Alzheimer's - Discussed with other prion protein diseases. Now showing new advances in treatment up to Nov. 2016



Prion Protein Discussion
Prion Protein Discussion This contains all of the original work with new addition research and information added as it occurs.
I had been asked by some friends to write an understandable piece on Alzheimer’s disease and its relationship to other prion protein diseases that affect both humans and animals and if there was any danger of crossover between the species.
It is almost impossible to write such an article without a certain amount of jargon creeping in and towards the end I have tried to explain some of the terms and conclusions reached. If any of you have any particular questions you can ask them through the comments section and I will do my best to answer.
To use a simple analogy, the study of prion protein disease is like someone giving you a 5000-piece jigsaw with no picture on the box. When you open the box there are 5 pieces all of blue sky (i.e. what we know at the moment). All you have to do is discover the remaining 4995 pieces, without knowing what they look like or how they fit together. Just to make it a little more difficult there will be, thrown in, at least, another 5000 pieces (dead ends, unrelated conditions etc, etc) that have absolutely nothing to do with the original prion protein puzzle.
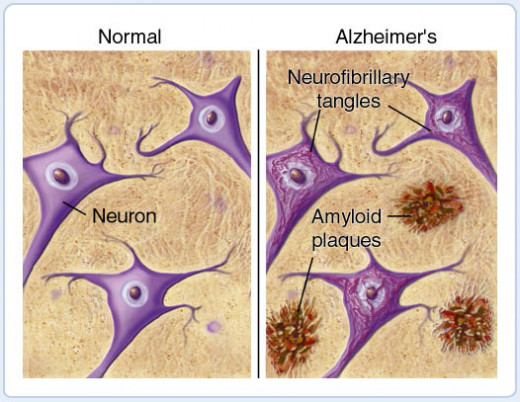
To even diagnose Alzheimer’s, in the initial stages, is pure guesswork as no one can be certain without a post-mortem examination of the brain tissue (looking for amyloid plaques and neurofibrillary tangles), which is a mite difficult on a live patient.
This brings us to a common question “is there such a thing as mild Alzheimer’s ?”
It is a progressive disease, but one that is very difficult to diagnose, with certainty, in the first place. Before anyone can be “suspected” of contracting Alzheimer’s it is necessary to eliminate other, more common, causes of decreased mental capacity. These can be anaemia, vitamin B deficiency, depression, abnormal thyroid levels, or chronic infection of either the liver or kidney. There is a simple urine test to eliminate these under the trade name of AD7C (manf. by Nymox Pharmaceuticals). Memory impairment alone is not sufficient for a diagnosis of Alzheimer’s it must also have one or more of the following present before it can be suspected in the early stages:
Aphasia – difficulty with language
Apraxia – problems with complex movement
Agnosia – difficulty with object identification
Impaired executive function – making everyday decisions
Studies are being carried out on a worldwide basis and the work is too complex to précis into a short comments. As a start, I would recommend looking at the work of Dr Harald Foster, (just type his name into a search engine) who looks closely at food, water treatment and the modern environment, in general, as contributors to the cause and progression of Alzheimer’s.
What can you do to help ? – Well very little if the disease has progressed to the point where the patient is non-co-operative. In the early stages adding magnesium, calcium, Vitamin E and Gingko Biloba supplements may help and interestingly Marijuana has been found to stall the decline from Alzheimer’s. Ibuprofen (400 mg) has been found to delay the progression of Alzheimer’s and would therefore seem the painkiller of choice. For those women considering the use of oestrogen, studies have proved positive in protecting against Alzheimer’s as has drinking 2-3 glasses of wine a day. From a lifestyle point of view try to remove aluminium, in all its forms, from contact with the patient – this includes tap water, cooking utensils, antiperspirants, canned drinks, etc.
New treatments come and go and you may wish to talk to your GP or consultant about any of the following (its suitability will depend on the degree of progression of the disease)
Galantamine (trademarked as RAZADYNE or NEOTROFIN I believe – mostly used in the treatment of mild to moderate)
Tacrine – used to improve memory impairment, but with some side effects
Aricept – as above but less side effects
Exelon – as above
Memantine – as above – good results on moderate to severe.
Reminyl – as above
Neotophin – enhance nerve cell function
Donepezil – cognition enhancement
Cognex – acetylcholineinhibitor
A new urine test may help show if your loved one has Alzheimer's or if the decreased mental capacity may be caused instead by any one of several other possibilities: anemia; vitamin B deficiencies; abnormal thyroid levels; depression; a chronic infection or liver or kidney problems. Your doctor can order and perform the test, and it may be covered by some insurance programs or HMO's. There may soon be other help for Alzheimer's victims as well.
According to an article in the January/February issue of the Saturday Evening Post, a new neural thread protein urine test, AD7C, is being manufactured by Nymox Pharmaceutical Corporation. The test has been available since 2006/2007
I hope some of this may encourage you to investigate further, but always talk to your GP or Consultant first (obviously don’t talk to him about marijuana – just enjoy it !)
We follow on now to look at other forms of prion protein diseases
The following is not intended to be an authoritative reference, but purely a précis of the facts relating to the subject.
It would seem that many people are still confused by the possible relationship between BSE and NvCJD. I have taken the liberty of preparing a brief factual guide to this frightening condition in order that people may understand it better and therefore be in a better position to discuss the implications, possible blame and action needed.
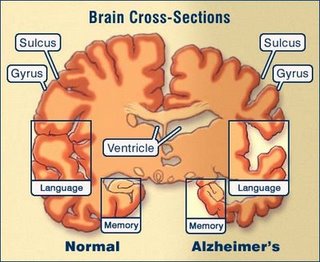
Firstly I think we need to understand just what we are dealing with. Currently the accepted theory is that the agent is a modified component form of a normal cell known as a prion protein. This is a pathogenic protein form that is both less soluble and more resistant to enzyme degradation than normal. Work attributed to Leicester University, describes a prion as an infectious agent which (almost certainly) does not have a nucleic acid genome. It is defined as “small proteinaceous infectious particles which resist inactivation by procedures that modify nucleic acids”. The discovery that proteins alone can transmit an infectious disease has come as a considerable surprise to scientists. Prion diseases are often referred to as spongiform encephalopathies as the brain appears with large vacuoles (holes) in the cortex and cerebellum. The probability is that most mammalian species can develop these diseases. They include:
• Scrapie: sheep
• TME: (transmissible mink encephalopathy): mink
• CWD: (chronic wasting disease): muledeer and elk
• BSE: (bovine spongiform encephalopathy): cattle
In addition humans are susceptible to several prion diseases:
• CJD: Creutzfeld-Jacob Disease.
• NvCJD: new variant Creutzfeld-Jacob Disease
• GSS: Gerstmann-Straussler-Scheinker syndrome.
• FFI: Fatal familial Insomnia
• Kuru
• Alpers Syndrome.
