Bacteria: the Good, the Bad, and the Resistant!

Are bacteria to blame?
The body is a natural host to trillions of indigenous (native) microflora, a lot of which are bacteria. Most of the bacteria dwelling on and within the human anatomy are neutral, having no positive or negative effects. In fact, just by occupying space,neutral bacteria are prohibiting disease causing microorganisms from colonizing. [2]
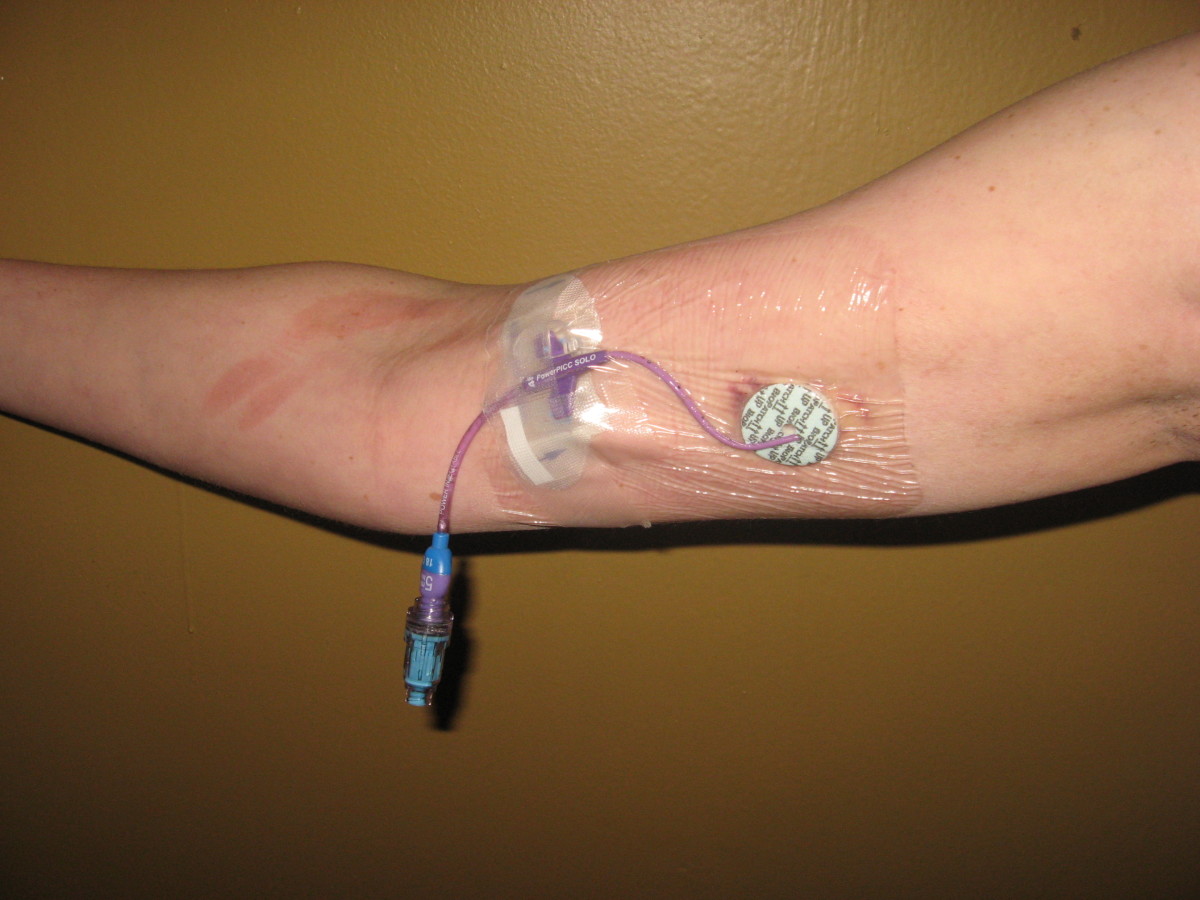
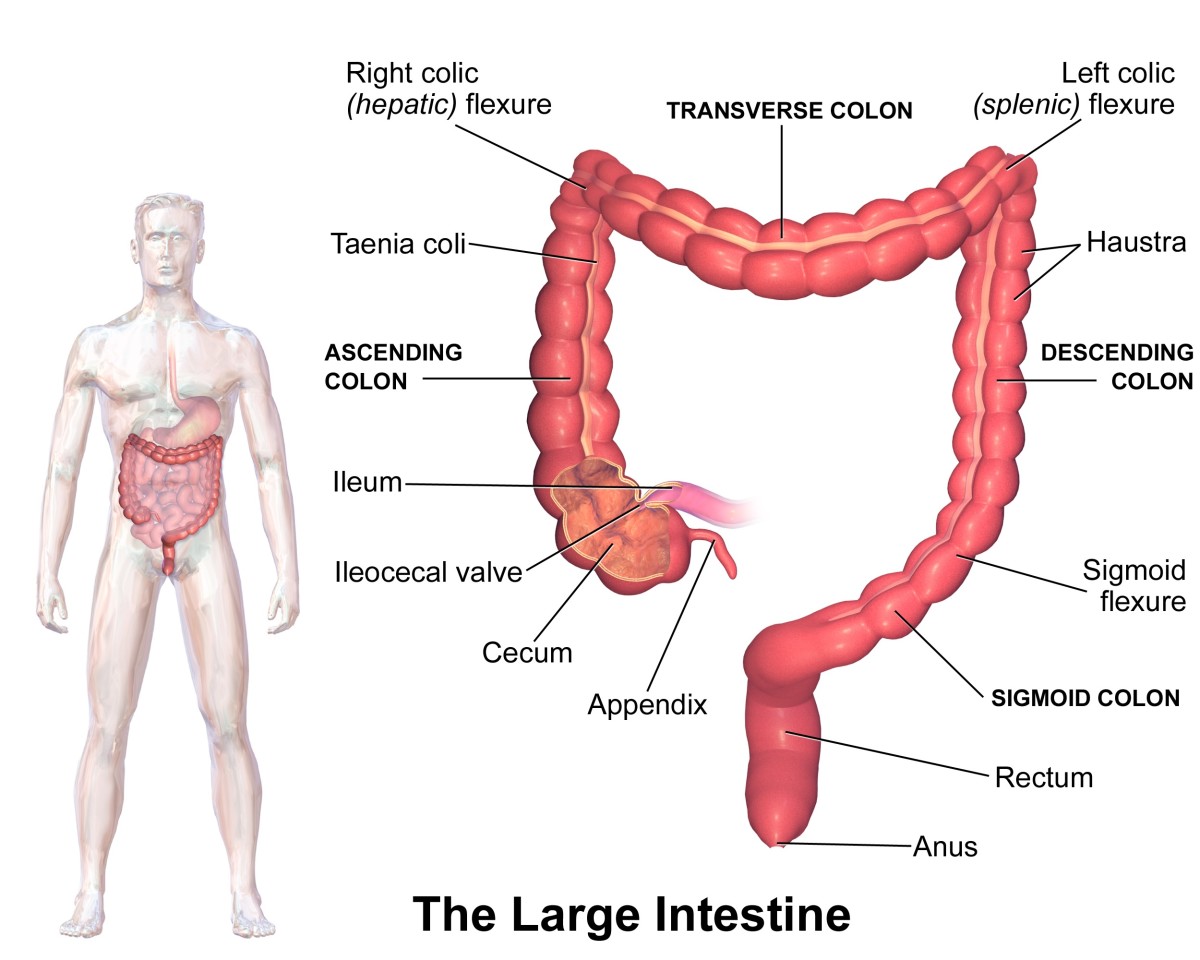
However, not all residential bacteria are neutral. For example, the common gut dwelling bacteria Escherichia coli (E. coli) have both positive and negative effects on the body. While E.coli may synthesize vitamin K, vitamin B12, biotin, pyridoxine acid, and pantothenic acid it is still an opportunistic pathogen (disease causing microorganism). This means that even though E.coli is beneficial to human physiology in a balanced environment, it may become infectious when the scales start to tip. Whether it is caused by a suppressed immune system, a vulnerable surgical wound, or even diarrhea, bacteria like E.coli can quickly turn from friend to foe. [2]
Antibiotic Performance
When patients are sick with either an indigenous or transient (originates outside of the host) bacterial infection, doctors can prescribe them antibiotics. These are drugs that assist and protect the patient's immune system by subduing the pathogenic (disease causing) bacteria.
There are four ways that antibiotics accomplish this:
- They disrupt the development of the bacterial cell wall.
- They interfere with protein synthesis.
- They alter the functions of the cell membrane.
