Vitiligo Holistic Solutions
Frances Blewitt CL.N

Vitiligo-Intro
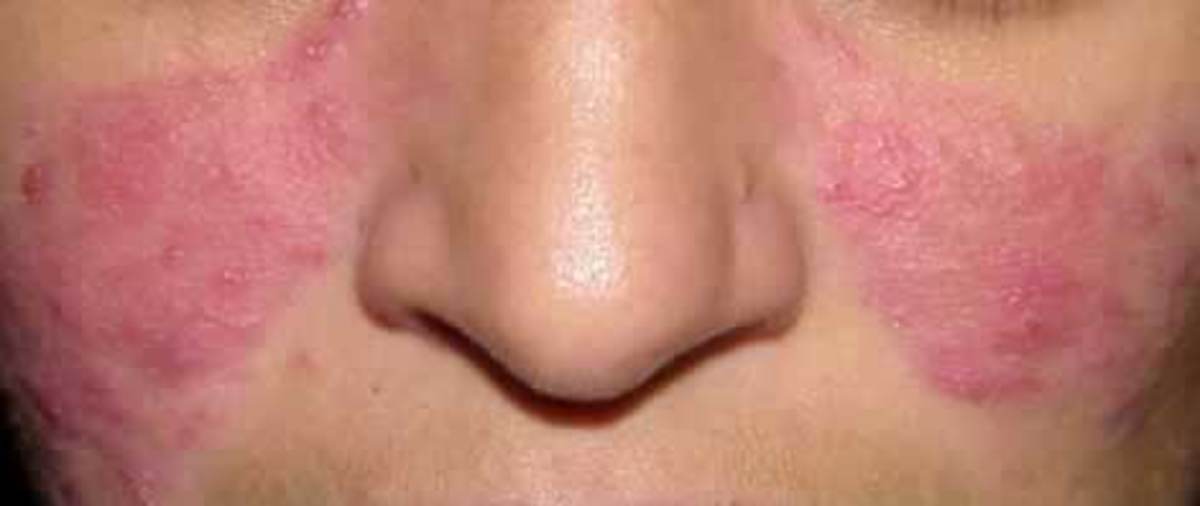
Vitiligo is a rare skin condition that presents itself as white patches on the skin. It is not considered life-threatening but the cause is unknown and there is no accepted known cure. Then why write this article? Back in the 1980's I had vitiligo and as a nutritionist I researched all of the scientific studies, articles and writings at that time and put that information together with my own integrated knowledge of health subjects and my personal health assessment and put created a program that would reverse my condition as it did and I have never been re-subject to this disorder again. Now I'd like to help others.
Studies have been done on specific nutrients mostly those involved with re-pigmentation of the affected skin, but the problem with that is that the white patches that appear on the skin are a symptom of the condition, not the cause. To date there are no thorough studies using nutrients to address what may be the cause of destruction of the melanocytes. The treatments available may address the symptoms, but they have many adverse side effects including causing more of the problem-more white vitiligo patches.
Symptoms and Signs
Possible symptoms may include any or all of those listed below
Patchy loss of skin color
Premature white or gray scalp hair, facial hair including eyebrows, eyelashes and beard.
Loss of color of the mucous membranes (tissues that line the inside of the mouth and nose)
Loss of, or change of, the color of the retina in the eyes
Inflammation of the eyes or hearing loss when those melanocytes in those areas are affected
Causes and Triggers
Vitiligo is believed to be an autoimmune disorder that occurs when the immune system attacks the melanocytes in the skin that produce melanin (skin pigment). It is also noted that it tends to run in families and appears most often in individuals with certain other diseases such as other auto immune diseases like thyroid disease and Addison disease. Oxidative stress may be a factor.
There seems to be no connection to race or gender but most cases appear in people in their twenties. Its first appearance is uncommon in the elderly, but has been diagnosed in newborns.
Highly stressful life situations such as death of a loved one often precede the initial symptoms and trauma to the skin such as sunburn or another injury seem to trigger new de-pigmented patches.