The incidence of sporadic CJD occurs world-wide with roughly even incidences of between 0.5 and 1 per million per year. Higher rates (up to 100 fold) have been reported in Slovakia and Libyan born Israelis, but this is explained by the high incidence of a certain mutation of the PrP gene in these groups. The geographical distribution of CJD in the UK, in the past 25 years, has shown no evidence of spatio-temporal aggregation of cases, despite the occurrence of local areas of relatively high incidence over short periods. There is no evidence of case-to-case transmission and spouses of sporadic cases do not have an increased incidence of the disease. GSS occurs at about 2% of the rate of CJD. It is estimated that 1 in 10,000 people are infected with CJD at the time of death, although these figures are likely to be underestimates as prion disease may be misdiagnosed as other neurological disorders. Alpers syndrome is the name given to prion disease in infants.
Scrapie is a neurological disease of sheep first described in England, France and Germany in the early 18th century. Affected sheep rub their fleece against a tree or building as if it itches – hence the name scrapie. In French it is known as “le remblante” describing the shaking of the animal due to ataxia, another symptom. There are two possible methods of transmission in sheep:
1. Infection of pasture with placental tissue carrying the agent, followed by ingestion, or direct sheep – lamb transmission.
2. That it is not an infectious disease at all, but a genetic disorder that may be eradicated by selective breeding.
However, it has long been known that some genotypes of sheep often develop scrapie and in the UK two genotypes are almost always identified in scrapie-infected sheep. In contrast only one sheep of the genotype Ala136Ala, Arg154Arg, Arg171Arg has been identified with scrapie, these animals being resistant to both scrapie and BSE. Surprisingly the scrapie susceptible genotypes are common in Australia and New Zealand, which is thought to be free of scrapie. Samples of these sheep have been brought back to the UK and quarantined and have not developed scrapie. From this we can conclude that the genotype does not confer scrapie on the animal but rather a susceptibility to scrapie infection. Scrapie would therefore seem to be an infectious disease, not a genetic one. This observation may have implications for families carrying a mutant prion gene. There is no evidence of transmission of scrapie from sheep to man and there is no increased incidence of CJD in countries with scrapie compared to those without (i.e. UK and Australia)
Humans may be infected by prions in two ways:
1. Acquired infection (diet or following medical procedures such as surgery, growth hormone injections, corneal transplants etc), thus implying an infectious agent.
2. Apparent hereditary transmission.
This is one of the features that single-out prion disease, as they are both infectious and hereditary diseases. In addition they can also be sporadic, meaning that there are cases in which there is no risk factor apparent.
H G Creutzfeld is credited with the first description of the disease in 1920 followed in 1921 by a more complete work by another German neurologist A Jacob. At the time the majority of patients were aged between 50 and 75 and it appeared to occur as a predominantly sporadic disorder.
This brings us to Kuru, a condition that was discovered by Zigas & Gajdusek and first brought prion disease to prominence in 1957. A particular tribe in the Fore Highlands of New Guinea, for religious reasons, ingested the brain tissue of dead relatives in the form of a pale grey soup. Clinically Kuru resembles NvCJD. Other tribes in the area with the same habit did not develop the disease. The speculation is that at some point a member of the original tribe developed CJD and it was passed on by the consumption of infected brain tissue. Afflicted tribes were encouraged not to continue with this practice and the disease rapidly declined and is now almost unknown.
In May 1996 an unpublished letter was sent to The Lancet suggesting that NvCJD is a strain of Kuru. The diagnostic characteristics showed that NvCJD had more in common with Kuru than CJD.
In 1998 Dr Bryce Larke, attached to Canadian Blood Services, wrote a paper entitled “The quandary of Creutzfeld-Jacob disease”. In this he discussed the possibility of the transmission of CJD by blood products. The arguments were long and complex and finally inconclusive. However, the suggestion was made that screening for prion disease should be carried out on all blood and blood products.
In June 1997 the USA FDA prohibited the use of mammalian protein in sheep and cattle feed.
It should be remembered that unlike NvCJD, BSE is a relatively new disease. In 1986 a small farm in Surrey reported more than one cow developing a strange neurological disease. The cattle were killed, the brains removed and the animal remains destroyed. When it was found that the cattle had a disease never reported before, the farmer wanted to publish the data, but was told not to, by MAFF. Estimates show that approx. 100 cattle had developed BSE symptoms prior to 1987 and many more would have been infected. It is now suggested that MAFF had been shown cattle with this disease before and may have known about it since 1983, but did nothing. Despite the concern of the farmers, who were receiving less than half the value of their herds, when compulsorily slaughtered, the Government was showing incredible complacency and MAFF quite startling incompetence.
(Update on BSE, CJD and NvCJD)
Earlier I suggested that NvCJD showed a greater similarity to Kuru (epidemic spongiform disease found in Papua New Guinea) than to CJD.
Using research figures and from Collinge, Rossor, Ford, Will et al and Gajdusek, there is more than a passing similarity, which can be demonstrated by the following brief facts:
• Amyloid plaques are rarely present in CJD, but are common in NvCJD and Kuru
• EEC spikes are present in CJD but absent in NvCJD and Kuru
• Age is commonly over 50 in CJD but commonly under 50 in NvCJD and Kuru
• The disease presents itself as dementia in CJD but as ataxia in NvCJD/Kuru
• CJD normally has an incubation period of less than 1 year whereas the others are in excess of that and in the case of Kuru, up to 20 years.
It is therefore becoming increasingly apparent that we need to separate the prion protein diseases BSE and CJD from NvCJD and Kuru and treat them as two distinctly different problems.
From 1979 to 1998 the USA recorded a total of 4751 deaths attributed to CJD (average annual death rate of between 0.78 (1980) rising to 1.13 (1997) per million persons). The median age at death was 68 years, which would support CJD as the cause. However between 1994 and 1997, 101 persons under the age of 55 died and 10 of the deaths were younger than 30 years, which may point to NvCJD or Kuru as the cause. The USA is notoriously sensitive about NvCJD as it continues to claim to be free of the disease. However, it is common knowledge that doctors, pathologists and others are reluctant to carry out autopsy investigations on CJD and/or suspected NvCJD deaths, preferring instead to show Alzheimer’s or normal CJD as the cause of death.
In the period ending December 2000, in the UK a cumulative total of 84 persons had died of either definite or probable NvCJD with a median age of 27.5 years, with a further 20 dying in 2001.
As can be seen, there is a clearly defined age group for CJD and for NvCJD.
What conclusions can we draw from this information ?
1. We know that both BSE and CJD are now recorded and present in every country in the world.
2. We know for sure that NvCJD is unrelated to either BSE or CJD.
3. We know that NvCJD and Kuru exhibit different patterns from other prion protein disease.
4. What possible connection can there be between a prion protein disease (Kuru) known only in Papua and the sudden outbreak of an apparently similar disease on the opposite side of the world?
The short answer is that there is no connection; both are mutations of the PrP, similar in effect but arising from different circumstances. We should understand that prion protein disorders manifest themselves in several diseases – Parkinson’s Disease, Alzheimer’s Disease (“Tau” prion), Motor Neurone Disease (amyotrophic lateral sclerosis). The acquisition of the mutant protein can arise in various ways. In Kuru and TME it is by infection, some, like GSS develop spontaneously by genetic susceptibility or mutation. Both animals and humans have a genetic tendency to acquire the disease, although the suggestion of cross specie infection is patently unproven.
