Umbilical Cord Blood
What is Cord Blood?
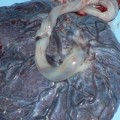
Cord blood is actually short for placental blood or umbilical cord blood. When a baby is born and the umbilical cord is cut, there is some blood that stays in the blood vessels of the placenta and the portion of the umbilical cord that remains attached to it. This cord blood contains red blood cells, white blood cells, platelets and plasma. It is also rich in blood-forming stem cells which are cells that have the ability to transform into just about any human cell. These blood-forming stems cells, also known as hematopoietic progenitor cells (HPCs), are similar to those found in bone marrow.
When a child or small adult has certain diseases, these HPCs can be used to replenish their blood supply with new, healthy cells. The stem cells can also help the body recover from some cancer treatments like chemotherapy or radiation. Only 3 to 5 ounces of cord blood are taken from the cord, and since cord blood has a limited number of stem cells, there is only enough to treat children or small adults.
Cord Blood Collection
Cord blood is collected after a mother gives birth. There is no risk to the mother or the baby since the collection of the cord blood takes place after the delivery. It must be collected within in the first 15 minutes after giving birth. After the cord blood is collected, it is cryopreserved.
At one time, the umbilical cord and placenta which contained cord blood would have been thrown out as medical waste. However, research has shown that cord blood may be used to treat blood diseases and genetic disorders. Thus, the growing trend of cord blood banking.
Cord Blood Banking
The parent of a newborn can choose to store the cord blood. This is known as cord blood banking. It can be done in a public or private blood bank.
Private Cord Blood Banking
Storing cord blood in a private blood bank can be expensive. Banks normally charge around $2,000 for the initial processing fee and then around $125 a year to store the cord blood. The cord blood may then be good for up to ten years. Researchers are unsure at this point how viable the blood cells are after this length of time. When parents decide to store the cord blood privately, they are doing so for their sake of their own child from whom the cord blood came. They make this decision in case their child ends up having a disease that could be potentially treated from the child's own cord blood.
If the parents want to use the cord blood for a family member who gets sick or who is already sick, there is still a 75% chance that the family member would still need a donation from another donor's cells.
Statistics vary but the American Academy of Pediatrics suggests there is only a 1 in 1,000 to 1 in 200,000 chance that a child could be helped or cured by being treated with its own cord blood and that there are very few cases documented of a child receiving its own banked blood for treatment.
According to Stephen Feig, professor of pediatrics at UCLA, "The diseases in children that we can treat with their own cord blood stem cells are really rare."
Public Cord Blood Banking
With public cord blood banking, the parents donate their child's cord blood for free. It can then be used for anyone who might need it. If the cord blood is not used and if the child from whom the cord blood came from gets sick, it would be relatively easy for the parents to get that cord blood back for their child's treatment.
The downside of public cord blood banking is that in most of the country, public donation is not even possible. There are only 19 public collection and storage facilities in the country. Most have agreements with individual hospitals on the East or West coasts, making collection all but unavailable in many other areas.
Besides the low number of public blood banks, most parents do not even know that cord-blood preservation is an option. Only 17 states have laws that require the mothers be told about it.
Another hurdle of public collection is the cost of collection and processing which the blood bank must cover. Despite this, the nation has set a goal of nearly doubling the number of units in the public banking system by 2015, to just under 300,000.
Diseases Treated with Cord Blood
Cord blood has been used to treat more than 70 illnesses over the past two decades, including cancers and blood and immune-system disorders. Besides the following types of diseases there are other potential uses emerging including type 1 diabetes, cerebral palsy, stroke, deafness and pediatric brain injuries.
Diseases Currently Treated with Cord Blood Include:
- Myelodysplastic Syndromes: bone marrow stem cell disorders resulting in ineffective blood production this can progress to acute myeloid leukemia (AML)
- Stem Cell Disorders such as severe aplastic anemia
- Myeloproliferative Disorders: a bone marrow disease in which excess cells are produced
- Lymphoproliferative Disorders such as non-hodgkin's lymphoma and hodgkin's disease
- Phagocyte Disorders or Primary immunodeficiencies in which part of the body's immune system is missing or does not function properly.
