The Duty Imposed upon Hospitals and Nursing Homes to Prevent Patient Falls
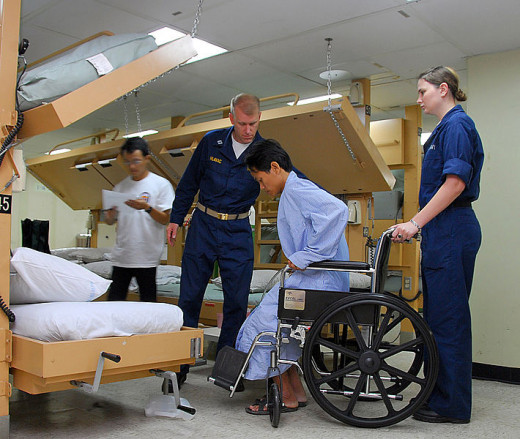
One third of adults aged 65 years or older fall each year. These falls occur in many places including Hospitals and Nursing Homes. Falls among people aged 65 years and above remain the third leading cause of death for this age group in the United States. According to the CDC, 1,800 Nursing Home residents die each year from falls. [1] Many falls also lead to fractures, other serious injuries and debilitation. Most Hospitals and Nursing Homes have fall prevention procedures in place. Despite these measures, a high rate of falls continue to occur in these settings.
The Joint Commission’s Involvement
The Joint Commission is a health care organization that accredits health care facilities in the United States. Accreditation means that a health care facility meets the quality set out by the accrediting board. Accreditation is usually a condition of licensure and receipt of Medicare and Medicaid reimbursement.
The Joint Commission established certain Patient Goals to reduce the incidence of falls in health care facilities. The performance standards for these safety goals are as follows:
- The facility must take steps establish a fall reduction program.
- The program includes an evaluation of the patient fall risks.
- The fall reduction program includes implementation of interventions to reduce he fall risk.
- The program must provide for Staff education and training.
- Patient and family must be educated about the program.
- The facility evaluates the effectiveness of the fall reduction looking at factors such as assessment, intervention and education. [2]
Reportable Events
The Departments of Health in many states require the reporting of any serious preventable events. Serious reportable events are preventable event that lead to death, sprains, fractures, or dislocations that require casting, splinting, pinning or other surgical intervention. [3]
In States such as New Jersey, the report must be made by the hospital to the Department of health within 48 hours of the occurrence. The Hospital must provide the State Department of Health with a root cause analysis of the problem with 45 days of the occurrence. [3]
Many of the falls that occur in hospitals result from patient neglect and are usually among these serious preventable events.
In order to ensure compliance with Quality measures the Joint Commission conducts routine audits of health care facilities. The Joint Commission’s aim is to ensure quality care in health care facilities. Patients with concerns about a facility may first make a report to the facility's management. If the facility management fails to address the concerns, patients have the option of reporting their safety concerns to the State Department of Health and Senior Services as well as to the Joint Commission. If the Joint commission cannot directly address a problem it will forward the concern to the Appropriate Department. The Joint Commission will not reveal your identity without your consent.
The State Department of Health also makes routine Audits of Hospitals and Nursing Homes and will review records to determine areas that affect patient safety.
Patients have been known to voice their concerns during these Audits.
Risk Factors for Falls
Categories
| Quick Areas to Assess
|
|---|---|
Age
| Over 65
|
Mobility
| Unsteady gait, uses cane, wheel chair, walker
|
Vision
| Legally Blind, Needs Glasses
|
Cognition
| Problems with awareness, Lack of Understanding
|
Medications
| Anthypertensives,Duiretics, Nitrates, Anticonvulsants, Sedatives, Opiods, Antidepressants
|
Urinary Patterns
| Frequency, Urgency
|
Diagnoses
| Dementia, Osteoporosis, Parkinson’s disease, Arthritis, Seizure Disorder, Diabetes Mellitus.
|
History of Falls
| Fallen within last 30 days, Fall requiring Hospitalization
|
Fall Assessment Tools used by Hospitals and Nursing Homes that you should know about.
A Patient fall is a significant factor in health care facilities. As such an assessment looking at risk factors must be conducted upon each patient admission. This is in compliance with Joint Commission requirement. A Registered Nurse is responsible for conducting this assessment. Fall assessment must be conducted with the first 24 hours of admission.
