Topical Pain Creams As An Alternative to Oral Analgesics
Overview of Topical Medications
There are several different classes of prescription topical medications that are available today. While these types of medications are not generally recommended as part of an initial treatment plan, they can be a valuable treatment option in some cases when oral medications are not tolerated. Typical first line medications would include oral NSAIDs, such as ibuprofen or naproxen, muscle relaxants, such as Baclofen or Flexeril, and opioid medications, such as Oxycodone, Hydrocodone, and Morphine. With the exception of NSAIDs, the other 2 classes of medications have significant risks for dependence, addiction, abuse, and overdose, especially with use beyond 1-2 months. As a result, they are not generally indicated for long term use or for patients with only mild pain.
As discussed in another one of my articles on this topic, concerns for opioid use have been growing over the last 2 decades. At this point, the opioid problem has become somewhat of an epidemic in the US. In an attempt to prevent opioid dependence and addiction, treatment alternatives are necessary. Topical medications could be a good treatment alternative in some cases. However, there are also potential risks with topical creams and their efficacy in treating more severe forms of pain is questionable.
Each class of topical medication has very specific indications for use. I have been seeing chronic pain patients for 13+ years and have become very familiar with these topical medications. The following information in this article is based upon a combination of my own anecdotal evidence of outcomes in the patient population that I see as well as evidence based guidelines/studies.
Topical Administration of Medications
As outlined in the Official Disability Guidelines from the Work Loss Data Institute, "topical pain medications are applied locally to painful areas with advantages that include lack of systemic side effects, absence of drug interactions, and no need to titrate." As noted above, several different classes of medications can be used topically, including (but not limited to):
- Anti-inflammatory medications (NSAIDs);
- Opioids;
- Local anesthetics;
- Cannabinoids;
- Anti-depressants;
- Muscle Relaxants
Topical application of medications does not include transdermal medications, such as the opioid fentanyl, as transdermal medications are formulated to penetrate the skin layers into the tissues with systemic effects. Alternatively, topical medications are indicated for local effects at the site of application only without any intention for systemic exposure.
It is important to note that topical medications in general are considered to be experimental/investigational, as there are very few evidence based studies that prove efficacy. It is common for many of the topical agents to be compounded into one topical cream. However, when any one of the topical agents in the cream is not indicated for the diagnosis, then the entire cream would not be appropriate for use.
Indications for Use
One of the more common conditions that is treated with topical medications would be neuropathic (nerve) pain. However, topical medications are generally not recommended until after oral medications have already been tried and either have failed to provide benefit or caused intolerable side effects. One of the primary benefits with topical application of medication is that it is not absorbed into the blood stream, metabolized by the liver, or excreted by the kidneys, as would be the case with oral medications. As a result, there is less risk for systemic problems, such as liver/kidney damage, gastrointestinal problems, and addiction.
Topical Anesthetics
Local anesthetics, such as lidocaine, bupivicaine, and benzocaine, are used commonly for dental procedures. Lidocaine is also used as a numbing agent for many injections. Local application of lidocaine to the skin or gums results in a loss of sensation, or numbness, which causes the nerves to lose their ability to send pain signals to the brain. When the lidocaine is injected, it can cause numbness in deeper tissues. For example, lidocaine is often used during spinal injections, including epidurals and facet blocks, with the intention of numbing painful sensations coming from pathology.
As I discuss in another one of my articles, pain relief after an injection of local anesthetic into the facet joints in the spine is considered to be diagnostic for facet mediated pain. However, the beneficial effects of the local anesthetic wear off very quickly; typically after several hours or up to 2 days, which prompts the need for treatment that can provide longer lasting benefit, such as an injection of steroids or radiofrequency ablation of the nerves innervating the joint. In this example, it is clear that although a local anesthetic is capable of providing significant relief from pain, it needs to be applied directly to the pain generating lesion in order to be effective and would need to be reapplied frequently when it wears off. This is why topical anesthetics have very specific indications for use.
