Stem Cell Transplants For Cancer Treatment
Bone Marrow and Blood Stem Cell Transplants: A Guide For Patients
In my previous article, I discussed what are stem cells and shed some light on hematopoietic stem cell transplantation. In brief, stem cells are the master cells from which other cells, tissues, and organs generate. Now to reduce any damage caused to stem cells from blood cancer treatments like radiation therapy and chemotherapy, the stem cells from the bone marrow are removed and preserved before the patients receive chemotherapy or radiotherapy. The stem cells are then reinfused into the patient’s bone marrow after cancer treatments where they migrate to the bone marrow and start producing fresh blood cells. Most patients with non-Hodgkin's lymphoma and multiple myeloma are offered this technique as part of their cancer treatment. Once the stem cells are collected, they are usually infused immediately to the patient where they migrate to the bone marrow. Once stem cells reach there, they can repopulate the blood with normal RBCs and leukocytes to save the patient and treat his/her’s severely morbid condition. This technique is a miracle for some types of cancer.
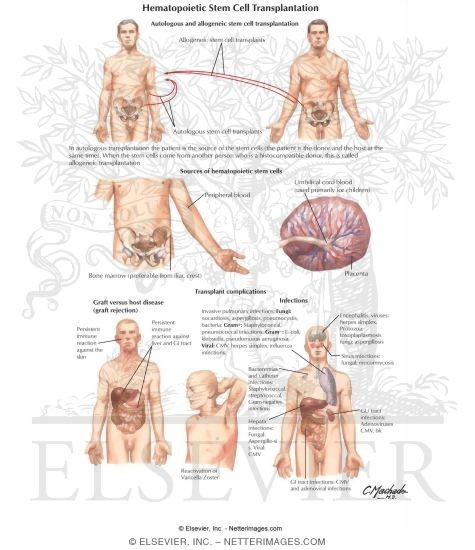
On the other hand, stem cells are harvested from a donor and are “cryopreserved”, which means that they are frozen in liquid nitrogen for many years. At a later stage, they can be thawed and infused into a patient.
The success of stem cell transplantations of blood depends on the interactions of the markers on the surface of all body cells including immune cells of both the donor and the patient. Normally, all the cells of patient's body peacefully coexist in a self-tolerant state because they all carry the same proteins. These proteins are also called as antigens because when these antigens are introduced to a new environment, they are able to stimulate a powerful immune reaction. This situation happens when a preparation of hematopoietic (blood) stem cells with antigens is transplanted into a patient whose antigens from self are very different.
Some donated blood stem cells bring their own distinctive self-antigens. Sometimes, the immune system of the patient, who is known as host to these antigens detects no match and as a result the patient's immune system attacks these donated transplanted cells, creating a situation that can lead to transplant rejection by the patient. However, more often, some mature donor immune cells that are mixed between transplanted hematopoietic stem cells recognize antigens in cells from the patient as foreign. This rejection causes the attack of immune cells to transplant tissues and organs of the patient. The result is graft verus host disease, which can be very fatal for the patient.
Successful stem cell transplantation of blood depends on finding a compatible pairing of antigens in cells and tissues of the donor. In many cases, this situation means finding a match that is slightly different, but not too different. For this reason, it becomes not necessary for a donor to be related to the patient, but they must have a reasonable amount of compatibility. A blood test known as tissue typing is used to find good combinations.