When Health Anxiety Becomes A Way Of Life
Opening The Door
With all the attention in healthcare turning to preventative medicine and early detection these days, it’s no wonder that an increasing number of people are affected by health anxiety to some extent. Healthcare marketing even goes as far as to try and plant the question in the minds of people regarding whether they are healthy. While a certain amount of concern for your health is normal, the manifestation of compelling fear that something serious is wrong can be detrimental your well-being and ironically, even bad for your health in some instances.
Many factors influence our level of concern about health in general, but in the instance of debilitating anxiety wherein a serious illness or condition is thought to exist, there but is a single factor responsible for its intractable nature. For most people experiencing persistent health anxiety, there is nearly always a precipitating cause, including death of a family member, exposure to serious illness in a loved one or having suffered a serious illness, misapplication or misunderstanding of medical information and even unexplained symptoms by the person with health anxiety.
Individuals with chronic health anxiety typically misconstrue unfamiliar changes in body function as symptoms of an underlying condition or disease. By far, the most common unusual sensation that occurs as a departure from normal for most people is the sensation of heart palpitations and for the sake of brevity, we’ll discuss this particular feature as a means to illustrate the general progression of health anxiety.



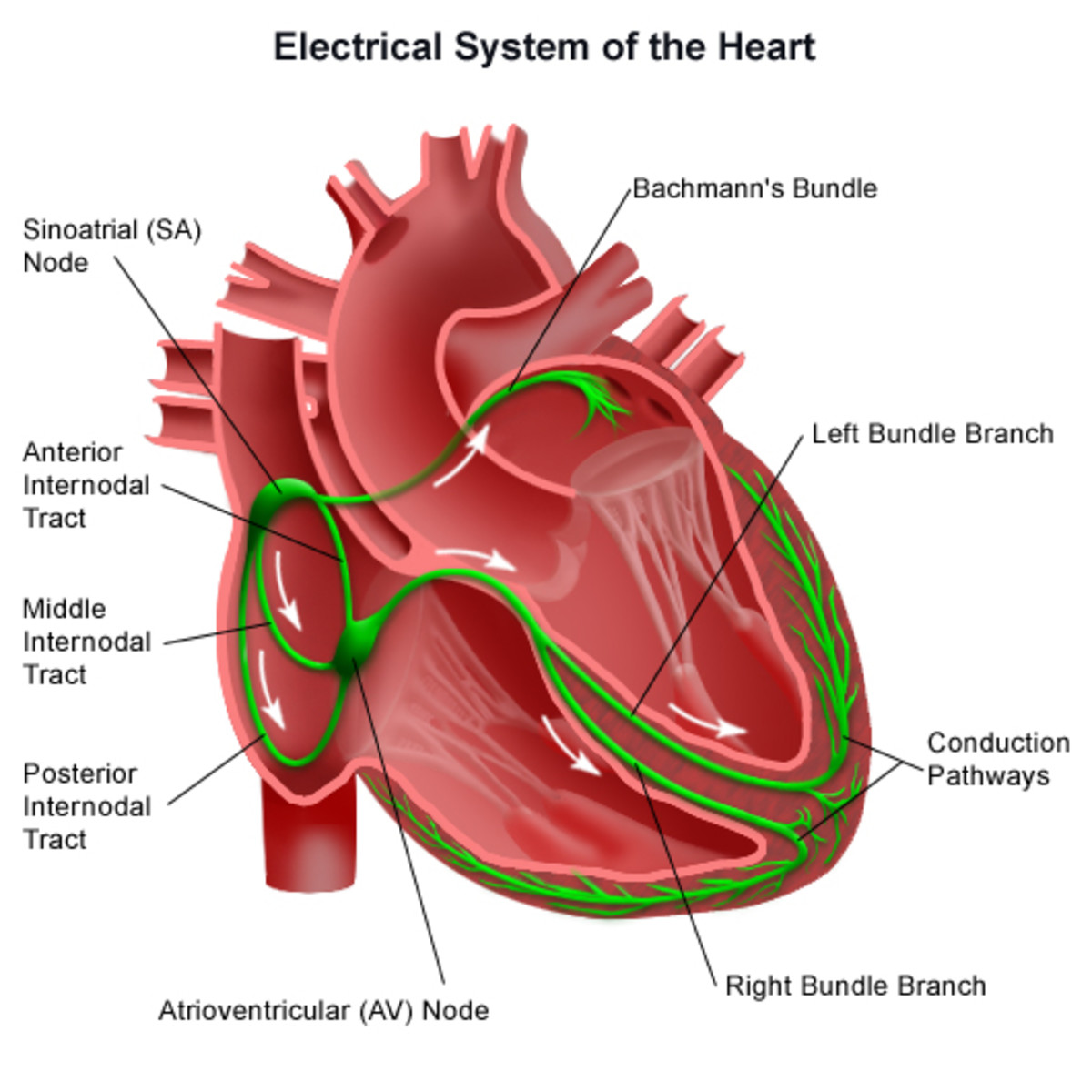
Heart Palpitations
While the clinical definition of a heart palpitation is the ability to sense one’s own heartbeat, we’ll take it a bit further and clarify a heart palpitation as the ability to sense a change in one’s heart rhythm. It’s important to note that in the instance of paroxysmal contractions, or heartbeats occurring where they normally shouldn’t, these events are almost universally misinterpreted by those who detect them as a sign that the heart is experiencing trouble of some kind. This perception largely arises because most laypersons derive information about medical matters through the Internet and one of the most high profile topics in that regard is heart disease as it relates to premature death.
