What is Hepatitis? History of Hepatities, Type of Hepatitis, Causes, Symptoms, Diagnosis and Treatments
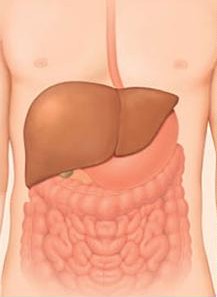
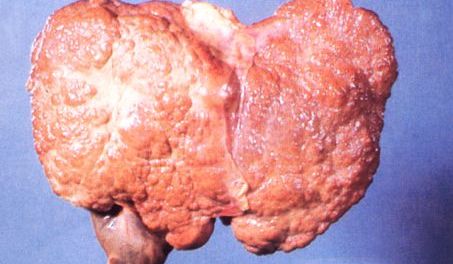
Hepatitis :
What is Hepatitis?
Hepatitis is an inflammation of the liver that can be caused by viruses, chemicals, drugs, alcohol, inherited diseases, or the patient’s own immune system. This inflammation can be acute, flaring up and then resolving within a few weeks to months, or chronic, enduring over many years. Chronic hepatitis may simmer for 20 years or more before causing significant symptoms related to progressive liver damage such as cirrhosis (scarring and loss of function), liver cancer, or death.
The word hepatitis simply means an inflammation of the liver without pinpointing a specific cause. Someone with hepatitis may:
- have one of several disorders, including viral or bacterial infection of the liver.
- have a liver injury caused by a toxin (poison).
- have liver damage caused by interruption of the organ's normal blood supply.
- be experiencing an attack by his or her own immune system through an autoimmune disorder.
- have experienced traum
The History of Hepatitis:
Hepatitis was believed to exist in viral form from ancient times. It is known that a disease existed that affected the liver and caused yellowing of the skin (jaundice). Between the 1800s and early 1900s, 2 types were identified as either serum type or viral type. In 1963 there was a major breakthrough which identified the cause of serum hepatitis and named the hepatitis B virus (HBV). Ten years later the cause of infectious hepatitis was found and named the Hepatitis A virus (HAV), and although scientists knew other viruses existed it was not until 1989 that the hepatitis C virus (HCV) was isolated.
Although the hepatitis delta virus (HDV) was known about since the mid 1970s, it was only in the late 1980s -1990s that it was understood to exist only in the presence of hepatitis B. In 1990, hepatitis E virus (HEV) and in 1995, Hepatitis G virus (HGV), were identified. Other viruses, hepatitis F virus (HFV) and transfusion transmission virus (TTV) are thought to exist, but are not as yet proven.
Hepatitis C An American Tragedy :
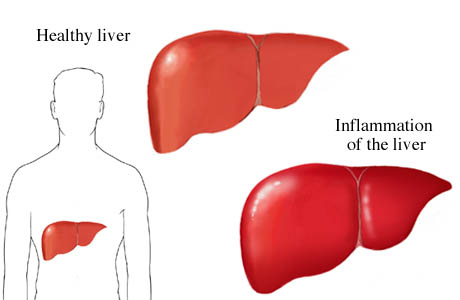
Types of Hepatitis :
Types of Hepatitis?
There are 5 types of hepatitis -
Hepatitis A
Hepatitis B
Hepatitis C
Hepatitis D
Hepatitis E
Note:- Each Hepatitis caused by a different hepatitis virus.
