Brain Research: Transplanted Neurons Can Restore Brain Function, and Control Obesity
As a biologist interested in brain research and human behavior, I was fascinated by the study of Jeff Macklis and colleagues (Science, Nov 2011)--who demonstrated how inserting neurons in the brain can lead to changes neural function---and in this particular study, resulted in decrease in body weight on mice.
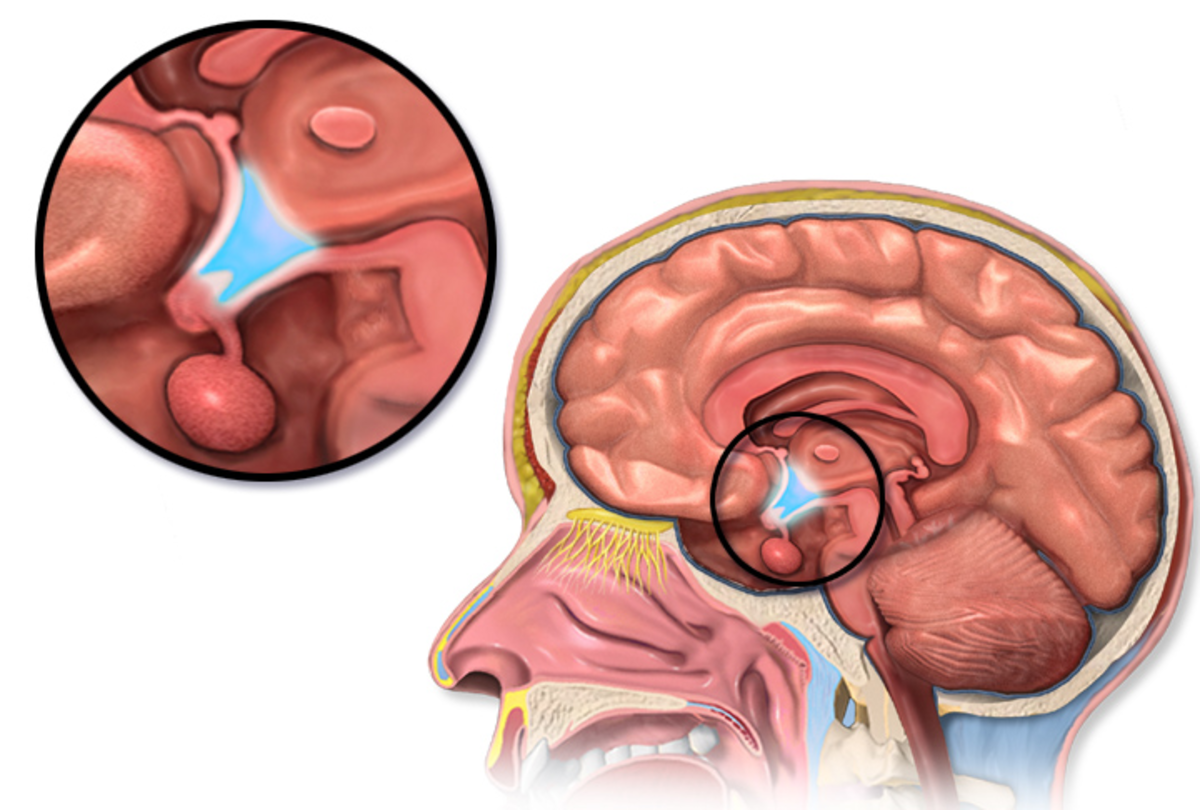
The study involved the insertion of fetal neurons labeled (with a bioluminescent gene that glows)-- into areas of the brain that had been previously damaged. The researchers could track the presence of the new neurons by their glowing under certain conditions.
Obesity of mice and humans has been previously linked to high circulating leptin levels and leptin resistance (El-Haschimi and others; Journal of Clin. Invest. 2000). Scientist also knew that resistance induced diet evolved through the course of a diet high in fats and has at least two independent causes: "an apparent defect in access to sites of action in the hypothalamus which limits peripheral leptin from activating hypothalamic STAT signaling, and an intracellular signaling defect in leptin-responsive hypothalamic neurons that lies upstream of STAT3 activation."
Not all neurons would work for this kind of transplants. The transplanted cells need to be immature--and beginning to differentiate into hypothalamic neurons. Because, there in hypothalamic neurons is where the defect has been previously identified--and thus where the problem could be corrected. The insertion of the 'new' neurons seems to create pathways that allow either of the previous damaged mechanisms to operate--thus allowing proper leptin regulating function to occur.
Inserting neurons in mammals seems to be a whole new frontier. It is like the mammalian GMO, though a bit different. A few years ago, these experiments may have been in the realm of science fiction, not anymore.
