Why You MUST Get a Second Opinion: How I Learned the Hard Way
Let's Start from the Beginning
In November 2018, I found a lump in my left breast. At 38 years old, I had found odd bodily things before that usually went away on their own. This was different. The alarm going off in my head and gut was so loud and horrifying that I didn't take my usual "wait and see" approach.
Due to my husband starting a job with a new employer the previous April, our new insurance hadn't kicked in until July. We had not yet secured a new primary care provider. Instead, I called the office of the gynecologist I already had an appointment with to see if we could move the appointment up. Sadly, there was no urgency on their part, which was extremely upsetting.
I waited several days before I finally had enough.
My call to the breast center of the hospital where I birthed all three of my children resulted in me being told me I couldn't get a mammogram without a physician referral. I was told "sorry" and "good luck" in the coldest of tones.
My next call was to the second largest hospital in our area in which I was once again told that I needed that referral.
The third call was to a primary care physician I saw four years prior. I found that he was in the new insurance company's network. Repeated calls resulted in no answers because no one was picking up the phone.
The anxiety was eating me from the inside out. I had this urgency that wasn't being satisfied. I made one more call to a Kentucky women's center and they directed me to one of their urgent care facilities. I was told, "They will tell you they can't give you a physician referral, but they will if you are persistent."
The urgent care doctor felt the lump and also worried about my 172/109 blood pressure reading. He knew from what he felt and my mental state that that lump didn't belong and gave me that referral. The next morning, I had a mammogram and an ultrasound.
All Alone In a Room of Heartache
After the mammogram, I was taken to a bright, cold room of breast models and posters. "The radiologist will be in to talk to you in a few minutes," I was told.
But it wasn't the radiologist that entered the room.
A nurse navigator sat down in front of me to tell me that the mammogram result was a BiRADS 5, which means you have only a 3% chance of it NOT being breast cancer. I wasn't surprised considering breast lumps weren't my normal and that lump just didn't belong.
I processed what she told me, despite the fact I was willfully alone at this appointment. She told me I was going to have to have a biopsy that, while it was likely cancer, there was still that tiny possibility it wasn't. The biopsy would tell the tale.
I found out that day that the biopsy was going to be in exactly a week. It's not an exaggeration that that was an excruciating week. Breast cancer in women under 40 is usually very aggressive. The time between the mammogram and the biopsy result that came exactly two weeks later had me begging God to please not take me away from my three small children and my husband. I had no context without any test results, so painful scenarios were going through my brain.
I agonized in prayer because it was just before my diagnosis that I had found myself and my family in such a great place in our lives. We were making new plans with such joy and hope. This was the blow we never saw coming.
Tests, Tests, and More Tests
The blows were mixed with good news. The tests become a way of life for a little while because they are many and frequent. You get blood tests, imaging, tons of people pawing all over your chest, and biopsies.
The breast biopsy wasn't that bad. I was adequately numbed. I also had to have a lymph node biopsied at a later date because it was enlarged.
It was found, based on the breast biopsy results, that the tumor was possibly a purely mucinous carcinoma that had slowly grown over years. It was 2.5 cm x 1.6 cm, over 95% estrogen positive, over 95% progesterone positive (very good), grade 1 (very good), and highly treatable. I didn't feel it until it was large enough to feel because a lot of mucin in a tumor can make it soft.
However, the biopsy didn't conclude if the tumor was purely mucinous or mixed. Purely would mean it was a type of tumor that constitutes only 3% of all breast cancers, which is less than 1% in my age group. I wasn't banking on this due to the rarity, but wondered because of how "soft" the tumor seemed to be.
By this point I started to feel better because the lymph node biopsy came back negative, which meant that there was a significant possibility that the cancer was confined to just the breast. Things were looking up.
