Future Treatments for Pancreatic Cancer
Introduction
There have been many advancements that have been made in the treatment of cancer overall. Despite this reality, pancreatic ductal adenocarcinoma is a malignancy that carries among the worst prognosis. It is one of the few cancers whose prognosis has not been markedly improved over the past two decades. The main reasons for this are that it usually remains asymptomatic until it has metastasized. In addition, it also forms proteins that protect the tumor, making it difficult for the chemotherapy drugs to get to the actual cancer cells. These protective proteins are known also as scaffolding.
Currently, only 5% of people diagnosed with pancreatic ductal adenocarcinoma are alive after five years. There are as many as 16 different types and subtypes of pancreatic cancer. Almost all of them are placed into one of two categories, exocrine and endocrine. 95% of pancreatic cancer are exocrine tumors, most commonly adenocarcinoma.
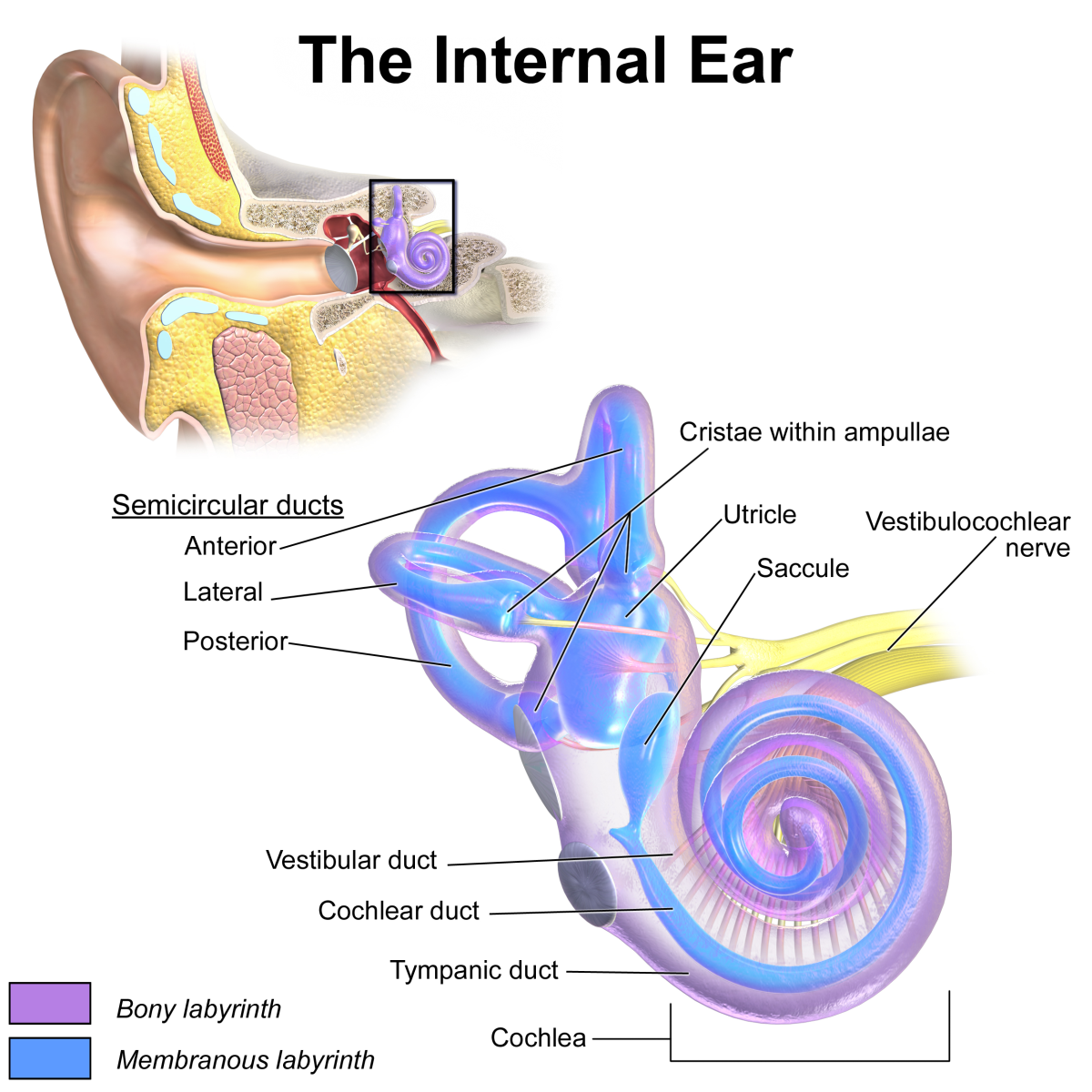
The Pancreas
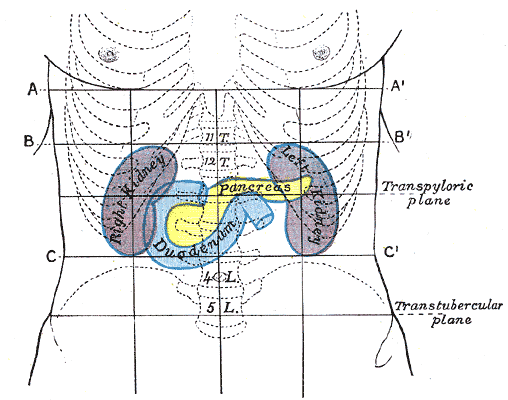
The pancreas is a gland that has two functions. The exocrine cells secrete enzymes into the duodenum. The endocrine cells through ducts called the islets of Langerhans push insulin into the body. It is located behind the stomach, and is connected to the liver and duodenum. It works together with the biliary tree (liver, gall bladder, and duodenum) to produce the enzymes and fluids that digest the food.
Treatments of the Future - Gene and Stem Cell Therapy
In a malignant tumor, there is a small group of cancer cells, called cancer stem cells, that drive the abnormal cell replication and tumor growth. If chemotherapy puts cancer into remission, but these stem cells are not killed, the cancer is very likely to eventually return. These stem cells in the case of pancreatic ductal adenocarcinoma are very resistant to chemotherapy drugs. While they are less than 2% of the cancer cells of the tumor, they are the hardest to kill.
