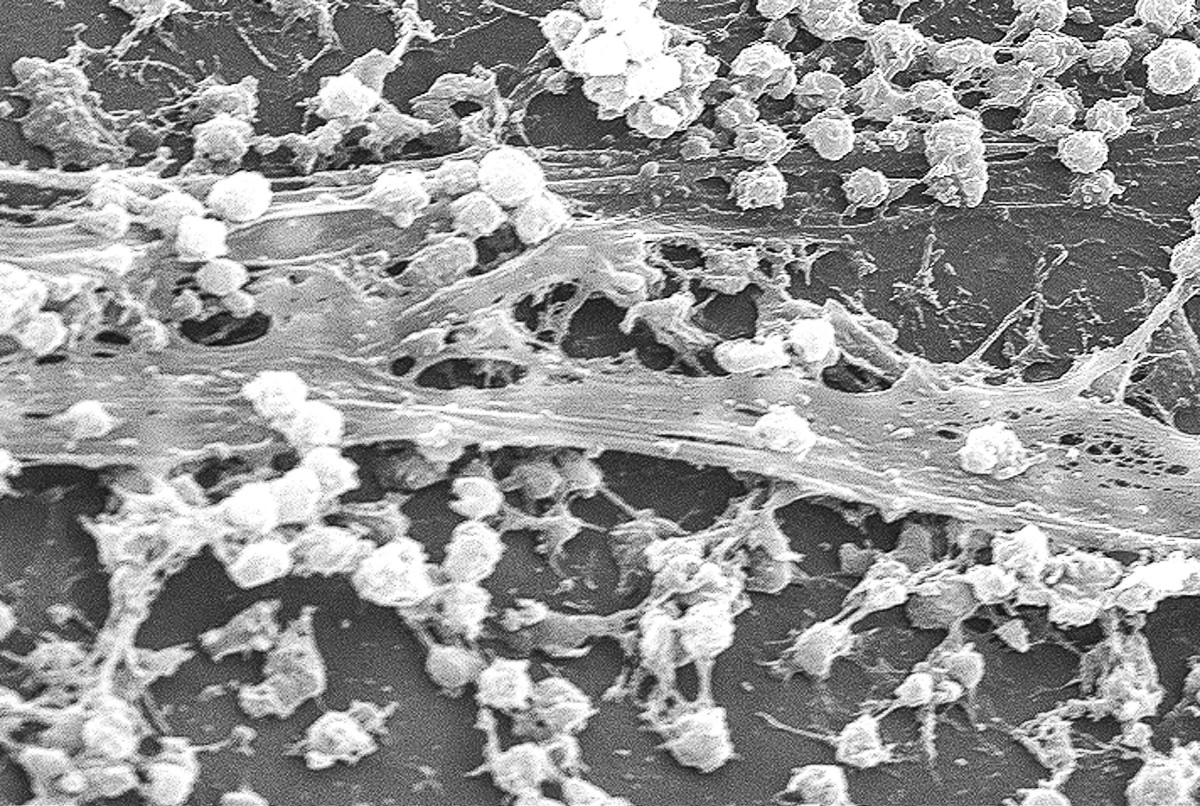
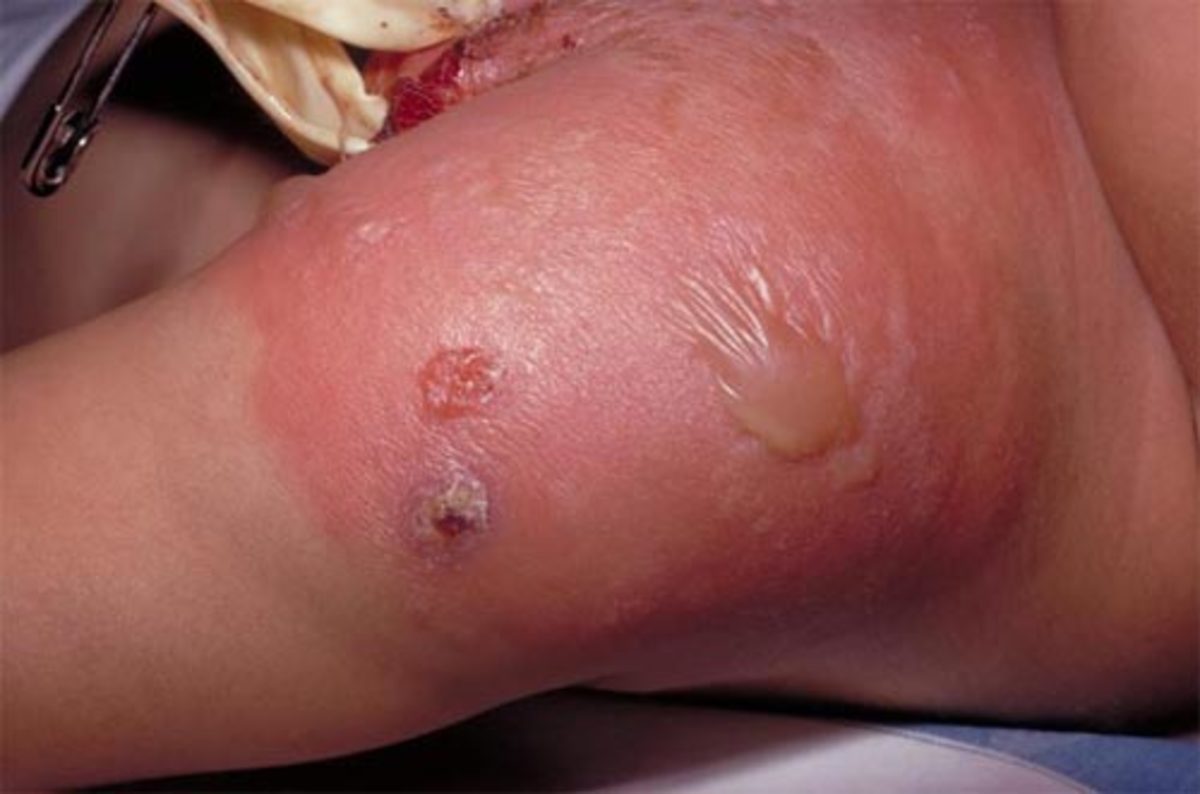
Antibiotic resistant bacteria
Scientific presentation at a World Health Organization meeting
Antibiotics are considered as one of the most important discoveries of the 20th century. The real problem lies in the increased development of antibiotic resistance in hospitals and other environments where antibiotics are used. The remarkable genetic abilities of bacteria have greatly benefitted from the overuse of antibiotics. This has given bacteria the ability to develop resistance genes and multiple resistance mechanisms for every antibiotic introduced into clinical use. The booming application of any therapeutic agent is jeopardized by the probable development of resistance to the agent from the first instance of use.
The discovery of antibiotics dramatically shifted human health; infections once considered deadly could now be treated. However, the frequent use of antibiotics over long periods put the bacteria under selective pressure (Louw et al. 3182). This meant that bacteria with special traits could resist antibiotics and further divide, the result being a new breed of resistant bacteria. Over time, it has been noted that gene exchange is a property of bacteria. It has occurred through the centuries of microbial evolution. This evolution also transfers the genes associated with antibiotic resistance across different bacterial species. Gene transfer occurs through plasmid-mediated gene transfer. This has become a major focus of research because of its medical significance. Most of the bacterial species linked to human disease outbreaks have undergone evolution as a result of the factors listed above. This has resulted in the emergence of multidrug resistance (MDR) forms due to uncontrolled antibiotic use. For instance, the multidrug-resistant form of tuberculosis has become a key pathogen in developing and industrialized countries. Other examples of acute nosocomial (associated with hospitals) pathogens include; Enterobacter spp, Escherichia coli, and Streptococcus pneunimoae. “Superbugs” is a term used to refer to bacteria with an improved mortality and morbidity as a result of several mutations conferring increased levels of antibiotic resistance, particularly to antibiotics recommended for their management.
The most widespread gram-negative bacteria such as Klebsiella pneumonia cause a myriad of diseases in humans. A strong link between the use of antibiotics in the management of these diseases and the development of antibiotic resistance has been observed over the past few years.
