immunosuppressive drugs, impaired immune system, increased infection risk - Autoimmune diseases
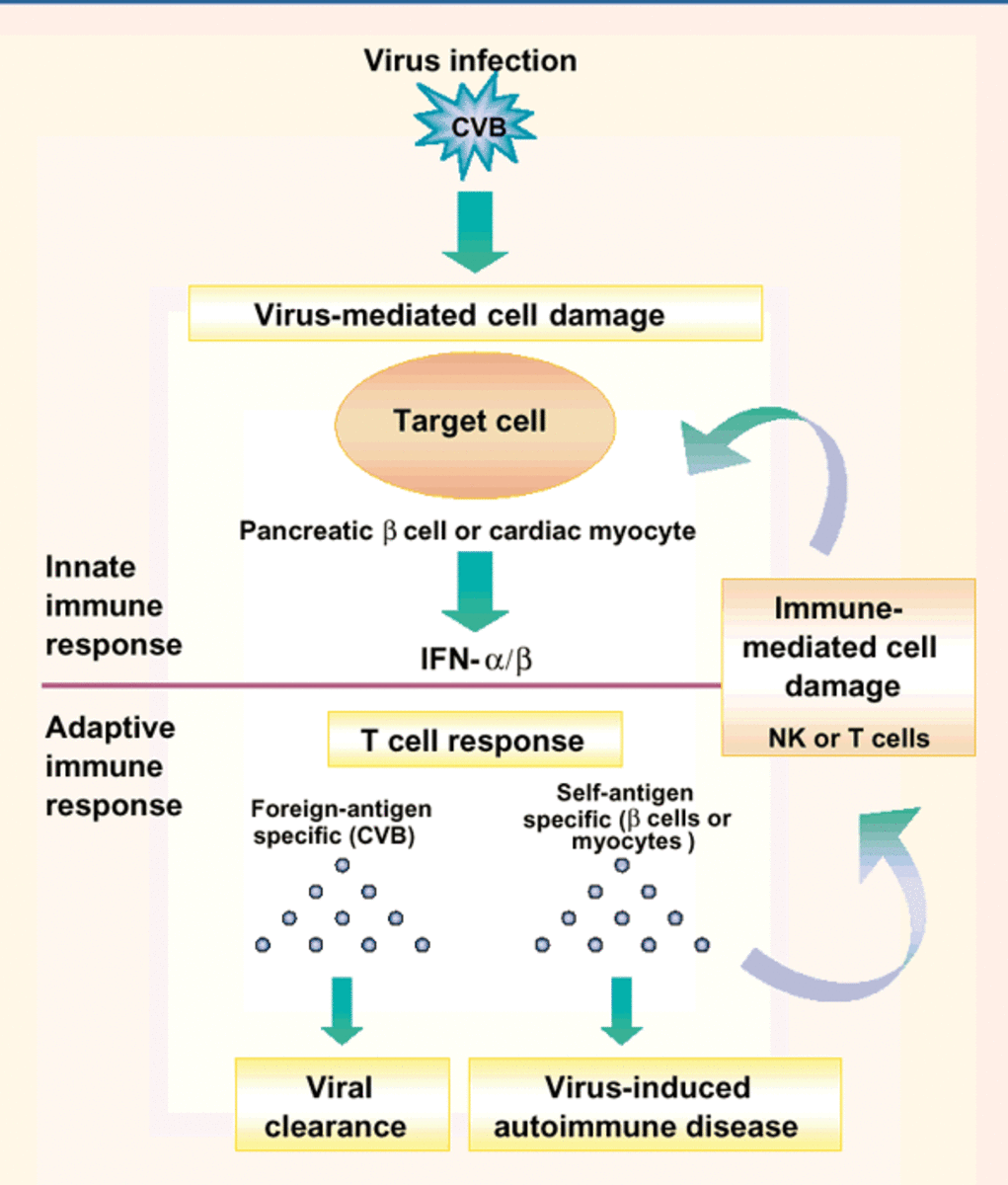
Soon after autoimmune diseases were first recognized more than a century ago, it was believed that their development was associated with viral and bacterial infections such as Mycobacterium tuberculosis complex. The connection between infection and autoimmune disease is often explained by a mechanism known as “molecular mimicry,” whereby microbial antigens are postulated to resemble self-antigens. The induction of an immune response to the microbial antigens results in a cross-reaction with the self-antigens and the induction of autoimmunity.
