Five Medical Bills You Shouldn’t Pay
If you are puzzled by a medical bill you’ve received in the mail, there may have been some sort of mistake that was made at your expense. It could be due to a lazy employee or an employee who doesn't understand the scope of their position. .
Patients are too often afraid of being sent to collections and/or receiving a negative impact on their credit report if they don’t pay a medical bill immediately. Providers and billing services have the ability to put an account on hold while a patient reviews or disputes a charge. Feel no shame in calling the agency that billed you to request that your account be put on hold while you determine what you are being billed for—you are not asking for a favor by doing this. You are simply substantiating the charges.
Listed below, are the top five erroneous medical bills a patient will receive. Not only have I seen these circumstances, but I have experienced it as a patient.

STUDIES
If you are participating in a study that your physician is part of, you should not be billed for the services—no ifs, ands, or buts about it. If you are being billed while participating in a study, you need to speak with either the office manager or the physician.
There are four phases of a study, ranging from phase I through IV. Depending on what phase the study is in, participants will often receive compensation. In every stage of the study, the manufacturer of the device or drug reimburses the physician for the amount of time spent with a patient and to fill out and submit necessary paperwork.
Patients are often billed for participating in studies that their physician participates in, because whoever is handling the billing doesn’t realize the office visit is related to a study. You should always keep your study records separate from your normal office visit records.

NO PRIOR AUTHORIZATION
This circumstance usually arises during an emergency, in which case you need to appeal the decision, or have the provider appeal the decision for retro-authorization with the insurance company.
If, however, you received the services from a provider you see on a routine basis, this issue needs to be taken up with the provider, and a call needs to be made to your insurance company.
Though provider’s offices will often say it is the patient’s responsibility to verify benefits and obtain authorization, insurance companies understand that patients are laypersons and, most of the time, rely entirely on a provider’s office to handle the administrative aspects of healthcare. You will need to stress to the insurance company that the provider in no way alerted you that authorization would be needed for the services and that you were given the impression you were receiving routine care. The provider’s office will most likely submit an appeal for medical necessity to obtain a retro-authorization for services.
This is something the provider’s office should have done when the denial was received; however, someone in the billing department was either too lazy or didn’t understand the scope of their duties.