Hepatitis A Virus (HAV) :
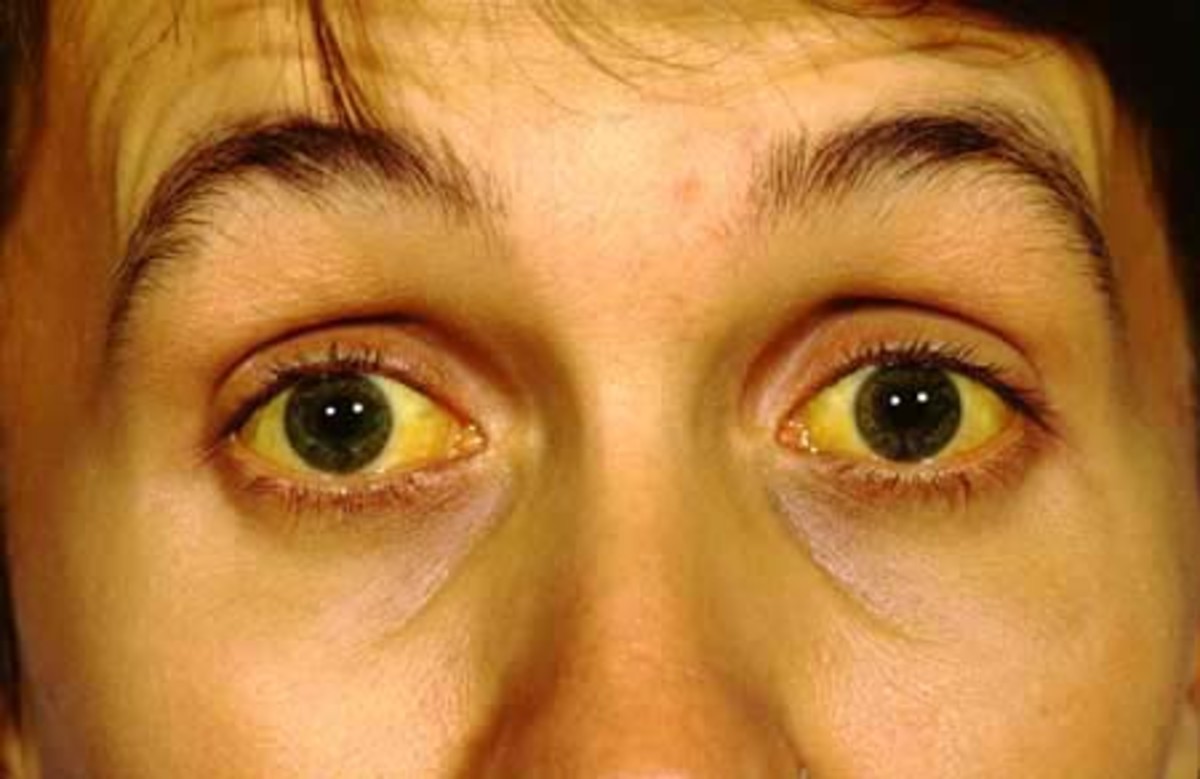
Hepatitis A is an inflammation of the liver due to the A type virus and is commonly known as infectious hepatitis. It is thought of as the least serious form of hepatitis as the person infected never goes on to experience the chronic form of the disease. People with this type of hepatitis generally make a full recovery. People with hepatitis A feel pretty awful, rather like experiencing a severe flu with jaundice (yellowing of the skin and whites of the eyes caused by the accumulation of the yellow/brown color bile pigment 'bilirubin' in the blood). A small percentage of infected people, notably the elderly or those with pre-existing liver disease, are at risk of experiencing severe symptoms of acute hepatitis and may become so ill that they require a liver transplant. Hepatitis A will not lead on to liver cancer or cirrhosis. Vaccine is available and is advisable for certain groups of people, workers and when traveling to various countries around the world.
What are the symptoms of hepatitis A?
Symptoms usually begin with fever, loss of appetite, nausea, abdominal discomfort and tiredness. These symptoms are generally followed in a few days by jaundice (a temporary yellowing of the skin and eyes), dark colored urine, and pale stools. Infected people can have symptoms that range from mild to severe, or can be infected without noticeable symptoms. Young children frequently have mild illness, or no illness at all. Recovery is usually complete.
