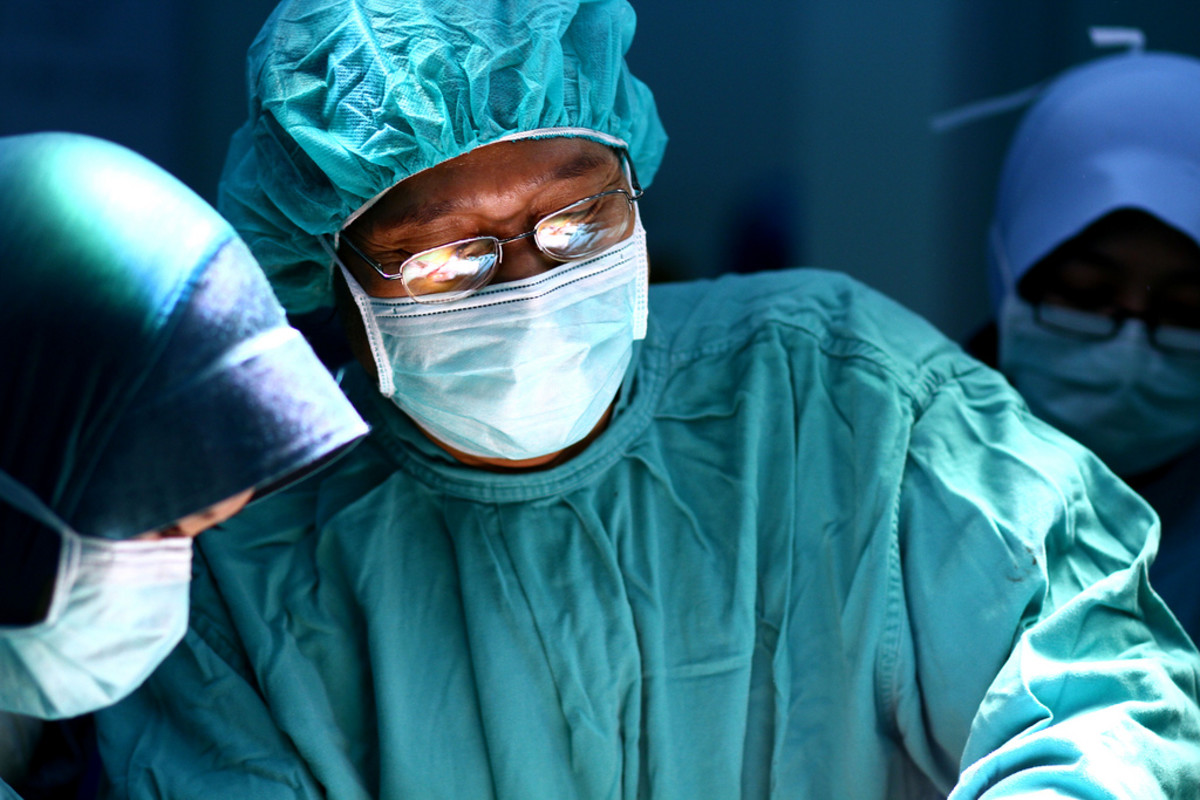
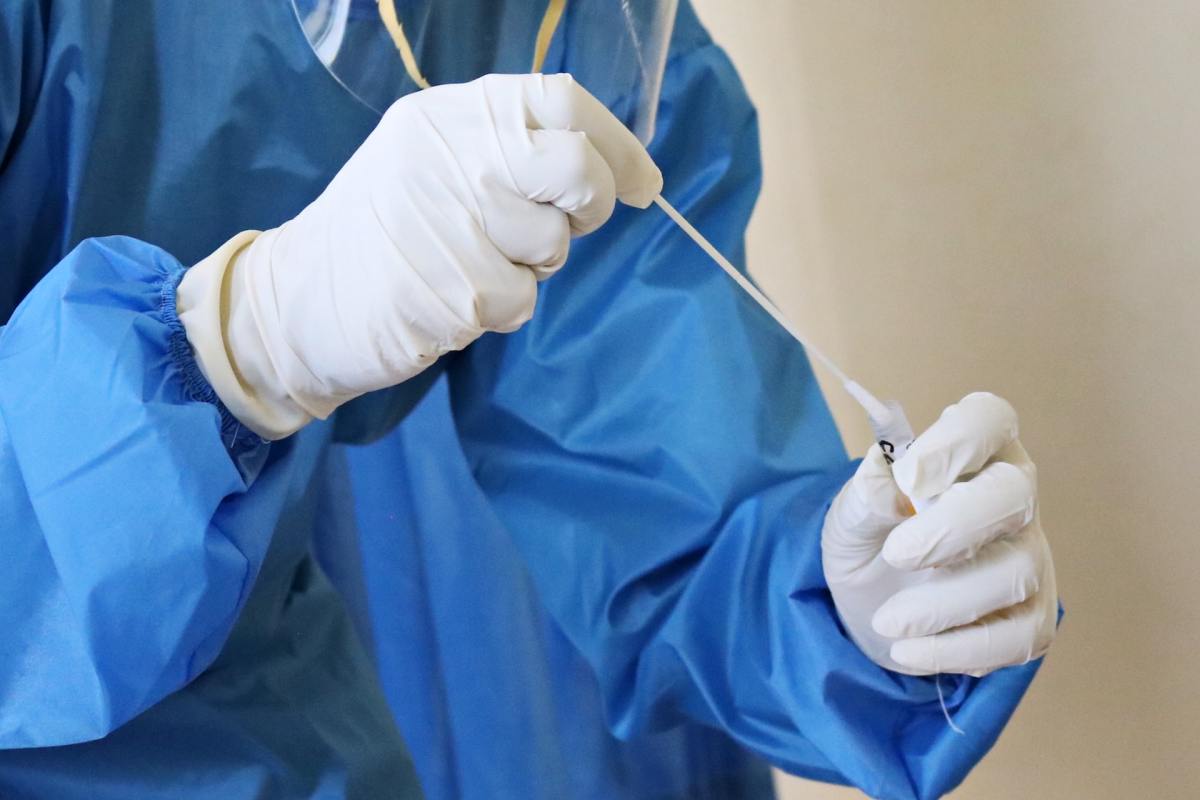
How to be a Medical Advocate
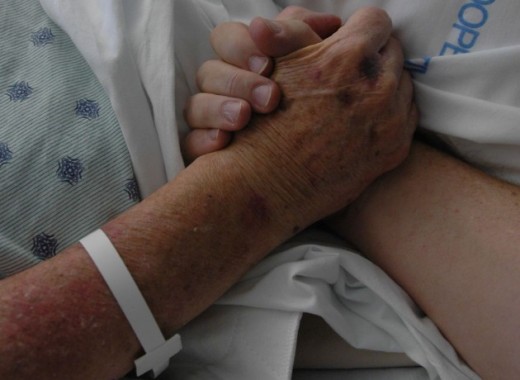
The role of medical advocate can be both personal, as in self-advocacy, or on behalf of someone else, for example a friend or family member. There are many private medical advocates available for hire as well. This article explains the role of the medical advocate, and provides tips on how to be an effective patient advocate, for yourself or someone else.
Thanks to Google and internet research, people are taking a more proactive role in their health than ever before. However, the internet can in no way replicate the information obtained during a physical health assessment. Likewise, taking a lab test result, and using the internet to diagnose its' meaning, excludes the correlating physical symptoms that could completely change that diagnosis. That is not to say that being a "Google Doc" is pointless - knowledge is power - but I would suggest that the primary benefit of learning more about a symptom or disease on the internet is to form better questions; this is where the value of research lies.
In my experience as a critical care nurse, I find that those of Generation X or younger, have a questioning nature and want to be fully informed about their health. I still meet quite a few elderly, those in their 70's and older, who are still willing to accept whatever advice or treatments their physicians present. It is also my experience as a bedside nurse, that it is incredibly frustrating to be called away from my patient to answer numerous phone calls from multiple family members and friends. The solution to this is for the patient to designate one person to be given updates and who is available for meetings with health team members, a medical advocate. While many people can be their own advocates for routine medical visits, I would advise that for appointments with specialists, or when a person is admitted to a hospital for treatment, that someone be carefully chosen for the role of advocate.
Know the Health History!