These bacteria are omnipresent in the atmosphere; their consequences are provoked by situations such as violence, civil unrest, global travel, natural disasters and poor hospital practices. On the global management of pandemic and endemic infectious diseases, lack of reliable tracking systems for tracking outbreaks is a significant problem. In spite of the vital efforts of the World Health Organization, global travel is still a significant problem.
In addition to these factors, another significant contributing factor for antibiotic resistance is the economic considerations taken by major pharmaceutical companies involved in the production of antibiotics. Antibiotics can be used for a short while because prolonged use eventually results in resistance, a highly undesirable trait (Wright, 593). It costs a major pharmaceutical company up to one billion dollars to develop an antibiotic. The antibiotic can then only be used for treating bacterial infections for only a couple of years at most. Therefore, it does not make any economic sense to spend huge sums of money on a project that will not be profitable in the end. The company has to concentrate on projects which are economically viable in the long run. It is for this reason that Pfizer, a major pharmaceutical company spearheading antibiotic development shutdown its antibiotic research efforts.
Antibiotic resistance is inevitable. As a result, many steps have been put in place to control it. Knowledgeable experts from major global health groups like WHO and the CDC have proposed different solutions for this problem. These include; stringent controls on human antibiotic use, no sale of antibiotics without prescriptions and requiring appropriate prescriptions for antibiotic use.
Bacteria resistant to all antibiotics
Audience analysis for the World Health Organization meeting
This report is written for health and biological scientists; these are seasoned academics and professionals in the field. Therefore, it is an assumption that my audience is as well conversant with the scientific terms, in addition to this they may also have in-depth experience with the key terms I have used. My audience may be very passionate towards antibiotic resistance studies, or they may work for research or corporate entity involved in such studies or both. For this reason, my audience expects a presentation which lays more emphasis towards logic and evidence than that which appeals to pathos.
