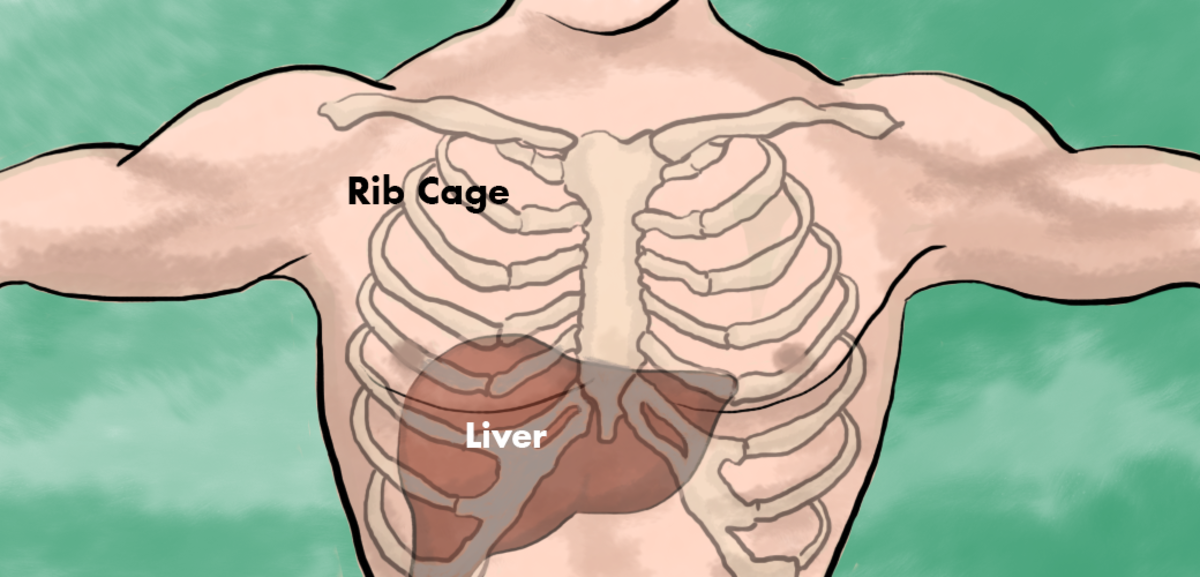
What is Deep Vein Thrombosis & a Pulmonary Embolism and how can you treat it effectively?
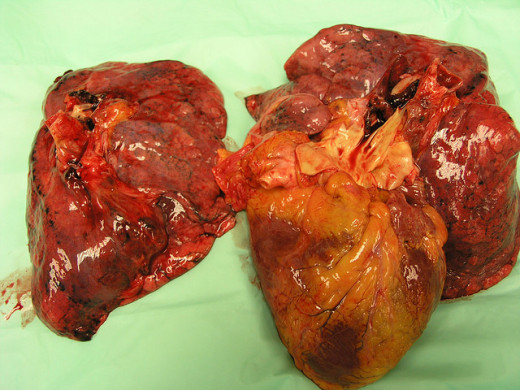
How well do you know PE?
What is a Deep Vein Thrombosis or Pulmonary Embolism?
Pulmonary Embolism, is a very large blood clot that has managed to reach within the confines of either side of the lung, or could even lay in the Pulmonary Artery as well. There is heavy evidence that state that genetics could play a very genetic role, particularly on a mothers side. Pulmonary Embolisms starts as a small clot that typically branches off from around the back of the knee, thigh or hip, and if left untreated, can reach major arteries where it could cause major problems.