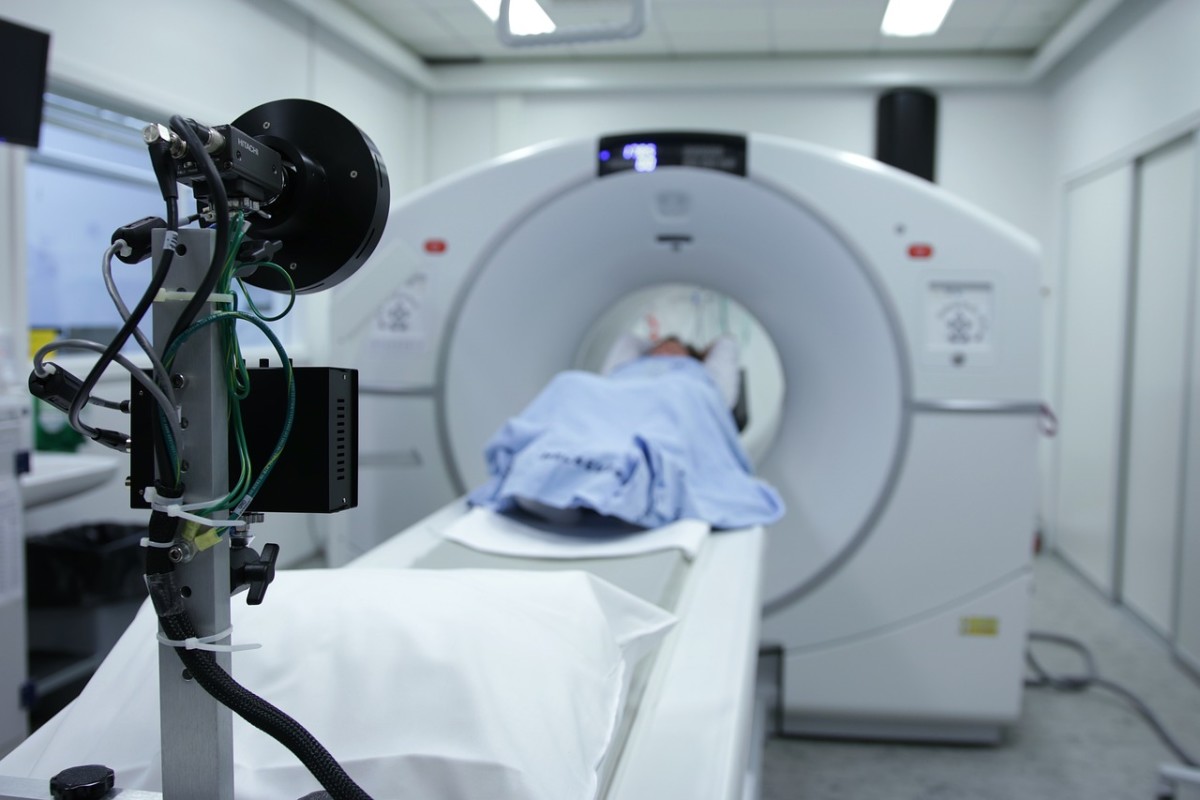
On December 20, 2018, I had a breast MRI. That was the most miserable test of them all. I had to hold completely still with a shoulder injury that I acquired in October from a fall in the mud. It was excruciating!
The next morning, I saw my oncologist and he told me that the MRI results revealed that a lumpectomy would suffice. At 5:30 that afternoon, he called to tell me that the tumor board met after our appointment and reviewed my case. The radiologist was in that meeting and pointed out two lines coming from the tumor that came within 4 mm of my chest wall and the only way to get it all was by mastectomy.
I. Was. Devastated.
With all of my medical professionals on the same page, I didn't question this. I wanted the cancer gone. So far, the urgency was on point and my mastectomy was scheduled for January 24th after I declined immediate reconstruction that would delay the process further. The meeting with the plastic surgeon wasn't promising anyway. I took my best friend with me because my husband had to work. She could tell the plastic surgeon didn't really want to do the reconstruction. Based on the information he had from the MRI report, he didn't think I'd have the chest muscle to support reconstruction. No one needs that type of hesitation over something so sensitive.