The main function of the immune system is to protect the host against invasive microorganisms bacteria, fungi, parasites and viruses, and to maintain the homeostasis and a surveillance control. Immune responses can be classified roughly as innate (natural and nonspecific) and acquired (adaptive) responses, in which the reaction is directed to a specific determinant (antigenic determinant or epitope).

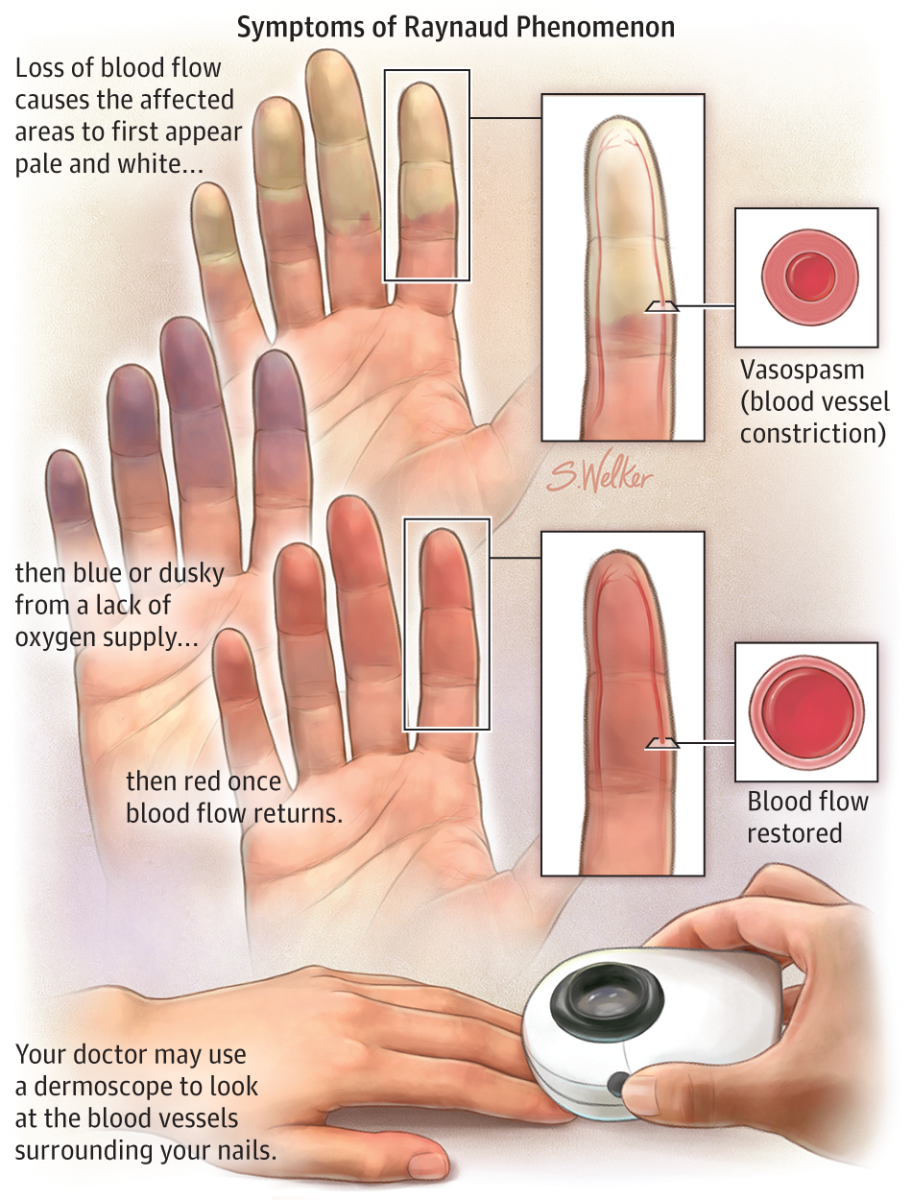
The specific type of autoimmune disease that develops depends on the predominant location of the inflammation. When inflammation occurs in a joint, rheumatoid arthritis can develop; in the brain, chronic fatigue syndrome (myalgic encephalomyelitis) may be the result; in the blood vessels, vasculitis may be the resulting condition; within the gums, periodontal disease can result; or in the lungs, asthma may be triggered. If the antibodies attack the lining of the gut itself, the result may be irritable bowel syndrome, ulcerative colitis, or Crohn’s disease. If the bacteria that causes gingivitis enter the bloodstream and attack the arterial walls, causing inflammation and cholesterol deposition, heart disease and stroke may ensue.
