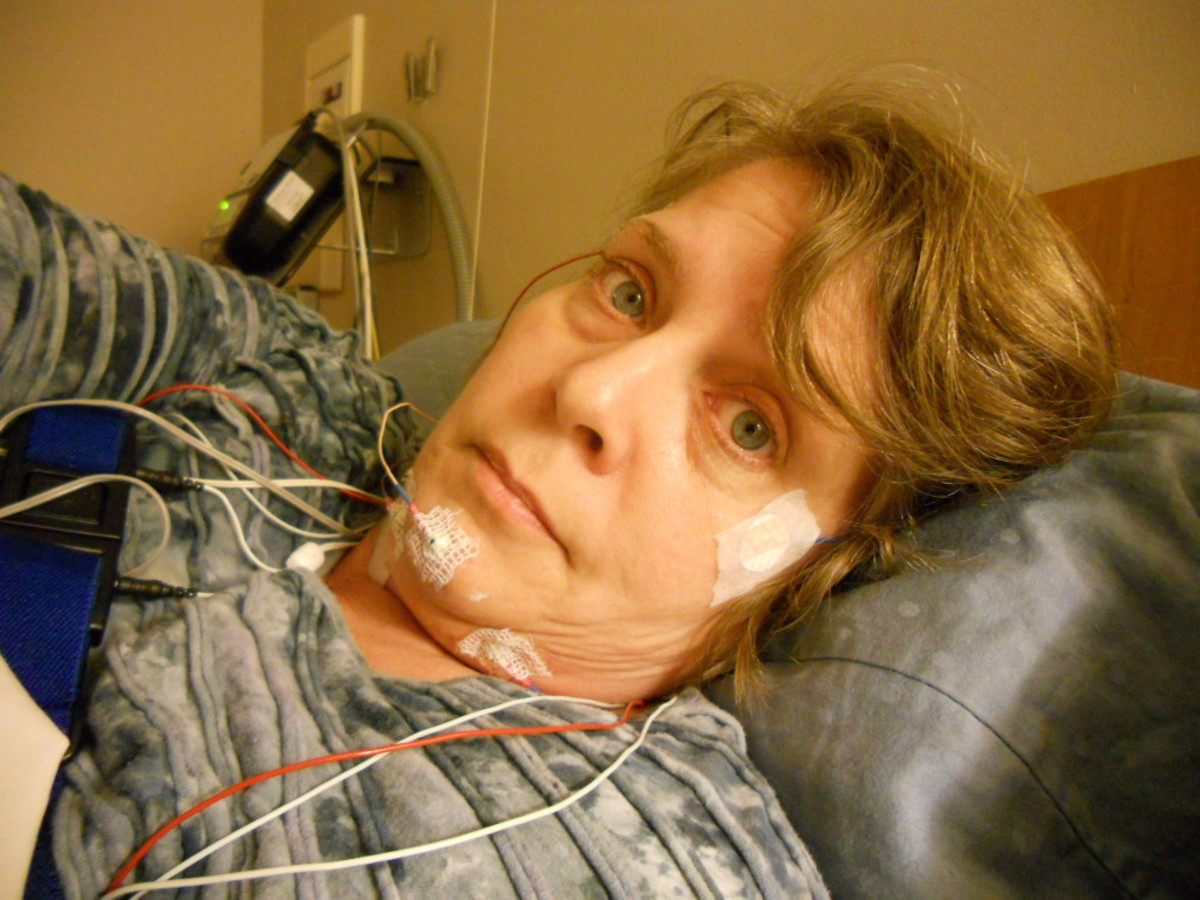
What to Expect during a Sleep Study
While many people drift fast asleep with images of sugar plum fairies dancing in their head; others try everything from counting sheep to drinking warm milk in order to fall asleep, stay asleep or combat issues that interrupt their slumber. For those with issues affecting the quality of their sleep and wake times a sleep study may be just the thing the doctor ordered.
I recently completed a sleep lab at my physician’s request to look for signs of apnea, a common sleep disorder in which breathing can stop and start resulting in inability to breathe properly, snoring, and other nighttime disturbances. Read below to learn about sleep studies, how to know if you need one, and what to expect for your upcoming appointment including things to prepare, what happens while you’re sleeping, and follow-up care with your physician.
What is a Sleep Study?
Have you ever had a sleep study?
A sleep study, also known as a polysomnogram, is an overnight study in an accredited lab or center is the best way to fully diagnose what is going on with your body at night while you pass through different stages of sleep.
What are the different stages of sleep?