Researchers at the University of Michigan hypothesize that these cancer stem cells are resistant due to a malfunctioning in the expression of a gene called Ataxia Telangiectasia Group D Complementing gene (ATDC). They believe that instead of attacking the stem cells directly, it may be more constructive to target the gene that is causing them to be resistant. If the gene can be repaired, the cancer cells themselves will be more vulnerable to chemotherapy attack.
Immunotherapy
Johns Hopkins is currently working on the development of a pancreatic cancer vaccine. Certain immune cells in the body are unable to detect cancer cells. The vaccine injects pancreatic cancer cells that have been rendered incapable of reproduction through radiation. Their genetic makeup has also been shifted. The altered cells give off a protein that enables the immune cells to spot the cancer cells and tumors, and hence strengthen their ability to attack them.
This vaccine is currently in early phase clinical trials and has showed marked improvement in survival time.

New Drugs
For over a decade, gemcitabine, with the trade name Gemzar, was the only chemotherapy drug available for pancreatic cancer. In most cases it would only modestly prolong life. Increasingly, the understanding of pancreatic cancer as having heterogenous causes that vary with the individual have given rise to using combinations of drugs, as well as drugs that were previously only used for other cancers. Abraxane and Folfirinox, which is actually a combination of four different drugs, have in many cases showed superior results to Gemzar, or when used in combination. Over the next decade, these drugs will more often be a first choice in a chemotherapy attack as opposed to Gemzar, or in addition to Gemzar.
Early Detection Tests
As stated before, one of the main reasons for the poor prognosis of pancreatic cancer is the fact that one usually displays no symptoms until it has already metastasized. Methods of early detection are currently rudimentary and in many cases unreliable.
An extraordinary potential breakthrough came last year at the hands of a 15 year old boy named Jack Andraka. Instead of looking directly for pancreatic cancer cells, he sought to isolate proteins that are biomarkers for cancer formation. He found that a protein called mesothelin was present in all cases. He created a sensor made out of paper with carbon nanotubes that reacted to the presence of mesothelin.