What do you know about varicocele?
various pictures on the Spermatic cord
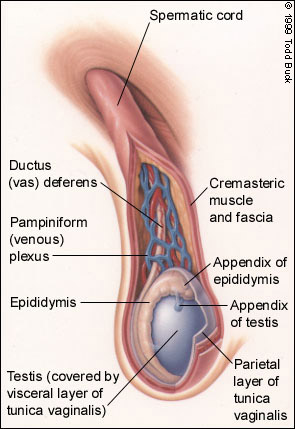
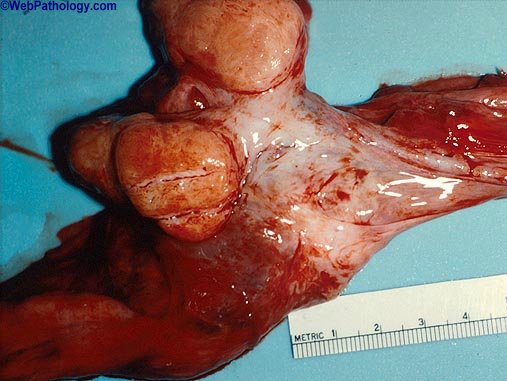
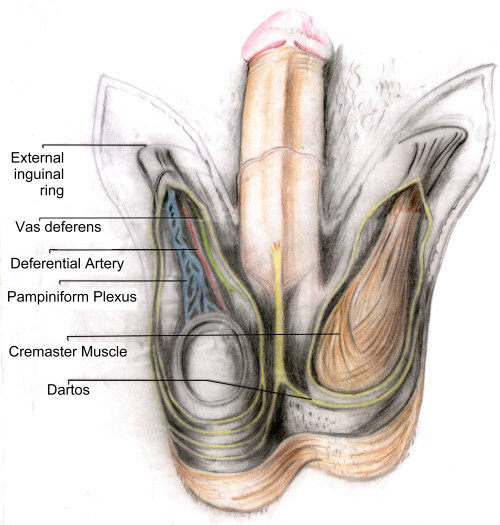
Overview
Varicocele is a mass of enlarged veins that develops in the spermatic cord, which leads from the testicles (testes) up through a passageway in the lower abdominal wall (system-inguinal canal) to the circulatory system. The spermatic cord is made up of blood vessels, lymphatic vessels, nerves and the duct that carries sperm from the body (vas deferens). If the valves that regulate blood flow from these veins become defective, blood does not circulate out ot the testicles efficiently, which causes swelling in the veins above and behind the testicles.
Due to impaired circulation of blood created by a varicocele, the blood does not cool as it does normally. The increased temperature of the blood raises the temperature of the testes, which is believed to contribute to infertility, as heat can damage or destroy sperm. The increased temperature may also impede production of new, healthy sperm.
Incidence of varicocle is 10-20% and is highest in men between the ages of 15 and 25. The sudden appearance of varicocele in an Older man may indicate a renal tumor blocking the spermatic vein. Approximately 40% of infertile men have a varicocle and among men with secondary infertility-those who have fathered a child but are no longer able to do so-prevalence may be as high as 80%.
A varicocle develops when the valve that regulates blood flow from the vein into the main circulatory system becomes damaged or defective. Inefficient blood flow causes enlargement (dilation) of the vein. Most men who have a varicocele have no symptoms. Asymptomatic (i.e, symptom-free) cases are often diagnosed during a routine physical examination. Signs and symptoms may include the following.
- Ache in the testicle
- Feeling of heaviness in the testicles
- Infertility
- shrinkage (atrophy) of the testicles
- Visible or palpable (able to be left) enlarged vein.
DiagnosisLarge varicocele may be seen with the naked eye. Medium-sized varicocles may be detected during physical examination by feeling (palpating) the area. A patient suspected of having a varicocele should be examined while standing up, as a varicocele is more prominent in this position than in the supine (i.e, lying down, face up) position. Small varicocles may be discovered by a physician using one of the following procedures.
- Doppler Ultrasonography uses ultrasound technology to detect pockets of heat caused by pooled blood.
- Venogram is an outpatient procedure performed under local anesthesia. the physician makes a small puncture in the groin and then injects a special dye into the spermatic vein. The dye in the blood stream enables the physician to see the anatomy in the vein on X-ray and detect the presence of a very small varicocele.
TreatmentIf the varicocele causes pain or atrophy, if it damages the testicles(s), or if the condition is causing infertility, surgey may be recommended. Most varicoceles can be corrected through a surgical procedure called varicocelectomy (i.e, surgically "tying off" the affected spermatic veins). The following methods are used.
- Surgical ligation usually requires general or regional anesthesia. In this procedure, a 2- or 3-inch incision is made in the groin or lower abdomen, the affected veins are located visually, and the surgeon cuts the veins and ties them off above the varicocele to reroute the blood through unaffected veins. An incision in the groin (transinguinal) is commonly used and a lower abdomen (retroperitoneal) incision is used in patients with scar tissue from a prior varicocelectomy or hernia repair. Surgery can be performed on an in- or outpatient basis. The patient typically can resume light activity within a week and strenous activity in about 6 weeks.
- Embolization is a non-surgical procedure that takes about an hour and half. A small tube (catheter) is inserted into a small incision in the groin to block the flow of blood to the varicocele. Venography is used to push tiny coils into place to block flow to the dilate vein. This eases the pressure, reduces enlargement and restores normal circulation. Light sedation, sometimes called "twilight anesthesia", is used during the procedure, the patient does not lose consciousness. Stitches are not needed. Normal activity is usually resumed within 2 days.
- Laparoscopy is a technique in which the surgeon inserts a tiny camera attached to a long cylindrical tube into the abdominal cavity through a small incision. Using the camera to locate the varicocele, the surgeon then inserts other instruments through the same incision to isolate an tie off the dilated veins. This technique requires a smaller incision than surgical ligation and is sometimes regarded as less invasive. The laparascope, however, can sometimes damage abdominal organs, which is not a risk factor in open surgery. The procedure takes about 2 hours and recovery about 2 days.
acknowledgement