The hypothesis of MAFF/DEFRA that BSE was as a result of infected feed is now totally discredited. The ruminant feed ban enforced in July 1988 has had an insignificant effect on the incidents of BSE. Using figures provided by Dr Sarah Myhill during the BSE enquiry of 1999, cases of BSE were as follows:
1986 – few cases, 1987 – 420, 1988 - 2185, 1989 – 7136, 1990 – 14180, 1991 – 25025, 1992 – 35045, 1993 – 36755(incomp). By Nov 1994 138444 cases had been reported on 31561 farms. Since 1993 figures have started to fall, but Dealler & Kent have shown statistically, that this was due to under-reporting due to a change in the regulations. In addition MAFF made it clear to its own employees, the media, vets and farmers that reported cases of BSE were expected to fall quickly. As a result vets are less willing to diagnose BSE, even when previous cases existed in the same herd and farmers are slaughtering and burying cows, unreported.
We know from MAFF’s own experiments in 1992 that cattle deliberately feed large amounts of BSE infected matter did not develop the disease. In addition cattle kept at MAFF’s experimental farm at Liscombe, developed BSE, even though they were feed no animal protein. Injecting cattle with Scrapie causes spongiform encephalopathy but is clinically and pathologically different to BSE. (Known in the USA as Downer Cow syndrome) In addition injecting sheep with BSE causes spongiform encephalopathy, but this is not Scrapie.
Where does this information lead us ?
Prion protein disease differs from animal specie to other animal specie, both in its form, origin and method of transmission or occurrence of mutation. If we hypothesise that BSE in cattle has only emerged in less than the last two decades (exact dates are unknown as MAFF suppressed the information) and NvCJD in humans was only reported in the same period, then we need to find a common denominator. The clue to this was provided by cattle farmer Mark Purdey, who demonstrated that the common factor might be the compulsory use of “Phosmet”, an organophosphate used to treat lice and warble fly. The work is long and complex, but suffice to say, it provides overwhelming evidence that it causes a mutation of the PrP to a PrPse (the mutant prion), resulting in the symptoms and eventual consequences of both BSE in animals and NvCJD in humans.
Increasingly frantic attempts by MAFF/DEFRA to discredit his work, have themselves proved false and to date the use of such chemicals seems the most likely cause of this devastating epidemic.
How do organophosphates poison the animals ?
We already know that, except in the case of Kuru and TME, infected animal protein in feedstuff does not cause BSE/scrapie. However, organophosphates (OP) are not just used for animal parasite control. They are used in the EC grain mountain to control weevils, but if the dose levels rise too high, the grain is condemned and used as animal feed. Many other foods, used for animal feed, are also treated with OP – these include pulses, nuts, citrus pulp, coffee and cotton waste etc. There are other routes of introduction, OPs were present at high levels in the brains of sheep that had been dipped. In addition the recommended method of sheep dip disposal was to spray it onto grass pasture, where it was eaten by both cattle and sheep. There were more direct methods of exposure where OPs were used in worming bolus, pour-on treatment for lice, warble fly and impregnated fly strips, ear tags, vaporising strips and fly repellent sprays.
“There is now positive correlation between the incidence of BSE and the compulsory treated warble fly scheme.” (Evidence of Dr Sarah Myhill to the BSE enquiry)
We now need to address the implications for humans. Two questions require answers – 1. Can the BSE prion protein be passed directly to humans ? 2. Can neurotoxic chemicals (OPs) stimulate a “de novo” prion disorder in humans ?
Consider the following:
a) Since the beginning of the BSE epidemic in 1986, SDEs (spongiform degenerative encephalopathy) has been recorded in 11 new species of mammal. All of these are either domesticated or zoo animals which are likely to have been exposed to OP chemicals.
b) Research on the transmission of spongiform encephalopathies has been done using injection, not by feed. There is no recorded incidence of cattle acquiring BSE, experimentally via infected feed.
c) Since the start of the BSE epidemic, 5 dairy farmers have contracted BSE. Is this due to exposure to OP chemicals or infected cattle ?
When an animal is diagnosed clinically as having BSE, it is slaughtered and the brain examined for the prion protein. In abt. 80% of clinical cases the prion protein is present and the animal declared as “BSE positive”. However, in 20% of cases there is no prion protein present and the animal declared “BSE negative”. If we accept the OP poisoning theory of Mark Purdey, it can be explained as follows: BSE positive – antenatal OP exposure and BSE negative – post-natal chronic OP poisoning.
With regard to the human implication we should be aware of the following two scenarios:
Degenerative.----------…………-------------- Encephalopathy
Prion present .------------------………-------- Prion absent
Chemically induced or acquired by infection. -----Chemically induced or many other triggers
Invariably fatal. -----……..------------------------Chronic long-term morbidity
Progressive neurodegeneration CJD Effects reversible with approp Treatment
Motor neurone disease (AML) -----…----------CFS/ME (“sheep dip flu”)
Alzheimer’s disease.---------------------...------- Gulf War Syndrome
Parkinson’s disease
In conclusion, it is difficult to produce “acceptable” evidence to support the OP theory of BSE, as MAFF/DEFRA control the research. However, Mark Purdey paid for research to be carried out by Steve Whatley of the Institute of Psychiatry in London with the following result:
Whatley took tissue culture expressing prion protein to which phosmet was added. He demonstrated a phosmet-PrP specific reaction as low as 2ppm. The reaction was proportional to the phosmet dose and involved abnormal movement and distribution of phosmet within cells. “The preliminary results are dramatically positive”.
I was then posed a series of questions concerning the relationship between BSE/Scrapie and NvCJD – here follows my answers:
Discussing and trying to make sense of a subject, such as prion protein disease, is like exploring a labyrinth – paths lead in all directions. Data seems to relate to information or events, but, more often than not, eventually self-disprove. We have facts that point to exciting links, which subsequently lead nowhere or become total non-sequiturs.
This spider’s web of known fact, hypothesis, supposition and just inspired guess-work combines with a cynics view of Government “misinformation” and interpretation of published data to result in an area worthy of further investigation. It is an inescapable fact that the more a Government or commercial company protests and denies, the more likely it is that there is something serious to cover up.
• What is the difference between an amyloid plaque and an EEC spike ?
Amyloid plaque – this appears to be a peptide (an insoluble protein build-up), which stifles surrounding brain cells. It creates neuronal degeneration and inflammation and is commonly found in Alzheimer patients. Dr Alois Alzheimer first observed it in 1906 and the presence of beta-amyloid plaque has been long observed in the brain tissue of those who have died from Alzheimer’s disease. For this reason many cursory post-mortems probably (conveniently) overlook NvCJD as the cause of death and show Alzheimer’s.
EEC spike – this refers to seizures more commonly observed in epilepsy and is often genetic in origin and/or cause.
• So CJD causes mental breakdown and NvCJD/Kuru bodily breakdown.
0Basically yes – ataxia in NvCJD/Kuru is responsible for the clumsy and awkward movements and the degeneration of the spinal cord and nerves. The spinal cord becomes thinner and the nerve cells lose some of their myelin sheath causing “shorting” of the nerve impulses.
• Have they found a cause for Kuru ?