There are 3 phases of “Non-REM” sleep, including drowsiness, light sleep, and deep sleep. Then we pass through “REM” sleep which usually happens about 90 minutes after you fall asleep. You can cycle through the different stages of sleep many times throughout the night.
A study overnight is the best way to analyze your brain and physiological response during all the different phases of sleep.
Your brain waves, breathing, and heart rate will all be monitored during your overnight stay.
How do I know if I need this study done?
This test is usually ordered by your physician or health care provider to find out if you have a sleep disorder that may be affecting your overall health or well-being during your waking hours. It is also used to tell if you have any type of apnea that may be obstructing your breathing, resulting in drowsiness, sleepiness, lethargy or other symptoms during the day.
Most commonly, your doctor will order a sleep study due to the following reasons and symptoms:
Apnea
| Narcolepsy
| Bedwetting
|
Day drowsiness
| Sleepwalking
| Insomnia
|
Problems sleeping
| Snoring
| Restless legs
|
Conducting an overnight study is usually the only sure way to diagnose the root of the issue causing your symptoms and find the right treatment for you individually. While preparing for your overnight stay may seem like a hassle, think of it as a necessary test to add value to your well-being during your waking hours. After all, who wants to live with symptoms like those listed above? The study will be your answer to all of your sleeping issues.
My doctor recommended a sleep study because of my short stature there are often concerns with sleep apnea issues.
Getting Prepared

Dos & Don’ts before your study:
- Fill out any paperwork ahead of time. Some centers will send you a diary to keep a week or few days before your study to understand your typical sleep pattern.
- Do wash your hair and go in with a clean scalp.
- Do not apply hair sprays or gels onto your scalp that may interfere with sensors.
- Avoid caffeine and alcohol in the afternoon and evening.
- Take any medication as usual and as prescribed.
- Follow your normal routine the day and evening before so as to not interfere with your sleep that night.
- Pack an overnight bag.
What you should bring in your overnight bag:
- Shampoo & conditioner (through many center’s provide shampoo you can use the next morning to get the gel out of your hair from where the sensors were applied).
- Towel or wash rag.
- Toiletries needed to brush your teeth, comb your hair, apply makeup etc. both before you go to bed and when you wake up the next morning.
- A change of clothes for the next day.
To prep for my own overnight stay, I wore the clothes I planned to sleep in that night (soft pajama pants and a t-shirt) and packed a change of clothes for the next day along with my tooth brush and cell phone. A small bag should be all you need. In fact, I didn’t even use much of what I packed at all. The night I completed my study I was the only patient scheduled and left by 6:30 in the morning so I went straight home still wearing my clothes from the night before. Most facilities provide showers to clean the gel they use to adhere the sensors to your head out of your hair in the morning. The lab that I stayed at did not have a shower in the room though I packed a small bottle of shampoo and conditioner just in case.
Arriving at the Center