Conventional Treatments
Medical
- Topical steroid therapy. Steroids are used as an anti-inflammatory
Steroid based products like corticosteroid cream is used to restore color. This procedure may take months and may have side effects such as skin thinning or streaks or lines on the skin.
2.Topical (applied to skin) psoralen photochemotherapy (PUVA)
This therapy uses the coombination of psoralens with light therapy. Psoralen is a plant-derived substance that is either taken orally or applied to affected skin and then the person is exposed to certain light forms-ultraviolet A (UVA), UVB light or excimer light.
Psoralens makes you sensitive to light. Treatments are typically 3 times a week for up to 12 months. The use of oral psoralens can also make the lens of your eyes photosensitive. As a precaution wear protective eyewear for at least 12 hours after each treatment.
Oral psoralen photochemotherapy (PUVA)
Side effects include nausea and vomiting
PUVA treatment side effects may also involve severe sunburn and blistering, too much repigmentation or darkening (hyperpigmentation) of treated patches, increased risk of skin cancer, and is contraindicated with patients with known lupus erythematosus, porphyria or xeroderma pigmentosum, treated with cyclosporine or methotrexate and those who are pregnant or nursing.
Treatment is contraindicated for those with liver disease (may experience toxic levels of psoralens) and those with any medical condition in which a patient cannot tolerate heat, light or prolonged standing.
Possible drug interaction can occur with the oral use of psoralens when patient is taking other photosensitizing medications, non-steroidal anti-inflammatory drugs (NSAIDS), diuretics, antifungals, neuroleptics, and certain antibiotics such as tetracyclines and fluoroquinolones.
All these treatments are done under a medical doctor's care.
Tacrolimus or pimecrolimus (calcineurin inhibitors) with ultraviolet B (UVB) light are sometimes used for small areas.
The FDA (Food and Drug Administration) has warned about a possible link between these drugs and lymphoma and/or skin cancer.
Depigmentation
Depigmentation is used in patients who have vitiigo over large portions of their bodies to help blend skin tones. Removing remaining color (depigmentation) if vitiligo is widespread and if other treatments have failed to produce desired results. A de-pigmenting agent is applied and gradually lightens the pigmented skin so it will blend with the white patches or areas. These treatments are typically done once or twice a day for a minimal of 9 months. With these treatments, the treated skin never regains pigmented color and remains light sensitive indefinitely. It is considered non-reversible. Michael Jackson-the most famous case-is reported to have used this treatment. It is reported that at autopsy, the diagnosis of vitiligo was confirmed.
Side effects include irritation, redness, swelling, itching, dry skin, and permanent sensitivity to light.
Surgical
Used alone or with other therapies
- Skin grafts from persons own tissues (autologous)
Procedure removes very small sections of normal pigmented skin and attaches it to areas where you’ve lost pigment.
Risks include infection, scarring, a cobblestone appearance, uneven color and failure of the procedure.
2. Skin grafts using blisters
Called Blister Grafting-Your doctor creates blisters on pigmented skin usually with a suction, then removes the tops of the blisters and transplants them to an area of discolored skin.
Risks: scarring, cobblestone appearance, failure of the procedure, and procedure triggering new patches of vitiligo.
3. Micropigmentation (tattooing) The doctor implants pigment into your affected skin. Skin color may not match exactly and procedure can trigger new patches.
Research into possible future treatments include:
- Afamelanotide-implanted under skin to promote growth of melanocytes
- Prostaglandin E2 applied as a gel to skin
- Tofacitinib-oral drug typically used to treat rheumatoid arthritis.
Holistic Approach
The holistic approached is aimed at assessing the individual's complete and specific needs. Full assessments are conducted in areas such as deficiencies and higher hereditary requirements, immune function, stress loads, diet and supplement analysis, health and family health history to name a few in order to develop a complete health profile. This profile is then used to create an individually based nutritional, supplement and herbal protocol designed to correct the body's imbalances, and strengthen the immune system, adrenal functions and other systems involved in restoring natural pigments to the skin, and controlling the misguided immune system to stop its attack on the body.
© 2018 Angelllite