This type of beginning problem is normally called a DVT (Deep Vein Thrombosis), and if left untreated, could break off and become a very fatal condition rather quickly. If you feel symptoms such as the following:
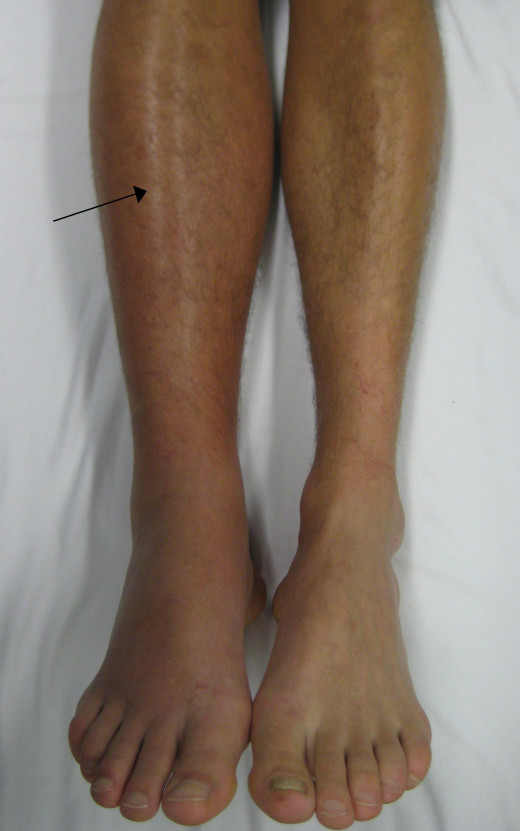
- Pain/Swelling behind the knee
- Radiating Pain that does not seem to disperse with activity or rest
- Warmth
- Discoloration or Vein color differences in the area of affected pain or discomfort
Remember that there are other subtle symptoms, and don't have to happen within the knee, but anywhere where a blockage may occur. There are some cases as well where there are no cases whatsoever, and a sudden faint or heart attack could present that the DVT has become a PE or worse, reaching a situation that can be fatal almost instantly.
So what causes a DVT?
In the Consensus of Deep Vein Thrombosis or Pulmonary Embolisms, there are many causes that could be causing your problem, but do not be feared, the chances of survival are much higher today. Twenty years ago, the chances of survival would have been maybe two out of ten patients survived. In the year 2014 however, the chances have skyrocketed to ninety-five out of one hundred patients surviving with proper and swift treatment. There are quite a few causes, from genetic abnormalities to simple problems like under-activity, even laying in a hospital bed for too long. Here is a list of possible causes so that you have them in front of you rather than reading back through the data, as follows:
- Inactivity such as being in bed to long, either hospital or simply at home
- With or Without Surgery, particular traumas to the soft tissue and veins/arteries
- Long Car Rides & Plane Takeoffs/Landings - This can be due to pressure changes that can potentially affect your natural body blood pressures, causing clotting to occur
- Obesity can constrict veins and other parts of tissue, causing ways for the blood to mimic an attack on itself, clotting.
- Pregnancy, especially after having the child with a Cesarean involved, the body attempting to re-adapt, creating clotting conditions to occur
- Smoking is known to cause a 20% increase in constriction within your blood vessels, creating ideal conditions for clotting to occur, especially in the lower extremities
In the end, it is safe to say that constant activity, being a avid health advocate for yourself, and staying away from smoking could cause alot of DVT issues from even occurring. With that said however, there is still a genetic deformity where your Chromosomes contribute in your genetic patterns, thus predisposition some people to the disorder, causing a hyper clotting condition.
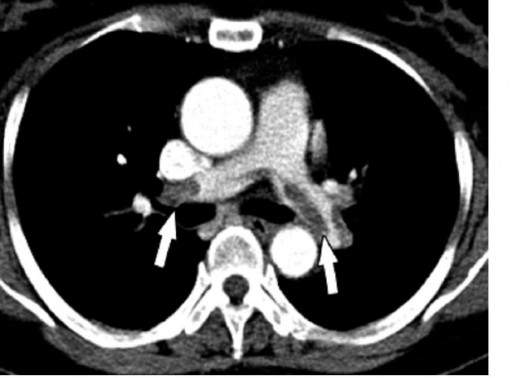
So My Doctor said it's now a Pulmonary Embolism, now what?
So you've found that the Deep Vein Thrombosis may have gone unnoticed and you had these weird feelings in your chest, maybe especially on the right side. It could even be shortness of breath and feel as though something is attempting to climb out of your right rib cage. These are signs that your Deep Vein Thrombosis has now broke off and started its travel to your lungs. This is called a Pulmonary Embolism, or a PE. Things can become quite complicated after this, as now specialists need to be called in called Hematologists, or Oncologists, to determine the severity of the situation. Here is a few of the symptoms accompanied with the Pulmonary Embolisms, and they can hurt, be forewarned:
- Dizziness
- Calf Pain
- One Sided Chest Pain, unless the blood clots havve become bi-lateral
- Heart attack symptoms on a daily basis
- Sweating and clammy skin
- When you take a breath, you may feel short of breath or extreme pain when doing so, unable to complete your respiration
- Spasms
- Cough that may include bloody sputum (Spit) that may get worse if the clot is breaking
- Your heart may feel as though it is continuously producing irregular palpitations, giving you the feeling of a heart attack.