Topical Lidocaine
As outlined by the Official Disability Guidelines, topical lidocaine is indicated in the treatment of localized, peripheral neuropathy in patients who have failed to respond to oral first line medications, including NSAIDs, tricyclic antidepressants, SNRI antidepressants, and anticonvulsants. Neuropathic conditions that are characterized as being both peripheral and localized would include carpal tunnel syndrome, cubital tunnel syndrome, and complex regional pain syndrome, to name a few. All of these conditions have a lesion that is on a peripheral nerve and is causing localized nerve pain in that region. Because lidocaine needs to be applied directly to the pain generating area, it is only beneficial when the pain comes from a cause that is very close to the skin. In carpal tunnel syndrome, the median nerve is compressed in the wrist just below the skin and dermal layers. As such, the lidocaine is capable of numbing the area.
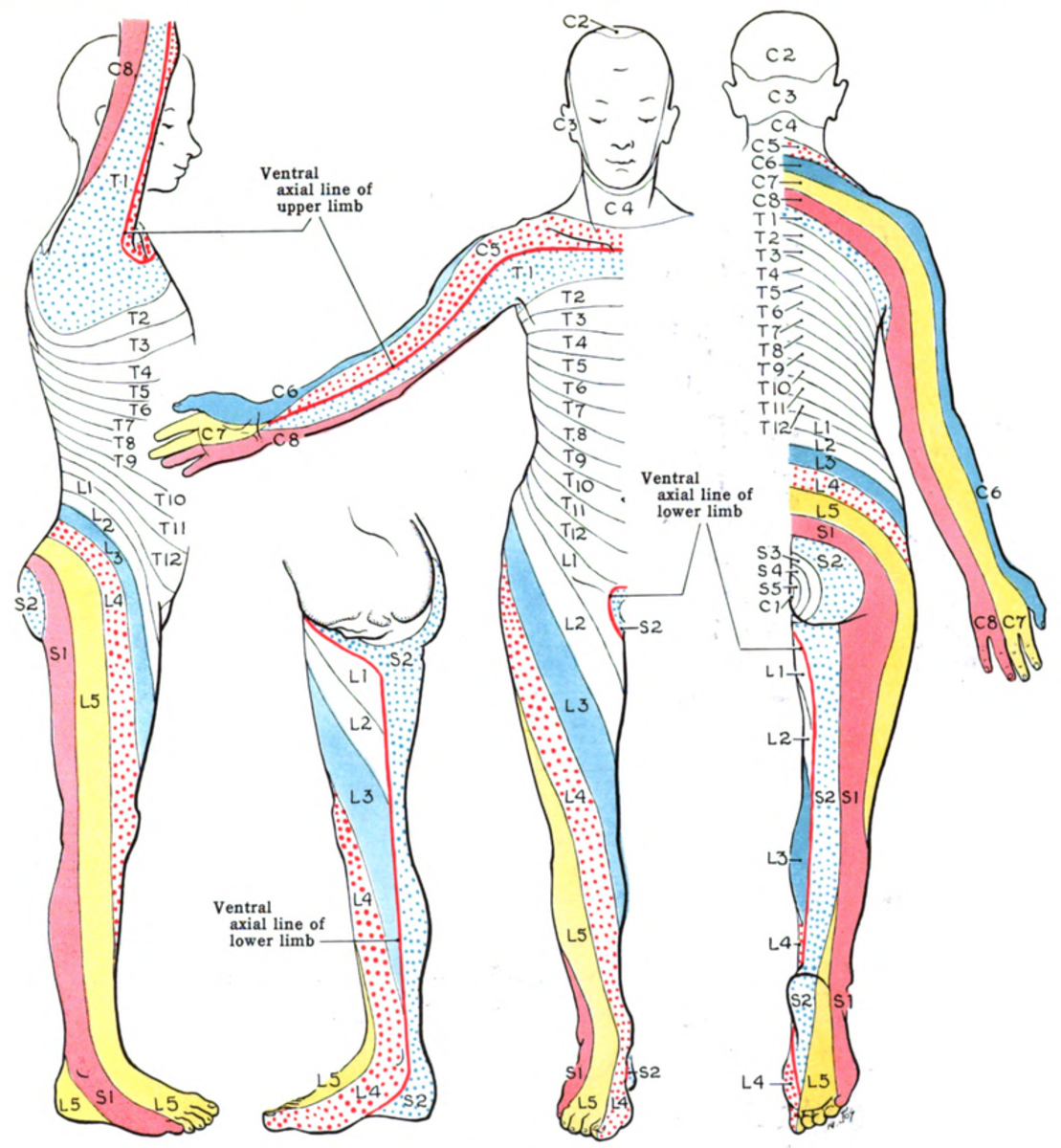
Topical lidocaine is not indicated for neuropathic pain from central lesions because it cannot penetrate deep enough to numb the area. One good example of this is neuropathic pain that is caused by compression of the nerve roots exiting the spinal cord and vertebral column, which is more commonly called radiculopathy, or sciatica. Although the cause of the neuropathy is in the spine, the pain is felt in the extremities in the areas that are innervated by that nerve root. These areas of pain follow a specific pattern dependent upon where the nerve root compression is located. These areas are called dermatomes. You can reference the picture below for a detailed view of the various dermatomes throughout the body. Topical application of lidocaine to the spine would not penetrate deep enough to reach the nerve roots. Additionally topical application of lidocaine to the painful area (or dermatome) on the extremity would be ineffective because the pain is generated in the spine.