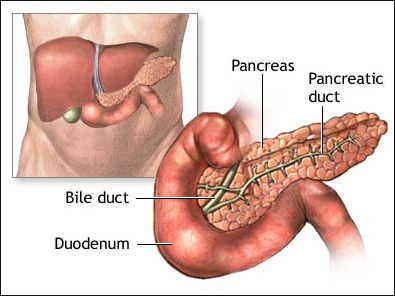
Hepatitis Treatment
Hepatitis B Virus (HBV) :
Hepatitis B - this is an STD (sexually transmitted disease). It is caused by the virus HBV (Hepatitis B Virus) and is spread by contact with infected blood, semen, and some other body fluids. You get Hepatitis B by:
- Unprotected sexual intercourse with an infected person (unprotected sex means without using a condom) Using a syringe that was previously used by an infected person (most commonly happens with drug addicts and people who inject steroids).
- Having your skin perforated with unsterilized needles, as might be the case when getting a tattoo, or being accidentally pricked. People who work in health care risk becoming infected by accident in this way. Sharing personal items, such as a toothbrush or razor, with an infected person.
- A baby can become infected through his mother's milk if she is infected.
- Being bitten by someone who is infected.
- The liver of a person infected with Hepatitis B swells. The patient can suffer serious liver damage due to infection, resulting in cancer. For some patients the hepatitis becomes chronic (very long-term or lifelong). Donated blood is always tested for Hepatitis B.
Hepatitis B Symptoms:
The symptoms of short-term hepatitis B vary, and can include:
- Loss of appetite
- Nausea
- Vomiting
- Fatigue
- Headache
- Fever
These symptoms may be followed by jaundice, an abnormal accumulation of the chemical bilirubin in the blood, which causes yellowing of the eyes, skin and body fluids (such as tears), as well as a darkening of the urine.
Other symptoms of hepatitis can include:
- Itching
- Weight loss
- Abdominal pain
- Sleep disturbance
- Confusion
- Loss of sex drive
Most people recover from short-term hepatitis and are no longer infected with the virus when their illness ends. However, up to 10% of adults may develop long-term (chronic) hepatitis. If an infant is infected with hepatitis B at the time of birth, the infant usually doesn't have any symptoms, but has a greater-than-90% risk of developing a chronic infection.
People with long-term hepatitis can have a broad range of symptoms. Some may not have any symptoms. In others, the disease is debilitating. The most common symptoms include:
- Fatigue
- Yellow skin (jaundice)
- An ill feeling (malaise)
- Decreased appetite
- Aching joints
A small number of people with chronic hepatitis develop liver cirrhosis. These people may develop symptoms of advanced liver disease, including jaundice, fluid within the abdominal cavity (ascites), swelling of the legs and changes in mental status such as difficulty concentrating or confusion. People with hepatitis B who develop cirrhosis are at risk of developing liver cancer.
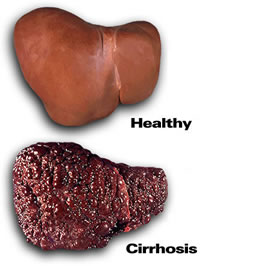
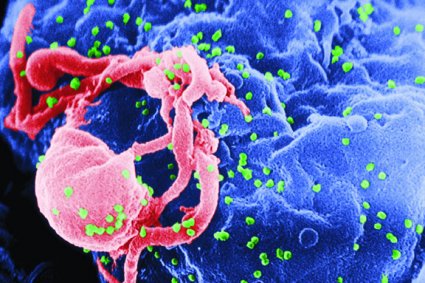
Hepatitis C Virus (HCV):
What is Hepatitis C?
The hepatitis C Virus (HCV) is one of several viruses that can cause hepatitis, a serious inflammation of the liver.
Complications of hepatitis include chronic liver disease, liver cancer, and liver failure.
Hepatitis C was first identified in 1989, before then it was known as Non A - Non B Hepatitis.
Since 1994, all blood donations have been screened for Hepatitis C.
