CD47 - The New Frontier in Cancer Treatment?
Introduction
CD47 is an abbrevation for the protein named Cluster of Differentiation 47. It is coded in the human gene also known as CD47. It is involved in a wide range of cellular functions, both in cell death, or apoptosis, as well as cell growth, or proliferation. It also plays a role in migration and adhesion.
CD47 also functions in several immune responses. For this reason, it is somewhat ironic that it may be one of the reasons many cancers can be so hard to kill. Normal, healthy cells carry this protein, so the immune system recognizes it as a friendly cell and does not attack. Cancer cells carry higher levels of CD47 than healthy cells. The immune system, therefore, does not attack the cancerous cells by itself, because it recognizes the cancer cells as normal body cells. The cancer is able to trick the immune system into leaving it alone. This is why up until now, most cancer treatments apart from resection are hard on the patient. It is often unavoidable to attack your healthy cells as well as the cancer cells. This has been true whether the treatment is systemic, such as chemotherapy, or a more isolated approach like radiation.
Initial Findings and Testing
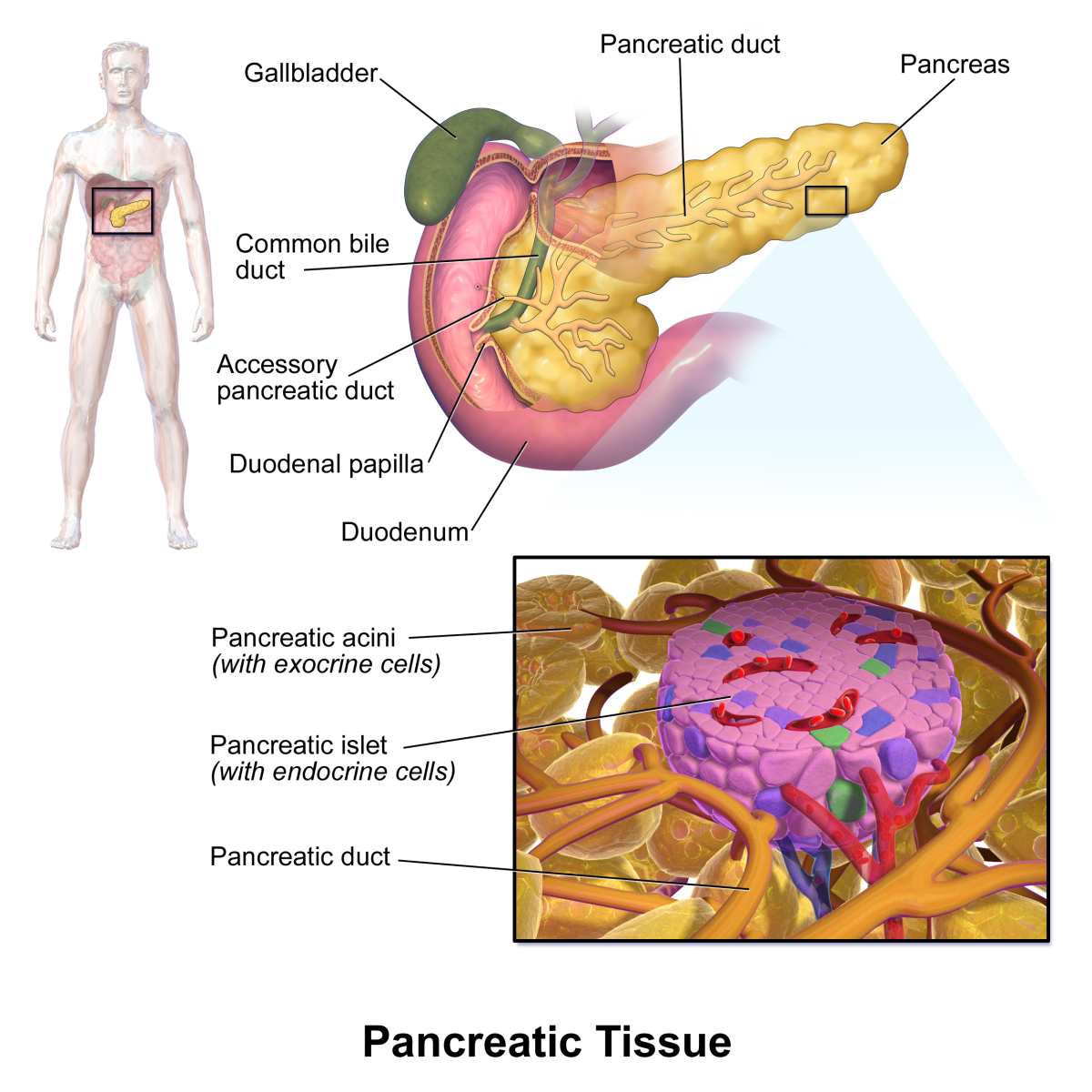
For many years, researchers were convinced that there would never be one cure for all cancers. Many even thought there may even have to be different treatments for the same type of cancer. One of the reasons for this is there is never only one cause or origin of a type of cancer. Pancreatic cancer can be the result of several different types of mutations. The heterogeneity of cancer led scientists toward a relatively new concept called targeted therapy. Because the same cancer can be caused by a wrong expression of a different gene in different individuals, what is effective treatment for one person may not be for another.