The severity and the frequency of these complications are linked to the mechanism and the strength of the immunosuppression provoked by the drug agent.
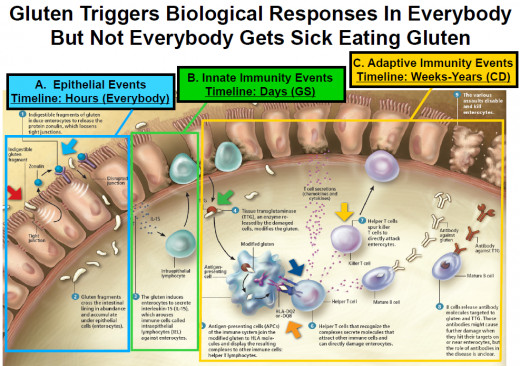
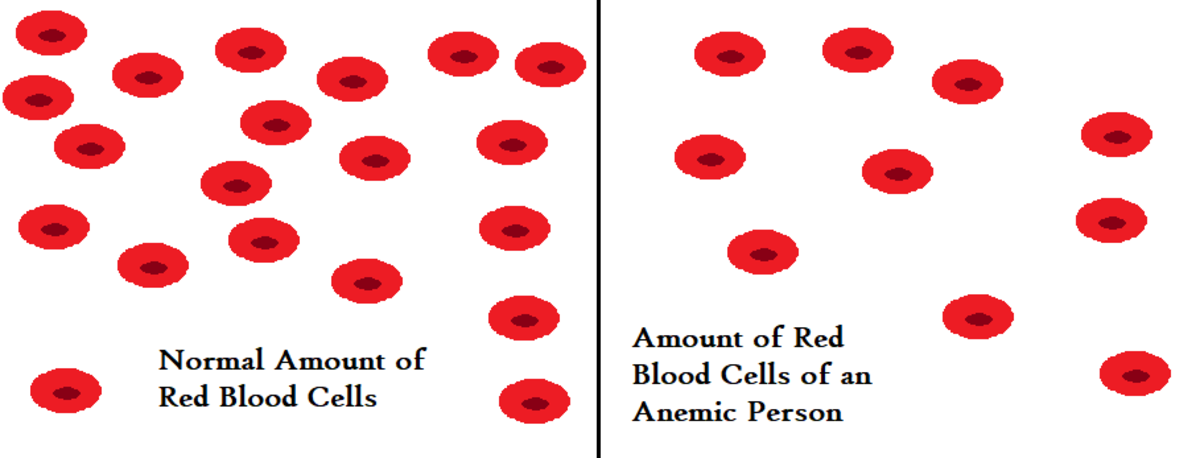
Studies, conducted at Townsville Hospital in Queensland, Australia, found that having type 2 diabetes as an adult makes one seven times more likely to develop tuberculosis (TB). This is more likely caused by an impaired immune system.
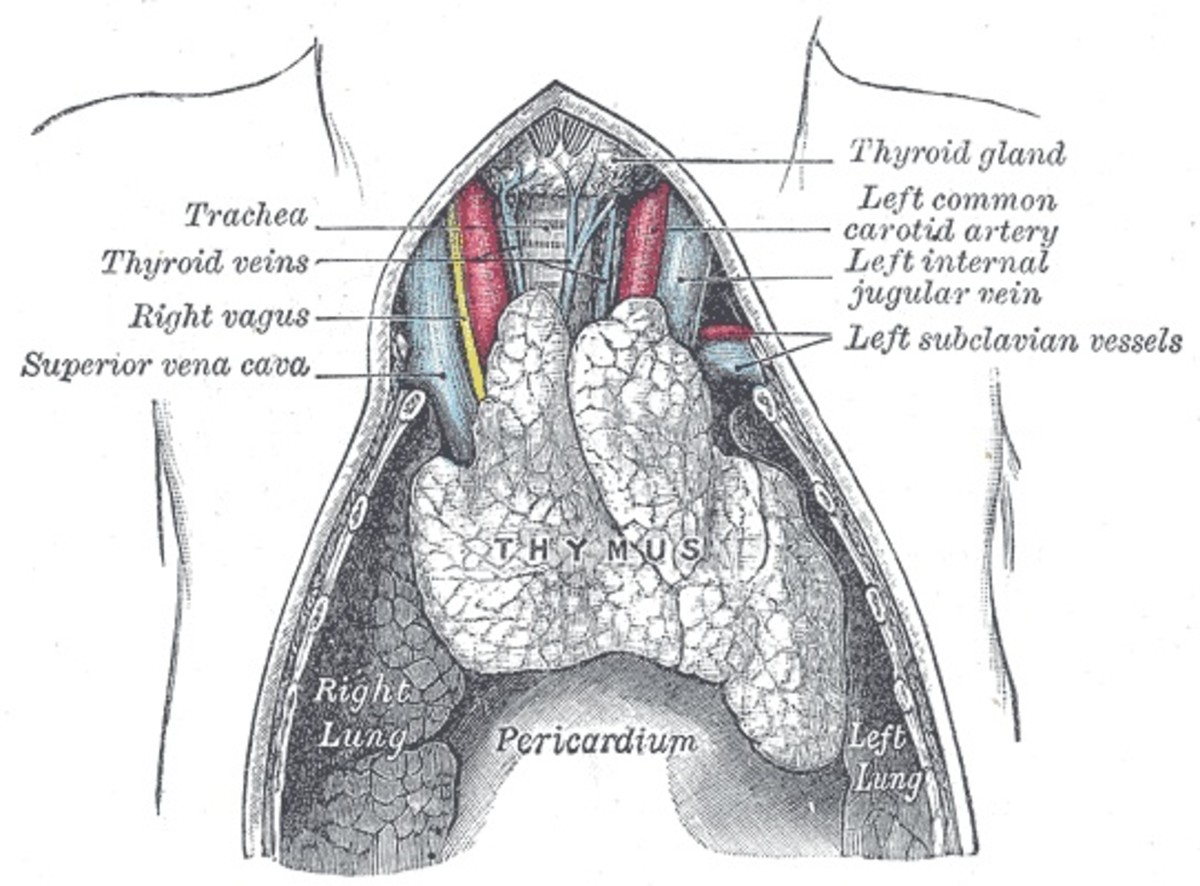
M. tuberculosis and other mycobacteria complex are intracellular pathogens that grow primarily in the phagosomes of macrophages, shielded from the effects of both antibodies and cytotoxic T cells. Peptides derived from such microorganisms can be displayed on the macrophage surface by MHC class II molecules. When these peptide:MHC complexes are recognized by the T-cell receptor of antigen-specific effector THl cells, the T cell is stimulated to synthesize membrane-associated proteins and soluble cytokines that stimulate the macrophage and enable it to eliminate the pathogen. This boost to antimicrobial mechanisms is known as macrophage activation. THl cells similarly activate macrophages to increase the destruction of recently ingested pathogens. This coordination between THl cells and macrophages underlies the formation of the immunological reaction called the granuloma, in which microbes are held in check within a central area of macrophages surrounded by activated lymphocytes.
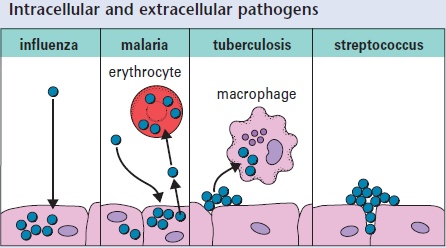
