Overview of Selective Serotonin Reuptake Inhibitors
Introduction
If you are suffering from a depressive disorder or an anxiety disorder (including PTSD) chances are good that somewhere along the line a physician will recommend that you take an antidepressant. Most likely the recommended antidepressant will fall into the family of the selective serotonin reuptake inhibitors, or SSRI’s for short. The reason this class of medication is likely to be the first one tried in any effort to combat depression or anxiety is that they are among the safest and best tolerated of the antidepressants.
Unfortunately, that doesn’t mean these medications don’t have side effects or risks. The aphorism “there’s no such thing as a free lunch” definitely applies to antidepressants. There just aren’t any, not even herbal ones, that don’t come with some problems to go along with the potential benefits. In this article I’d like to discuss the mechanisms of action, potential risks, benefits and side effects of the medications in this category just as I would with a patient. This advice doesn’t replace an honest, open discussion with your own physician, but I hope it will give you some initial information and a place to begin the conversation with your doctor.
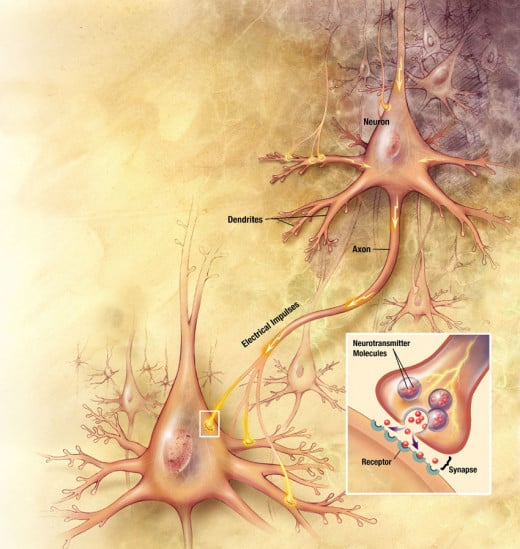
How SSRI's Work
Currently there are six antidepressants in the SSRI category. I will refer to them by generic names in the article because brand names change from country to country and some medications actually have more than one brand name. The current SSRI’s available in the United States are fluoxetine, paroxetine, fluvoxamine, sertraline, citalopram, and escitalopram. Fluvoxamine is very rarely used and so the information in this article applies mostly to the other five medications. Each of these medications will slow down your brain’s ability to pull serotonin (an important chemical in your brain that nerve cells use to communicate with each other) back into the nerve cell (also called a neuron) that initially released it. This is what the phrase “reuptake inhibition” means. In this way the amount of serotonin available to signal the receiving cell (another neuron) is increased. There are a lot of hypotheses about why this causes an improvement in anxiety and depression and there is some exciting research out there about that question, but the truth is no one is quite sure why this helps. Hopefully this answer will be found soon, as it will give us important information about how the disease of depression works inside the brain. We do know that the increase in serotonin itself isn’t what relieves symptoms; symptom relief can take 4 weeks or more from the time you start the medication.
No particular SSRI is any more effective than another SSRI. Research tells us that with any given medication about 1/3 of people taking it to relieve depression will experience a remission, which means their symptoms will completely (or near completely) resolve. This is the clinical outcome that doctors aim for. Another 1/3 of people will experience a response, which means their symptoms are about 50% better but they still may be significantly ill. Unfortunately, about 1/3 of people will not respond at all to a given antidepressant.
The reason some people do not respond is that medications for depression can be thought of as keys. The medication key needs to fit the particular “lock” (a receptor) on a person’s nerve cells in order to take effect. Just as most houses have different locks, most people have slightly different “locks” due to genetic variation. So no one medication will work for everyone. Currently there is no clinically available test that will show which medications will work for a particular person. However, if you have a biological family member, particularly a first-degree family member (parent, sibling or child) who has done well with a particular medication be sure to let your doctor know that. There is a much higher chance that medication will also work well for you. If one medication does not work, which means no significant improvement after 4 weeks on an adequate dose, ask your doctor to try another. I have had many patients respond to one SSRI but not another.