Then in the early part of the previous decade, biology researcher Irving Weissman of Stanford found that in blood cancers such as lymphoma and leukemia, the protein CD47 was overexpressed in the cancer cells. As previously stated, CD47 serves as a type of identification code to help macrophages recognize the cell as one of the body’s own. However, the fact that it is also expressed at higher levels in cancer cells enables them to hide from the immune system. A few years after this discovery, in 2007, a CD47 antibody was injected into a mouse that had been injected with human leukemia cells. A day later, the mouse astonishingly had no sign of the disease.
There is a concern to this therapy when injecting it into a human with a human cancer. If the antibody strips the protein from the cancer cell, that it might also strip it away from normal cells as well. In mice, however, this did not happen. The only side effect was a decrease in red blood cells, but no other normal tissues were affected.
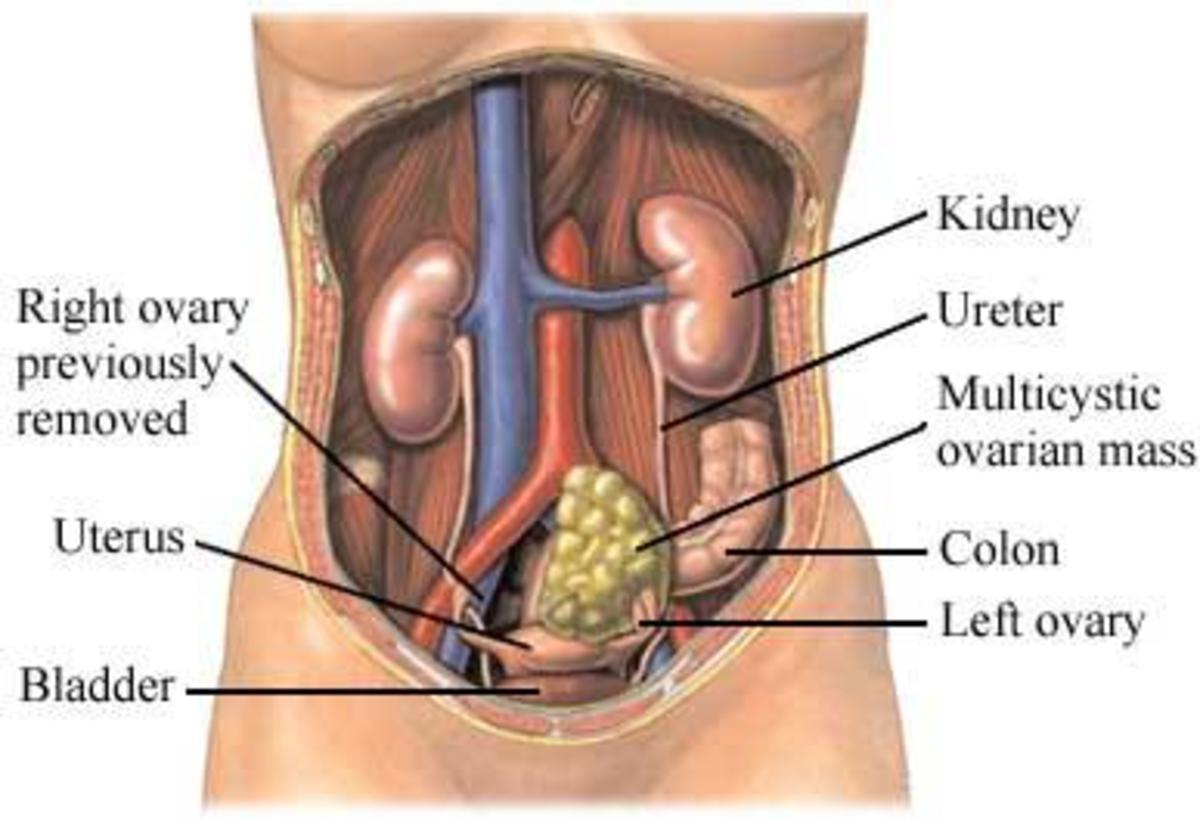
Researchers had hoped and perhaps expected to find the overexpression of the protein in a few other cancers. Their expectations were pleasantly exceeded. The overexpression of CD47 was found in every single type of cancer they tested. Not just blood cancers, but solid tumor cancers such as liver, ovarian, bladder, colon, brain, and prostate. So far, the type of cancers investigated has reached 20, and all are positive for the overexpression of CD47.
When the solid tumor cancers were tested in mice, they experienced similar results. Large solid tumors did not necessarily disappear, but they were shrunk and prevented from metastasizing. Small solid tumors were either shrunk or disappeared altogether. Even if a large tumor is not completely eradicated by the antibody, if it is made smaller and prevented from metastasis, it can then be either resected or further attacked by radiation.
On the Horizon
Stanford has obtained a $20 million grant to pursue this further. At present date, they expect to start human clinical trials in mid 2014. It is necessary for them first to craft a version of the antibody specifically tailored to the human system. The version of the CD47 antibody used in mice is incompatible in humans. Hypothesized levels to inject humans must also be optimized.
If the human system is only capable of taking a certain level of an antibody at any one time, multiple treatments and injections may be required for large tumor burdens. In blood cancers, localization may be a difficulty due to the fact that they have no solid tumors, the cancer cells are spread throughout the blood in the body.
Despite these concerns, researchers seem to be cautiously optimistic that it is possible for this to be a huge breakthrough in cancer treatment. The antibody does not carry the same type of side effects that chemotherapy drugs have. Killing of healthy cells appears to be at a minimum. The initial phase trials will be very telling of how rapid this proposed therapy could advance.