Kuru was first discovered by Zigas & Gajdusek in 1957. A particular tribe in the Fore Highlands of New Guinea, for religious reasons, ingested the brain tissue of dead relatives in the form of a pale grey soup. The speculation is that at some point, a member of the tribe developed CJD and it was passed on, in a mutated form, by the consumption of the infected brain tissue. Interestingly, other tribes in the area, with similar habits, did not develop the disease. The afflicted tribes were discouraged from this practice and the disease rapidly declined and is now almost unknown.
Whilst the practice of consuming infected brain tissue is beyond doubt, current thinking would suggest CJD begets CJD, not a variant similar to NvCJD. Although CJD was first described by H G Creutzfeld in 1920 and more completely by A Jacob in 1921 – would they have suspected a mutated variant in 1957 ? In addition we have the complication that the infected tissue, although consumed as soup, could also have been transmitted directly into the blood stream of those preparing it by the sharp bamboo spikes used in its preparation. In addition there was a massive eruption, in 1911, of a local volcano, which showered the Fore region with black manganese oxide ash, contaminating the food chain. The decline of Kuru may be related to the importation of foodstuff from outside the region.
As you can see, yet more coincidences.
• Why is the current Governmental research still geared to follow the link theory ?
To answer this we must first accept that Mark Purdey’s theory of OP mutation is feasible. The British Government, in 1984 (under the Warble Fly Order) was initially unique in the compulsory use of “Phosmet”, an organophosphate pesticide, which was originally developed as a nerve toxin by the Nazis and is related to Thalidomide of birth defect notoriety. Phosmet was made by Zeneca, (subdivision of ICI) and tellingly a week after HMG first announced the link between BSE and NvCJD, Zeneca sold the patent to a Gowan Company, Yuma, Arizona, presumably to avoid possible legal action. Although compulsory, Mark Purdey did not treat his organic herd with Phosmet, preferring to use natural derris to treat the warble fly, instead. Despite cattle all around him going down with BSE, his cattle remained free of the disease. He bought an infected cow from another herd and treated it by injecting oxime, which is an antidote to pesticide poisoning. The animal showed significant signs of recovery, but before the cure could be effected, MAFF arrived to destroy the animal and removed the carcass.
Although MAFF/DEFRA claim that any credible theory regarding BSE will receive funding, the research into Phosmet has received nothing.
The full theory of Mark Purdey is as follows:
Prions are designed to protect the brain from the oxidising properties of chemicals activated by dangerous agents such as ultraviolet light. When the prions are exposed to too little copper and too much manganese, the manganese replaces the copper that the prion would normally bind to.
BSE appeared in British herds at the same time MAFF banned derris and forced all cattle farmers to treat their animals with an organophosphate pesticide “Phosmet” at far higher doses than anywhere else in the world. The pesticide had to be poured along the line of the spinal cord. It has been proven that Phosmet captures copper and at the same time cattle feed was being supplemented with chicken manure, from birds dosed with manganese to increase egg yield. Thus the prion protein in the cows’ brain were both deprived of copper and dosed with manganese.
Later the use of Phosmet in France first became mandatory in Brittany and 20 of France’s initial 28 cases of BSE emerged there.
There is even a direct correlation with human cases of NvCJD. Of the two main clusters, one was in Kent where huge quantities of organophosphates and manganese-based fungicides are used in the fruit and hop growing areas. The other is in Queniborough, Leicestershire, where a dye works, which used huge quantities of manganese, burnt down spraying chemicals all over the village and had, for years, dumped some of their residues into the sewers. (For further reading on the effects of manganese and humans look at “manganese madness” and “mystery dementia” degenerative brain disease suffered for decades by manganese miners) High levels of manganese are also present in areas of volcanic acid rain, steel, glass, ceramic, dye and munitions factories, lead-free petrol refineries and directly under aircraft runways. In addition we need to take into account silver, another transition metal (in place of manganese) that readily substitutes at copper ligands on prion proteins. Here we find high levels around ski resorts, reservoirs, airport flight paths and coastal districts where silver iodide “cloud seeding” is practised.
• Are these figures drawn from general statistics obtained via death certificates, or from conclusions following researched cases on diagnosis of disease? Could younger people have died from similar disease but gone unrecorded or diagnosed as having some other reason of death?
The figures were taken from US Dept of Health and Human Services. Vital Statistics Mortality Data, Multiple Cause Detail 1979-1998.
The USA has persisted with its denial that neither BSE or NvCJD exists within the United States. It, however, admits that TSEs (transmissible spongiform encephalopathy) does exist in the form of CWD. CWD or chronic wasting disease affects elk or deer and is almost identical in effect to BSE in cattle and this has now spread to 45 states.
In 1985 Dr Richard Marsh (a TSE researcher at the University of Wisconsin) was investigating a mysterious outbreak of TME (transmissible mink encephalopathy). He found that the minks diet comprised almost entirely of “downer” cows i.e. animals too sick to stand (abt 100,000 downer cows die each year in the USA). In 1994 he showed that when the brains of infected downer cows were feed to healthy mink, they developed TME. Worryingly when healthy cattle were injected with infected tissue from TME infected mink; they developed BSE, thus proving the existence of a previously unrecognised TSE infection in cattle in the USA. The symptoms of USA BSE like disease are, however, different to UK BSE. In the USA they simply collapse whereas in the UK they are skittish and crazy before death. In 1990 in Texas, healthy cows were injected with USA sheep scrapie infected tissue and developed BSE, became lethargic and staggered to their death, just like “downer” cows. Despite the USDA describing their testing programme as “aggressive” Drs Gibbs, Prusiner and Gambetti (eminent in their field of prion protein disease) all agree that BSE exists in the USA. 37 million animals are slaughtered each year, for consumption in the USA and less than 1000 are tested – wholly inadequate.
CWD predates BSE significantly and the first cases were noted in Colorado in the 1960s. In the wild, the disease spreads slowly through the herds, but the trading of animals between game farms has accelerated the spread substantially. In December 1999 the USDA started to look specifically at the deaths from CJD among the deer hunters. Hunters in the over 50 age group do not raise any undue alarm, but the recent deaths of four young hunters in their 20s certainly does.
This does leave an unanswered question – if we accept that in the case of UK BSE/NvCJD the most likely cause was mutation brought about by Phosmet/manganese, then what was the cause in the USA variant ? We should not throw out Mark Purdey’s theory, because we do seem to be comparing two different diseases, sharing only a mutation of the PrP gene as the common factor. However, one similarity they share is again manganese. Wild deer and elk, at certain times of the year feed on pine needles which can store large amounts of manganese – despite annual blanket culling, deaths from CWD continues unabated.
We can also see scrapie clusters in Iceland where altitude and melting snow acidify the soil causing manganese (200 mg/kg) to be more readily available in the food chain. Hereditary CJD (BSE type) has been known in Slovakia for generations; here they brew a tea from pine needles, which, together with soil figures, gave a reading of 951 mg/kg. A nearby village Poprad, gave figures of only 59 mg/kg and had no recorded cases. For Britain, figures to date (July 2002) show that there have been NO instances of BSE or NvCJD on organic farms (nor were they afflicted with Foot and Mouth). Some use meat meal in small quantities, but none use pour on organophosphates.
