- HubPages»
- Health»
- Mental Health»
- Clinical Depression
Omega-3 consumption in the treatment of depression.
Depression and nutrition.
ABSTRACT –
The purpose of this critical review is to analyze the effects of omega-3 in individuals who have diagnosed depression. The experiments being reviewed show the effect of omega-3 in depressed individuals using randomized control trials, placebo-control groups, and elimination of confounders where possible and large sample sizes. Overall, results varied but there was no evidence for a deterioration of depressive symptoms with omega-3. There is evidence of improvement in depressive symptoms but this based on a small number of well-controlled studies. There were a number of studies that provided supporting evidence but they had small numbers, were poorly controlled or were individual case studies. So far there is no reason to say that omega-3 is harmful but further research is needed with regards to the hypothesis that omega-3 will reduce symptoms of depression.
BACKGROUND -
Omega-3 in particular docosahexaenoic acid (DHA) and arachidonic acid (AA) make up 25% of the total fatty acid content in the brain and therefore are crucial for the anatomical structure of the central nervous system [12]. Adequate DHA intake has been shown to improve cognition and behavior in children [13]. One study showed that a dietary DHA supply positively affects performance on the “Bayley mental development index” in 12 month olds [14]. DHA and AA are produced from alpha-linolenic acid but cannot be synthesized within the body and must be obtained from external sources such as white fish, shellfish and fatty fish [9].
Several studies show a significant reduction in the Omega- 3 levels of depressed individuals compared with matched controls [7]. The brain is selfish when it comes to ingested fuel and utilizes a disproportionately large fraction of our food intake. It is therefore a reasonable hypothesis that nutrition contributes to the quality of mental health in an individual [1]. The world health organization has estimated that depression is the leading disability worldwide [2]. The disease is characterized by feelings of worthlessness, change in weight and appetite, suicidal thoughts, disturbed sleep, increased anxiety and mental and physical slowing [9]. Depressive symptoms need to be apparent for at least consecutive two-week period prior to diagnosis [9]. Instances of depression show similar rates to that of coronary artery disease [2].
Fish and seafood are the highest source of dietary omega-3 polyunsaturated fatty acids [3] and in the studies cited below supplementation with omega-3 showed improvement in individuals with depressive symptoms [2-8]. This report will explore the effects of omega-3 consumption on depression. The conclusion will take into account the nature of these studies in a critical fashion, underlining the key findings and highlighting likely causes of error.
REVIEW OF EVIDENCE -
Appleton et al. reviewed 20 randomized trials on the effects of Omega-3 essential fatty acids on depressive scores in over 1000 individuals. Each of the studies had placebo-controlled groups. Appleton et al. concluded that placebo results were not significantly different to supplemented groups. Subsequently there was not enough evidence to determine if the decrease in depressive symptoms were due solely to Omega-3 and stated that further research be conducted [9].
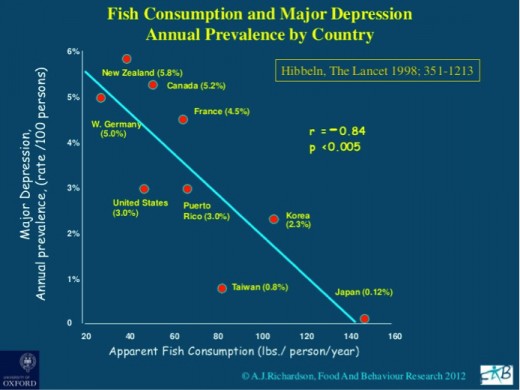
A cross-national comparative study was conducted by Hibbeln to test the hypothesis that high fish consumption could be correlated with lower rates of major depression. The studies create confidence as they used a large sample size, random prospective design, repeat sampling and multiple communities sampling. The data on fish consumption was calculated by fish catch plus imports minus exports. The core biological symptoms of depression were measured to determine prevalence’s. The results of this trial are displayed in a linear regression line below [2].
Figure.1 Fish consumption and prevalence of major depression
The correlational regression model produces a Pearson’s value of r=-0.84 which indicates a potential dependence between the two variables.