Most SSRI’s are started at a low dose, a dose that is considered too low to provide benefit. The reason for starting at a low dose is to decrease side effects by allowing a person’s body to adjust to the medication over time. Typically the dose should then be increased every one to two weeks until a therapeutic dose, a dose that is likely to provide clinical benefit, is reached.
Side Effects
Most of the side effects of SSRI’s are class effects, which means they apply to all the medications in this category. The side effects of SSRI’s do seem to be directly related to the increase in serotonin between the nerve cells and tend to start immediately. This is one of the major drawbacks to this category of medication – unpleasant side effects can start immediately, while benefits can take weeks to arrive. Many people have trouble tolerating the side effects long enough to see if they will achieve any benefit. The common side effects of SSRI’s as are follows:
Stomach upset. This can range from feeling mildly nauseated or having loose stools to frank vomiting or diarrhea. In my experience most people will only have mild nausea, and this will improve after about 1 week on the medication, although it is likely to recur when the dose is increased. Less than 10% of my patients have experienced vomiting or diarrhea from an SSRI. Most of the time if someone is actually vomiting from a medication they will need to be switched to something else, since in general it is not very reasonable to tolerate a week of vomiting while you are waiting to get used to the medication. Don’t be afraid if one SSRI causes severe stomach upset. Another one is very likely to be better tolerated.
Akathisia. This is a temporary (1-2 weeks) feeling of increased restlessness or jitteriness that is typically experienced more in the body than in the mind, although it can make some people feel more anxious. It does not happen to most people, and when it does happen it is generally mild, causing people to feel mildly keyed up. However when it is severe it is very, very uncomfortable (one patient described it to me as “my skin is crawling all over my body”) and needs to be treated. Usually the best way to address this is a lower dose or an additional medication to block this particular side effect, taken for 1-2 weeks until your body adapts to the medication.
Sexual Side Effects. These are some of the most problematic side effects of this class of medication, because they occur in over 75% of people who take SSRI’s and will be present for as long as you take the medication. They will resolve when you stop the medication and in my experience sexual side effects are a big cause of people stopping their SSRI’s prematurely. In women the side effects tend to be loss of interest in sex and decreased in ability to experience orgasm. In men the side effects are usually decrease in ability to experience orgasm and loss of interest in sex, but I have had some male patients complain about erectile dysfunction as well. Many patients are embarrassed to talk to their doctor about these symptoms, but they are very important to discuss. Sexual problems can lead to increased relationship stress that can exacerbate the underlying depression and anxiety that the medication was supposed to be treating. Sexual side effects of SSRI’s can also be easily treated, usually by adding an additional medication to block this side effect.
Discontinuation. Like anything you take regularly for a long time (think about caffeine, sugar, carbohydrates) your body will get used to the presence of an SSRI. This is not the same thing as addiction. You will not be addicted to your SSRI. Addiction, from a medical perspective, means that you want to use increasing amounts of the medication in order to obtain a euphoric (buzzed) effect. Trust me, no one ever wants to take more and more of their SSRI, and they are not going to make you feel buzzed.
When it is time to come off the medication (about 6-12 months after remission of symptoms is achieved, if this was a first episode of illness) you will need to do this gradually and under a doctor’s supervision. There are three major symptom clusters I have seen when people stop taking an SSRI abruptly. The first is that their initial symptoms return. What that usually means is that the medication was working to control the symptoms but the episode of illness isn’t over yet. I recommend going back on the medication and then discussing with your doctor when another trial of coming off it is appropriate. The second is feeling dizzy, achy and generally quite ill as if you had a viral illness. This can last for a week or more. The third frequently heard complaint is a sense of electric shocks running down the arms. I am not sure why this symptom occurs but I have heard it many, many times from patients who abruptly stopped their medication. Any of these symptoms will go away over time, but I strongly recommend not stopping your antidepressant on your own or too quickly.
Suicidal Thinking. This is one of the two most dangerous side effects of antidepressants. There are a few studies out there showing that antidepressants (all antidepressants, not just SSRI’s) can in some patients (particular adolescents and young adults, under the age of 25 years) lead to an increase in thoughts of suicide. There have not been any studies linking antidepressants to an increase in suicide attempts or suicides, but this is still a very concerning and serious side effect. It has not been well explained and some researchers wonder if it truly exists. Regardless, the FDA has mandated that all antidepressants be labeled with a warning about this side effect.