What are the symptoms of hepatitis C?
- Jaundice (yellowing of skin or eyes)
- Loss of appetite
- Weight loss
- Nausea and vomiting
- Fever
- Tiredness
- Headache
- Stomach pain
- Dark urine
Symptoms usually appear 2 weeks to 6 months after exposure; however, most people (as many as 80%) experience no symptoms or very mild symptoms. It is important to remember that people without symptoms can still infect others. About 85 percent of people who become infected with HCV will become chronic (long-term) carriers.
Hepatitis C Is a Deadly Disease :
According to Dr. Eugene Schiff (University of Miami), the Hepatitis C virus (HCV) emerged in the U.S. population beginning in the 1960s, related to blood transfusion and injection drug use. The extent of the problem was only apparent after 1990 when reliable HCV blood tests first became available. Studies indicate that over the first 20 years of chronic HCV infection, 20% of chronically infected patients will develop cirrhosis, and many of those will progress to liver cancer. HCV-associated end-stage liver disease is a leading indication for liver transplantation in the USA and the developed western world.
Who is at risk for hepatitis C?
- IV drug users
- Health care workers
- People who have multiple sex partners
- Homeless people (risk of potential drug use, poor hygiene, poor nutrition, and unsafe living conditions)
- Military veterans who served in the Vietnam War era and those who have participated in high risk behaviors such as drug use and unsafe tattooing
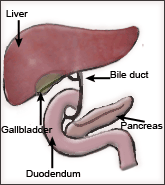
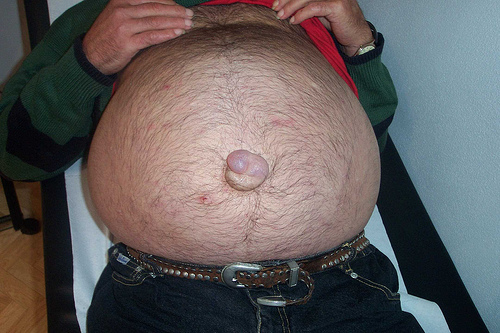
Hepatitis D Virus (HDV) :
Hepatitis D :
Hepatitis D, also called delta virus, is a defective virus that requires the helper function of the hepatitis B virus to multiply and is therefore only found in people who are infected with hepatitis B. Hepatitis D is the least common but most severe form of viral hepatitis.1
Worldwide the pattern of hepatitis D infection is similar to the occurrence of hepatitis B infection and it has been estimated that 15 million people with hepatitis B (HBsAg+) are infected with hepatitis D.2 Hepatitis D is not a common infection in Australia. Over the past 6 years there have been between 20 and 30 cases of hepatitis D diagnosed and reported each year.3
Hepatitis D infection can occur as a co-infection, which means it occurs at the same time as hepatitis B infection; or it can occur as a superinfection, in people who already have chronic hepatitis B.
People who are co-infected with hepatitis B and hepatitis D may experience a more serious acute illness and have a higher risk (2%–20%) of developing acute liver failure compared to people infected with hepatitis B alone.4
However, most people who are co-infected will clear hepatitis D and never develop chronic hepatitis D infection.
People with chronic hepatitis B who are infected with hepatitis D (superinfection) usually develop chronic (long term) hepatitis D infection. Long-term studies of people with hepatitis D superinfection show that between 70% and 80% develop cirrhosis (liver scarring) compared to 15% to 30% of people with chronic hepatitis B alone.5Up to 40% of people with hepatitis A have no identifiable risk factors for infection.
Hepatitis D Symptoms :
Hepatitis D may increase the severity of symptoms associated with all forms of hepatitis B.