Surgery and Its Aftermath
I am grateful for my surgeon. He has a great bedside manner and is thorough, not to mention he's extremely supportive. I was in surgery for 4 to 5 hours and the mastectomy removed the tumor. My lymph nodes looked good as well, so only one was removed for final analysis.
However, my surgeon said that the margins were clear by more than a centimeter. I was relieved to hear this and he was excited about it.
Once the dust settled, I was wondering what happened to that 4 mm from the chest wall that spooked the plastic surgeon so much.
Let's keep in mind here that the 4 mm came from the radiologist that read the MRI and constructed the report. I understand that it's not always exact, but nothing else was ever said about the "lines."
At this time, I was focused on recovering from the surgery. I had to sleep in the recliner for weeks. Once I was able to sleep in my bed, I had to sleep propped up on my back. It was months before I could sleep on my side. Fortunately, I healed well and had no complications.
The Treatment Protocol from Hell - It Doesn't Stop with Surgery
At least things didn't get further complicated until it was treatment time. Should I call it "Hell?" Maybe not because it could have been worse, but it's bad enough.
I didn't have to have chemo because my OncoTypeDx score was a 7. This means the chance of recurrence is low. It's not impossible, but it's not likely it will pop back up as long as I take my meds. I was told that anything below 16 would mean no chemo. I didn't have to have radiation because I had a mastectomy that cleared everything.
That means it should all be over, right?
This is where I want to set the record straight. As much as someone in my case wants it to be over, it never is. Having a mastectomy puts your body off balance. A part of you has been removed in order to save your life. It is a "trade off," but not one you ever want to have to make.
You also have the fear of the cancer coming back, which is why there's a long-term treatment protocol. Breast cancer has the highest probability of recurrence within two years because those cells can be sneaky. Some kind of treatment is put in place for at least five years in case there are any sleeper cells or sneaky ones that weren't seen. This means that the appointments and tests with the different players in your medical team don't end, so the medical bills continue to accumulate. You don't go back to the way things were before cancer, but it's possible to deal with it and restore as much normalcy as possible.
My faith is the cornerstone of my restoration. While fear and faith can't exist in the same space and either one be sincere, measures must be taken to keep the cancer away.
It came to light that the tumor was, in fact, a purely mucinous carcinoma. The odds of that being the type of tumor I had still makes my jaw drop. I took the genetic test and have no deletions or mutations, but estrogen dominance was an issue with me and it was an estrogen fed cancer. It's hard to pinpoint exactly why breast cancer happens in some women and not others, but the medical community has an idea of what some of the contributors are. Estrogen dominance is one of those.
Anyway, my oncologist cited the TEXT and SOFT studies to justify suppressing my ovaries with Lupron and estrogen production in my endocrine system with Exemestane. This involved being thrown into chemical menopause in a matter of about two weeks.
The next thing you know, you're under 40 years old and feeling 80. This treatment protocol also puts bone density at risk.
Something that was difficult for me, especially having three small children and being in a profession that requires my brain to be in tip top condition, was the brain fog. Suddenly, I had to start writing down things I wouldn't normally have to write down. I was forgetting names, events, and losing my sense of self. My enthusiasm for anything started to dwindle.
I was just melting away. It's a feeling I can't adequately describe. When you begin believing that certain things in your life would be better off without you because you're suddenly cognitively impaired, something is terribly wrong. My sense of identity was slipping away and I felt no good to anyone.
To deal with some of the side effects like the joint pain and extreme hot flashes and night sweats, I was put on low dose Effexor. When insomnia started plaguing me, my primary care physician put me on a low dose of Trazodone.
Having to take meds to deal with meds, the brain fog, not feeling like myself, and the side effects that weren't totally done away with proved that it's not over. I was and continue to be as optimistic as possible. However, I can't count how many folks would say the words, "Thank goodness it's over" when it isn't. I just smile and go on while weeping on the inside because telling them would overwhelm them and make them want to run from me. The absence of the tumor doesn't mean the fight ends.