•. The only additional comments I would have is that USDA have not published the results of any post mortems. The US Environmental Protection agency is reviewing Phosmet’s safety and the US Centers for Disease Control, in experiments on mice, have confirmed the organophosphate risk. They also have “enhanced” its CJD surveillance unit using mortality data from 1979-1998. In addition it is investigating deaths of CJD victims below the age of 55 and has established the National Prion Disease Pathology Surveillance Center in collaboration with the American Association of Neuropathologists.
• When did the research start in the UK ? USA shows recorded deaths from 1979-1998, but the figures for the UK only mentions the period ending 2000.
BSE was first officially diagnosed in November 1986, but it is known that MAFF was aware of a previously unknown prion protein disease since before 1982 and probably as early as the 1970s, and had suppressed the information. In February 1989 the Southwood Committee published a report blaming the inclusion of scrapie infected meat into cattle feed, as a result of the changes to rending processes in the late 1970s. On the basis of the “infected feed” hypothesis, they recommended a ruminant protein feed ban claiming that BSE would decline to a “very low” incidence by 1996 and subsequently disappear.
With regard to CJD, people have been dying, throughout the world, of this disease since before it was identified in 1920. However, to coincide with the official diagnosis of BSE and its claimed jump to NvCJD, the National CJD Surveillance Unit was set up in Edinburgh to monitor CJD deaths in the UK and they publish figures from 1985. According to their figures the first confirmed deaths from NvCJD was 1995.
The following may answer some questions raised by the foregoing:
• Where was this (BSE and CJD) first recorded or discovered ?
BSE – November 1986 – UK
CJD – 1920/1 – Germany
• Due to the findings of Amyloid Plaques or EEC spikes present on post mortem examination samples ?
Yes, but not restricted to just these two findings. Work is progressing to discover a test for BSE, CJD and NvCJD, which can be carried out while the subject is still alive.
• One causing dementia and the other ataxia ?
Yes – however, it is reported that in the cases of NvCJD and Kuru there are commonly three stages. 1. Exaggerated startle response and emotional instability with pathological bursts of laughter. 2. Advanced states are characterised by dementia. 3. In the terminal state the patient is generally totally placid, mute and unresponsive.
• Surely the $1 million question ? Could exports of people or produce from other Countries be a contributory factor ?
I have to say that is unlikely to be that simple. It is more a matter of the environment, man-made chemical pollution or interference and/or genetics.
• Is there much research into the trigger ?
The answer to this is mostly covered above.
• How ? Can you explain a little more about the mutation of the PrP to a PrPse please ?
Purdey predicts that OP chemicals phosphorylate either the serine hydroxyl site of the “normal” prion (PrP) molecule (or possibly active sites on glycine or tyrosine) which, after ageing, is converted into PrPsc i.e. the mutant prion. (sorry in my original piece I notice a typo and referred to it as PrPse – which is incorrect.) It is well known that OPs will invoke protease resistance by phosphorylation of the serine active site on several other proteins, such as cholinesterase – indeed this is its mode of action as an anticholinesterase. The next stage is to demonstrate protease resistance of this new OP-PrP complex. However this is not possible, in the UK, for any independent laboratory to continue the work, as all research work is licensed by the Central Veterinary Laboratories and they only allow in house research !
• (Kuru and TME) Bit more please ??.. Lost again.
This should have been explained in the Kuru info above.
• Yes! So are you suggesting ………….
Essentially yes, but I am pointing out that organophosphates are present in both our food and the animals, without the more obvious pour-on applications (incl. Anti-lice hair shampoo in children)
• “de novo”
Means new or from the beginning. In this instance it is suggesting that neurotoxic chemicals can stimulate a previously unknown or new prion disorder.
• What caused the symptoms in the 20% negative cows ? Or was this testing as a result of the OTMS.
Clinically and pathologically, BSE is remarkably similar to chronic OP poisoning. In addition neuronal damage caused by chronic OP exposure is very similar to that caused by BSE e.g. degenerative cells or ballooning vacuoles in the neurones. There are many other features common to both BSE and OP poisoning. In many instances the effect of OP poisoning can be reversed, but as mentioned above there is no test, currently, to identify BSE/OP in the living animal.
• Can you explain tissue culture “expressing prion protein” please ?
Not all tissue from the animal will contain prion protein, it is concentrated in a particular area in the nervous system and rather than saying “we used the bit with the prion protein in” it is shorter to use the more pompous phrase.
We should now take a look at some natural remedies to help and later on details of new treatments.
Great assistance can be given to sufferers and their carers by the use of essential oils and for suitable formulas please see my hubs on depression and stress.
Where advanced sufferers are concerned the creation of a relaxed atmosphere will be great comfort to them. The use of Lavender, Rose, Rose Geranium and Ylang Ylang in a burner or better still in an essential oil fan will provide a comfortable peace which may help those who are agitated.
The best oils to stimulate the mind and improve the memory are Rosemary and Peppermint and they can be used alternately with the essential oils above which are for relaxation.
Some work was done in another form of aromatherapy by introducing aromas that may stimulate a response. Pine Oil was used to simulate a forest, Gum Turpentine to simulate a carpenters shop, Rose Oil for a garden (or other floral scents depending on the patients preference) even such odours as Fish Oil, Leather, Motor Oil etc. The possibilities are endless and can be tailored to the patient’s previous life.
Essential oils were used as a trial with severely mentally handicapped patients who were suffering from deafness, blindness and severe mental disturbance. The dramatic effect was quite startling, back and abdomen massage resulted in calmness, relaxation and some interaction not previously seen for a long while. Interestingly the fragrance of the oils seems to calm the other patients as well.
Choline – This is used by the body in the production of acetylcholine which is a neuro-transmitter. Low levels have been detected in persons suffering from aging and memory loss. Back in the 1970s it was demonstrated that the brains of Alzheimer’s patients showed dramatically reduced levels of the enzyme, in the liver, needed to make acetylcholine from the diet. It is available as a supplement Choline Bicartrate or Phosphatidy-choline and the dose should be 500mg per day.
Another product similar to Choline is DMAE which is used to help patients suffering from autism to dementia and impaired memory loss. It improves the mood and mental alertness. Dosage is not every day but as needed when a 500mg table once per day can be taken.
Gotu Kola – This is an Indian Ayurvedic herb which supports circulation and can help improve memory and cognitive performance. It contains compounds known as sugar esters (asiaticciosides) which help protect the neurons from beta amyloid toxicity (present in Alzheimer’s) It’s also a sedative and anti-convulsive and rich source of vitamin B5. (Take care as it can increase the blood glucose levels in diabetics).
Huperzine A – This is a Chinese herb which has been used extensively in China for the treatment of Alzheimer’s. It is an extract from the plant Club Moss (Huperzia Serrata) and the compound has been used to treat over 100,000 patients by the Shanghai Institute of Materia Medica. In a trial of 50 Alzheimer’s patients, who were given a dose of 200mcg of Huperzine for 8 weeks, 29 showed significant improvements in memory and cognitive and behavioural function based on the international testing standards Weshsler memory scale and Hasegawa dementia scale. It works in the same way as conventional drugs by preventing the breakdown of acetylcholine.