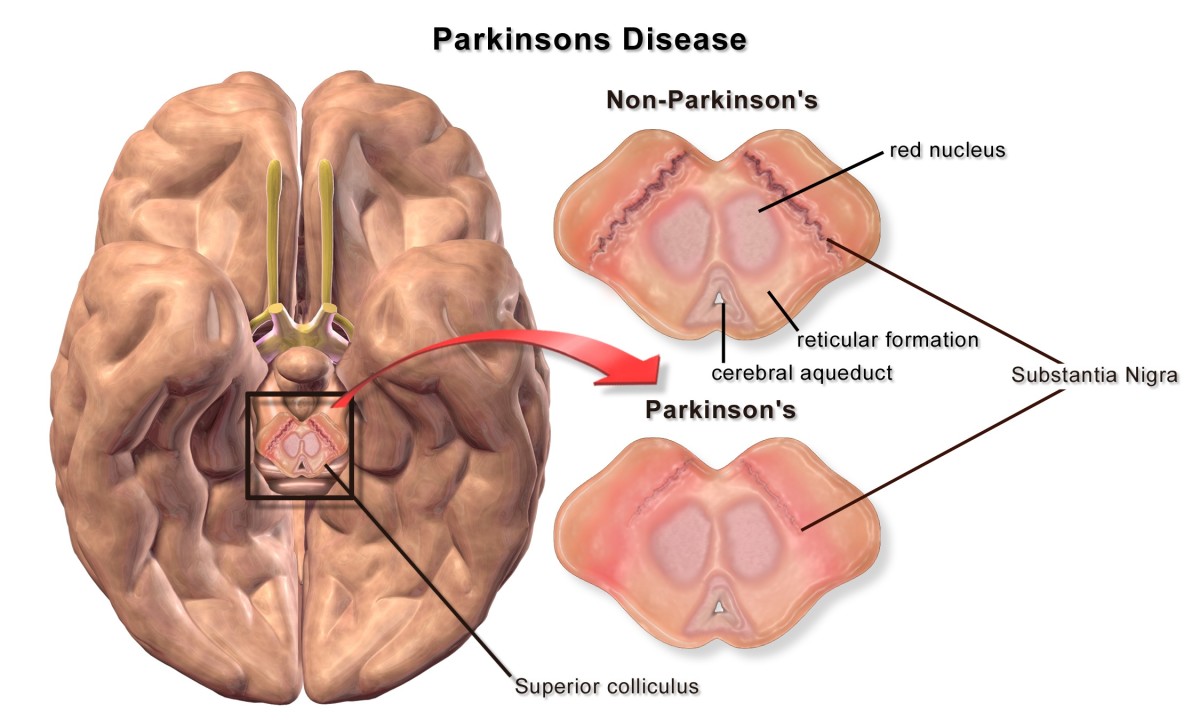
Previous experiments that target cancer with nanoparticles--are on the frontier of science manipulations, though they generally do not involve the brain. Proposed treatments for Parkinson Disease using stem cells, involved trials in mammalian brains yet so far they failed.
Perhaps, because the brain is the master of bodily functions, and somehow has been mystified because of the functions of the mind, anything that have the capacity to alter brain function in a mammal--and possible humans, is rather fascinating.
The fact that this altered neurons can be inserted in a mammal, specifically mice make me think that we are not too far from inserting them in humans. I clarify here that the study does not target humans, although it has implications for the regulation of obesity in humans as well as for the treatment of other conditions.
How many things are possible by changing neural pathways? Even though there may be ethical barriers--that currently prevents these experiments in humans, the mechanisms could be applied to target conditions such as Parkinson, dementia, schizophrenia, psychosis, and Alzheimer.
When science meets desperation, people are willing to try even methods that are not yet validated. Would you accept a neuron insertion if you knew some of your pathways, for e.g., hormonal regulation, memory, and so forth were damaged? In the answers to such questions lies the frontier of science and of these type of research.
Today, we know that without surgery, it is possible to stimulate the brain to continue growing neurons, and that the new neurons have the ability wire up or attach to previous pathways. We now with this experiment, know that even if the previous neurons weren't there new neurons can be inserted--and those neurons have the potential to change certain pathways or sustain function, in ways that ten years ago would have not been predicted.
Macklis and colleagues investigated if fetal neurons transplanted into a part of the mouse brain that does not normally produce new neurons of its own could repair an abnormal neural circuit. Indeed the mouse that lacked the pathways would grow to be extremely obese adults--because it has the defects associated with leptin regulation. The mice that received the 'new neurons' were still a little big, but not as obese as the controls that were not treated. This means a lot, for the many other pathways -and conditions that may have a window of opportunity to be re-visited. It perhaps would bring hope to many people.
While this experimental techniques remain inaccessible to medicine, and to the treatment of obesity and other conditions, the solutions for people whose neuroendocrine pathways are not fully damaged would still remain in the realm of the simple: a diet that has a high nutritional value, with low sugars and fats, along with physical exercise. To keep the brain sharp and also to maintain our neuron factory, scientists recommend brain exercises and activities of all sort, including reading and writing, as well as learning new things, and avoiding toxic substances.
As individuals, we have the ability to modify our behaviors. If retraining or changing behaviors do not work, and if diet does not work, the approach shall be more holistically. It shall include checking hormone regulations and investigating other factors associated with obesity.
Researchers have proposed that leptin has a role in the neuro--endocrine system. For example, leptin is also involved in the stop of ovulation on food-starved female mice. Endocrine system anomalies have also been associated with obesity.
It has not been easy for scientists to untangle all the factors and mechanisms that regulated conditions such as obesity, but it seems that there are enough advances in this area. It is not easy for people with problems of obesity to ...understand what is happening with them even if in some cases is a diet and exercise, because getting to change something for which our own brain has already set up pathways and wants to follow...e.g., craving for sugars, is not easy.
I think families and friends that have individual with obesity, shall all cooperate modifying their diet collective. They can do that in such a way that the person who follows a diet, does not feel he/she is on a special diet.
For example, I grew up in a low salt, low sugar diet that included a lot of fresh foods, because that is what was available at home. My mom follows a diet low in salts and we all ate what she cook; if dad cook--his food contain lots of veggies. Later, I found myself cooking and eating law salt and lot of veggies. My pathways were trained that way as a child, and now, I naturally dislike foods that are high in salt, and I enjoy eating fresh food. This does not mean that you wouldn't keep your mind open to try other styles of food, but somewhat if you start educating the children, obesity caused by inadequate diets could be prevented, while the other more resistant types would require medical intervention.
Help your kids develop good eating habits,
© 2011 MSantana