While my breast cancer subtype wasn't the super aggressive kind and I am very grateful for that, it did take my breast. My recurrence percentage stays at its lowest as long as I am in treatment. If I decide I don't want to take my meds, I am at a higher risk. If breast cancer comes back, it happens in the brain, bones, lungs, or liver. We don't want that.
Things Start Getting Weird
So, as the dust settled some more, I had to do physical therapy for my shoulder. The mastectomy aggravated the injury to the point I could barely use my arm. Fortunately, I regained full use of my shoulder and arm thanks to my wonderful therapist. However, I started having a pain under my arm near the mastectomy scar a few months after therapy ended.
An ultrasound was ordered under the arm, but the ultrasound result was quite cryptic.
At my next oncology appointment, my oncologist said I had lymphedema. This confused me since I had only one lymph node removed during my mastectomy surgery. Only one removed means the lymphedema risk is very small. I was sent to the lymphedema specialist who said I didn't have lymphedema.
My oncologist's nurse practitioner ordered another ultrasound, which showed that the lymph node described in the results from two months prior had increased in size to 1.83 cm. It was still non-pathological in size, but it was getting very close to pathological. I repeatedly called for answers, but I was told I would get answers at my next appointment. To me, a lymph node that increased in size by 1/2 cm in two months with pain in the area was a big deal considering I was less than a year out from diagnosis.
After the last, "He'll talk to you at your appointment" that was still almost 6 weeks away at that point, I had enough of being jerked around. I called The James Cancer Center to have my care and everything reviewed by an oncologist that specializes in breast cancer. Part of me felt ridiculous for this because the surgery was done and a treatment protocol was in place that I read was more effective than Tamoxifen alone. However, there was that small voice that said, "do this."
Before my appointment at The James, I had to get my fourth Lupron shot of the year (quarterly shot). Before my shot that day, I got a call from my local cancer center to cancel an appointment for December 9, 2019 with my oncologist. I told the lady on the phone that I was never scheduled for an appointment on that date to my knowledge. She was as confused as I was.
That afternoon when I went to get my shot at the local cancer center, I asked who made the appointment and why. The response was, "What's important is that you see him on the 17th." I told them that I had been trying to get answers about some very cryptic ultrasound results and asked if it had to do with that.
They never answered me.
Now, let me say that I am a good and cooperative patient. Not once had I been a pain in their rears. Did I owe the cancer center money? No. I paid off what I owed them and owed nothing else because the mastectomy, a $53,000 surgery, hit my deductible and out-of-pocket max in January. Did I owe the hospital? Yes. Unfortunately, that bill becomes one that is difficult to pay quickly because it's high. I managed to pay everything owed to the individual providers, but the hospital is a different story. Plus, I was diagnosed at the end of 2018 and didn't meet my deductible before everything reset on January 1. By the end of January 2019, what I owed the hospital more than doubled. I applied for assistance from the hospital system and they declined it, citing my husband alone made too much money. Their payment plans are unreasonable. It's like taking on another house payment.
After the unsettling dialog at my shot appointment, I scratched the oncology appointment for the 17th since my appointment at The James was to be on the 18th. What I did do is see my surgeon on the 17th and told him why I called The James. He gave me his support, which I greatly appreciate. He had a student in the room and echoed the more than 1 cm margins when telling her about my case, which, once again, made questions come to mind.
My surgeon also found an order for a lymph node biopsy that had been sitting for nearly 6 weeks. He said he would order a new one. As of this date, January 4, 2020, the hospital has not scheduled this procedure.
I did, however, go to The James on December 18, 2019 and it was an eye-opening experience.
The James Cancer Center - Things Can Change Fast
My dear best friend who navigated and continues to navigate this journey with me went to this appointment nearly two hours from where we live. My husband had to work, which was fine. He pays for the insurance and my income was seriously impacted this past year because of my diagnosis, so I'm grateful that he has a job that is able to support our family of five.