It can certainly rattle even the most unflappable individual when the heartbeat becomes abnormal and there is a natural presumption that a problem exists because the heart otherwise functions in a very predictable manner. The heart also naturally represents to most people the one single organ responsible for keeping us alive, without which we would immediately expire. While it is true that there are a number of actual cardiac arrhythmias considered to be pathological, the instance of palpitations being discussed here, and which occur most commonly in otherwise healthy persons, is entirely benign. The fact is, everyone experiences benign palpitations of the heart at some point in time, but some people become sensitized to their presence. We’ll talk more about their cause later, but first let’s discuss some basic physiology and brain function responsible for what makes us afraid and why palpitation events commonly arise in persons with anxiety.


To Stand And Fight Or Run?
The human body is cast by genetics and is replete with all the bells and whistles to increase the greatest likelihood for safety and survival. It’s a shared trait in most living things, stronger in some species than others. By bells and whistles, we’re speaking of reflexes. Reflexive actions are the pre-programmed responses by the body in response to a variety of conditions. In fact, a portion of what we do each day is very basically reflexive in nature and doesn’t require active thought. We seemingly adjust automatically to some changes in the environment around us without thought to make it occur.
For purposes of our discussion here, the reflexive characteristic that we wish to focus upon is known as the fight or flight response. This is the brain’s natural response to fear. Essentially, when this reflexive response is initiated, the brain makes rapid adjustments to the body’s physiological status in order to improve the chances of survival and ultimately seek safety. You can sort of think of all aspects related to survival as the gas pedal and the elements of safety as the brake pedal, where the gas pedal is actually the sympathetic nervous systems and the brake pedal is the parasympathetic nervous system. It’s very important to understand how this system functions with regard to health anxiety.
When we’re confronted with threat to our safety, whether perceived or real, the brain automatically responds by temporarily altering the body’s physiology in preparation to either physically overcome the threat or alternatively escape from it. Among these changes epinephrine, or adrenalin, is increased which correspondingly causes an increase in heart rate to make sure that the turnover of oxygen-rich blood is accelerated for intense muscular exertion. Respiration is also increased for the same reason. GI motility is decreased in order that blood is more available to the limbs, nervous system function is accelerated such that the body’s senses all become extremely acute and reaction time is increased considerably. Even the brain demonstrates increased vigilance to the focus of the threat. Many more changes occur, but the point is that the sympathetic nervous system is preparing your body for combat or escape with the ultimate goals of safety and survival.
Conversely, once the threat has passed, the brain signals the body to revert to normal. Epinephrine returns to normal output levels and the heart returns to its basal rate, respiration is reduced and GI motility is increased. The nervous system also returns to the range of normality and senses are adjusted accordingly. It is the parasympathetic nervous system that dominates here. The one critical note to emphasize is that the fight or flight response absolutely remains engaged until such time that safety is recognized. Only when the elements necessary to project safety are restored does the mechanism disengage and allows the body to function in the context recognized as normal.
You can see these two opposing nervous system functions readily displayed in lower animal forms wherein the predator and prey roles regularly pose challenge. Observe such animals in this context and you can see a confrontation to threat is typically responded to with a threat of force or actual combat in animals so equipped and in the escape from threat in animals likewise more suited, both with the common goal of survival and ultimate safety. Humans portray these very same characteristics, some more suited to combat and others better suited for escape in order to achieve survival and safety. Humans, however, are far more complex than any other animal form and their advanced brain function greatly broadens their interpretation of their environment. This increased awareness subsequently produces a much broader range in how humans respond in an environment that is far more socialized and complex.

No Cause For Alarm
With regard to benign heart palpitations, the events don’t actually arise as a function of the heart itself, but rather by consequence of access to the heart by the vagus nerve. The vagus nerve, or 10th cranial nerve, is the largest mixed type nerve in the body, innervating many organs including the GI tract, the stomach, spleen, heart, lungs and larynx. During times of stress, nerve activity is generally increased and this is especially true of sensory nerves like the vagus. By example and unrelated to the vagus nerve, take into consideration the manifestation of twitching muscles associated with the eyelid, known as eyelid myokymia. The sensation occurs as a result of inappropriate muscle activity by hyperstimulation of the associated nerve and the condition often arises during times of emotional stress or excessive caffeine use.
