Electro-convulsive therapy (ECT) - the facts and controversies about ECT
What is electro-convulsive therapy?
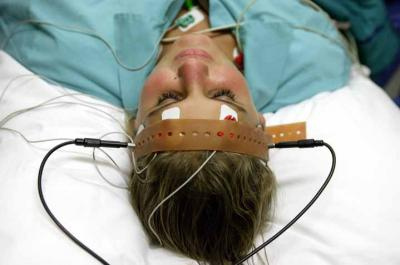
Electro-convulsive therapy (ECT) is a form of psychiatric treatment where electrodes are placed on a person’s temples and electricity is applied to the brain to produce an epileptic fit. The electric current can be applied either to both sides of the brain at the same time (referred to as ‘bilateral administration’) or to just one side of the brain (referred to as ‘unilateral administration’).
Unlike times gone by, the patient receiving ECT is now given a general anaesthetic and a muscle relaxant so that there is much less risk of injury during the fit. The treatment is only given in a hospital environment, almost always while the recipient is a patient on an acute psychiatric in-patient ward.
The number of treatments administered varies from patient to patient, a typical number being eight, delivered over a period of three to four weeks.
Who invented ECT?
Two Italian psychiatrists, Cerletti and Binni, were the first to use ECT on human patients back in the 1940s. At this time, medical experts believed (wrongly, as it turned out) that epilepsy and schizophrenia could not occur together; if you had one it was thought you were immune to the other. Under this misapprehension, Cerletti and Binni developed ECT as a way of triggering epileptic fits in the hope it would ease the symptoms of schizophrenia (that is, voice-hearing and distressing delusional beliefs).
Cerletti and Binni had first got the idea for ECT after observing pigs being stunned by electric shocks in a slaughter-house.
TRUE or FALSE? Electro-convulsive therapy should no longer be offered as a psychiatric treatment.
What sort of mental health problems is ECT for?
There is a troubling discrepancy between the formal guidance describing who might benefit from ECT, and the people who are given it. In the United Kingdom, NICE (the Department of Health body that provides guidance about effective treatments) recommends that use of ECT should only be offered to people with severe depression who have not responded to alternative treatments (medication and psychological therapy), and to those suffering persistent mania or catatonia.
In practice, whether one is given ECT seems to depend as much on a person’s age and gender as it is does on the mental disorder. In the United Kingdom, around two-thirds of recipients are women and, with regards to age, almost half are 65 or over, these skews being mirrored (or more blatant) in most other countries, including the USA.

What do the recipients say?
Patients who have received ECT report mixed experiences. While around one in three people surveyed described ECT as helpful, a similar proportion labelled it a very distressing experience.
Research conducted by Lucy Johnstone, a distinguished British psychologist, interviewed ECT recipients and found that the procedure often evokes an array of negative emotions, including terror, humiliation and a sense of having been abused.
Is ECT effective?
Research into the effectiveness of ECT has led to starkly different conclusions. The Royal College of Psychiatrists (the professional body for psychiatrists in the United Kingdom) claim that ECT is ‘the most effective treatment for severe depression,’ and many psychiatrists believe it can often be life-saying. In contrast, Professor John Read (a clinical psychologist) conducted a recent scholarly review of the literature and concluded that, ‘the cost-benefit analysis of ECT is so poor that its use cannot be scientifically justified.’
ECT is a controversial treatment and much of the research into its effectiveness is sullied by vested interests; some of the American studies have been carried out by doctors who have shares in the companies who produce the ECT machines.
The only research studies that deserve serious consideration are those that compare the effects of ECT with a control group who have received sham ECT (where the patients receive the general anaesthetic but without the electric shock). These investigations have concluded that any benefits from ECT were restricted to a small group of very depressed patients who were physically slowed down. Importantly, any improvements achieved from the procedure did not persist beyond four weeks.
Contrary to the claims of many psychiatrists, there is no evidence that ECT prevents suicide.
Peter Breggin, an outspoken American psychiatrist, suggested that any reported improvements following ECT correspond to the known consequences of brain trauma, namely, superficial emotions, denial and transient euphoria that lasts up to four weeks.
What are the side effects of ECT?
Prior to the introduction of general anaesthetic and muscle relaxant in the 1950s, the fits evoked by ECT were so extreme that fractures of the limbs were commonplace. Although modern-day practice has eliminated perils of this nature, there are other negative consequences linked to ECT, some well established by the research evidence, others more contentious.
