Understanding BMT (Bone Marrow Transplantation)

Uses for Bone Marrow Transplantation
Bone marrow transplantation (BMT) is used to treat certain cancers and other bone diseases. It basically means taking healthy bone marrow (stem cells) and injecting it back into the person from which it came or into another person. It is beneficial in patients whose bone marrow is no longer healthy.
What is BMT used to treat?
- acute lymphocytic leukemia
- acute myelogenous leukemia
- chronic lymphocytic leukemia
- chronic myelogenous leukemia
- myelodysplastic syndrome
- non-Hodgkin or Hodgkin lymphoma
- aplastic anemia
- multiple myeloma
- sickle cell disease
- thalassemia
- immune deficiency disorders
- other bone marrow disorders such as destruction of stem cells in treatment of certain cancers
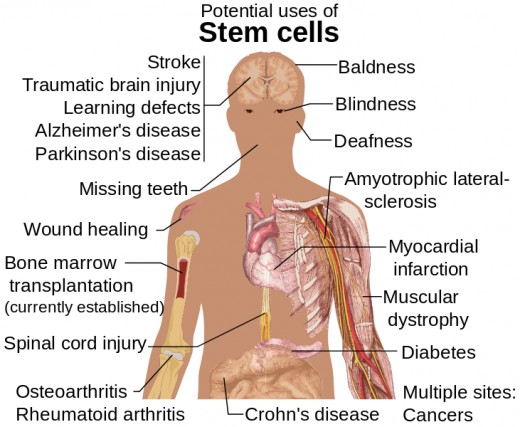
About Bone Marrow
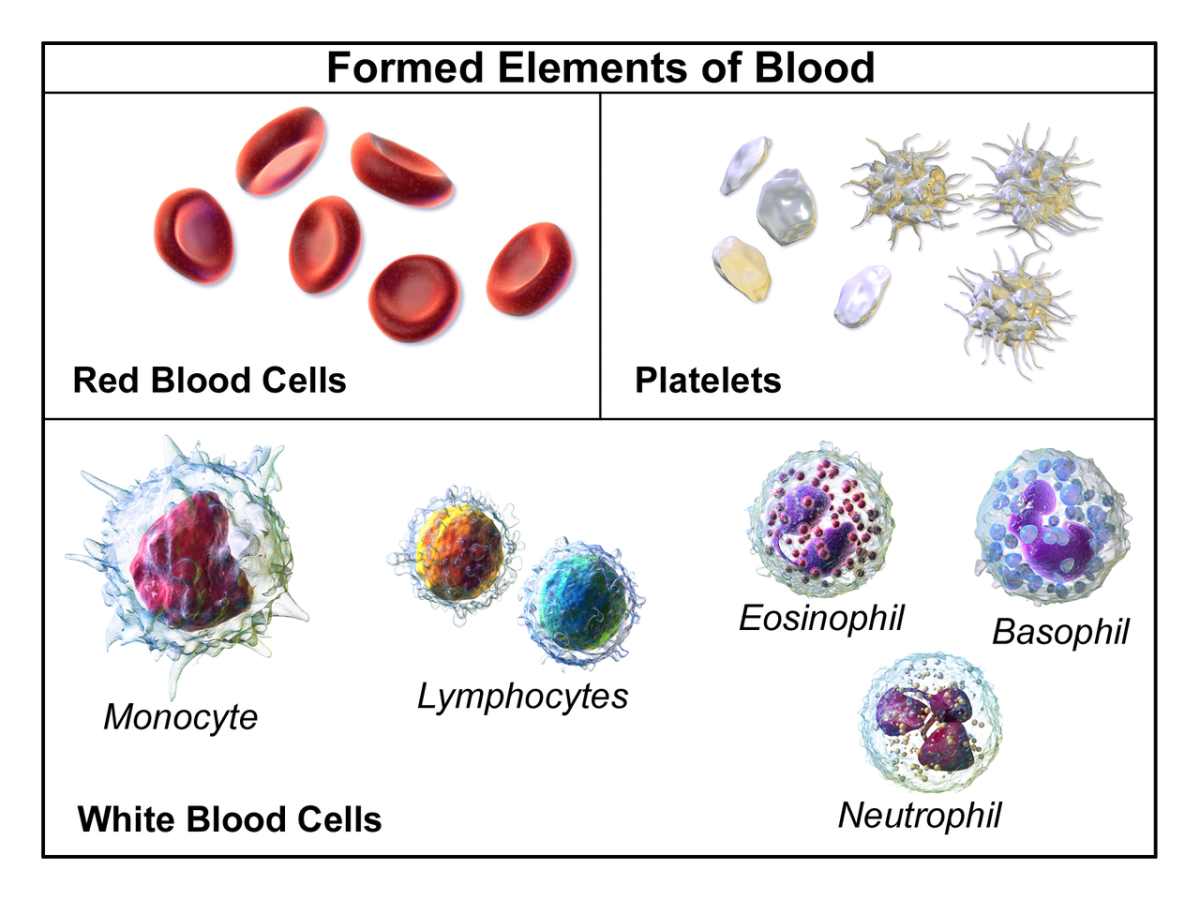
Bone marrow produces the body's blood cells and stores three types of cells:
- red cells - carrying oxygen to tissues
- white cells - preventing infection and aiding in immunity
- platelets - affecting blood clotting
Stem cells are immature blood cells that produce the above types of cells which then mature and function within the body.
Stem cells in the form of bone marrow transplantation replace diseased marrow and can be used in the treatment of aplastic anemia, leukemia or conditions like sickle cell disease.
Bone marrow transplants can also be given to regain normal bone marrow after bodily insults such as massive radiation treatments or chemotherapy. BMT is used in this instance as a rescue procedure to restore the bone marrow to its original vitality to maintain health and increase survival after many forms of cancer treatment.