Much like eyelid myokymia, the heart can experience inappropriate stimulation by the vagus nerve under similar conditions of significant emotional stress, excessive stimulant use and other factors that produce hyperstimulation. Remember that unlike most other organs, the heart is very much a muscle as well and as such, is vulnerable to responding similarly to the same sort of wayward nerve activity. Consequently, benign heart palpitation events are not an indication of trouble within the heart or its function, but rather more akin to a simple and harmless muscle twitch. Much like a twitching muscle in the eyelid cannot consequently cause blindness, benign heart palpitations are equally incapable of causing heart failure. The paroxysmal beats of palpitations are extra beats and do not replace those of the heart’s own pacers, nor can the presence of chronic palpitations weaken the heart muscle in any manner. Again, it’s more akin to a simple muscle twitch with the caveat that it coincidentally happens to be the heart muscle being affected.
Disturbances of the vagal nerve are also responsible for vasovagal responses, more commonly known as fainting. This is why many people under the strain of significant anxiety can suddenly feel lightheaded or in some instances, actually faint as a result of vasovagal action. Additionally, the vagus nerve also innervates the larynx. Many people experiencing significant anxiety often complain of a sensation in their throat that feels like a blockage or lump, presenting the fear that their airway is becoming compromised or that they cannot get enough air. This is simply a misguided sensation produced by the vagus nerve and no actual compromise of the airway occurs. Many of these manifestations, while entirely harmless and a consequence of stress-induced changes in physiology, are some of the very characterizations that people with health anxiety misconstrue as symptoms of a particular disease or disorder.
Some persons also experience heart palpitations in the presence of intestinal bloating and indigestion, even pregnancy. This arises because the vagus nerve, termed the pneumogastric nerve at the level of the GI tract, is inextricably part of the same nerve reaching the heart. Factors related to compression or disturbance of the nerve can produce wayward evoked potentials, or nerve impulses, which travel along the vagus nerve until reaching the terminal endings, one of which is the heart.
The example above, with respect to benign heart palpitations, is a prime example of how perception can induce imminent fear sufficient enough to engage the brain’s fight or flight response. If the person believes that their heart could fail as a result of the palpitation events, then it constitutes a direct threat to their safety and survival, thus producing the host of physiological changes described earlier. You can see how the onset of fear and subsequent manifestation of physiological changes reinforces the belief that something both dreadful and imminent is about to occur. This is where the complexity of response occurs in humans.


A Life Not Your Own; Health Anxiety Unleashed
It is a known fact that persons who experience heart palpitations and express health anxiety do not stray far from home or put themselves in a position where help cannot be reached. Their social lives are often attenuated because home actually produces some sense of safety and a mild reduction in fear or symptoms. These persons also begin a long an arduous journey to their physician for answers. The problem usually begins to only reinforce their fears because all tests seeking to define a problem with the heart are negative, as they naturally will be because in actuality the heart is fine. It is only the presence of the palpitations that convince the individual that their heart is malfunctioning and as long as the palpitations are present, so is the fear and drive to find safety by determining and treating the cause.
The gradual increase in negative test results is typically regarded by the affected individual as an inability on the part of health professionals to find the problem or that the test itself is too insensitive. Repeated tests or more invasive tests are quite common, again only yielding negative results. It’s important to note here that diagnostic tests such as the ones mentioned are based upon algorithms of actual disease. If the disease is truly not present, the test will only return a negative result. The problem is that a negative finding only increases the anxiety of the affected individual, sometimes even calling into question the competency of their health professional. This is particularly true in instances where health professionals cautiously extend the possibility that the problem is psychological in origin, which most people regard as an insult.
In the later stages of health anxiety, many individuals will sometimes begin to express sentiments of hopelessness. Their symptoms are both real and demonstrating progression, yet cannot be diagnosed and treated. Anxiety is often further elevated, which correspondingly increases the presence of physiological manifestations. Some people have actually quit their job and become reclusive to varying degrees because their unrelenting fear has produced chronic engagement of the fight or flight response, unable to be resolved. They no longer participate in family outings or if they do, find them to be cut short by the expression of, or change in, symptoms. You might well imagine that such a premise results in relative exhaustion, weakness and diminished outlook. Persons at this stage generally feel sick and as though the thriving life they once knew is nothing more than a memory. This is a graphic example of what misperception can do in actually altering the life of someone with heath anxiety.