Nursing Homes
In Nursing Homes a document called the Minimum Data Set (MDS) is usually used for patient assessment. The Minimum Data set is a federally required clinical tool that is utilized by Nursing homes to assess patients who receive Medicare and Medicaid benefits. The MDS looks at areas such as; cognitive functioning, communication, hearing patterns, vision, physical functioning, continence,affect, behavior, disease diagnosis and ability to engage in activities. A clinician will assess how deficits in these areas may affect patient safety and fall risk.
Based on the MDS assessment, clinicians are then able to formulate an individualized plan of care tailored to the need of each patient. The patient is then given a Resource Utilization Groups score (RUG score). The RUG score is used is measure the cost of labor and resources required to care for each patient. [4] Fall prevention equipment are included in the cost or resources.
Caring for patient safety needs that includes fall prevention is a fundamental part of the MDS and Resource Utilization in Nursing Homes.

Fall Assessment Tools used by Hospitals
Hospitals are required to use an assessment tools to evaluate risk for falls in patients upon admission. Some hospitals utilize a numeral scale. Hospital staff is required to evaluate fall risk by looking at outlined risk categories. A typical tool evaluates; Age, History of Falls, Mobility, Cognition, Visual Impairment, Diagnosis, Medications:
Patients are then given scores within each category. For example, the score range on a fall risk assessment tool may be 0-14. The tool may designate a score of 0-3 as low; 4-8 moderate; 9-14 high. Please note that a low risk does not mean that a patient will not fall.
Patients who have high scores have a high risk for falling. Patients with low scores have a low risk for falling. Some patients fall in the mid rage with a moderate risk for falling. Some tools look at modifiable risks for falling. All disciplines are involved in helping to prevent falls i.e., Physical Therapy, Respiratory Therapy as well as Nursing departments.
The categories may be evaluated as follows:
_______________________________________________________________
Low =0-3, Moderate= 4-8, High =9-14
- Age
- 65-70 (1 Point)
- 71-79 (2 points)
- Age 80 and above (3 points)
2. History of Falls
- Has the patient fallen in the last 30 days? (6 points)
- Has the patient been hospitalized for falls? (5 points)
3. Mobility
- Unsteady Gait (3 points)
- Recent surgery on lower extremities (3 points)
- Amputation (2 points)
- Uses cane, wheel chair, walker
4.Cognition
- Does the patient have altered awareness? (3 points)
- Does the patient lack understanding? (2 points)
5. Visual impairment
- Is the patient legally blind?( 3 points)
- Does the Patient wear glasses? (1 point)
6. Diagnosis
- Does the patient have any of these conditions; Dementia, Osteoporosis, Parkinson’s disease, Arthritis, Seizure Diabetes Mellitus? These diseases are known to place elderly patients at risk for falls. (
- 1 diagnosis (2 points)
- 2 diagnoses (4 points)
- Greater than 2 diagnoses (5 points)
7. Medications. Certain medications may cause certain side effects that predisposes patients to falls:
- Anti-hypertensive medications- Medications used to treat high blood pressure may cause dizziness and weakness. Sometimes getting up suddenly may cause a sudden drop in blood pressure (orthostatic hypotension) causing a patient to pass out. Patients are required to change body positions slowly when on these medications. Examples of Antihypertensive drugs are; Capoten and Aldomet, Aldactone and Cardizem.
- Anti-convulsants Medications- These medications cause problems with balance. Patients on these medications may have seizures if proper blood levels of these medications are no maintained. Some examples of anticonvulsant medications are; Dilantin and Depakote.
- Opiod Analgesic Medications- These medications may cause sleepiness, confusion, cognitive impairment. Examples of Opiod Analgesics are; Vicodin and Percocet.
- Antidepressants- These medications may cause agitation in patients. Examples of Antidepressant drugs are; Prozac, Zoloft and Paxil.
- Diuretics- These medication may cause increased ambulation. Examples of Diuretics are; Lasix, Amiloride and Aldactone.
- Sedatives- These medications may cause drowsiness, dizziness and confusion. Examples of Sedative drugs are; Lorazepam, Klonopin and Ativan.
- Neuroleptics- These medications may cause visual disturbances such as blurred vision. Examples of Neuroleptic drugs are; Haldol, Mellaril and Navane.
- Nitrate and Vasodilators- These medications may cause syncope. Examples of Nitrates and Vasodilators are: Glyceril Trinitrate, Nitopaste and Isordil.
- 1 Medication (2 points)
- 2 medisctions (4 points)
- Greater than 3 medication (6 points)
Patients should learn the names, indications, categories and side effects of medications that they take in order to help ensure their own safety.