All infectious agents spread to infect new cells by passing through the body fluids or tissues. Many are intracellular pathogens and must infect cells of the body to divide and reproduce (e.g. viruses such as influenza viruses and malaria, which has two separate phases of division, either in cells of the liver or in erythrocytes). The mycobacteria that cause tuberculosis can divide outside cells or within macrophages. Some bacteria (e.g. streptococci, which produce sore throats and wound infections) generally divide outside cells and are therefore extracellular pathogens.
The two other species currently in the complex, Mycobacterium microti and Mycobacterium pinnipedii are almost exclusively associated with different mammalian hosts, but a few cases have been reported in immunocompromised patients such as those with HIV, AIDS and immunodeficiency syndrome.
The combination of abatacept and TNF-á blocking agents resulted in more mycobacterium complex infections and more serious infections than were seen with abatacept alone. As a result the FDA has required the prescribing information for these agents to include warnings to avoid combinations of two or these agents or concurrent therapy with other immunosuppressive agents.
Abatacept is a “biologic drug” manufactured by Orencia
Abatacept is sometimes called a “biologic drug”. The brand name is Orencia®. It is given to decrease pain and swelling and slow the progress of RA. Abatacept is in a class of medications called „selective costimulation modulators‟ which block the activity of T-cells. When T-cells are active, they signal other cells to cause inflammation around the infectef joint damage. Abatacept blocks this activity, which reduces the signs and symptoms of rheumatoid arthritis. It is usually prescribed when other DMARDs (disease modifying anti-rheumatic drugs) or other biologics do not work well, but it can be expensive.