Symptoms may include:
- Jaundice
- Nausea
- Vomiting
- Fatigue
- Abdominal pain
- Loss of appetite
- Joint pain
- Dark-colored urine
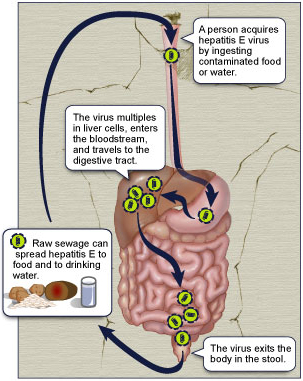
Hepatitis E Virus (HEV) :
Hepatitis E :
Hepatitis E virus (HEV) is the aetiological agent of non-HAV enterically transmitted hepatitis. It is the major cause of sporadic as well as epidemic hepatitis, which is no longer confined to Asia and developing countries but has also become a concern of the developed nations. In the Indian subcontinent, it accounts for 30-60% of sporadic hepatitis. It is generally accepted that hepatitis E is mostly self-limited and never progresses to chronicity. It has a higher mortality in pregnant women where the disease condition is accentuated with the development of fulminant liver disease. Currently, no antiviral drug or vaccine is licensed for HEV, although a vaccine candidate is in clinical trials. HEV genome is 7.2kb in size with three open reading frames (ORFs) and 5' and 3' cis acting elements, which have important roles to play in HEV replication and transcription. ORF1 codes for methyl transferase, protease, helicase and replicase; ORF2 codes for the capsid protein and ORF3 for a protein of undefined function. HEV has recently been classified in the genus Hepevirus of the family Hepeviridae. There are four major recognised genotypes with a single known serotype. The absence of a reliable in vitro propagation system is an obstacle to deciphering HEV biology. The genome of HEV has been cloned, sequenced and the infectious nature of these replicons has been established. However, questions related to replication, transcription, virus-host interactions and pathogenesis remain to be answered. This comprehensive review summarises the progress made so far in HEV research, and addresses some of the unanswered questions.
Hepatitis E symptoms :
The symptoms of Hepatitis E virus include fatigue, poor appetite, fever, vomiting and occasionally joint pain, hives or rash. Urine may become darker in color, and then jaundice (a yellowing of the skin and whites of the eyes) may appear. Some individuals may experience few or no symptoms. Symptoms usually appear two to nine weeks after exposure, but usually within 40 days.
How is Hepatitis E Virus spread?
Hepatitis E virus is transmitted through the fecal-oral route. This means that you get the infection by eating or drinking something that was contaminated with feces. Outbreaks in other countries are associated with contaminated water supplies.
Hepatitis

Treatments for hepatitis :
Hepatitis A Treatment:
Hepatitis A virus cannot grow outside of the human host, thus time and temperature controls are not relevant. Control of hepatitis A infection relies on prevention of contamination of the food through good sanitary practices, adequate personal hygiene and effective handwashing. Infected food workers must be excluded from handling food. Vaccines that provide immunity against hepatitis A are available. While the CDC suggests that vaccination protects against the spread of hepatitis A virus, widespread vaccination of food handlers has not been recommended to-date, mostly because the disease is not common. Vaccination of handlers may be considered as a precautionary measure in areas that experience a hepatitis An outbreak.
Control of shellfish-acquired hepatitis A includes preventing harvest from contaminated growing waters. In molluscan shellfish, it has been demonstrated that ≥ 4 log10 reduction of the virus can be obtained by heating to an internal temperature of 185 to 194°F (85 to 90°C) for one minute.2 In the interest of being conservative, the United Kingdom standards recommend holding commercial shellfish at an internal temperature of 194°F (90°C) for one-and-a-half minutes to assure inactivation of the virus.3
Validated high-pressure processing may be useful for control of hepatitis A in shellfish. A study in artificially contaminated oysters showed reductions of >1, >2 and >3 log10 of virus particles respectively with one-minute treatments at 350, 375 and 400 megapascals (MPa), within a temperature range of 8.7 to 10.3°C.4 A recent study shows that high-pressure processing may be more effective in inactivating hepatitis A virus if applied at elevated temperatures (>86°F or 30°C).5
Hepatitis A is a reportable disease in the United States and other countries. A doctor treating an infected individual or a retail establishment manager who is aware of an infected worker must contact the local health department. Food handlers should inform their managers if they contract or are otherwise exposed to hepatitis A.
