Juvenile idiopathic arthritis
What is Juvenile Arthritis?
Juvenile arthritis is a condition that is characterized by pain, swelling and heat in one or more joints. It may affect only a few joints or it may affect many joints. As the name suggests, juvenile arthritis affects young people. Symptoms may present for the first time anywhere between the age of six months and 16 years. To be classed as juvenile arthritis, symptoms must last longer than 6 weeks.
The condition is not particularly common. Research indicates that around 1 in 1000 children have the condition. However, the condition is common enough that any child presenting with possible symptoms of juvenile arthritis should be investigated by an appropriate health professional. This article will explain the condition, how it is diagnosed, treatment options and prognosis.

Juvenile idiopathic arthritis or juvenile rheumatoid arthritis
The most common type of juvenile arthritis is called juvenile idiopathic arthritis. This is also referred to as juvenile rheumatoid arthritis. These two terms generally refer to the same condition. However, juvenile arthritis should not be confused with adult rheumatoid arthritis. Adult rheumatoid arthritis is a different condition.
Juvenile arthritis is considered an autoimmune condition. The body's immune system fails to identify some of the body's own tissues in or around the joint. The immune system then begins to attack them. In other words, the body attacks itself in the same way that it would attack invading bacteria or viruses. This ongoing attack on the joint tissues results in pain, swelling and heat in the affected joints.
Deals from Amazon
Pediatric rheumatologist discusses juvenile arthritis
What is the cause of juvenile idiopathic arthritis?
The precise cause of juvenile arthritis condition is generally unknown. It is likely that a complex mix of genetic and non-genetic factors contribute to whether someone develops the condition. In addition to genetic traits, other factors contributing to juvenile arthritis may be related to infection, environment, trauma, hormonal abnormalities and psychological stresses.
Clinical research has allowed us to understand the autoimmune nature of the condition. However, the reason why this occurs in some people but not others (or even in some joints but not others) remains unclear. It is believed that in some cases the condition may be first triggered by an invading pathogen (such as a bacteria or virus).
Deborah talks about living with juvenile arthritis
How is juvenile arthritis diagnosed?
The condition is usually diagnosed based on information from a number of sources including. This information includes:
1. Detailed history
2. Physical examination
3. Lab tests (such as blood tests)
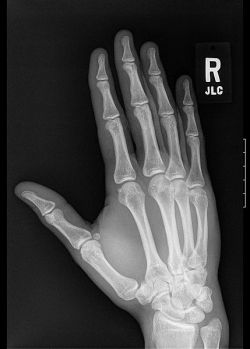
4. Imaging (such as x-rays or more complex radiological investigations)
Signs and symptoms present in juvenile idiopathic arthritis may include (but are not limited to):
1. Joint pain and swelling
2. Heat in the joints
3. Changes in walking pattern (gait)
4. Reduced range of joint motion (in affected joints)
5. Weight loss
6. Fatigue
7. Inflammation in the colored part of the eye (the iris)
Laura, talk about living with her sister's juvenile arthritis
How is juvenile arthritis classified?
Juvenile arthritis can be classified into three very broad categories. These broad categories include Oligoarticular, Polyarticular and Systemic juvenile idiopathic arthritis.
1. Oligoarticular category includes arthritis with symptoms in four or less joints.
2. Polyarticular category includes arthritis with symptoms in five or more joints.
3. The systemic category is used when the condition affects the whole body. It is not uncommon for children with systemic juvenile arthritis to develop high grade fevers, develop a rash or look very pale and feel generally ill.
More than 90% of juvenile arthritis cases can be classified into one of the three broad categories above. However, the International League of Associations for Rheumatology uses a more technical classification system. This system includes seven subtypes. These categories include:
1. Oligoarticular
2. Polyarticular rheumatoid factor positive
3. Polyarticular rheumatoid factor negative
4. Systemic
5. Psoriatic
6. Enthesis Related Arthritis and
7. Undifferentiated arthritis.
It is noteworthy that categories five to seven tend to account for less than 10% of juvenile arthritis cases.
What is the treatment for juvenile arthritis?
Treatment for juvenile arthritis usually involves a number of health professionals as well as medications. Health professionals involved in treatment may include doctors, physical therapists, occupational therapists, dietitians, psychologists, podiatrists and possibly others. The general aim of therapies is to help reduce pain, strengthen muscles, keep the joints moving and promote normal development.
There are several types of medications used to treat juvenile arthritis. The medications prescribed for each person will depend on the nature, severity and duration of symptoms. A combination of analgesics, anti-inflammatory drugs (both steroidal and non-steroidal) and disease modifying anti-rheumatoid drugs (DMARDs) are common. Analgesics and steroids can relieve symptoms but do not alter the disease. Disease modifying anti-rheumatoid drugs (DMARDs) alter the underlying autoimmune response.
A range of negative side effects are associated with some medications used to treat juvenile arthritis. The benefits and side effects of each medication will need to be considered on an individual basis. Not all people will experience the same level of benefit or side effects for each possible medication.
What is the prognosis for children with juvenile arthritis?
Children with many joints involved or a positive rheumatoid factor (detected with a blood test) are more likely to have ongoing symptoms. Children with fewer joints involved are generally considered to have a better prognosis. Many people with juvenile arthritis eventually go into remission.