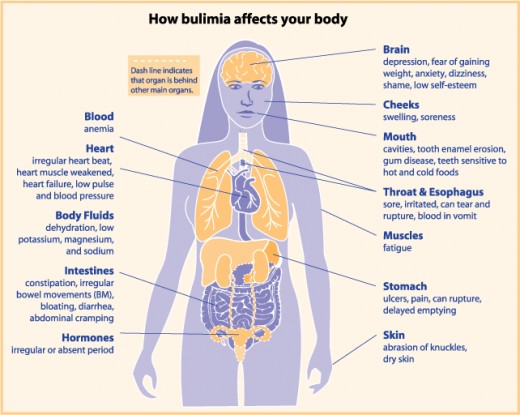
Physical Symptoms
Shown in the chart below:
What to Do Next
So you've gone down the list, with someone in mind, and you're pretty sure your friend or family member (or yourself!) has an eating disorder. What do you do now? Seek help. An eating disorder is a disease, and as a disease, it can be treated. Just as anorexia and bulimia both possess physical and emotional attributes, treatment must be multidisciplinary to address all the aspects of the illness.
The first step is to find resources in your area. The National Eating Disorder Association (http://www.nationaleatingdisorders.org) provides help in locating both psychological and nutritional professionals to aid you or your loved one in regaining health. If inpatient treatment becomes necessary, they also have referrals of the countries top facilities.
Remember: there is no magic potion, no quick fix, for this problem. Just as a diabetic must check blood sugar and take insulin daily, a disordered eater will need to continue to monitor him- or herself, even after he or she no longer meets the diagnosis. Life is a journey, or so it is said. And so is recovery.