The use of BMT can also aid in combatting congenital abnormalities or genetic disease processes.
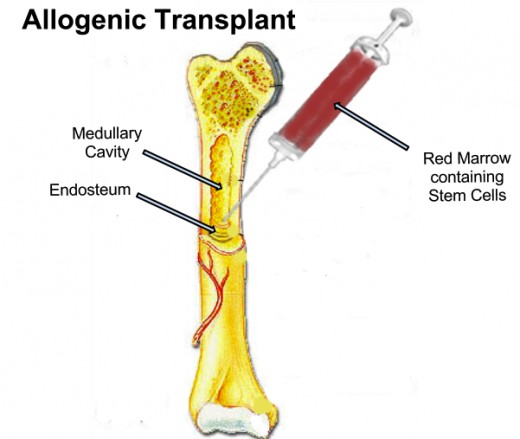
Different Kinds of BMT
There are several different types of bone marrow transplantation
- autologous - this comes from the patient himself or herself - cells are taken from the patient after he or she has received intensive ablative treatment. This is usually considered a rescue effort to reset or restore the patient's bone marrow to a healthy state. The bone marrow is usually frozen for later use - but it's important to note that someone with unhealthy marrow would not be a candidate for autologous transplantation
- allogeneic - donor bone marrow is a genetic match for the patient and BMT is given to the patient by someone else. Though usually a sibling's bone marrow or stem cells are used, matched and partially matched donors can be found through the national registry or a parent's bone marrow can be used if the marrow is a half match at the very least. Parental bone marrow transplants are more rare. Donors are given white cell growth factor to encourage development of more white cells and dislodgement of stems cells from the bone marrow into the blood stream
- umbilical cord blood transplant - cells taken immediately from the umbilical cord of an infant after birth. They are stored after testing and typing by freezing. These are newly generated stem cells and due to their T-cell properties, eliminate the possibility of graft versus host disease in the recipient and there is much less need for matching
Who Might Receive BMT?