- Inherited Platelet Abnormalities
- Histiocytic Disorders
- Inherited Erythrocyte Abnormalities
- Plasma Cell Disorders
- Other Malignancies such as neuroblastoma
Adult and Embryonic Stem Cells
Besides cord blood stem cells, there are also two other kinds of stem cells that are currently being researched and may have the potential to cure other diseases.
Adult Stem Cells
An adult stem cell is thought to be an undifferentiated cell, or a cell that has not yet developed into a specialized cell type. Adult stem cells maintain and repair the tissue in which they are found which includes organs and tissues such as: brain, bone marrow, peripheral blood, blood vessels, skeletal muscle, skin, teeth, heart, gut, liver, ovarian epithelium, and testis.
There is a very small number of stem cells in each tissue, and once removed from the body, their capacity to divide is limited. Scientists are experimenting with ways to make large quantities of stem cells and manipulate them to generate specific cell types.
Some examples of potential treatments include regenerating bone, developing insulin-producing cells for type 1 diabetes, and repairing damaged heart muscle following a heart attack with cardiac muscle cells.
Embryonic Stem Cells (some question if this is an ethical option)
Embryonic stem cells come from embryos. Most embryonic stem cells come from eggs that have been fertilized in vitro. Human embryonic stem cells come from embryos that are usually four or five days old. An embryo at this age is a ball of cells called the blastocyst.
In order to grow embryonic stem cells, the cells are isolated by transferring the cluster of cells inside the blastocyst, otherwise known as the inner cell mass. It is these cells that eventually make the embryo and then the fetus. These cells are put into a culture dish which contains a special kind of nutrient causing them to divide and cells and spread over the dish.
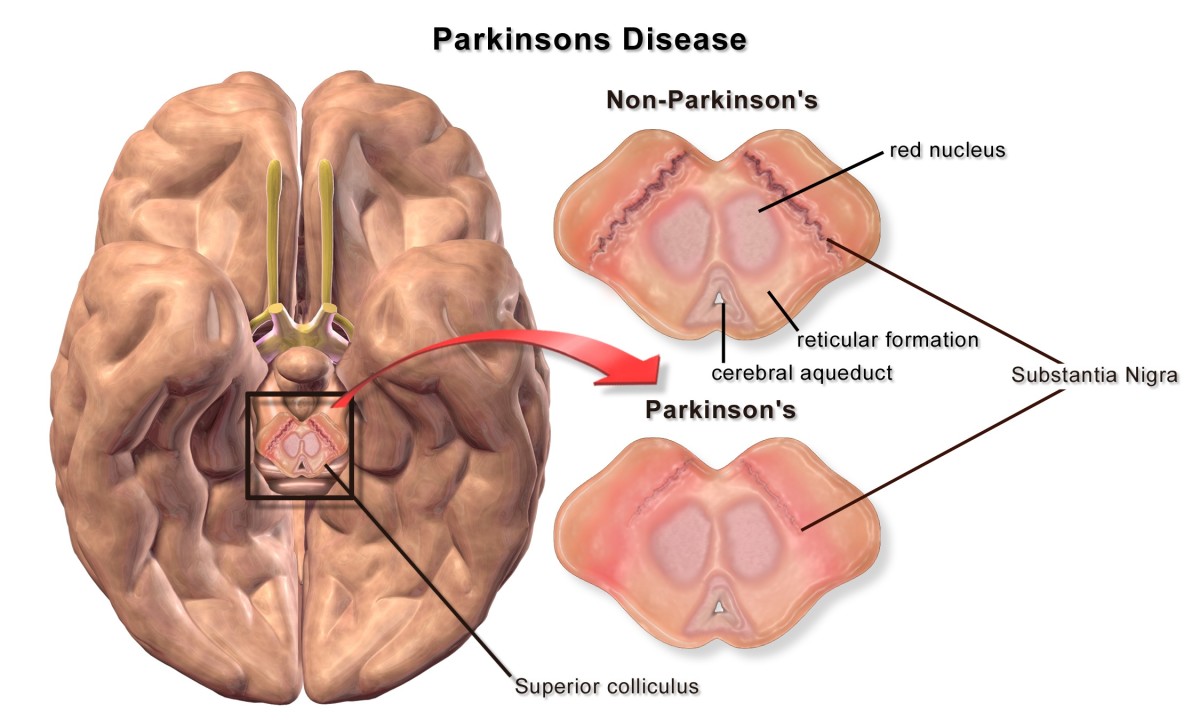
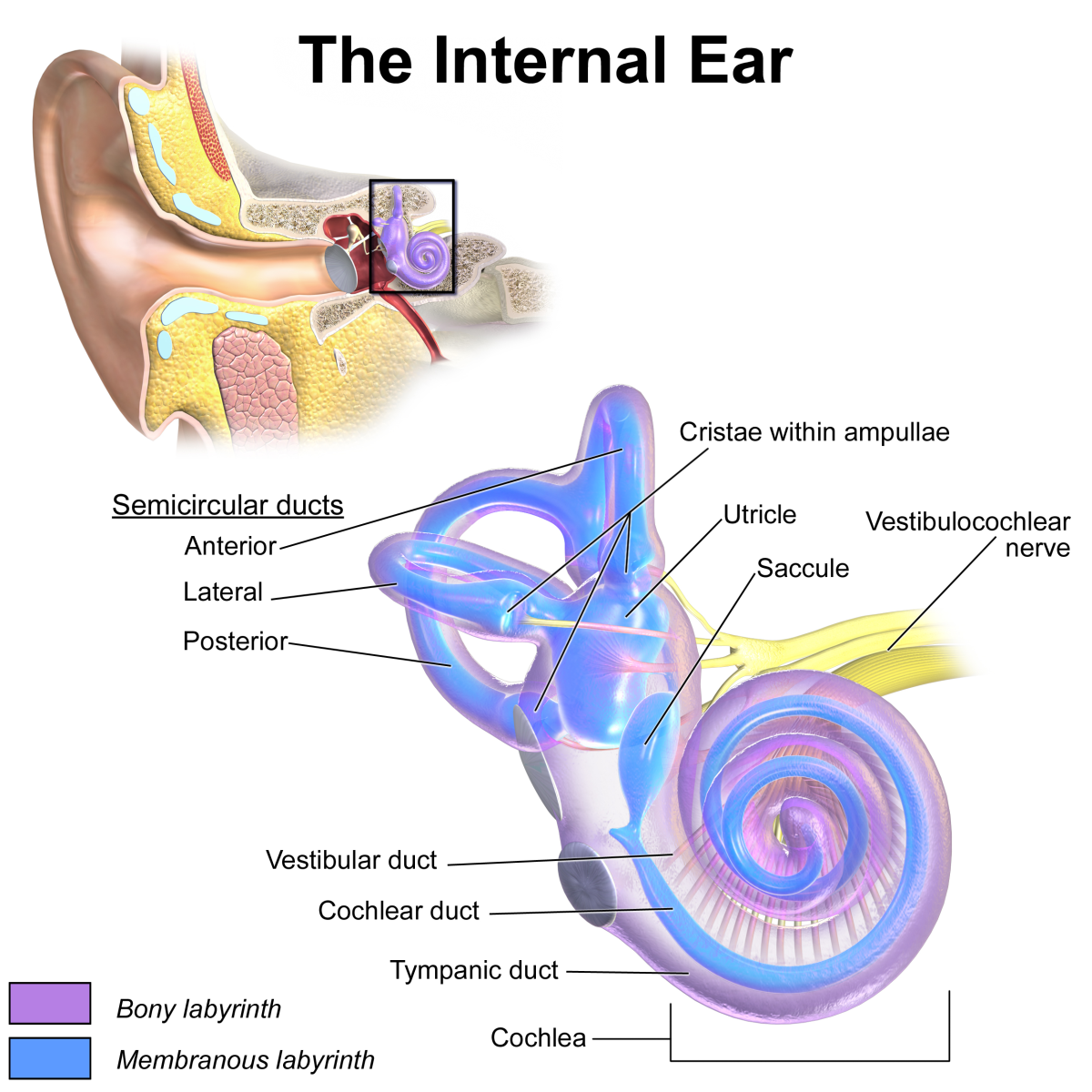
If scientists can reliably cause embryonic stem cells to acquire the feature of a specialized cell such as a heart, diseases that could be treated by transplanting cells generated from human embryonic stem cells include Parkinson's disease, diabetes, traumatic spinal cord injury, heart disease and vision and hearing loss.