NOT MEDICALLY NECESSARY
Usually encompassing the same circumstances as no prior authorization, the same avenue should be taken with correcting this sort of bill.
If the charges are in relation to a surgery or an inpatient claim, and some of the bill was paid by the insurance and some was denied, someone messed up—big time—and, most likely, you should not be responsible for the charges.
For example, though all surgeries, to the patient, seem like a big ordeal, the fact is that some surgeries are extremely simple. It is not unusual for a physician to assist with a surgery if he has nothing better to do on any given day, and he decides to hang out with his surgeon buddy and assist. Insurance companies will not pay for an assistant surgeon if the procedure is considered simple. You should not be responsible for this bill, and you should dispute it with the surgeon. A phone call should be placed to your insurance company if you are unable to remove the charges from your account.
With inpatient claims, hospitals employ nurses in charge of utilization review and coordination of care and benefits. It is that person’s job to notify the insurance company on a daily basis of your condition and not the ill patient’s responsibility. If there are denied days, the hospital needs to submit an appeal based on medical necessity. If the hospital is billing you for denied days, a phone call should be made to the insurance company in order to determine if the hospital is allowed to bill you. If you have insurance through an employer, sometimes enlisting the aid of the Human Resources Department proves to be an extremely useful tool in arguing with an insurance company to approve the denied days.
Lastly, sometimes providers will “upgrade” care or an item. For example, if you are receiving an orthotic device or some sort of durable medical equipment and it has some fancy features, it may not be covered by your insurance company. If the item supplied had been without the fancy features, it might have been covered. Patients are usually able to decide whether to pay for the additional features by paying out-of-pocket for the upgrade or inform the provider they don’t want the extra features. You might need to make a phone call to your insurance company if your provider’s office did not explain this to you and is unwilling to exchange an item.
If the charges are for a service that can’t be returned, a call should be made to the insurance company. Explain that you were not informed by your provider that the service would not be covered and that you were under the impression you were receiving routine care.
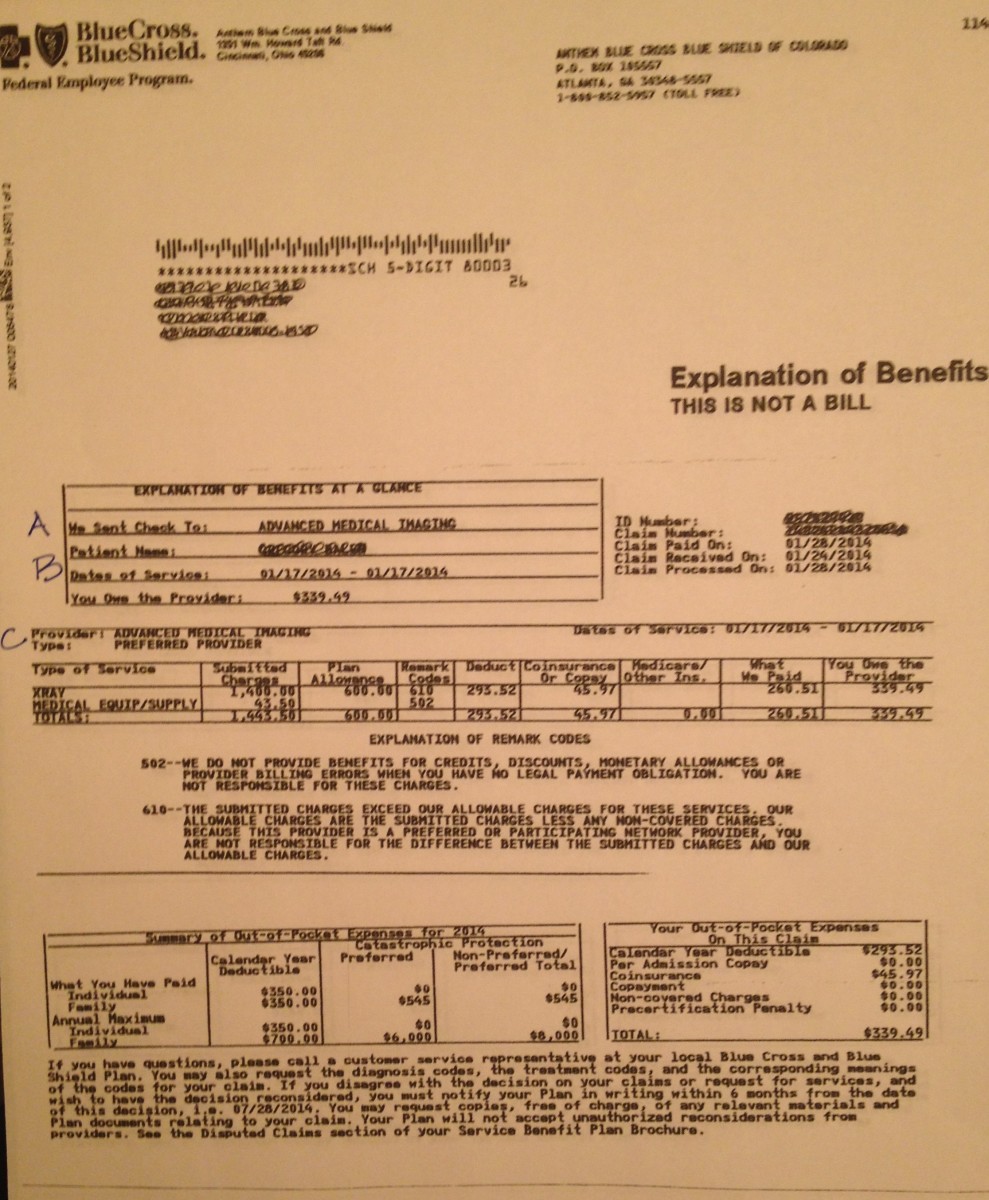
CONTRACTUAL ADJUSTMENTS
If your provider is a preferred provider with your insurance company, you should not be receiving a bill for the balance remaining on a service after the insurance company has paid the claim, unless it is for a copayment or coinsurance. You will need to refer to your insurance company’s explanation of benefits to determine if you are being billed for contractual adjustments.
TIMELY FILING DENIALS
I saved the best for last, because it is so common. Did you receive a medical bill out of the blue? Is the service date a year or older? If so, this is probably because the provider didn’t submit the bill to the insurance company. Insurance companies have timely filing requirements, and if the bill was not submitted in a timely manner, the bill is denied. Often, providers will attempt to bill the patient, and these are charges that must be eaten by the provider.
You most likely signed a form with your provider that indicates a courtesy is being performed when they submit your bill. This doesn’t hold water when it comes to timely filing requirements (and often won’t hold water in relation to any sort of denial—they just hope you believe it). The form indicates that they are performing a courtesy, and at no time did they inform you that they will not perform the courtesy.
If a provider is billing you for an old service that has been denied by your insurance company for timely filing, don’t bother placing a phone call to the provider. Bypass the provider’s office, and place a phone call to the insurance company. If the person you speak with is not helpful, speak with a different representative or a supervisor. The insurance company will either hold a conference call with you and the provider, or agree to call you back once the issue is resolved.
Related Hub
- Does Your Doctor Overcharge You?
Not all doctor visits require co-payments, yet some physicians offices will routinely collect them, resulting in a credit balance on an account. Often, people enter a physicians office and immediately...
PHOTOGRAPHY
- Error on Flickr - Photo Sharing!
- Jon sleeps at work. on Flickr - Photo Sharing!
Jon sleeps at work. - Beach wheelchair on Flickr - Photo Sharing!
Wheelchair with fat tyres for use on the beach.