(Image source: http://www.slideshare.net/TheAdlerSchool/the-importance-of-nutrition-for-mental-health-dr-alex-richardson)
In another journal, Tanskanen et al. reported that patients with diagnosed depression have shown depleted levels of omega-3 polyunsaturated fatty acids in plasma or cell membranes. They reported the findings of a double-blind placebo-controlled experiment, which showed an improvement in bipolar patients in their depressive symptoms with omega-3 supplementation.
Tanskanen et al. performed their own randomized clinical trial using a sample of subjects from Kuopio, Finland (N=3004) between the ages of 25 to 64. Depression was measured using the 21-item Beck Depression Inventory and a person was considered depressed if the BDI score was greater than or equal to 10. Fish consumption was then measured using a questionnaire and high frequency was said to be twice a week or more. The results showed that suicidal thoughts were significantly lower in those who had high fish intake frequencies compared to those who had low intake. The study took into account confounding variables such as general health, smoking, alcohol intake, physical activity, sex, age, financial status etc. Tanskanen et al. referred to the polyunsaturated fatty acids as “mood stabilizers”, but declared a need for further large-scale trials in this area [4].
Nemets at al. performed a randomized control trial using 20 (17 women and 3 men) patients who had been diagnosed with depressive disorder using the 24-item Hamilton Depression Rating Scale that were rated >18. The study ruled out any individuals who had additional unstable medical diseases, mania, psychotic features, alcohol and drug abuse, obsessive-compulsive disorder, panic disorder or any other combined psychiatric diagnosis.
Patients were between the ages of 18-75 and diagnosed with depression after multiple sessions with a psychiatrist. Blood chemistry was analyzed of each individual at the commencement of the experiment and they were then each assigned into a fish oil or placebo group.
All patients, bar one, were already undergoing medical treatment using antidepressants (for >3months) yet the chosen participants still displayed episodes of depressive disorder. The experiment was over the course of four weeks using a double-blind procedure and parallel groups (one given fish oil and one given placebo). Patients continued taking their anti-depressant treatment at the same dose they had been on for at least 3 weeks prior to the experiment. The fish oil groups were administered two grams of eicosapentaenoic acid (EPA) daily. One patient had to withdraw by week three as she said her symptoms had become worse (she was in the placebo group). The results showed a significant difference between the two groups at week’s 2, 3 and 4 on the Newman-Kuels post hoc test with a p value of <0.001. Results were measured using each individuals Hamilton depressive score at the conclusion of the study. Six of the ten patients receiving the EPA treatment showed 50% reduction in their score whereas the placebo group (excluding the individual who withdrew) only one in ten showed a 50% reduction in their Hamilton depressive score. These results were clinically meaningful [5].
Puri et al. performed a study, which treated one man with a seven-year history of severely depressive, and suicidal symptoms. The omega-3 fatty acid EPA was added to his current anti-depressant. After one month of the EPA addition the patient displayed a significant change in suicidal behavior and social phobia. Registered difference images showed that the EPA was accompanied by an effect on his brain structure with a reduction in the lateral ventricular volume [6].
Khajehnasiri et al. performed a randomized, double-blinded, placebo-controlled trial on 136 depressed men in the Tehran Shahid Tondgoyan Oil Refinary. These men had a Beck Depression Inventory (BDI) score of 10 or more. The study consisted of four groups with one taking a combination of omega-3 and vitamin c, one taking a placebo, one taking just vitamin C and one with only omega-3. This trial went for two months. The results showed a significant reduction in BDI scores in all four groups. However, the largest decrease in BDI score was in the omega-3 fatty acid supplementation (alone) with a mean score decrease of 6.29 (p <0.001) [8].
CONCLUSIONS -
Appleton et al. found that in their review of 20 trials omega-3 did reduce depressive symptoms but there was not a significant difference between the placebo-control and omega-3 group. Hence, they could not conclude that the improvement in the depressed individuals was due exclusively to omega-3. However, it cannot be said that omega-3 is not the cause for these improvements [9].
Hebbeln’s method for fish consumption in the cross-national experiment is not a direct measure of cause and effect as it leaves room for many other confounding variables. Additionally, this study does not show if there is an improvement in depressive symptoms in comparison to a previous time period. Therefore it cannot be concluded that higher fish consumption prevents or alleviates depressive symptoms and further research is needed [2].