Ginkgo Biloba – This is a much abused Chinese herb which is often suggested for just about every condition known to man. It does, however, have a serious and proven use in the treatment of Alzheimer’s, by helping memory loss and depression. In recent trials a Ginkgo extract was given to 50 patients suffering from chronic cerebral arterial insufficiency. The result was that it could help delay or even reverse the mental deterioration associated with early Alzheimer’s. It works in several ways by enhancing the uptake of oxygen and the use of glucose in the brain. It can also make the platelets less sticky and prevent clotting. It also improves the nerve transmission rate, improves the synthesis of chemicals in the brain and normalises the acetylcholine receptors in the hippocampus. The dosage should be 180mg of standardised extract. To improve the performance make up the Ginkgo as a tea with additional Sage (put 1 or 2 sage leaves into 150ml boiling water for 5 to 10mins then add the Ginkgo – take 3 times per day. ) Obviously allow to cool before drinking. Do not take these teas at the same time as conventional medicine and do not use if you are taking Warfarin.
The following covers further advances in the detection, treatment and coping with Alzheimer’s
Dogs for Dementia Victims - In the short term students from Glasgow School of Art had the brainchild to train dogs to work with dementia victims and their careers. These "dementia dogs" have been trained to help people with early-stage dementia reminding them to take their medicine and help them get out and about. With the support of Alzheimer Scotland, Dogs for the Disabled and Guide Dogs Scotland, Golden retriever Oscar and Labrador Kaspa underwent 18 months of training and have now been working with their new owners for four months. Their training includes responding to alarms and bringing medicine pouches, nudging their owners to read a reminders and making sure they get out of bed in the morning. Unusually the idea came from students at Glasgow's School of Art. They were asked to come up with products to help people with dementia. Alzheimer Scotland worked with Banbury-based Dogs for the Disabled and Guide Dogs Scotland to identify suitable couples and dogs, with some extra funding from the Design Council and the Scottish government. The first two dogs have proved such a success that two more are already undergoing training and the charities involved say dementia dogs could be a significant new way of helping people with early-stage dementia.
Blood tests for Alzheimer’s disease - Alzheimer's becomes more of a problem as people tend to live longer. In July 2013 research was carried out at Saarland University, in Germany into developing a blood test that could diagnose Alzheimer's disease. At the moment there is no definitive test for the brain-wasting disease and doctors rely on cognition tests and brain scans. The blood tests are based on tiny fragments of genetic material floating in the blood and could be used to identify patients suffering from or likely to suffer from the disease. The success rate was excellent and found to be accurate 93% of the time in trials on 202 people. The earlier the disease can be detected the earlier the treatment can start perhaps years before symptoms appear and before large parts of the brain are destroyed.
The University team, analysed 140 microRNAs (fragments of genetic code) in patients known to have Alzheimer's disease and also in healthy people. They found 12 microRNAs in the blood which were present in markedly different levels in people with Alzheimer's. These became the basis of their test with early trials showed it was "able to distinguish with high diagnostic accuracies between Alzheimer's disease patients and healthy" people.
However, more research is needed to improve accuracy and allow it to work at hospital level before the test would be considered as a way of diagnosing patients.
DDT
In addition to the known link to organophosphate another pesticide has been shown to increase the chances of developing Alzheimer's disease, research in the USA has discovered.
The study, published in JAMA Neurology, indicated that patients suffering with Alzheimer's had around four times as much DDT present in the body as a normal healthy person.
DDT was an amazingly successful pesticide, initially used to control malaria at the end of World War Two and then to protect crops in commercial agriculture Whilst rarely used these days some third world countries still use the pesticide as the only affordable but successful way to control this deadly disease.
However, some years ago, there were questions about its impact on human health and wider environmental concerns, particularly for predators and it was banned in the US in 1972 and in many other countries. But the World Health Organization still recommends using DDT to keep malaria in check.
The health problems revolve around the fact that DDT (dichloro-diphenyl-trichloroethane) lingers in the human body where it is broken down into DDE (dichloro-diphenyl-dichloroethylene). The research team at Rutgers University and Emory University tested levels of DDE in the blood of 86 people with Alzheimer's disease and compared the results with 79 healthy people of a similar age and background. The results showed that a greater proportion of those with Alzheimer’s have had 3.8 times the level of DDE.
However, the results are not clearly defined as some healthy people had high levels of DDE while some with Alzheimer's had low levels. Importantly, Alzheimer's also significantly predates the use of DDT.
sts that the chemical increases the chance of Alzheimer's and may be involved in the development of amyloid plaques in the brain, a known indicator of the disease, which contribute to the death of brain cells.
Dr Simon Ridley, the head of research at the charity Alzheimer's Research UK, said: "It's important to note that this research relates to DDT, a pesticide that has not been used in the UK since the 1980s. While this small study suggests a possible connection between DDT exposure and Alzheimer's, we don't know whether other factors may account for these results. Much more research would be needed to confirm whether or not this particular pesticide may contribute to the disease."
Alzheimer's Research UK said more evidence was needed to prove DDT had a role in dementia.
Vitamin E
A daily dose of vitamin E could help people with dementia, recent research has discovered.
A study published in the journal JAMA suggests that people with mild to moderate Alzheimer's disease given a high dose of vitamin E had a slower rate of decline than those given a placebo. They were able to carry out everyday tasks for longer and needed significantly less help from carers.
However, The Alzheimer's Society said the dosage was very high and might not be safe.
In the study, 613 people with mild to moderate Alzheimer's disease received one of four drug doses, either a daily dose of vitamin E, a dementia drug treatment known as memantine, a combination of vitamin E and memantine, or placebo.
Changes in their ability to carry out everyday tasks - such as washing or dressing - were measured over an average of two years.
The study found participants receiving vitamin E had slower functional decline than those receiving placebo, with the annual rate of decline reduced by 19%. In addition, those on vitamin E (also known as alpha tocopherol) also needed less help from carers.
"These findings suggest that alpha tocopherol is beneficial in mild to moderate Alzheimer's disease by slowing functional decline and decreasing caregiver burden," said a team led by Dr Maurice Dysken of Minneapolis VA Health Care System.
Commenting on the study, Dr Doug Brown, director of research and development at the Alzheimer's Society, said treatments which can help people with dementia carry out everyday tasks are key to enabling those with the condition to live well for as long as possible. But he said more research was needed to see if vitamin E really does have benefits for people with dementia, and whether it would be safe to be taking such a high dose on a daily basis.
"It is vitally important that people always seek advice from their doctor before considering taking supplements," he said. In this instance, the dosage of vitamin E taken by participants was much higher than the recommended daily allowance and was at a level that could be significantly harmful for some."
Dr Eric Karran, director of research at Alzheimer's Research UK, said the trial suggested vitamin E may modestly slow the decline in day-to-day functioning in people with mild to moderate Alzheimer's, but without having an effect on memory and thinking skills. He said it was too early to recommend vitamin E as a treatment. Until the findings from this trial have been replicated, we would not encourage people to take high doses of vitamin E supplements to try to prevent or treat Alzheimer's," he added.
NvCJD carriers
Twice as many Britons as previously thought could be carrying the human form of "mad cow" disease, variant CJD.
Researchers believe one in 2,000 people in the UK is a carrier of the disease linked to eating contaminated beef.