Some of the factors considered before considering bone marrow transplant in a patient are:
- disease process or condition to be cured
- extent of disease
- overall prognosis/life expectancy without BMT
- premorbid conditions which might be life threatening or contributory to death
- age of patient
- patient's ability to withstand treatment
- availability of donor
- dedication to ongoing therapy and diagnostic testing most likely lifelong
Methods for Collecting Stem Cells
- apheresis - a needle is inserted in the donor's vein and a machine filters out the stem cells, returning the cleaned blood to the donor. It may take multiple sessions to collect enough blood this way for transplantation - sometimes blood growth factors are administered to increase the production of cells before obtaining samples
- bone marrow harvest or aspiration - a procedure done in the OR where a needle is inserted into the soft center of bone (usually hip or sternum) - once extracted, it is used to inject into the patient himself or herself or another recipient
- umbilical cord blood - collected at birth, the stem cells counted, the blood is typed and checked for viruses, then frozen and remains available for use at a later time or by another recipient through a national registry
Why Bone Marrow Transplant
How BMT Works
The patient is often given high doses of radiation and/or chemotherapy to ablate their resident bone marrow or wipe it out nearly to zero. This process is done to accomplish a "wiping out" of the bone marrow and stem cells so that there will be a clean slate for the new stem cells to find.
Bone marrow is not replaced in bone but rather the BMT is given as a blood transfusion. The new stem cells enter the bloodstream and begin regenerating healthy cells in the bone marrow, which thus cures the disease process. The regeneration usually starts to occur 15-30 days after the transplantation.
While the bone marrow is regenerating, the patient must stay in a sterile environment and be monitored closely for signs of infection and rejection as well as other complications.
The entire process is called engraftment and can take three to four weeks to begin to regenerate new healthy cells. Once the process begins, close monitoring will be carried out to assure further progress and watch for signs of failure or rejection.
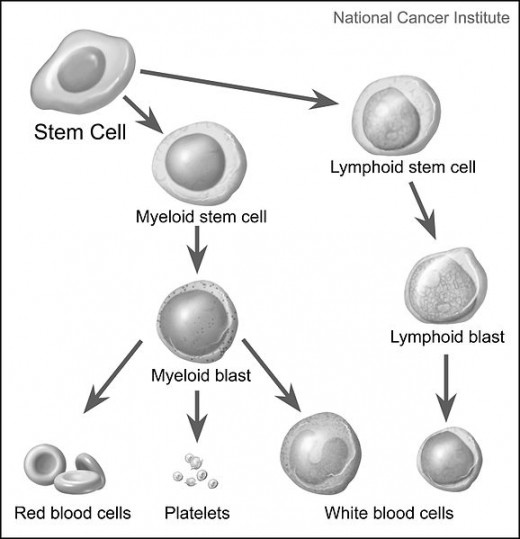
What is Engraftment?
When the donor cells (transplant) make their way to the patient's bone marrow and begin to regenerate new cells in his or her bone marrow, this is engraftment and is considered a successful transplant.
However, even after successful engraftment, the road can be a rocky one in terms of many stumbling blocks. Thus, the requirement for continual monitoring.
It can take months to years for the patient's immune system to fully recover and become functional again.
Did you know? Platelets are the last elements of the cells manufactured after BMT to recover?

How BMT Works
Worst Case Scenarios
Complications are always a possibility when transplants of any kind are involved. Some of the most common problems encountered in BMT are:
- infection - isolative precautions and antibiotics are often given as well as hygiene precautions strictly followed while the immune system is recovering. Infections can include viral, bacterial or fungal and patients may receive antibiotics, antifungals and antiviral medications, all with inherent risks
- pain - with immunity decreased and/or radiation and chemotherapy administration, patients are prone to pain in many locations but also from inflammation of mucosal tissues such as stomatitis or mucositis, sores in the stomach, esophagus and mouth
- low platelet counts and low red blood cell counts causing anemia - the patient may require transfusions due to the absence of these cells in their ablated bone marrow as without these two types of cells, hemorrhage can occur
- fluid overload - due to the increased volume being given after BMT, the kidneys oftentimes cannot keep up in eliminating excess fluid. Patients are weighed often and may have to be given diuretics and/or medications that help the kidneys function adequately to keep up with the increased fluid load
- allergic reactions such as hives, rash and swelling - these can occur from the transplant itself or from the medications used to treat other concurrent problems or reactions after the transplant
- stomach upset - many of the pretreatment regimens cause gastric distress in the form of diarrhea, vomiting or nausea. Medications are often required to help prevent patients from becoming dehydrated or requiring excess fluid boluses to prevent volume overload
- respiratory issues - these can occur as a result of infection or graft versus host disease should it occur or even from fluid overload. Oxygen may be a requirement during critical periods of respiratory distress
- organ damage - usually these include heart, kidneys and liver in response to some of the medications that are required prior to BMT but can also occur if there is volume overload