Some persons begin constantly sweeping the Internet, compelled to read about the broad range of heart disease and associated symptoms that they believe exist within them. In desperation, some folks start taking supplements like magnesium or potassium because others have given online testimonials of success using these products. What they fail to realize is that any changes noted from taking these supplements merely constitutes the placebo effect and true to the nature of such effects, the individuals claiming success are observed making comments in later forums still in search of an answer.

The Yellow Brick Road; A Pathway Back Home
The ultimate goal is for safety to be restored in the minds of these individuals to the extent that the fight or flight response is finally dormant once again. This is true not just in the instance of heart palpitations, but also in any instance where irrational fears have produced a steadfast engagement of the body’s fight or flight response in a manner unwarranted.
The first step in making the transition is to undergo direct evaluation by a primary care doctor or specialist to affirm that the palpitations or other symptoms are benign. If this has already been accomplished, then attention can be turned to addressing the presence of health anxiety from a personal standpoint. Once all warranted tests are negative for the presence of a problem with the heart, the result must be accepted as fact. Such tests are quite sophisticated and leave little to no room for error. Repetitive tests are unnecessary and simply constitute the patient’s compelling need to act on irrational beliefs rather than known facts.
It’s also important to note that many persons attempting to make the reversal in health anxiety summarily introduce ultimatums to offset the difficulty of making such a transition. They often make statements like “If these symptoms will go away, I can do it. It’s the palpitations that caused my anxiety!” It must be recognized that there are no concessions possible and trust must first be unequivocally restored by the person in order for their fears to subside, subsequently followed by the reduction in physiological manifestations, including the palpitations. They must come to trust that the heart palpitations have no capacity to do harm and that they were previously misinterpreted as symptoms associated with heart disease.
The road to recovery can certainly be challenging and a great deal of support is often necessary until a specific comfort level is obtained where positive change is recognized. Ultimately, most people recover from health anxiety of this magnitude and reengage their lives. If you experience health anxiety, it’s important to test it against the rigors of logic before it proceeds to later stages. Persons with significant health anxiety must deliberately steer a course in the direction of identifying errors in thinking and logic rather than seek the most extreme outcomes possible that are so tightly bound to their irrational beliefs.
Of equal importance, the permanent resolution of health anxiety is not available in the immediacy of pill remedies. The problem must be addressed through stepwise changes in thinking patterns that become assimilated into daily life and restore the self-confidence and identity that these individuals once knew and expressed with ease. From a clinical neurology perspective health anxiety is a state of mind, not a disease or mental illness. The ability to recognize this fact and take steps toward self-resolution is paramount.
This article is not intended to supplant the direct evaluation and advice by your primary care physician or specialist and you should always direct questions about your health to your healthcare professional prior to any subsequent exploration on the Internet or other information resource.
References:
1. Jansen, A. S. P., Nguyen, X. V., Karpitskiy, V., Mettenleiter, T. C., & Loewy, A. D. (1995, October 27). “Central command neurons of the sympathetic nervous system: Basis of the fight-or-flight response.” Science, 270, 644 -646.
2. Understanding the association between socioeconomic status and physical health: Do negative emotions play a role? Gallo, Linda C.; Matthews, Karen A. Psychological Bulletin, Vol 129(1), Jan 2003, 10-51
3. Warwick, Hilary M.C. A Cognitive-Behavioral Approach To Hypochondriasis and Health Anxiety. Journal of Psychosomatic Research, Volume 33, Issue 6, 1989, Pages 705-711.
4. Looper KJ. Kirmayer LJ. Hypochondriacal concerns in a community population. Psychol Med. 2001;31:577–584. [PubMed]
5. Barsky AJ. Klerman GL. Overview: hypochondriasis, bodily complaints, and somatic styles. Am J Psychiatry. 1983;140:273–283. [PubMed]
6. Torgersen S. Genetics of somatoform disorders. Arch Gen Psychiatry. 1986;43:502–505. [PubMed]
7. Mechanic D. Social psychologic factors affecting the presentation of bodily complaints. N Engl J Med. 1972;286:1132–1139. [PubMed]
8. Salkovskis PM. Warwick HM. Meaning, misinterpretations, and medicine: a cognitive-behavioral approach to understanding health anxiety and hypochondriasis. In: Starcevic V, Lipsitt DR, editors. Hypochondriasis: modern perspectives on an ancient malady. New York: Oxford University Press; 2001. pp. 202–222.
9. Knudson MP. The natural history of palpitations in a family practice. J Fam Pract 1987;24:357-60. MedlineWeb of Science
10. Zimetbaum P, Josephson ME. Evaluation of patients with palpitations. New Engl J Med 1998;338:1369-73.
11. Giada F, Raviele A. Diagnostic management of patients with palpitations of unknown origin. Ital Heart J 2004;5:581-6. Medline
12. Brugada P, Gursoy S, Brugada J, Andries E. Investigation of palpitations. Lancet 1993;341:1254-8