Their estimate in the BMJ comes from studying more than 32,000 samples of human tissue removed during appendix operations carried out between 2000 and 2012 at 41 hospitals. It remains unclear if any of these carriers will ever develop symptoms.
Early predictions of a vCJD epidemic didn't come to fruition. To date, there have been 177 UK deaths from vCJD. Most of these occurred in the late 90s and early 2000s. There has been only one death in the last two years.
But it appears that relatively few who catch the infectious agent that causes the disease develop symptoms. People can be "silent" carriers for decades and not even know it. The BMJ research identified 16 such carriers out of the thousands of appendix tissue samples studied.
Experts say many vital questions remain unanswered. Since the link between vCJD and bovine spongiform encephalopathy (BSE), known as mad cow disease, was discovered in 1996, there have been strict controls to prevent meat from infected cattle from entering the food chain. However, the average time it takes for the symptoms of vCJD to occur after initial infection is still unclear.
Preventing spread
This means people exposed to infected meat before the food controls were introduced continue to develop variant CJD, and may spread it to others. Experience tells us that the disease could be transmitted from human to human via blood. - In the UK, there have been three reported cases of vCJD associated with a blood transfusion. Blood donor services take measures to ensure blood is not infected but there is no test to screen for vCJD, although and there is currently no cure for the disease.
Dr Graham Jackson, of the MRC Prion Unit at UCL Institute of Neurology, said: "Given the high levels of infection indicated by this research, it is now crucial we establish how many people in the UK harbour that infection in their bloodstream in order to adequately assess the risks of transmission through contaminated blood donations. Studies to develop new blood tests for CJD must remain a priority to assist with screening and protecting the UK blood supply."
Huge advances have been made in stem cell therapy and successes in clinical trials will soon be made available. I will write additional information on this as it becomes available.
I hope this has gone some way towards clarifying the subject and wish to assure any reader that research into both control and even a cure for Alzheimer’s has advanced dramatically in the last few years and that some of this may spin off into other prion protein diseases.
Further research January 2015
A study, recently published, has linked commonly used medicines, including over-the-counter treatments for conditions such as insomnia and hay-fever, to dementia.
All of these types of medication are drugs that have an "anticholinergic" effect and experts say people should not panic or stop taking their prescribed medication. In the US study, (journal JAMA Internal Medicine), higher doses and prolonged use were linked to higher dementia risk in elderly people.
All medicines can have side-effects and anticholinergic-type drugs that block a neurotransmitter called acetylcholine are no exception. Patient information leaflets accompanying such drugs warn of the possibility of reduced attention span and memory problems as well as a dry mouth. However, researchers say people should also be aware that they may be linked to a higher risk of developing dementia.
Dr Shelly Gray, et al, from the University of Washington followed the health of 3,434 people aged 65 and above who had no signs of dementia at the start of the study. They looked at medical and pharmacy records to determine how many of the people had been given a drug with an anticholinergic effect, at what dose and how often and compared this data with subsequent dementia diagnoses over the next decade.
The most commonly identified anticholinergic-type drugs were medicines for treating depression, antihistamines for allergies such as hay-fever or to aid sleep/promote drowsiness, and drugs to treat urinary incontinence. Nearly 20% were drugs that had been bought over-the-counter.
Over the course of the study, 797 of the participants developed dementia. The study estimated that people taking at least 10 mg/day of doxepin (antidepressant), 4 mg/day of diphenhydramine (a sleep aid), or 5 mg/day of oxybutynin (a urinary incontinence drug) for more than three years would be at greater risk of developing dementia. The researchers say doctors and pharmacists might want to take a precautionary approach and offer different treatments instead. And when there is no alternative, they could give the lowest dose for the shortest time possible.
Dr Gray says some of the study participants have agreed to have an autopsy after their death. "We will look at the brain pathology and see if we can find a biological mechanism that might explain our results." Dr Simon Ridley, head of research at Alzheimer's Research UK said the study was interesting but not definitive - there was, he said, no evidence that these drugs cause dementia and Dr Doug Brown, from the UK's Alzheimer's Society, said: "There have been concerns that regular use by older people of certain medications with anticholinergic effects, such as sleep aids and hay-fever treatments, can increase the risk of dementia in certain circumstances, which this study supports" However, it is still unclear whether this is the case and if so, whether the effects seen are a result of long-term use or several episodes of short-term use. More robust research is needed to understand what the potential dangers are, and if some drugs are more likely to have this effect than others. "We would encourage doctors and pharmacists to be aware of this potential link and would advise anyone concerned about this to speak to their GP before stopping any medication." He said the charity was funding more research in this area to better understand any connections between these and other drugs on the development of dementia. The Medicines and Healthcare Products Regulatory Agency, which monitors the safety of medicines in clinical use in the UK, said it would review any new evidence.
New research August 2016
A new drug has been announced which appears to slow the brain's death and preserve mental function in patients with Alzheimer's disease, a new study shows.
But serious scientific questions remain as the drug - LMTX - inexplicably works only in patients not taking other dementia pills.
The results of clinical trials on 891 patients was presented at the Alzheimer's Association International Conference in Toronto.
Overall, the trial - which treated patients for 15 months - was initially a flop, as there appeared to be no benefit to taking LMTX.
However, an analysis on just the 15% of the patients who had not already been taking drugs to help manage their symptoms showed a significant benefit.
In this tiny subset of patients, tests showed thinking power was maintained and MRI scans found the death of brain cells was much reduced.
However, there are certainly too few patients in the sub-group to be certain of the drug's effect.
Dr Serge Gauthier, the director of the Alzheimer's Disease Research Unit at McGill University in Canada, said: "It is both encouraging to see improvements of this magnitude in the standard cognitive and functional tests and reassuring to see the supporting brain scan evidence of a slowing in disease progression”.
"In a field that has been plagued by consistent failures of novel drug candidates in late-stage clinical trials and where there has been no practical therapeutic advance for over a decade, I am excited."
Even the company that manufactures LMTX, TauRX, cannot explain why it might work only in patients not taking other dementia drugs.
Dr David Reynolds, the chief scientific officer at the Alzheimer's Research UK charity, told the BBC News website: "It does worry me as a scientist why it doesn't work with other therapies."
Possible explanations include:
■ the drugs interfere with each other
■ there is something different about the patients not on other medication
■ the small size of the sub-group in the trial means the results may have been fluked
Dr Reynolds added: "The data suggests it is slowing down the disease, but the important caveat is these small numbers. "It is encouraging, but we need more data and will have to run a study with it as just a monotherapy [on its own]. "It will still be a years from reaching patients even assuming it works."
The drug targets one of the key characteristics of Alzheimer’s disease - the build of tangles of the protein tau inside neurons.
It is thought these tangles may be the final stage that leads to the death of brain cells.
The study was eagerly awaited as it was the first to present large-scale data in patients on a drug that prevents tau tangles building up.
Dr Doug Brown, director of research and development at the Alzheimer's Society, said: "While it's disappointing to see another large clinical trial for Alzheimer's disease fail to meet its goal, there appear to have been some striking improvements for the subset of people who took the drug on its own. "After years of failure, we are now starting to see glimmers of hope for dementia drug trials. "The headway being made through research is starting to give a real sense of the possibility that we could one day stop dementia in its tracks."