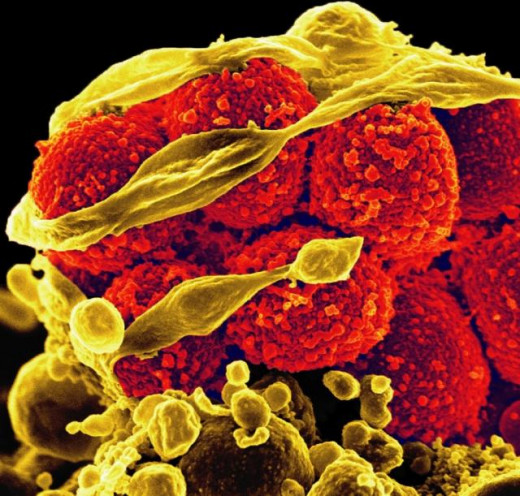
immunosuppressive drugs are used against the regulation of lymphocyte (T cells) activation and growth. TB Infection risk is increased on long term use of immune suppression drugs.
List of other immunosuppressive drugs.
Mycophenolate Mofetil; Cellsept®
Sargramostim; Leukine, Leukomax.
Tacrolimus; Prograf®
Zidovudine; Retrovir®, AZT, Hivid.
Saquinavir; Fortovase®, Invirase.
prednisone; Orasone.
azathioprine; Imuran.
cyclosporine; Sandimmune, Neoral.
Basiliximab.
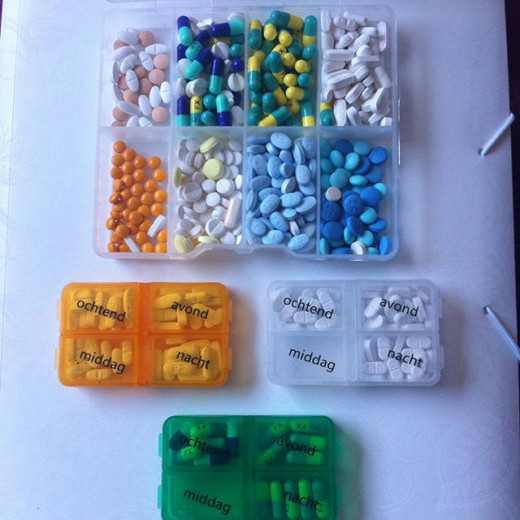
Inactive ingredients in Mycophenolate Mofetil CellCept 500 mg tablets and Oral Suspension capsules include black iron oxide, croscarmellose sodium, FD&C blue aluminum lake, hydroxypropyl cellulose, hydroxypropyl methylcellulose, magnesium stearate, microcrystalline cellulose, polyethylene glycol 400, povidone (K-90), red iron oxide, talc, and titanium dioxide; may also contain ammonium hydroxide, ethyl alcohol, methyl alcohol, n-butyl alcohol, propylene glycol, aspartame, citric acid anhydrous, colloidal silicon dioxide, methylparaben, mixed fruit flavor, sodium citrate dihydrate, sorbitol, soybean lecithin, xanthan gum and shellac.
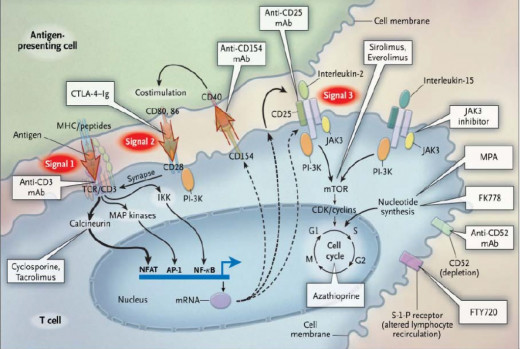
Although the knowledge of key molecular events underlying immune cell activation has advanced enormously in recent years, there still is short of a complete understanding of the sequence of events between antigen recognition, lymphocyte activation and cell proliferation. The most recent developments concerning the actions of new immunosuppressive drugs have however, shed light on several biochemical events crucial for immune system impairment.
One major precaution for those with autoimmune disease as these compounds can stimulate an already overactive immune system and make the condition worse. It is best to first detoxificate the body. The immune system is an amazing, versatile and complex system which will protect your body from any disease if you treat your body well and give it natural nutritional food at the right time and the right quantity.