WENT TO THEATRE AND RETURNED WITH AN ILEOSTOMY
WHAT'S CAUSING MY RECTAL BLEEDING
I was very excited when I joined the RAAF to do my Rookies Course. I was just seventeen years of age and being away from home, I was very nervous and home sick, but I soon settled in. I had been have a bit of nervous tummy, with occasional cramps and diarrhoea, and put it down to being away from home, hoping that it would settle down.
When it started to have blood in it, I got a little worried about it and then it stopped. I had forgotten about it, when it returned again but this time it was a lot more. I saw a medical officer at the Base Hospital, who examined me, and said you have haemorroids. He gave me some cream, and said come back if it is still bothering you. Well, I went away feeling like a bit of a dill making a fuss over haemorroids. The next day, I was in the barracks toilets, when I felt faint and realised I was losing a lot of blood, much more than before. There was no one around to get some help. There were usually lots of girls chatting but today, just when I needed someone to get some help, I was totally alone. I started to walk to the door and then I collapsed on the floor.
MY SURGERY
When I came too, I was in the emergency ward of the General Hospital. I was told that I had haemorrhaged so badly that I had to have a large blood transfusion. I inquired how I had got there was told that one of the airwoman had found me on the floor, and an ambulance had taken me to the RAAF Base Hospital. I was then transferred to the General Hospital. The surgeon came and saw me and said I would need immediate surgery because I had a mass in my abdomen, probably a sigmoid volvulus. This is when a loop of your bowel has twisted round itself and cuts off of the blood supply and there is subsequent dying of the piece of bowel that is not getting enough blood through it . In other words, you have a bowel obstruction. He said I was to have a colonoscopy as well, to determine the cause of the bleeding from the bowel.
SURGERY
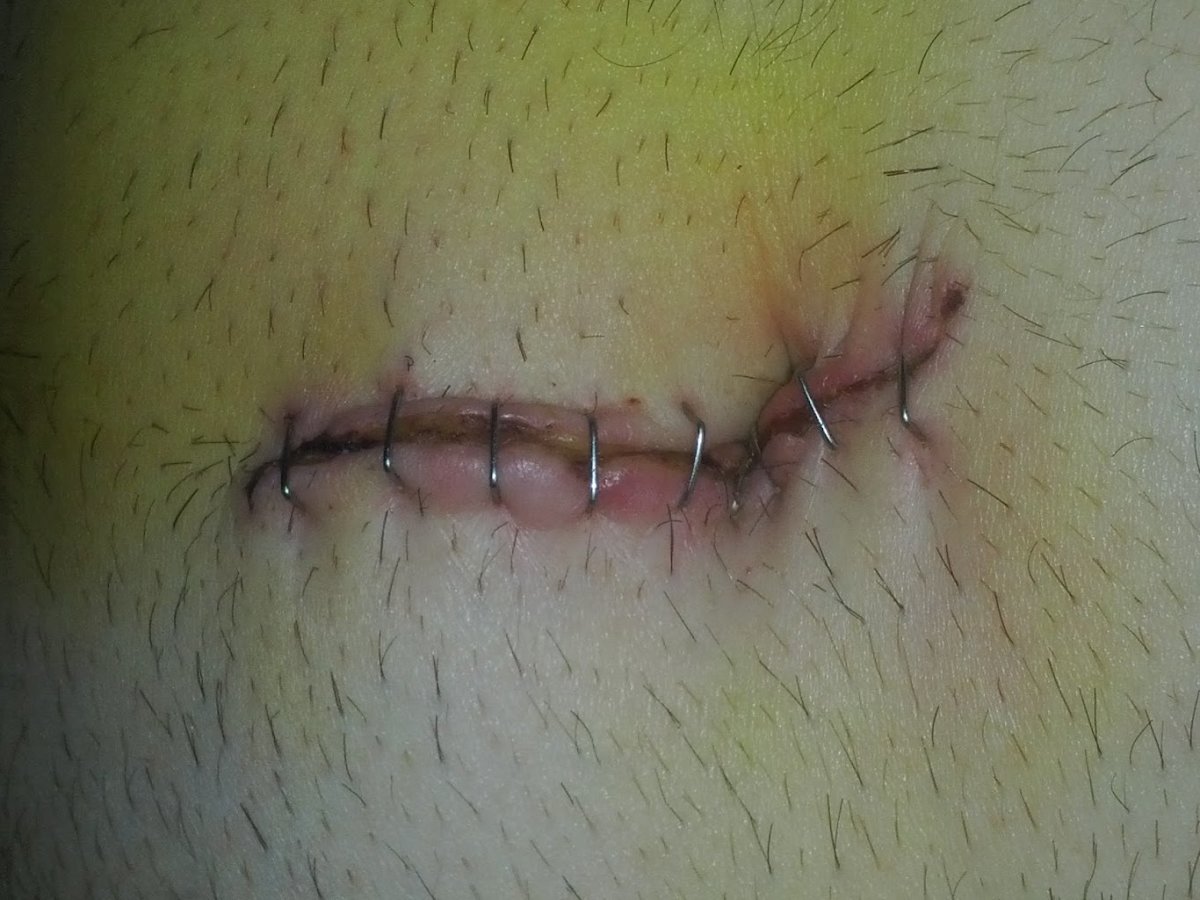
At surgery, the surgeon's fears were confirmed. Not only was there gross inflammation in my colon (large bowel) and rectum, but I did also have a sigmoid volvulus. There was a large area of my bowel that had been cut off from its blood supply and had subsequently died.The proper term for this is Ischaemic Gut Obstruction. Due to the large amount of inflammation I saw he told me, I suspect that you have Ulcerative Colitis , which is a disease of your colon and rectum with inflammation of your large bowel. I had to have extensive surgery to my bowel, requiring in the end an ileostomy to be performed.