Being a current survivor and fighter against seven to eight bilateral blood clots that are inside my lungs, I can tell you from personal experience it's a daily struggle. Luckily, if the clots have reached your lungs and you have not fainted or had heart failure and death, your one of the lucky ones. It is a blessing but be reassured that your lungs act as a natural filter to keep unwanted products from reentering your system to do continuous damage. The problem with this is that there is no instant solution, and some treatments can last from three to six months to the rest of one's life.
Well Known Phrases to remember
- INR - International Normalized Ratio
- PE - Pulmonary Embolism
- DVT - Deep Vein Thrombosis
- Coumadin - A Medicine that is prescribed to most patients after Injections to bridge them
- Lovenox/Heparin - Injection therapy to help Bridge you onto Coumadin Therapy to keep you therapeutic.
So What Treatments are there for Deep Vein Thrombosis or Pulmonary Embolisms?
Treatments for Deep Vein Thrombosis and Pulmonary Embolisms are one and the same, with few differences. A group of doctors, combined with a close check-in with your primary care physician (Make sure he's ready to take on your case) will decide the best course of action in order to keep you alive and well enough to perform half-way normally in society. It is going to be a life change, but if you want to live, this is the current technology that medicine has to offer.
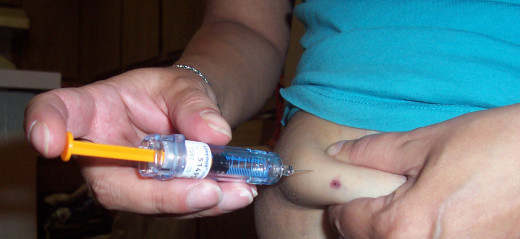
- Primary Care Doctors coupled with Specialists may want you on liquid anti-coagulants, a form of Heparin, Lovenox, or other Injection that you can use on yourself around the stomach area to help start a fast start to a potentially life threatening issue to resolve immediate problems.
- After your initial intake of injections, Specialists will then seek to bridge you onto a form of oral anti-coagulant like such as Coumadin after a process known as bridging you into a therapeutic level of blood thinning.
- This can be somewhere between 2.5-3.5 (INR) depending on weight and the such, and will be determined by your doctor. Your INR, or International Normalized Ratio, is your blood thinning normality that the doctors internationally deem to be therapeutic to keeping the blood clots from forming new ones. Of course, this will have to be checked every few days as determined by your specialist, to keep you in therapeutic range.
- If your like me, and your genetics along with the other 30-40% of patients that seem to fail Coumadin therapy, remember not to lose hope. Specialists will then consider placing you on a strict injection only therapy that will keep your blood thin without having to check for INR levels on an almost daily basis, and with other vitamins and a change in lifestyle, your life may be just as normal as it was before the events.
In Conclusion to DVT's and PE's
Remember, if you happen to have this disorder, and have not stumbled across this article for information only, there is hope. Remember to keep a active lifestyle, fight for your right to live. There is no reason to give up when there is plenty of hope to survive and even live on for a better life than you had before. Keep Active, change your current lifestyle, from smoking to drinking to anything that can be potentially harming to your body.
If you once followed a religion, and fell away from it, remember that when your in the hospital and fighting this, miraculous things can happen.Take the time to pray, keep faith in your hands, it's been working in my case, im still living to write this article for others to learn from what I've personally been through. There is more to life than just a hope for a better tomorrow, as you can be a part of that better tomorrow and make it that much better. Be grateful for what you have, enjoy the little things, you never know when it may be taken from you.

If you enjoyed this article, and would like to view others, click below:
- Genetic Memory: How is it found in biological perspectives?
Ancestral Recollection, Genetic memory that is the notion in which an individual displays unconscious instinct. What exactly is Ancestral Recollection, and how does it relate to our species or others - Selflessness: A True Beginning to Society and Culture
What exactly is Selflessness, and can it truly be reached in a lifetime? This article helps to explain the various notions behind this concept from the individual level onto the sociological aspects of culture and how it relates to Selflessness. - The Sono-Pictorial Connection: A Study of Dolphin Communication
Dolphins, regarded as man's best friend in the marine world, have intrigued scientists the world over in their complex functions throughout the marine world. Their Sonar has another feature: Language - The Hyperspace Equation: Could it work?
Ever wondered about the Possibilities of space or the discrepancies of such a exotic theory? The Star Trek Author thought it was possible, as does current NASA Research. What is your Opinion? - Factor V Leiden
Factor V Leiden is a condition that affects many people. It is genetic and can cause blood clots. These clots can cause problems in pregnancy, cause vein damage, and can be potentially fatal. Factor V Leiden causes a higher risk of pulmonary embolism