According to the Official Disability Guidelines, first line treatment for neuropathic pain would include oral antidepressants and oral anticonvulsants. In most cases of neuropathic pain, symptomatic relief is obtained from a combination of a tricyclic antidepressant, such as nortriptyline, paired with an anticonvulsant, such as gabapentin. However in cases where these medications do not help or cause intolerable side effects, topical lidocaine can be considered as an option.
Lidocaine can be prescribed as a cream, gel, or patch. Lidoderm is the brand name for the topical lidocaine patch, which is generally the preferred mode of application for the medication. The FDA notified the public in 2007 of a potential hazard of the use of topical lidocaine, especially when it is applied to large areas and left on for a long time, as this can lead to systemic exposure and side effects. As such, it is generally not appropriate to use lidocaine in any other formulation than a transdermal patch. With gels and creams, excessive amounts of the medication can be applied over large areas of the body, increasing the risk for serious adverse effects. With the patch, a specific amount and dose is used on a specific area.
Topical Capsaicin
Capsaicin is a topical analgesic medication that can be applied locally to painful areas. Capsaicin is derived from chili peppers. The agent that makes the chili peppers hot is what is derived into this topical analgesic. The intention is that it provides a local hot sensation, which interferes with and disrupts the painful stimuli from the nerves. The application of heat therapy to an injured area can also open up the blood vessels allowing more blood into the area. The increased blood flows brings increased nutrients and increased healing agents, which can accelerate the natural healing of an injury.
As with other topical medications, capsaicin is only recommended if oral medications cannot be tolerated. It is mostly recommended for nerve pain, but there are also studies that have found positive effects in the treatment of arthritis, fibromyalgia and back pain. However, only the 0.0325% formulation of capsaicin has been studied. At this time, doses above 0.0325% are considered to be experimental.
Capsaicin is available over the counter and can be purchased without a prescription. Capsaicin is often combined with Menthol and Methyl Salicylate for added therapeutic benefits. Ultra Strength Ben-Gay is an over the counter topical medication that contains capsaicin, menthol, and methyl salicylate. The Menthol acts as a cooling agent when applied to the skin. Application of ice/cold therapy to an injured area can decrease swelling by blocking the introduction of inflammatory agents in the blood and surrounding soft tissues.
Topical Muscle Relaxants
Muscle relaxants have been used as topical medications and are being researched to evaluate for possible positive effects. Baclofen, a muscle relaxant medication that is commonly prescribed orally to address painful muscle conditions, is currently in a Phase III study at the Institute of Health, in which it is being studied for its possible benefit for chemotherapy related nerve pain. However, it is still experimental at this time and there is currently no research that has proven a positive effect with topical muscle relaxants. No other muscle relaxant medications are proven effective or beneficial for topical use, either. Despite a lack of proven clinical benefit, cyclonenzaprine and carisopridol are prescribed by some physicians to treat patients with chronic musculoskeletal pain. These agents are sometimes compounded with other classes of medications. Some of the more common combinations are cyclobenzaprine with gabapentin; cyclobenzaprine with flurbiprofen; and carisoprodol with capsaicin. None of these combination topical medications containing muscle relaxants have proven clinical efficacy, either. The addition of another class of medication to a topical muscle relaxant does not alter the effects of these medications when used alone.