My audience typically consists of men, between the ages of 30 to 60 years. These make up the bulk of the scientific community. They are married. The audience is mostly upper class, with at least a university degree, though some may have college diplomas. Some members of the audience may have advanced education such as doctorate degrees and may be professors.
This audience is paying interest to my presentation because there has been increased interest in studies concerning antibiotic resistance in bacterial species. It is not only an emerging issue but a very important one since it claims the lives of tens of thousands of people every year. They are interested in learning all they can about this emerging issue.
This presentation will be seen in scientific journals and books. It will also be published in newspaper inserts
As stated earlier, this audience is interested in getting the correct facts about antibiotic resistant bacteria. They need correct, up to date information with all the facts concerning antibiotic resistance in bacteria. The audience will learn all about antibiotic resistant bacteria.
Presentation by the magazine reporter
Antibiotics have helped in controlling and destroying most harmful bacteria that have the ability to make us sick. However, in recent years, antibiotics have been losing their ability to fight bacteria. As a matter of fact, some bacteria are now fully resistant to today’s antibiotics. Unfortunately, the manner in which we have been using antibiotics has facilitated the emergence of new drug-resistant bacteria, also known as superbugs. These are a strain of bacteria that have resistance to most types of antibiotics. These drug-resistant bacteria kill over 23,000 people annually according to statistics from the U.S Centers for Disease Control and Prevention (CDC). Bacteria responsible for diseases like tuberculosis, staphylococcus infections and gonorrhea have now developed resistance to antibiotics. These are some of the few dangers that the society faces.
Antibiotics are undoubtedly the most prescribed drugs. They are very effective against bacterial infections like a sore throat, ear infections, and pneumonia. These drugs do not work against viral infections like those that cause flu or colds. Sadly, most antibiotics are unnecessarily prescribed to people who do not need them. This misuse and overuse of antibiotics have facilitated the development of drug-resistant bacteria. Antibiotic resistance is the ability of a bacterial species to endure the effects of an antibiotic. This type of resistance mutates naturally through natural resistance as a result of evolution. It can also occur because of the evolutionary stress or selective pressure on a population. Once the gene mutates, the transformed bacteria can then vertically or horizontally transfer the mutated gene to other bacterial species via plasmid exchange.
When a bacterium has several genes conferring resistance, it is known as a multidrug resistant species in medical circles or informally, a superbug. The mutated bacteria can then transfer this trait to its offspring. Antibiotics kill bacteria by interfering with a critical function. This can be equated to how criminals can crash a massive airplane by just cutting the hydraulic tubes. The antibiotic binds to proteins involved in cell wall synthesis. Once they inhibit these genes, the bacteria cannot replicate, thus effectively killing them.
With over a billion people traveling the globe, bacteria are now more transportable than they have ever been. This is the same case with superbugs. You can aid slow down the spread of these superbugs by taking antibiotics only when you need them. You should not insist on taking antibiotics when you are advised otherwise.
Major pharmaceutical companies do not see any economic sense in continuing to channel their efforts and resources towards the development of antibiotics. This is because the development of a single antibiotic regimen may require up to a billion dollars and a horde of scientists to complete. The antibiotic may not yield much profit since antibiotics do not last long in the market before the bacteria they were intended for developing resistance to them. Therefore, it makes more economic sense to pharmaceutical companies to divert their efforts towards the development of more profitable drugs.
Major global health groups like the World Health Organization and the Centers for Disease Control have proposed measures to control the development of antibiotic resistance like; limiting the use of antibiotics by human, offering alternatives to antibiotics and requiring antibiotics to be bought exclusively with prescriptions. Experts may seem to be doing too little, too late. However, antibiotic resistance can still be controlled by the concerted efforts of medical practitioners and the general public. In some instances like ear infections or sore throats, the body is still able to fight the infection. In such cases, it is not advisable to rush to seek antibiotics; this only contributes to antibiotic resistance. The easiest way of preempting infection is by frequent hand washing.
Audience analysis for the magazine reporter
The target audience is men and women who spend a generous amount of time watching television and flipping through lifestyle magazines. This is an audience looking for new information about lifestyle issues. They want to know all that entails their families and the society at large. These people are not very knowledgeable about the issues concerning antibiotics and bacterial resistance.
The audience is not very knowledgeable of scientific jargon. As such, I tried to limit my use of complicated scientific words, instead preferring to use more palatable words. I also explained the complex scientific terminologies that I could not avoid using. They are only conversant with simple everyday vocabulary, immersing them into tough jargon would be an uphill task for their comprehension.
My television audience is composed mostly of men who are interested in watching the news and staying up to date with current affairs. It is composed of men aged between 25 to 70 years. They are married, return home early and regularly buy magazines.
These women will be reading this presentation because they are flipping through a lifestyle magazine and are attracted to the idea that abusing antibiotics can have adverse effects on the body through the development of antibiotic resistant bacteria. They are interested in the fact that it is unsafe to abuse antibiotics.
This presentation will be seen in lifestyle magazines, newspapers, health journals and lifestyle news. It may also be read online. Specific needs that are addressed by this presentation include; the need for safe antibiotic use to prevent the development of resistance.