When you arrive at your lab or center to check-in for your study, you will usually arrive later in the evening an hour or two before you normally go to sleep. The staff will show you to your room, which is typically a private sleeping quarters that looks like a typical bedroom with a comfy bed, television, night stand and private bathroom. Don’t worry, most centers are not typical of a medical or hospital setting. They try to create as comfortable an environment as possible to encourage a good night’s sleep so they can gather good data from patients.
After you change into your pajamas, staff will begin applying sensors to your arms, legs, chest, and head. You may feel a little alien-like hooked up with a bunch of wires, but you will hopefully fall asleep not longer after you are hooked up.
Staff will then leave the room and typically turn on all of their monitoring equipment and cameras that they will use to monitor your sleep during the night. You will then typically be allowed to read or watch TV for a few minutes until you are ready to fall asleep.
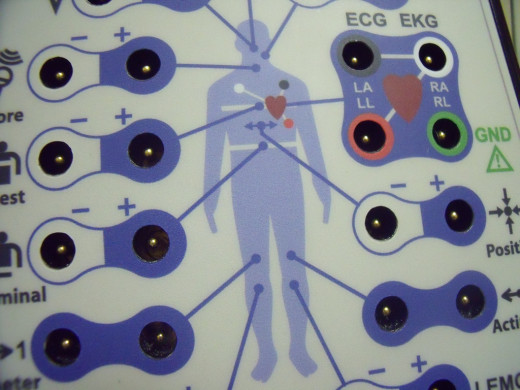
An demo of sensors used in a sleep study
Once I checked into my local center of sleep, I was ushered to my room and was pleasantly surprised to find the room very welcoming and cozy. It looked just like a bedroom you might find in a guest house, hotel or even your own home!
The technician began applying the sensors right away. There were two long cables that went down each leg and up through the top of my shirt which connected to my legs to detect any restless leg symptoms. Next, she strapped on breathing monitors across my chest and stomach then began to tedious apply the several tiny cables and sensors to my forehead, chin, behind the ears, and around the top of my head. Once I was all hooked up, it was time to climb into bed and connect all of the sensors together to a machine at the bed side table. The technician asked me to lay down and complete a calibration test where she asked me to take deep breaths, look in different directions, blink, and move my ankles up and down. Once she verified all of the sensors were reading properly, it was time to fall asleep.
Sweet Dreams

The hard part is over!
Now all you have to do is drift fast asleep!
A lot of people wonder how someone could sleep hooked up to electrodes and measuring wires, but the environment is built around providing the best sleep experience possible during your stay so you can get the results and answers you need.
What happens while you are sleeping?

While you are sleeping staff are monitoring you in a nearby room. All of the sensors are gathered up behind your pillow to allow you to freely change positions during the night. Often, staff are monitoring for sleep apnea issues. If they pick up any signals of apnea, they may awaken you to fit you with a CPAP or BiPAP mask that provides a steady stream of air through your nose or mouth to keep your airway open. You can then fall back asleep while staff monitor how you react to the CPAP treatment. Sometimes if apnea issues are detected a second study may be required to monitor how you react to different streams of air and find just the right pressure and CPAP settings that are right for you.
If you have to get up in the middle of the night to use the bathroom, usually you can simply say out loud that you need to use the restroom and the staff monitoring you can usually hear and communicate with you in the room.
I will admit it was slightly difficult to fall asleep right away in a new environment. I felt as though I never feel asleep very deeply and remember tossing and turning quite a bit throughout the night. Luckily, the technician never had to wake me up in the middle of the night to adjust any sensors or perform additional CPAP tests and the night passed by very quickly. Once she woke me up, we removed the sensors, filled out a survey about my experience, and I was able to drive straight home to wash the sensor gel out of my hair!
Follow-Up
What happens after your study?
After your study, a sleep technologist will analyze all of the data gathered including:
- Breathing patterns
- Heart beat
- Eye movement
- Leg and limb movement
- Brain waves
- The number of times you tossed and turned and more!
Results of your study will be scored and given to a doctor for follow-up to review with you. When visiting with your doctor about the results of your study, below are some questions that you may want to make sure you get answers to before the end of your visit:
1. What do these results mean for me?
Make sure you understand the results of your study in layman’s terms. Ask your provider to explain what the rapid eye movements or your high or low numbers mean in comparison to others who may be experiencing similar symptoms.
2. What treatments are available?
If a doctor recommends only one treatment that you are unsure about, don’t be afraid to ask if there are alternatives you can try.
3. Will my insurance cover them?
Find out how much your insurance will cover as you discuss treatment options.
4. When should I follow-up again?
Make sure you have a follow-up appointment scheduled to discuss how your new treatment, if any, is going. Find out if and when a follow-up study is needed.
Have you ever had a polysomnogram? How was your experience? Did you get beneficial answers/treatment as a result?