8. Urine and Bowel Patterns
- Urinary Frequency (2 points)
- Urgency (3 points)
______________________________________________________________________
Patients may get different fall risk scores based on items listed within the same risk category. For example, in the Age category, a patient may get a score of 1 if she is over age 65. That same patient may get a higher score of 3 in that same category if she is over age 80.
A patient may get a score of 2 for having one diagnosis that predisposes him or her to a fall. However, the score will change significantly to a 11 if that same patient is visually impaired, has one diagnosis that predispose him or her to a fall, as well as taking several different types of medications such as an Antidepressant, an Anticonvulsant and an Antihypertensive drug.
Fall Prevention Measures
Patient and family members should become familiar with fall prevention measures.
Patient at risk for falls should wear a bracelet indicating that they are at risk for falls. Most facilities usually use a yellow bracelet. A sign should be posted above the patient’s bed alerting everyone that the patient is a high risk for falls.
Patients who are a risk for falls should be assessed every hour. Patients who are at heightened risk for falls should be assessed frequently such as every 30 minutes. Ideally a sitter should be at the bedside. The patient should be constantly orientated to time place and person. The side rails of bed should also be elevated. All items needed by patients should be kept at the bedside.
A bed alarm should be put in place. A bed alarm is a device with a sensor pad that will trigger an alarm when there are certain types of patient movements. While the bed alarm itself does not prevent the fall it is a reliable method of putting staff on notice that a patient is moving about. Chair alarms (tab alarms) may also be used in wheel chairs.
Family members can help to ensure that Patients who are at heightened risk for falls are assessed more frequently. For example, if the patient is confused and climbing out of bed then ideally a member of the family should be at the bedside. Patients who need to use the bathroom frequently but have a high risk for falls should be placed on a toileting schedule. They may also benefit by having a family member assist with toileting. In such a situation a commode may also be placed at the bedside. Family also has the ability to assess the environment to ensure that safety measures are being complied with. For example, a busy caregiver may not notice an obstructed pathway or notice spillage on the floor.A caregiver may also walk away and leave the side rails of a bed down.
Family members who are present can quickly address these problems or remind caregivers to address them.
Patients should not be restrained unless they pose a danger to themselves or others. For example, an agitated patient who is attempting to stand and jump from a bed may be treated with a chemical restraint. According to the CDC, in most cases the use of restrains do not reduce falls and may worsen injuries caused by falls. [5]
How to help prevent your own Fall while in a Health Care Facility
There are many things that patients can do in helping to prevent their own falls. For example:
- Do not get out of bed without assistance if you feel weak. Call and ask for help.
- Communicate with staff. Advice staff that medications that you are taking causes mild to adverse side effects such as dizziness or drowsiness.
- Get used to using your call light. Put your call light on whenever you need to get out of bed.
- The hospital and nursing homes usually have non slip socks. Ask for a pair if none was provided to you. If not, ask family to purchase some for you or bring some from home.
- While in bed try to do arm exercises to maintain the strength in your arms.
- If your wear glasses you should put them on prior to getting out of bed.
- Use your controller to lower the height of your bed prior to getting out of bed. Remember that caregivers usually elevate the bed in order to perform procedures.
- Ask for help in getting into a wheel chair at the bedside.
- Do not get out of bed in a poorly lit room.
- Make sure that your wheel chair is locked prior to sitting down. One facility found that after the introduction of self locking wheel chairs the incidence of falls decreased.[6]
Conclusion
Hospitals and Nursing homes are required to take mandatory steps to prevent patient falls. Patients and family members should know the risk factors for falls and stay actively involved in ensuring patient safety.
[1]. Falls in Nursing Home, CDC. Available at:
http://www.cdc.gov/HomeandRecreationalSafety/Falls/nursing.html
[2] National Patient Safety Goals. Available at:
http://www.jointcommission.org/assets/1/6/OME_NPSG_Chapter_2014.pdf
[3] Report of Serious Adverse Preventable Event in New Jersey General Hospital. The New Jersey Department of Helath and Senior services. Available at: http://www.state.nj.us/health/ps/documents/irr.pdf
[4] MDS Quality Indicator and Residence Reports. Available at: http://www.cms.gov/apps/mds/
[5]. Falls in Nursing Home, CDC. Available at:
http://www.cdc.gov/HomeandRecreationalSafety/Falls/nursing.html
[6] Debora Pfeffer. Joint Commission National Patient Safety Goals, 2011. TIPS. Available at: http://www.patientsafety.va.gov/docs/TIPS/TIPS_JanFeb11.pdf