New Cholesterol-Lowering Drugs Can Reduce LDL Cholesterol By 60%

USA Today reported on August 17, 2016 that two promising new drugs recently approved by the FDA called PCSK9 inhibitors can reduce LDL cholesterol by 60%. However, the biggest drawback is the enormous annual price of $14,000 per person. According to USA Today, both pharmacy benefits managers and health insurance companies are balking at the high price.
The Journal of the American Medical Association (JAMA) published an economic analysis of these two new drugs on August 16 estimating that the annual $14,000 price tag per patient would increase USA annual health care costs by $120 billion. The authors questioned how much Americans are willing to pay for improved health. If all patients in need were treated with Praluent or Repatha, the yearly U.S. health spending estimated at $2.8 trillion would increase by as much as 4% which amount is an unacceptable increase for one single medicine.
An Alternative to Statins
PCSK9 inhibitors were approved by the FDA for patients unable to tolerate current popular statins medications because they can’t lower their cholesterol levels using them, or develop liver problems or muscle pain. Statins, also known as HMG-CoA reductase inhibitors, effectively reduce cholesterol and raising low-densite lipoprotein (LDL). Statins decrease the risks of strokes, heart attacks and other arterial disease related to high cholesterol.
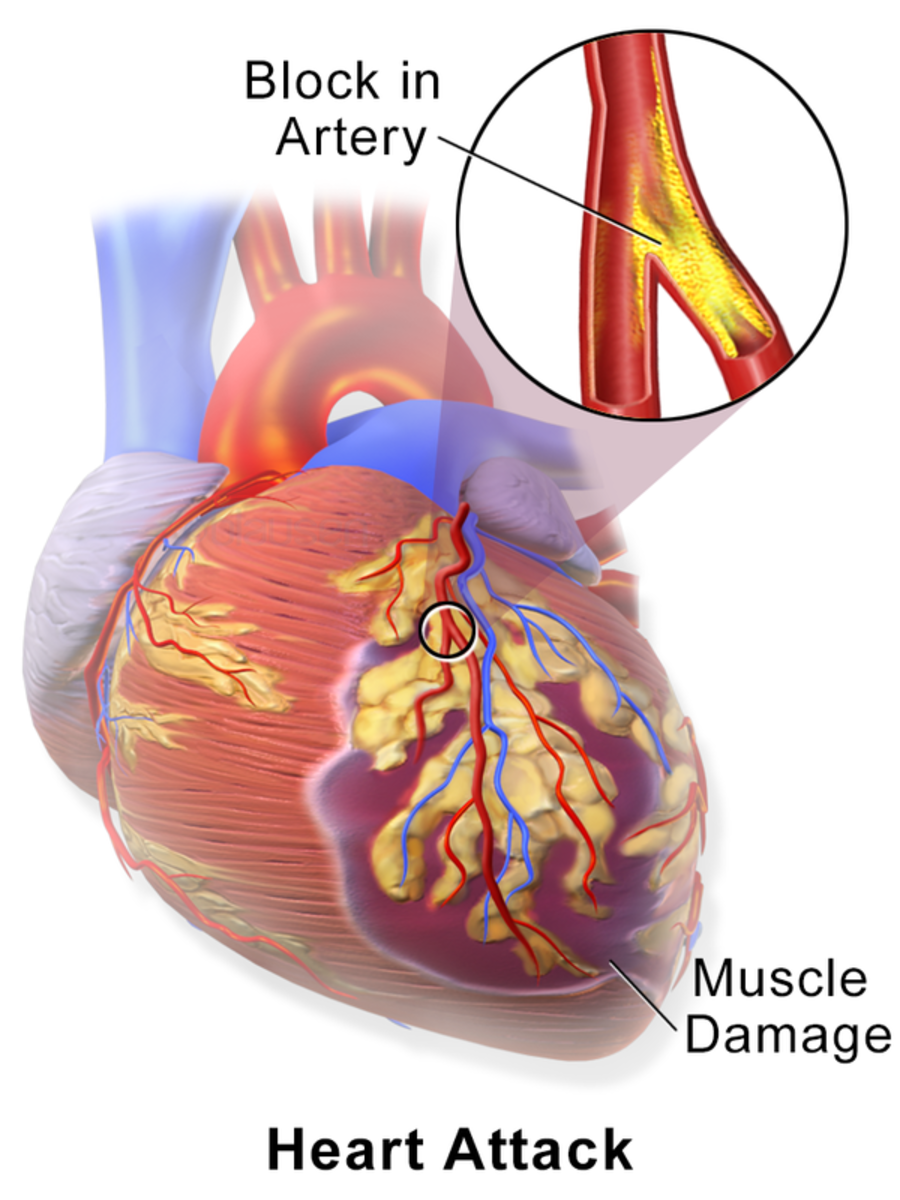
Cholesterol is a waxy, soft material found in all cell membranes and in the blood. Cholesterol is synthesized in the liver after being absorbed from foods. Hypercholesterolemia is the term used to describe high cholesterol levels in the blood which is a major risk for strokes and cardiac diseases because of the plaque formed in arteries leading to blockage of the arteries.
These new drugs are called Repatha, produced by Amgen, and Praluent, manufactured by Sanofi & Regeneron Pharmaceuticals. It is estimated that 9 million Americans between the ages of 35 to 74 can use them. These are the first new type of drugs to lower cholesterol since 1987 when statins were introduced.
The chairman of cardiovascular medicine at the Cleveland Clinic, Steve Nissen, stated that it is still too early to know their full benefits. Therefore, it won’t be known if these new drugs are cost effective yet. While these two drugs can lower cholesterol levels dramatically, an insufficient time exists to know if they prevent strokes and heart attacks.
Insurance Issues
Controversy exists regarding health insurance companies and these two new drugs. Health insurance companies are limiting the usage of these drugs because they believe health care costs will sharply rise, according to a spokesperson for Regeneron, Hala Mirza. According to Mirza, health insurance companies prevented access to around 75% of the patients presenting prescriptions from their physicians for the two drugs.
The Cigna insurance company does provide coverage for both drugs pursuant to an agreement with the drug companies last May. According to Christopher Bradbury, senior vice president of Cigna Pharmacy, both drug companies agreed to a significant initial “discount” to drastically decrease prices if the drugs fail to perform as they did in the clinical trials. Mr. Bradbury manages the customer prescription benefits program for Cigna. In addition, Mr. Bradbury emphasizes the importance to make pharmaceutical companies accountable to make it easier for Cigna to make the drugs available to the most qualified insured.
Cost Effectiveness
Another problem for the two drugs is that they failed a cost effective standard test because their costs are higher than $100,000 for every year a healthy life is saved which measures the quality of a patient’s life. To comply, the drugs will have to reduce their prices by 70% to approximately $4,500 per year making them within proximity of the drugs’ costs in Europe. According to Dhruv Kazi, the lead author of a new study on these two drugs and assistant professor of medicine at the University of California-San Francisco; the European Union (EU) normally negotiates drug prices for their members with drug companies.
In conclusion, more time is needed to evaluate the long term effect of these two new medicines and hopefully in the near future their prices will dramatically decrease to make them affordable. In the meantime, health insurers are reluctant to approve their usage for their insured clients.
This article is accurate and true to the best of the author’s knowledge. Content is for informational or entertainment purposes only and does not substitute for personal counsel or professional advice in business, financial, legal, or technical matters.
© 2016 Steven Rich