Topical Non-Steroidal Anti-Inflammatory Medications (NSAIDs)
Topical NSAIDs, such as diclofenac and ketoprofen, are generally indicated in the treatment of osteoarthritis in joints that are amenable to topical treatments, such as in the knee, elbow, wrist, hand, ankle, and foot. However, they are only recommended for short term use of up to 4-12 weeks, as chronic use beyond 12 weeks has not been found to be efficacious. NSAIDs were recently found to be helpful for acute soft tissue injuries, such as sprains and overuse injuries, as determined in an evidence based studied, but they are only recommended for very short term use of 1-2 weeks. However, the oral formulation would be recommended first unless there were contraindications to the oral formulation (such as history of gastric ulcers, liver/kidney damage/failure, cardiovascular disease, etc.).
The intention with topical NSAIDs is to achieve a therapeutic concentration of the medication in the tissues around the location where it was applied. This prevents the systemic exposure to the medication, which can decrease the risks for GI and cardiovascular events. However, at this time, the only FDA approved topical NSAID is diclofenac. Multiple other NSAIDs have not been proven to be similarly efficacious for topical use. Some side effects have been reported with the use of NSAIDs topically, including a rash or itching at the application site. However, these side effects have only been reported in 12% of patients who use topical NSAIDs and the rash/itching resolves once the medication is discontinued. It is also important to note that topical NSAIDs are considerably more expensive (6 to 10 times) that oral formulations. However, it has been theorized that the fact that patients are less likely to have the GI and cardiovascular side effects provides a cost savings long term.
Other Topical Agents
The multiple other different classes of topical medications have limited proven benefit. Agents like gabapentin (anticonvulsants) and antidepressants have not been proven to be efficacious. In fact, there are no peer reviewed, evidence based studies that show any efficacy with their use. Salicylates and menthol have some evidence of benefit from pain, but are only recommended when oral medications are not helpful. As noted above, Menthol is utilized for its cooling properties and is usually combined with methyl salicylate or capsaicin, or both. However, the FDA has released a warning that topical medications that contain menthol and methyl salicylates may cause severe burns.