- They stop the production of nucleic acids (RNA and DNA). [3]

Antibiotic Resistance
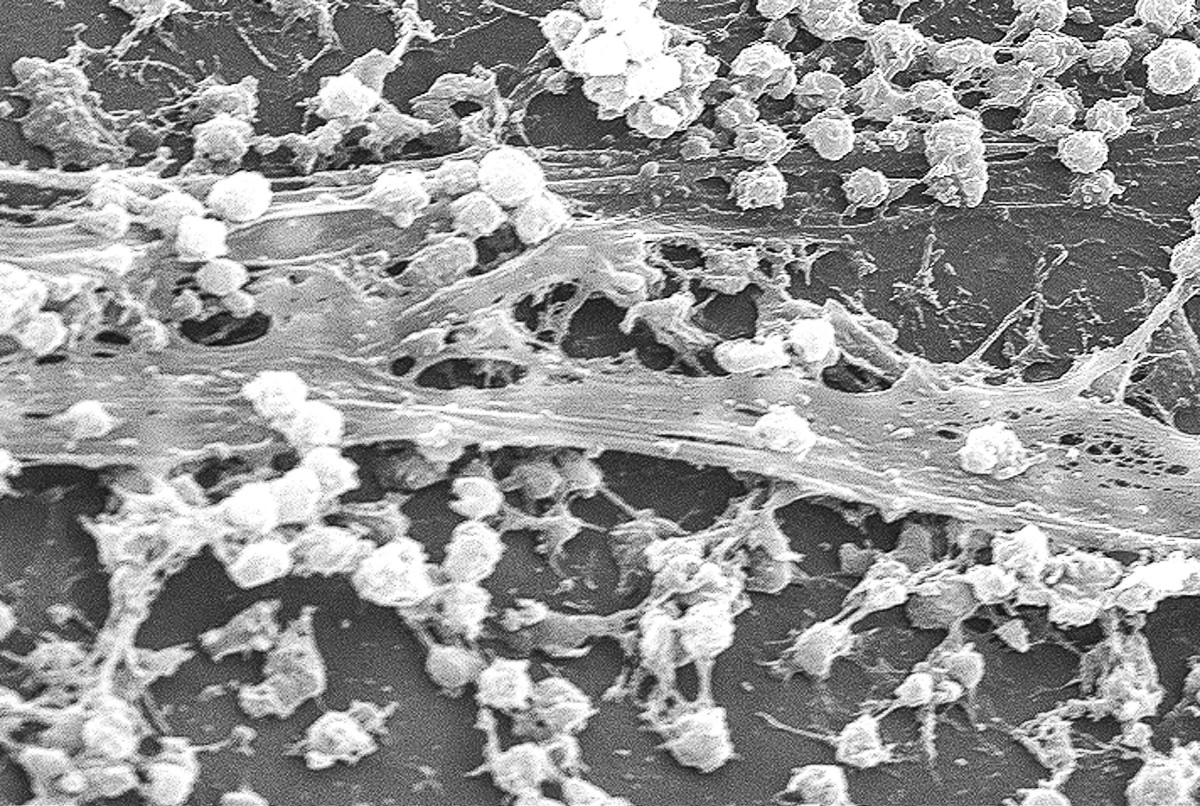
By adapting to the host environment, several bacteria have developed antibiotic resistance. Antibiotic resistance allows the bacteria to oppose the effects of antibiotic therapy.
The bacteria can withstand antibiotics in the following ways:
- Secreting enzymes that deactivate the antibiotic.
- Altering its cell membrane to keep the antibiotic from entering the cell.
- Changing the targeted area of the cell so that the antibiotic cannot affect it.
- Releasing a substance onto the antibiotic that prevents it from reaching the binding site.
When antibiotic resistance occurs, pharmaceutical manufacturers work to develop new forms of the antibiotic that can overcome the bacterial resistance. Unfortunately, sometimes bacteria can evolve too quickly for this to work. [3]
This can have devastating effects on the healthcare community and the general population. For example, Staphylococcus aureus (commonly known as staph) is usually a hospital-acquired infection. Between 1945 and 1950, it was easily treatable by the antibiotic penicillin. Unfortunately, by 1950, 80% of staphylococcus developed resistance. In the early 1960s, methicillin was introduced as an effective drug against staph, but by the late 1960s S.aureus continued to evolve, developing the stronger more resistant strain methicillin resistant S. aureus, also known as MRSA. Staph is precisely responsible for 17 % of postoperative wound infections. [2]
Factors That Contribute to Antibiotic Resistance
There are links between the rapid increase of antibiotic resistant bacteria and the misuse and abuse of antibiotics, allowing mutated strains to survive and reproduce.
Examples of the overexposure of antibiotics include:
- Prescribing antibiotics for viruses.
- Patients not completing their full course of antibiotics.
- Secondary exposure to antibiotics through the food chain and water supply.[3]
MRSA Survey
Have you or someone you know ever been infected with methicillin-resistant Staphylococcus aureus (MRSA)?

So, is my best defense to live in a plastic bubble?
No, you definitely shouldn't live in a plastic bubble. No matter how gross, disgusting, or even frightening the microbial world may seem to us, we rely on it just as much as we defend ourselves from it. My personal advice is to keep yourself educated on what is out there. Know how your body works! Listen to your physicians, and keep your environment clean. Wash your hands, and read your disinfectant labels. Be aware of the thriving micro environment that lives on and within you, and take care of those tiny do-gooders that help us stay healthy! The key to staying healthy is balance.
Washing your hands is your first line of defense against infectious germs! This is how you do it correctly.
Citations
1) ASMacademy. (2014, January). Retrieved from academy.asm.org: http://academy.asm.org/index.php/faq-series/5122-humanmicrobiome
2) Paul Price, C. M. (2003). Microbiology for Surgical Technologists. Clifton Park: Delmar, Cengage Learning.
3) Snyder, K. C., & Keegan, C. (2012). Pharmacology for the Surgical Technologist 3rd Edition. St. Louis, Missouri: Elsevier Inc.