Hepatitis B Treatment:
The majority of people with hepatitis B don't need specific treatment other than rest and they eventually make a full recovery. However it is important that the infection is monitored to check whether chronic disease develops, and the person is given advice about the risk of passing the infection on.
If the infection lasts more than six months (chronic hepatitis infection, where the virus continues to actively reproduce in the body) you may need more specific drug treatment to reduce the risk of permanent liver damage (cirrhosis) and liver cancer. Your GP should refer you to a specialist in either liver disease (a hepatologist) or general digestive diseases (a gastroenterologist). They may recommend treatment either with treatment called interferon, or with antiviral drugs.
Interferon (either alpha interferon or longer lasting pegylated interferon) is given as regular injections and helps boost the immune system to fight the infection. The response to interferon is variable, and some people who initially get better get worse again when the treatment is stopped. Others find that the side-effects of interferon mean that they cannot continue with treatment.
Several different antiviral drugs, known as nucleoside analogues, are also now used to treat chronic hepatitis. They are not a cure, but they suppress the virus. These drugs may also have side-effects - although not usually so severe as with interferon - and the virus may become resistant to them.
Hepatitis C Treatment:
The Food and Drug Administration has approved drugs for treating some persons with chronic hepatitis C. Unfortunately, treatment does not help all persons who have hepatitis C.
A person with hepatitis C should never drink alcohol because it may cause further damage to the liver. Check with your health care provider about tests, regular monitoring, and vaccination for other forms of hepatitis such as hepatitis A and B. Also, consult with your health care provider about all medications you are taking, including nonprescription and herbal remedies, to make sure they do not affect the liver.
Hepatitis D Treatment:
Chronic treatment for hepatitis D usually involves interferon therapy, either standard or pegylated. The antiviral medications used in treating hepatitis B, like lamivudine, aren't effective for hepatitis D. If the chronic disease progresses to liver failure a liver transplant may be necessary. The results of transplantation for hepatitis D are usually better than for hepatitis B.
Though treatment may be necessary, it's usually relatively expensive and will have side effects. Because of this, it's best to try to prevent infection in the first place.
Hepatitis E Treatment:
There are no specific medicines that can cure hepatitis E. Therefore, treatment of hepatitis E is focused on dealing with any symptoms or complications that may occur. This is known as supportive care. Even without specialized treatment for acute hepatitis E, most people recover completely within a few weeks.
However, there are some things you can do that might help you feel better. There are also certain things that you should avoid.
Following are some key steps to take as part of hepatitis E treatment:
Get enough calories. Many people with hepatitis E get nauseated, especially late in the day. In order to get enough calories, try eating the majority of your calories early in the day. Eating several small meals throughout the day (instead of three large meals) may also be helpful. If you feel sick in the morning, try eating some crackers or dry toast before getting out of bed. It may also help to drink lemon water or have a lemon drop.
Get plenty of rest. It's important to get as much rest as you can while your body fights off the virus.
Drink plenty of fluids. You should try to drink at least 10 to 16 glasses a day of water, clear juices, or other drinks that do not have caffeine in them.
Avoid medicines that can harm the liver. Talk with your healthcare provider about all of medicines that you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
Avoid alcohol. Alcohol poisons your liver and can cause even more damage to the cells that are already fighting the hepatitis E virus. The exact amount of alcohol that will harm the liver isn't known. Therefore, it's generally recommended that people with hepatitis E avoid alcohol completely.
Exercise regularly. Do light-to-moderate exercise, such as walking, for 30 minutes a day.
Once a person has recovered from a hepatitis E infection, the virus is no longer present in the body.