It is ultimately up to the individual to decide what medications work well. The benefits should always be weighed against any risks in determining the most appropriate medication regimen. Take a look at my other hub about topical medications, which more thoroughly discusses risks associated with their use.
Summary
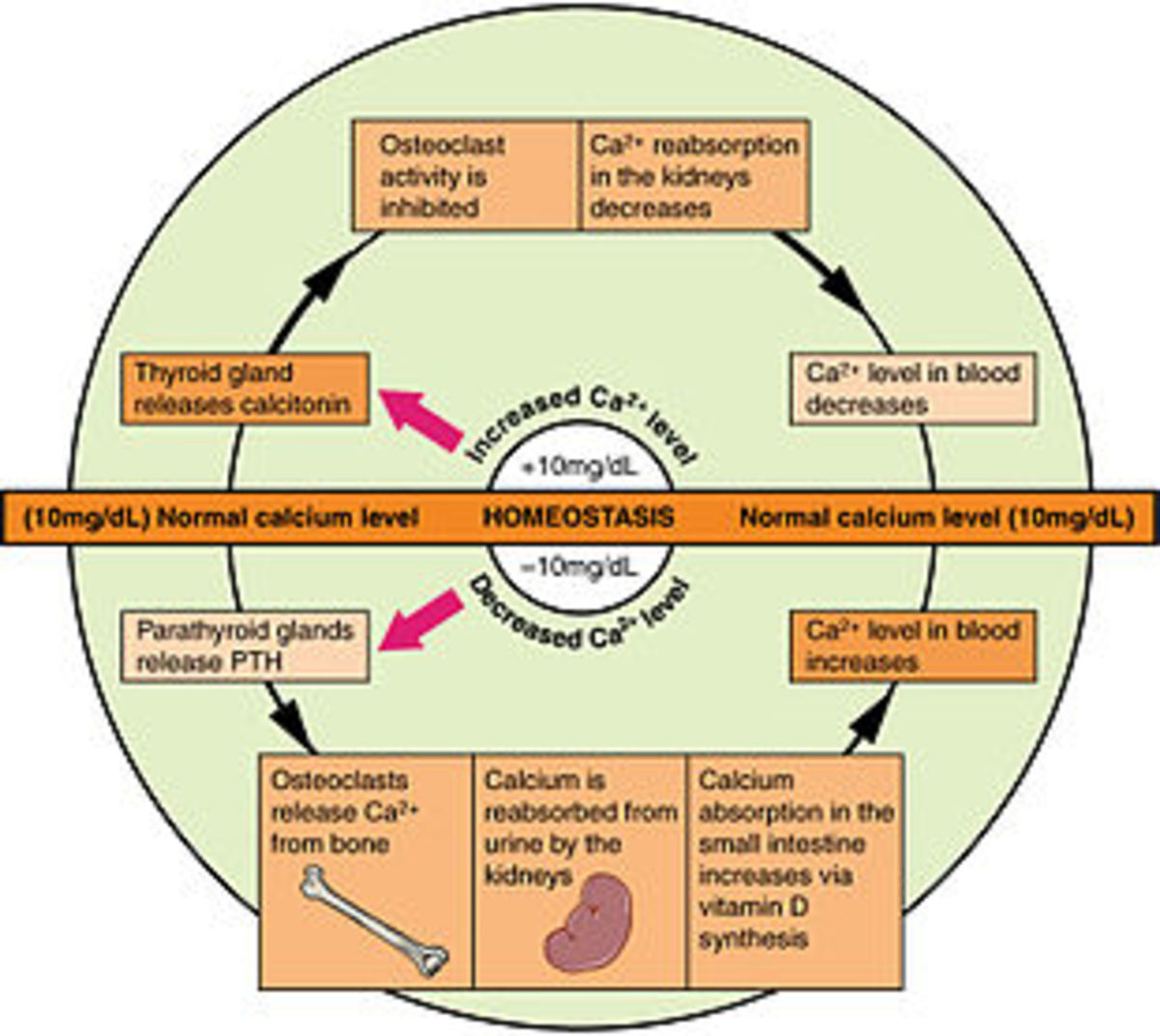
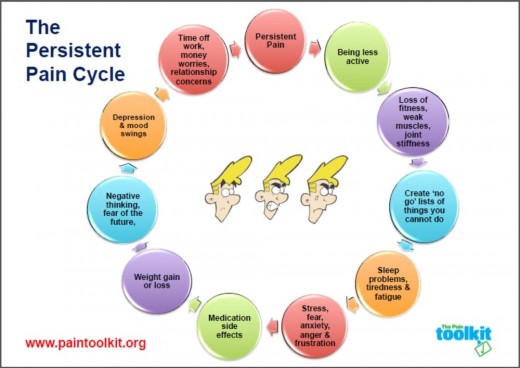
As you can see in the picture below, the chronic pain cycle can lead to multiple problems in many patients, including psychological and physical problems. In an effort to effectively treat patients with chronic pain, research is still ongoing as to what works and what doesn't work.
In general, it appears that topical medications do not offer a very promising alternative to oral medications to treat pain related to arthritis, muscle spasm, nerve problems and injury. However, many physicians who specialize in orthopedics, physical medicine and rehabilitation (PM&R), and pain management commonly use topical medications to supplement oral medications in hopes that they will help to decrease reliance on oral medications. Nonetheless, treatment response is variable, and not proven. Thus, topical agents do not provide a reliable alternative to oral medications in all cases.
If you enjoyed reading this article, comments are encouraged. I always appreciate the opportunity to hear stories from my readers about their own personal struggles and successes. Additionally, if there is any information you are still lacking after reading this article, I am open to suggestions for new articles or for additions to this article. My goal is to provide the most transparency I can to the public with regard to healthcare and I pride myself on providing original content containing information that is not readily available to the general public.
What topical medications have you tried in the past?
© 2012 Kortney T