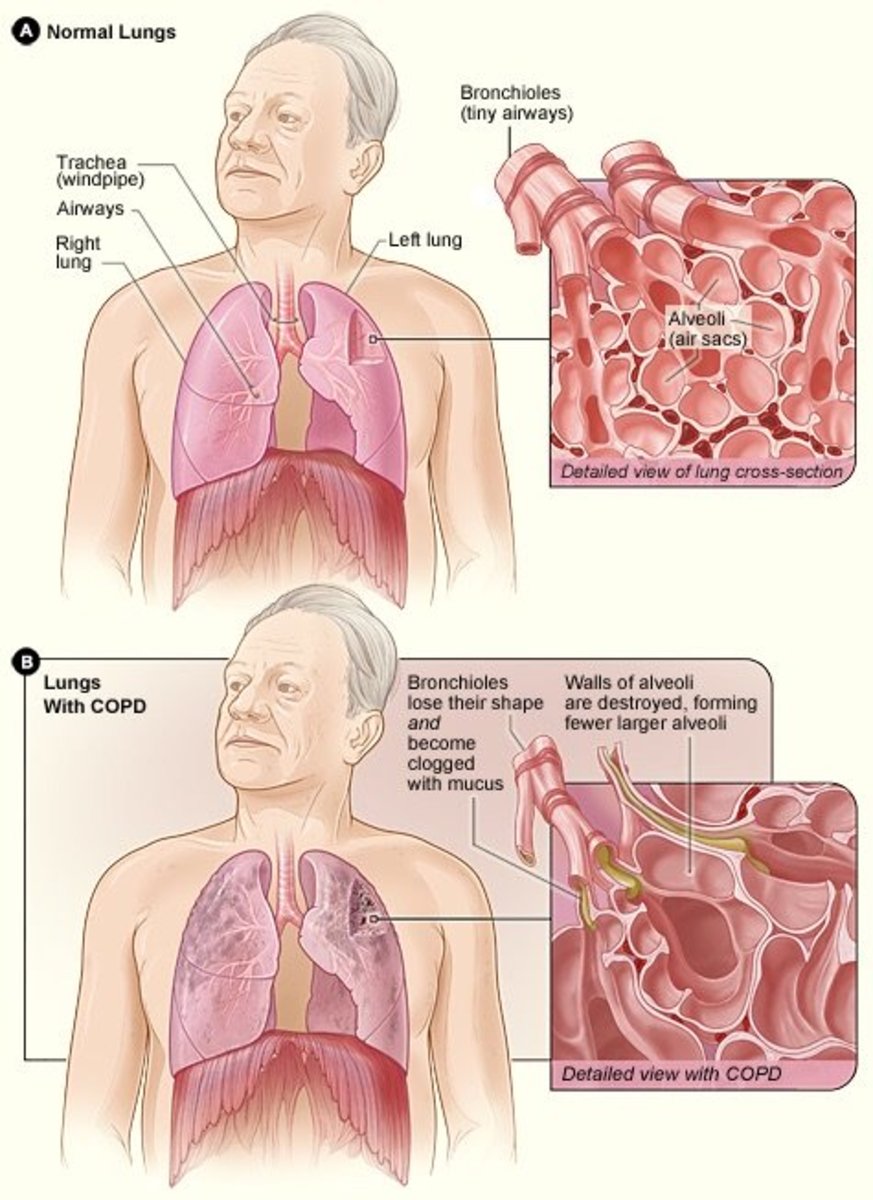
Possible Lung Injuries While Diving

Thes injuries listed are caused by the diver holding their breath on ascent after a dive.
Most body air spaces respond to pressure decrease with neither complications nor voluntary action by the diver. The Lungs respond to this as well, provided the diver breathes continuously to them keep equalized to the declining pressures.
If the diver holds their breath or air traps within a section of the lungs, and as pressure declines expanding air will almost always cause an over-expansion injury.
The "GOLDEN RULE" in diving - never hold your breath while on scuba and while underwater. Panic and ignorance have been the causes of divers holding their breath. Nausea, choking and carelessness have also been causes to this as well.
Obstruction in the lungs may also trap air in certain parts and in effect "hold its breath." A chest cold, or respiratory infection can cause mucus accumulation and cause an obstruction. Smoking has also been implicated in these injuries.
Lung injuries can occur from even a small amount of over-pressurization. Research has shown that starting with full lungs, holding ones breath and surfacing can have an injury in as little as a 3 to 4 feet distance.