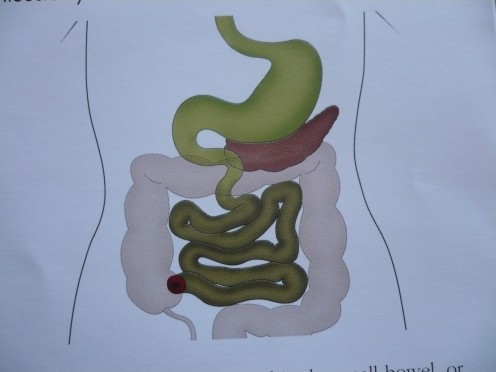
ILEOSTOMY; An artificial opending that is made between the ilieum and the outside. It is made surgically in the right lower abdominal wall when the colon has been removed, usually for ulcerative colitis.
RECOVERY PERIOD
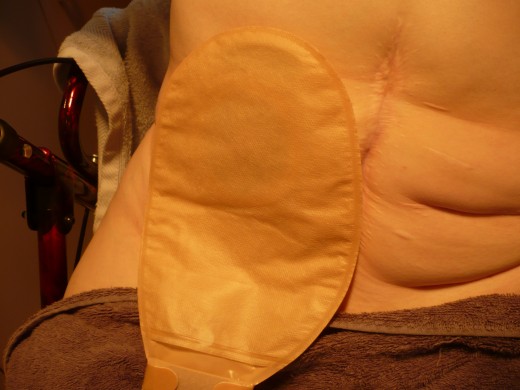
I spent the next few hours in recovery and then was taken to a room. I kept thinking about the bag that was now attached to my tummy, how long was it going to be there? How would I look after this thing? My tummy was sore from the big cut that the surgeon had made, but the Pethidine they were giving me was taking the edge of that . I felt so alone because this was Melbourne and I knew not a soul here. The nurse explained that I would be seeing a Stomal Therapist, who is trained to give you all the information about looking after your stoma. My what? Did she say stoma? She will also tell you about the types of appliances that are available and fit you with an appropriate one. There was a lot more to this ileostomy thing than I realised, but I was about to find out just how much more.
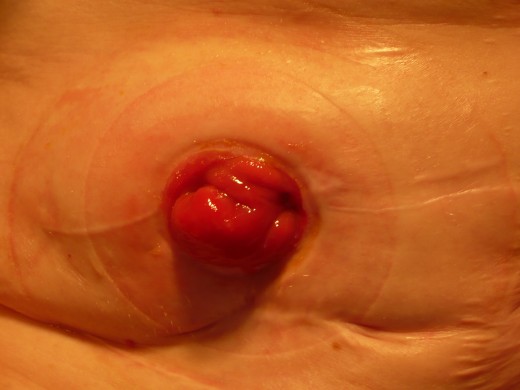
The Stomal therapist arrived just after breakfast, all cheery saying "and how are we feeling this morning, I hear it was touch and go with you. ischaemic bowel obstructions have to be caught fast, or you can die from one. You are very lucky indeed". Then why doesn't it feel that way to me, I said to her.You'll get used to having an ileostomy, very soon you will be a pro at changing your bag when it is appropriate. I just need to fit you for the correct appliance, as everyone is different and all stomas are different. She carefully lifted off the dressing that had been placed over my operation site. This is a well formed stoma, it shouldn't be too hard to find something suitable. She went on to fill me in on all the do's and don'ts about living with an ileostomy. I listened with much concern worrying how I was going to learn to cope with this bag attached to me. When everything was done, I looked down and saw this little pink thing, that looked something like a cherry (stoma). She placed the bag on top and said, i'll be back tomorrow to see how you are going. At least now I knew what a stoma looked like, but I still had my doubts about living with the thing.
COMING TO TERMS WITH MY ILEOSTOMY
I am now officially an ostomate accordingly to the Stomal Therapist. I continued to see the Stomal Therapist for the next ten weeks, getting more confident with my ileostomy each day that passed. I was starting to realise that really it wasn't so bad, afterall I could have died if the surgeon hadn't operated on time. I even gave my ileostomy a name which was very appropriate. The day I came home from the hospital, I took off my bag to empty and without any warning, this big spray of stuff came shooting out from the inside of my stoma and went everywhere. I thought the best name for my stoma was "SQUIRT''. Somehow, it was easier to refer to my ileostomy in those terms, so it was affectionately called this name.