The trial Tanskanen et al. conducted only used participants from one country. This could mean all individuals from Finland experienced a confounding variable that improved health. However, depressive disorder was only improved in omega-3 supplemented individuals [4]. Nemets et al. used 17 women and 3 men for their experiment. Consequently, gender may have impacted the results [5]. Puri et al. conducted an experimental trial based on the results of one individual. Regardless of the significant impact omega-3 seemingly had on the individual there is no baseline to measure the outcome against aside from personal history [6]. Khajehnasiri et al. displayed some very significant results. However, the trial was only inclusive of men [8].
In summary, there was no trial where omega-3 made depressive symptoms worse. Considering, there are experimental examples of significant benefits from omega-3 in depressed individuals I am able to support the theory that administering a high fish diet (rich in omega-3) could alleviate depressive symptoms in an individual. For future research I would recommend well controlled, long-term and large scale studies using consistent measures of depression.
References:
REFERENCES –
- 1. Beyer JL, Payne ME. Nutrition and Bipolar Depression. Psychiatr Clin N Am. 2016;39:75-86. Pubmed DOI: 10.1016/j.psc.2015.10.003
- 2. Hibblen JR. Fish consumption and major depression. The Lancet. 1998;351:1213 Pubmed
- 3. Tanskanen A, Hibbeln JR, Tuomilehto J, Uutela A, Haukkala A, Vinamaki H, et al. Fish consumption and depressive symptoms in the general population in Finland. Psychairicsermces. 2001;53:529-531
- 4. Tanskanen A, Hibbeln JR, Hintikka J, Haatainen K, Honkalampi K, Viinamaki H. Fish consumption, depression, and suicidality in a general population. Arch Gen Psychiatry. 2001;58(5):512-513
- 5. Nemets B, Stahl Z, Belmaker RH. Addition of omega-3 fatty acid to maintenance medication treatment for recurrent unipolar depressive disorder. Am J Psychiatry. 2002;159:477-479
- 6. Puri BK, Counsell SJ, Hamilton G, Richardson AJ, Horrobin DF. Eicosapentaenoic acid in treatment-resistant depression associated with symptom remission, structural brain changes and reduced neuronal phospholipid turnover. Int J Clin Pract. 2001;55(8):560-563
- 7. Puri BK. Cardiovascular disease and depression: the pufa connection. Int J Clin Pract. 2008;62:353-366
- 8. Khajehnasiri F, Akhondzadeh S, Mortazavi SB, Allemeh A, Sotoudeh G Khavanin, Zamanian Z. Are supplementation of omega-3 and ascorbic acid effective in reducing oxidative stress and depression among shift workers? Int J for vitamin and nutrition research. 2016. DOI 10.1024/0300-9831/a000249
- 9. Appleton KM, Sallis HM, Perry R, Ness AR, Churchill R. Omega-3 fatty acids for major depressive disorder in adults: an abridged cochraine review. BMJ Open. 2016;6:e010172. Pubmed. DOI:10.1136/bmjopen-2015-010172
- 10. Mocking RT, Harmsen I, Assies J, Koeter MJ, Ruhe HG, Schene AH. Meta-analysis and meta-regression of omega-3 polyunsaturated fatty acid supplementation for major depressive disorder. Transl psychiatry. 2016:6;e756; Pubmed DOI: 1.1038/tp.2016.29
- 11. Hadley KB, Ryan AS, Forsyth S, Gautier S, Salem Jr N. The essentiality of arachidonic acid in infant development. Nutrients. 2006;8:1-47. Pubmed DOI: 10.3390/nu8040216
- 12. Kuratko CN, Barrett EC, Nelson EB, Salem Jr N. The relationship of docosahexaenoic acid (dha) with learning and behavior in healthy children: a review. Nutrients. 2013;5:2777-2810. Pubmed DOI:10.3390/nu5072777
- 13. Koletzko B, Edenhofer S, Lipowsky G, Reinhardt D. Effects of a low birthweight infant formula containing human milk levels of docosahexaenoic and arachidonic acids. J Pediatr Gastroenterol Nutr. 1995;21:200-208