Rather than the lungs bursting like a balloon, an over-pressurization tears the lungs. The injury does not occur from the tear to the lungs, but from the air escaping and entering the tissues and / or the bloodstream.
Any lung injury causes pulmonary capillaries and alveoli to rupture, mixing blood and air in the lungs. This results, often times, to the victim is coughing up blood.
AIR GAS EMBOLISM (AGE)
This is the most serious type of lung over-pressurization injury. This result occurs when the air enters the blood stream from a rupture of the alveoli into the pulmonary capillaries, causing an air embolism or arterial gas embolism. Think of this as a blood embolism, but replace it with air. It acts the same way.
An embolism is any foreign object that enters the bloodstream that blocks its flow. An air embolism is the same but now it is an air bubble that blocks the flow of blood. So as you ascend the once small bubbles become larger and larger due to the expanding nature of the ascent. This is a bubble on the arterial side of the circulation.
Air enters the bloodstream in the lungs flows through the pulmonary vein into the heart, to the left side of the heart into the aorta and then the arterial system. This air bubble can lodge almost anywhere in the circulatory system - can cause severe damage by blocking blood flow to the tissue.
The first main branch off the aorta is the carotids. The carotids supply the majority of blood to the brain. If bubbles travel into the carotids, which is likely, they will go to the brain and cause cerebral air embolism.
The bubbles deny the brain of oxygenated blood, which causes a stroke. The symptoms include dizziness, confusion, shock, personality changes, unconsciousness, and death.
The effects of cerebral air embolism and other lung injuries tend to be rapid and dramatic. DCS tends to be delayed.
If the bubbles were to miss the carotids, and block the coronary arteries, the result would be a heart attack.
MEDIASTINAL EMPHYSEMA
Mediastinal means center of the chest. This is sometimes called pneumomediastinum, is far less serious that air gas embolism and pneumothorax This condition, air accumulating in the mediastinum presses on the heart and major blood vessels interfering with circulation. A victim may feel faint and short of breath due to impaired circulation.
SUBCUTANEOUS EMPHYSEMA
This occurs frequently with mediastinal emphysema as air seek its way from the mediastinum, and following the path of least resistance, into the soft tissues at the base of the neck.
Air accumulates under the skin in this area. This causes the victim to feel a fullness in the neck and to experience a voice change. The skin may crackle if touched.
PNEUMOTHORAX
If the over pressurized lung tears at it surface, the expanding air leaks between the lungs and the pleural lining (chest wall), causing the lung to collapse, either partially or entirely. This collapsed lung is called a pneumothorax. This is not nearly as life threatening as an AGE because the victim, in most cases, still has a working lung to breathe from. This collapse lung causes severe chest pain, and may cause the victim to cough up blood. There is another form of this condition called spontaneous pneumothorax. This occurs with out the expansion of the lungs but through a weakness in the lung itself. This causes a sudden tearing and collapse of the lung. This condition is uncommon, but can be more serious than the standard pneumothorax. especially if it happens underwater. This type can be aggravated on ascent, when the air pressing on the collapsed lung expands, increasing the pressure of the injured lung.Since spontaneous pneumothorax tends to recur, it inhibits further diving till surgery is performed to correct the problem. Since out a physician who specializes in pulmonary dive medicine.
FIRST AID
The first aid for both the decompression sickness and lung overexpansion injuries are the same. You can say that the first aid for the Decompression illness injuries are the same. In fact you do not have to determine on site which you are dealing with to start giving aid to the diver.
Give 100% oxygen to the diver Simply put, breathing 100% O2 accelerates diffusion of nitrogen from the body to slow and reverse bubble growth, and help bubble elimination. Breathing oxygen also raises the blood oxygen levels and maximizes the effectiveness of the blood that does reach the affected areas. Make sure the air ways are clear and treat for CPR if needed. The best first aid is to get them to a medical facility for proper care
Three out of the four conditions are not immediately life threatening, the presence of any of these conditions indicates a lung over-expansion injury has occurred. The AGE is the most life threatening and therefore when first aid is given, they treat any of these conditions as though they have AGE .AGE needs immediate compression to diminish the bubbles in the bloodstream and force them into solution. This restores blood flow to the tissues. None of the other conditions require decompression, provided there is no AGE. Pneumothorax requires surgical removal of the air from between the collapsed lung and the pleural lining, followed by a lung re -inflation. Mediastinum and subcutaneous emphysema will dissipate on their own as the blood slowly reabsorbs the trapped air. Breathing oxygen can speed up the re-aborbtion process.
REMEMBER DO NOT HOLD YOUR BREATH WHILE DIVING ON SCUBA.