Memory loss for recent past events occurs in all recipients of ECT. Impaired ability to learn new information following ECT treatment is also frequently observed. Although both these types of amnesia improve for most patients over time, in some instances memory impairments persist for many years. As one might expect, the more electric shocks a person receives, the more severe and enduring the memory loss.
Disturbingly, many studies have concluded that ECT leads to long term brain damage, particularly when the frequency of administration is three times per week and higher voltages are deployed. Peter Breggin convincingly argues that we should not be surprised that ECT causes permanent brain injury, pointing out that any accidental electric shock to the head of sufficient intensity to induce an epileptic fit would, in everyday life, be treated as a medical emergency. Despite mounting evidence of brain damage, advocates of ECT continue to assert that no enduring problems are associated with the procedure; for example, an ECT fact-sheet produced by the Royal College of Psychiatrists in the UK states that, ‘as far as we know, ECT does not have any long term side effects on your memory or intelligence.’
Some research studies have found that patients who have received ECT die younger, on average, than similarly depressed patients who did not receive ECT. The two most likely explanations for this trend are, firstly, that the emotional consequences of being subjected to ECT increase the likelihood of subsequent suicide - Sylvia Plath’s biographers suggested that her fear of further ECT was a significant factor in her suicide - or, secondly, that repeated electric shocks have a detrimental impact on the body’s physical integrity, perhaps by exacerbating any existing weakness in the heart. In recognition of these concerns, some organisations (ECT Anonymous for example), campaign for the prohibition of ECT.
Some jurisdictions across the world have banned the use of ECT. For example, in 1982, Ted Chabasinski (an American psychiatric survivor who spent much of his childhood in a psychiatric facility where he underwent intensive ECT treatment) successfully campaigned to prohibit the use of ECT in Berkeley, California. Predictably, a group of psychiatrists successfully petitioned to repeal the ban several weeks later.
.

How prevalent is ECT in mental health services?
In the UK the number of patients undergoing ECT has been steadily decreasing since a 1985 peak of around 28,000 people each year. By 1999, the figure was 11,000, reducing further into the new millennium to the present (2013) figure of around 4000. World wide it has been estimated that about 1 million people receive ECT each year.
Psychiatrists’ views on the appropriateness of ECT differ markedly. As a consequence, regions and individual consultants vary hugely in the frequency with which they resort to ECT. A logical conclusion to draw from this variation is that ECT is often given unnecessarily.
Conclusions
Based on a review of the evidence, two central conclusions can be drawn:
- Only a small sub-section of psychiatric patients benefit from ECT and, when they do, these benefits fail to endure beyond a month. Given the modest benefits, together with the associated memory deficits and potential for enduring brain damage, it is reasonable to conclude that ECT should only be considered a treatment of absolute last resort, when all alternative options have been exhausted.
- In light of the real possibility that any benefits of ECT might accrue from the infliction of mild brain damage, the legitimacy of offering ECT as a psychiatric treatment is an ethical question as much as one pertaining to clinical effectiveness
Personal note
In the 1980s, in my role of psychiatric nurse, I witnessed the ECT procedure on multiple occasions. Inflicting a fit-inducing electric shock to a patient’s brain is, in my opinion, a grotesque and degrading process, not unlike an invasive surgical procedure. The crucial difference, however, is that in general surgery there is a clear, specific and logical rationale for the intervention (the removal of an identified tumour, for example). No such underlying brain pathology exists for the patient receiving ECT, rendering its deployment even more difficult to justify, over and above the flimsy evidence base. It is highly likely that, at some point in the future, ECT will be condemned to its rightful place in psychiatry’s closet of shameful treatments, alongside leucotomy, insulin-coma therapy and genital mutilation – see http://gsidley.hubpages.com/_2cfco7m38svhk/hub/Psychiatric-atrocities-the-10-most-shameful-things-doctors-have-done-under-the-guise-of-treating-mental-illness
Further reading
Johnstone, J. (2003). A shocking treatment. The Psychologist, 16(5), 236 – 239.
Read, J. (2004). Electro-convulsive therapy. In J. Read, L.R. Mosher & R.Bentall (eds.) Models of Madness: Psychological, Social and Biological Approaches to Schizophrenia. Routledge.
Read, J. and Bentall, R. (2010). The effectiveness of electro-convulsive therapy: a literature review. Epidemiol Psichiatr Soc 19(4), 333 – 347.