It never ceases to amaze me when I ask someone what medications they take, and they say something like, "Oh, a blue one in the morning, and the white ones that help me sleep,". The best time to prepare for a medical crisis is before it happens! It is a great idea to type up the Health History and save it on your computer, adding to it as required, and keeping the list of medications current. It can then be printed out and taken to appointments or to the hospital. If you know who your medical advocate will be, it might even be wise to give them a copy.
1. Know the Patient's History
The medical "history" includes significant medical events in a person's life, allergies, current health status, immunization status, and a complete list of current medications. Remember to include:
- childhood illnesses (measles, scarlet fever)
- travel and exposure to any tropical illness
- any accidents or musculoskeletal injuries, especially those that affect current mobility
- chronic disease such as hypertension, diabetes, anemia
- previous surgeries and hospital admissions
- any issues with headaches, vision, memory, speech
- general vision and hearing status: should the patient be wearing glasses before signing any medical forms, can the patient HEAR what the doctor is saying!
- smoking, drug, and alcohol use: current and previous
- special dietary and digestive concerns; recent changes in weight
- allergy history: including specific reactions, and any food allergies
- Medications: name of medication, dose, and frequency. It is imperative that a person understand what medications are prescribed for and any special instructions on how to take them. Don't forget to include medications that are used only occasionally, such as for episodic pain or migraines.
- Names of Family Doctor and any Specialists
- Next of Kin contact information, and whether permission is granted for this person to be given updates on your condition.
- Any specific requests for your care or hospital stay, have you signed an Advanced Directive (stating your wishes for continuing treatment if your prognosis is poor or you have a Cardiac Arrest)
- The Course of Events leading to the current concern/issue: a documented timeline is especially helpful, "On Sunday evening I felt terrible, tired and nauseated, and went to bed early. Monday morning I still felt lousy and went in to see my family doctor who ordered an ECG. I had a phone call from my doctor's office Monday afternoon and they said there were 'ECG changes" and to come in here to Emergency."
Tips for Being an Effective Medical Advocate
1. Have the History!
2. Do some research on the medical issue so that you have a basic understanding of the problem, and start to learn some of the medical lingo! Use reputable internet sites for your research, such as the National Institute of Health www.nih.gov, or the Mayo Clinic www.mayoclinic.org
Ask the primary care physician what sources of information he/she recommends, some doctors even have their own websites that provide information for patients.
3. Ask for a current list of medications the patient is taking. It is expected practice that people are informed of what medications they are given, so if a nurse is busy and says, "Here are your pills," it is ok to say, "Can you tell me what they are."
4. If there is a new diagnosis or the problem will affect the patient's life long-term, see if there are any support groups available. Taking in a lot of information can be overwhelming for a person who is not feeling well. Written materials or videos that a person could view as they are able, or offering to go with the person to a support group, will likely be appreciated.
5. In a hospital, there are a multitude of specialists available. Ask any professional who comes into contact with the patient - physiotherapists, dieticians, nurses, social workers - what they recommend to optimize recovery, most are happy to share this information. Remember the main reason most people choose a medical career is that they like to help people!
6. Take notes! Especially when the MRP (Most Responsible Physician) makes rounds. Remember that unless formal patient meeting has been arranged, the doctors are usually quite busy. It might be a good idea to write out some pertinent questions, both to allow the doctor to consider the answers and get back to you, and also so they don't get forgotten. I make it a habit to ask my patients and their families if they have any questions, so that I am able to ask on their behalf if they forget while the doctor is present. It is a nursing role to advocate for the patient as well, so make sure your nurse knows what it is you are concerned about! Some good questions are:
What is the plan?
What does the treatment/surgery/procedure involve?
What is the expected recovery like?
What follow up care is expected?
What are the common complications?
How many of these operations/procedures have you done? Were they successful?
What are the side effects of this treatment?
What would you do if it were you?
The doctor must explain when obtaining informed consent for an invasive procedure what the risks and benefits are, and usually must quote a mortality risk. The mortality is the likelihood of death as a result of the procedure. Morbidity is associated injury or complication from the procedure, for example, wound infection.
The advocate should take notes during these discussion so that the patient might later review the answers and process them. If this task is overwhelming to the patient or advocate, ask for a nurse to be present who can serve as a communication link between doctor and patient.
Youtube: Doctor learning about patient advocate's role
Recommended Hubs
- Don't Be Your Own Doctor
Medications and health