- graft versus host disease - this occurs when the BMT is rejected by the recipient's bone marrow and the new cells begin attacking the patient's cells. Complications can include all of the above scenarios which all can cause many complications and ultimately death if they are not reversed
- failure of transplant - if the stem cells fail to regenerate in the patient's bone marrow, this is considered transplant failure. Another transplant may be attempted once a suitable donor is found
- cataracts - these can occur due to many factors including the many medications given before and after BMT and are a known side effect
- delayed growth in children - stunted growth or delayed growth in children has been noted to occur with BMT due to the toxicity of medications and the stress put on the entire body by the aggressive treatments required for treatment of cancer and other diseases
- early menopause - for women not yet menopausal, there can be hormonal changes that occur as a result of the toxic therapies utilized with BMT
Rejection
It must be pointed out that unlike an organ transplant where the risk of rejection is centered around the organ transplanted (though other serious complications resulting in death can occur), BMT rejection or graft versus host disease in bone marrow transplant involves the rejection of the entire transplanted immune system. Bone marrow transplantation thus is far more complex than transplantation of an organ.
Did you know?
- Only 3 out of 10 people find a matched related donor
- It can take a long time to find a matched unrelated donor

How are Donors Matched?
Matching for BMT is achieved by examining the structure of the patient's and the donor's HLA, which is human leukocyte antigen. These antigens exist on the surface of white blood cells and are the markers of someone's immune system. There are over 100 HLA components but there are several which are considered essential to being identical for transplantation. However, the more HLA matches that exist, the better the chances for a successful transplant.
Matched related donors are governed by the premise that half of the HLA in the patient comes from the mother while half comes from the father. Thus if there are siblings with the same mother and father, each brother or sister would have a 1 in 4 chance of being an HLA match for a patient needing BMT. However, 7 out of 10 people needing donor marrow do not find HLA marker matches within their family.
The alternative is to enter patients into the National Marrow Donor Program (NMDP) and other registries for BMT. The closest match is selected from umbilical cord blood or stem cell donations and the match may be complete (matching all HLA components) or partial (matching only some of the patient's HLA markers).
Reduced-Intensity Transplants
For patients requiring BMT over the age of 60 or with certain diseases, the full bore ablative pretreatment for BMT may not be appropriate. Thus, the protocol of reduced intensity transplant may be used. This does carry an increased risk of failure or the need for retreatment or retransplant, however, this can be a viable option for individuals who cannot withstand the rigors of total ablative therapy such as combination high-dose chemotherapy and radiation therapy. These are referred to as mini-transplants and the intensity of treatment is significantly reduced.
Other Uses for Bone Marrow Transplantation
There is a protocol currently being used at Johns Hopkins for upper extremity transplantation which involves bone marrow transplantation. It is called the Immunomodulatory Minimization Protocol or IMP. In essence, it involves harvesting the upper extremities from a deceased donor but at the same time, also harvesting the same donor's bone marrow.
The patient receiving the donor extremities goes through the transplant surgery for the extremity or extremities, and then several weeks later, receives the donor's bone marrow as a blood transfusion. What's so incredible about this is that this protocol has been shown to reduce the risk of tissue rejection since the recipient now has the donor's immune system working inside his or her body. This means that the grafted organs or tissues would be less likely to be rejected by the patient because the immune system "recognizes" the extremity or extremities that were transplanted.
The other amazing part of this protocol is that it has taken triple-drug anti-rejection drug therapy and reduced it to single-drug therapy. The toxicity of the anti-rejection drugs that most transplantation participants have to take lifelong is relatively nonexistent in this scenario as the single drug that is being administered doesn't have all these associated health risks nor the potential for malignancy enhancement.
This could mean breakthrough therapy for all kinds of transplants. It remains to be seen how far BMT can go to modulate other disease processes as well as be an aid in organ and tissue transplants.