I was impressed with how smoothly things operate at the Stefanie Spielman Comprehensive Breast Center, which is part of The James, which is part of the Wexner Medical Center. All of this is part of Ohio State University. It's a top 20 cancer center in the country and #28 in the world. If there's an accreditation for it, they have it.
I immediately wished I had started my journey there, but the urgency of the situation made traveling back and forth to Columbus, Ohio seem too daunting and time consuming. I was researching what my local cancer center did to ensure I was getting what I needed and everything checked out.
However, a biopsy order sat for weeks, I kept hearing that the margin was more than 1 cm when I was told it was possible part of my chest muscle would have to be taken, and the rarity of my cancer type had me doubting my treatment protocol despite the studies I read.
I also obtained copies of everything on CDs from the local hospital to take to The James and reviewed them myself. I saw things I had never seen before and even saw that the complaint on one of the ultrasounds was not the exact complaint I made regarding the pain under my arm.
A review of the final report on my surgery
At The James, the breast oncologist's NP sat down with me and reviewed the final report after my surgery in which there was no mention of the lines that forced me into mastectomy. I am seeing a surgical oncologist that specializes in breast surgery on January 22, 2019 to see what is going on under my arm and see what he has to say about the MRI and the "lines" that aren't in any reports except that MRI report. It doesn't change anything, but either something was left behind or the lines didn't actually exist.
An aggressive treatment protocol
I also learned that my treatment protocol was too aggressive. I told the doctor that I was dealing with the side effects because I have to to prevent recurrence. He mentioned brain fog and everything inside me melted because I told him the brain fog is horrific. My doctors at home refused to give me a referral to remove my ovaries so I could stop getting the Lupron shot. Technically, you aren't supposed to get the Lupron shot for more than 12 months in a lifetime because of its toxicity.
The doctor at The James said they don't even give that shot there. When I asked him about removing my ovaries, he informed me that my cancer subtype doesn't warrant the treatment I'm on and, therefore, doesn't justify ovary removal. I told him my oncologist at home cited the TEXT and SOFT studies. The James oncologist said that those studies show that ovarian suppression and endocrine therapy reduce recurrence in more aggressive cases than mine. In purely mucinous cases like mine, Tamoxifen has the same level of effectiveness in preventing recurrence and isn't as harmful.
That day, I was able to halt the exemestane. However, the Lupron will still be in my system for up to 8 months before my body will normalize. The good news is that just removing the exemestane has helped the brain fog. I feel more like myself. When the Lupron leaves my system, my body is in for another harsh transition at 40, but I like the idea of allowing my body to age naturally while working to prevent recurrence.
What Lies Ahead? And Don't Be Afraid of a Second Opinion
Aside from finding out what is causing the pain under my arm, I am excited to have these new, world-class providers that specialize in breast cancer. That is all they do.
In my area, it's likely there haven't been many purely mucinous carcinomas of the breast seen. Of course, the TEXT and SOFT studies are going to seem sensible when choosing a treatment protocol for invasive ductal carcinoma. Unfortunately, Lupron and exemestane had a negative impact on the quality of my life. Lupron is still having that effect, but I'm doing well on the Tamoxifen.
Once I got home from The James, I researched what I was told there and studies showed a 1% to 2% improvement in survival when taking Tamoxifen for purely mucinous carcinoma over ovarian suppression and endocrine therapy. I just wish I could rush the Lupron out of my body.
So while I felt ridiculous for making that call after so much had already happened, I'm glad that I did it. I am now in the hands of people that have dealt with more cases like mine. Had I not made the call, the brain fog would have continued to get worse and I'd be getting that Lupron shot again in March.
Also, there are more reconstruction options at The James than there are at home. I have an upcoming meeting with a reconstructive surgeon so I can restore a little more of what cancer took away. This wouldn't be happening if I hadn't made that call.
When you're gut tells you that you need to do something, do it.