What I would like to tell you about suicidal thinking is this. Any suicidal thinking is an emergency. It is as serious an emergency as a heart attack and should be treated as such. If you ever, for any reason, regardless of medications you are or are not taking, experience thoughts of wishing you were dead, wanting to be dead, planning to kill yourself or others or other suicidal thoughts, please get immediate help. Call 911. Have someone take you to the nearest emergency room. Call the national suicide hotline at 1-800-273-TALK. Please do not harm yourself or anyone else. Your life is precious and there is hope for you. Please reach out for help. And if someone reaches out to you, please take that person very seriously. Suicidal thinking is never a joke. Please get that person to medical attention, immediately. You will probably be saving a life.
Serotonin Syndrome. Serotonin syndrome is the other very dangerous possible side effect of medications that increase the amount of serotonin in the body. If the amount of serotonin goes too high, you will become very ill. The basic symptoms of serotonin syndrome are muscle rigidity or jerkiness, changes in your heart rate, temperature or blood pressure, and mental confusion. This is a possibly lethal condition that is almost always seen as the result of taking medications in combination. Besides antidepressants, there are several other medications (some pain relieves, some antibiotics, some herbal medications, some over the counter cold medications) that can increase the amount of serotonin in your body. For this reason, it is very important to always keep a current written list of your medications with you. Include any over the counter or herbal medications you are taking on the list. Make sure every doctor you see knows all of the medications you are taking and be sure to ask your doctor about potential dangerous interactions. It is also important to know that the herbal antidepressant, St. John’s Wort, is able to cause this syndrome just like prescription antidepressants can.

Other Considerations
You may have noticed that I didn’t mention weight gain in the above, rather scary list. That’s because weight gain with antidepressants is highly variable. Some medications, like paroxetine, are very likely to cause weight gain. Some, like fluoxetine, are very unlikely to cause weight gain. The others are variable. I have had more patients complain about weight gain on sertraline than citalopram or escitalopram. None of the medications will alter your metabolism to make you gain weight, but paroxetine at least has a tendency to make people feel hungrier.
A frequent complaint I have heard from patients after starting an antidepressant is that they feel numb, which is very unpleasant. I have heard this more from patients being treated for depression and less from patients being treated for anxiety. Usually what has happened is that the antidepressant has started to work but is not fully addressing the depression. It has removed some of the terrible feelings of sadness, but that good and joyful feelings have not returned. For most patients, an increased dose actually helps them get their symptoms completely into remission, so that their normal emotional functioning returns. For a few patients it has meant that a change in medication has been needed. It is not normal to feel numb on an antidepressant. Medication, when dosed appropriately, should have the effect of pulling back your depressive and anxiety symptoms so that you can be yourself once again.
If you a woman considering having children there is an entire additional layer of complexity added to the decision to take antidepressants. That topic is too intricate to cover adequately in this article. I strongly encourage you to discuss the possible risks and benefits of an antidepressant to an unborn child with your doctor at the time you start an antidepressant, and well before you actually conceive. Research data about this question is hard to come by and harder to interpret, but the current information shows that there are risks both to untreated depressive and anxiety disorders as well as to medications. Different medications also have different levels of risk, so expert advice relying on the most current data is very important.
If you are suffering from symptoms of depression or anxiety, there is relief available. The choice to take an antidepressant is a frightening one for many people. I hope this article is helpful to you as a beginning point in your researches. I encourage you to speak honestly to your doctor about your symptoms and ask about treatment options. Together you can discuss your symptoms and evaluate if the risks of an antidepressant are worth the potential benefit in your particular circumstances. Current studies seem to show that the best effects of antidepressants are seen in moderate to severe disorders. Research also shows that psychotherapy alone is appropriate for mild to moderate symptoms. Psychotherapy and medication in combination is the best available treatment for depression and anxiety disorders at this time. Regardless of your treatment choices, please know that your symptoms can improve and that you can return to a full, functional and joyful life.