Copyright Peter Geekie 2013/16
Additional research Sept 2016
A new drug Aducanumab,that destroys the characteristic protein plaques that build up in the brains of patients with Alzheimer's is showing "tantalising" promise, it has been announced..It is still in the early stages of development.but a study in Nature has shown it is safe and hinted that it halts memory decline. Larger scale studies are now under way to fully evaluate the drug's effects.
The build-up of amyloid in the brain has been a treatment target for many years.and this study, of 165 patients, was designed to test if Aducanumab was safe to use.
After a year of treatment, it also showed the higher the dose the stronger the effect on amyloid plaques.The researchers then carried out tests on memory and found "positive effects".However, 40 people dropped out of the study, half because of headaches which were much more common with a higher dosage.
The next phase of research - phase 3 - involves two separate studies. They are recruiting 2,700 patients with very early stage Alzheimer's across North America, Europe and Asia in order to fully test the drug's effect on cognitive decline.
Dr Alfred Sandrock of the biotech company Biogen, which worked with the University of Zurich on the research, said: "Phase 3 really needs to be done and I hope it will confirm what we have seen in this study. One day I could envisage treating people who have no symptoms because if you have amyloid in the brain it's likely you'll develop Alzheimer's one day." Dr David Reynolds, chief scientific officer at Alzheimer's Research UK, said the results provided "tantalising evidence that a new class of drug to treat the disease may be on the horizon".
And Dr James Pickett, head of research at the Alzheimer's Society, added: "What is most compelling is that more amyloid was cleared when people took higher doses of the drug. "No existing treatments for Alzheimer's directly interfere with the disease process and so a drug that actually slows the progress of the disease by clearing amyloid would be a significant step."
Further research to detect NvCJD in October 2016
In October 2016 scientists reported in the journal JAMA Neurology that it was discovered that urine could potentially be used for a quick and simple way to test for CJD or "human mad cow disease", rather than wait for a post mortem result.
The Medical Research Council team say their prototype test still needs honing before it could be used routinely but this is a great improvement as currently there is no easy test available for this rare but fatal brain condition. Instead, doctors have to take a sample of spinal fluid or brain tissue, or wait for a post-mortem after death. What they look for is tell-tale deposits of abnormal proteins called prions, which cause the brain damage.
Building on earlier US work, Dr Graham Jackson and colleagues, from University College London, have now found it is also possible to detect prions in urine which might offer a way to diagnose CJD rapidly and earlier, they say, although there is still no cure.
The study looked at urine samples from 162 people. Of these:
■ 91 were healthy controls
■ 34 had neurological disease that was not thought to be caused by CJD
■ 37 had a diagnosis of CJD (20 of these were sporadic CJD)
The urine test gave no "false-positive" results - meaning it did not falsely suggest there was CJD in any of the patients known not to have the disease. But it was less reliable when it came to detecting actual cases. It accurately detected just under half of the sporadic CJD patients and even fewer of the vCJD patients. The researchers hope they will be able to improve the test further so it can reliably detect all types of CJD.
Dr Jackson said: "Although there is currently no cure for this disease, an accurate and early diagnosis is extremely important for patients and their families. In the future, as trials of potential therapies become available, the earlier a patient can be diagnosed the more effective any treatment is likely to be. This test could be a critical step forward."
To date, more than 2,000 UK people are thought to have died from CJD.
In the UK, a person's lifetime risk for developing sporadic CJD is about one in 5,000.
The current government spending is around £5.5m a year on CJD surveillance and research.
Additional research November 2016
There is recent evidence to suggest that people who experience frequent drops in blood pressure or dizziness when suddenly standing up are at increased risk of dementia. It is suggested that less blood reaches the brain during these moments, leading to brain cell damage over time. Dementia experts say this is a "robust study" and "plausible explanation" that needs further investigation.
However, Charities point out that factors such as smoking carry higher risks. But they say the work adds to growing evidence that changes in blood pressure have an impact on the brain.
Previous studies have linked high blood pressure to types of dementia but in this paper scientists focused on transient periods of low blood pressure - also known as postural hypotension - which become more common in older age. These episodes can sometimes leave people feeling dizzy or give them "head rushes" when standing up suddenly.
Researchers from the Erasmus Medical Center, in the Netherlands, tracked 6,000 people for an average of 15 years and they found those who suffered repeated periods of low blood pressure on standing were more likely to develop dementia in the years that followed.
Researcher Dr Arfan Ikram said: "Even though the effect can be seen as subtle - with an increased risk of about 4% for people with postural hypotension compared to those without it - so many people suffer from postural hypotension as they get older that it could have a significant impact on the burden of dementia across the world." He told the BBC: "If people experience frequent episodes of dizziness on standing, particularly as they get older, they should see their GPs for advice." But he added that young people, who have one-off episodes of dizziness when standing up because of dehydration for example, should not be unduly worried. This is not death sentence'
Professor Tom Dening, from Nottingham University, described the research as "an important study". He added: "The suggestion is that feeling dizzy, which results from a fall in blood pressure, may interfere with the circulation of blood around the brain and that over time, this causes damage which may contribute to dementia. This is a plausible hypothesis and has support from other research. It is possible that something else may be going on." He said: "A dizzy spell is not a death sentence nor does it mean you are certain to develop dementia. On the other hand, if this problem occurs frequently, then it is worth seeing your doctor as there may be remediable causes, for example if you are taking medication it should be reviewed."
Dr Laura Phipps, of the charity Alzheimer's Research UK, said: "While the risks found in this study are reasonably small compared to other known risk factors for dementia, it adds to a growing and complex picture of how blood pressure changes throughout life can impact the brain. As well as maintaining a healthy blood pressure, the best current evidence suggests that not smoking, only drinking in moderation, staying mentally and physically active, eating a balanced diet, and keeping cholesterol levels in check can all help to keep our brains healthy as we age," she said.
Motor Neurone Disease - another prion protein disease
- Motor Neurone Disease - Help with oils, herbs and with Stem Cell therapy.
Motor Neurone Disease (MND) is a very serious disease of the prion protein disease family. There are various ethical pharmaceutical medicines but it can also be helped by a number of natural products including essential oils. It is a prime contender
Common products that can cause Alzheimer's
- There are two common products that can lead to Alzheimer's disease.
Two common products are implicated in causing Alzheimer's and other forms of dementia
BSE infected tallow in power stations
- Serious Alzheimer's infection agent- Contaminated material falling from power station chimneys.
The disposal of BSE infected Tallow by burning in coal-fired power stations raised an unacceptable public risk. Thousands of tonnes of this toxic material was burnt with the infectious fallout landing on densely populated areas. This unburnt material
Space age electronic healing device
- Amazing space age electronic healing device
The Kosmed/Scenar hand held machine seems to offer amazing results in a wide variety of injuries and illnesses. What is it and does it work. Clinical trials seem to back up claims and now in common use in Russian hospitals
Alzheimer's disease - are you confident a cure can be found in the near future ?
How confident are you that a cure can be found quickly ?
© 2012 Peter Geekie










