Treatment for Porphyria - Glucose
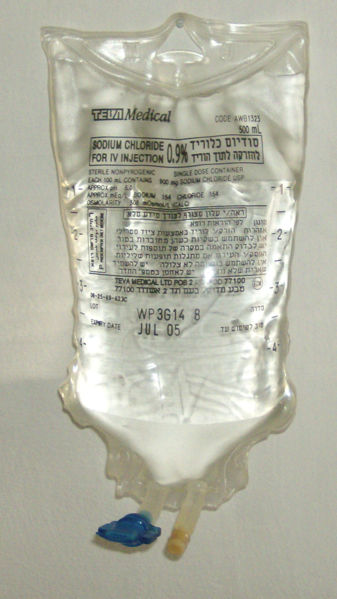
The most often used treatment for porphyria is glucose, either by IV or orally. This helps to limit the number of porpyhrins in the blood stream. Reduced prophyrins and toxins can reduce the intensity of attacks ore keep them from happening in the first place.
How many calories you eat each day should be sufficient to keep an ideal body weight. Just as important, you need the right number of calories in the right proportion of nutrient categories. Patients need to limit heme production while still having a balanced diet.
Patients with porphyria should try to stay within 10 percent of their basal metabolic rate each day. The BMR is how many calories your body burns just in your normal routine for the day before any additional exercise. Your body burns a surprising amount of food just keeping your body temperature up, thinking and processing waste.
Fad diets and aggressive weight loss, especially the low-carb Atkins diet seems to be why there is an increasing number of symptomatic porphyria in the world. People who have had the gene that causes porphyria may not have ever had enough symptomatic attacks to diagnose it were it not for the low-carb diet craze.
Why Does Glucose Help?
Eating carbs partially prevents the synthesis of d-aminolevulinic acid, or ALA. Perhaps this is why people who have porpyhria and eventually contract Type 2 diabetes stop being symptomatic. Type 2 diabetes may also stop ALA synthesis.
Glucose helps give the liver a break on making ATP for cellular energy. With a steady supply of glucose, your liver doesn't need to make as many porphyrins.
How do you get glucose?
First things first, do not count alcoholic beverages as a source of carbohydrates. Besides being a bad thing for your liver anyway, alcohol also stimulates heme production.
A good portion of your carbs for each day should be consumed with breakfast. The time you spend snoozing is time your liver has to make energy using ATP and the associated porphyria toxins with it. You should eat small meals every 2-3 hours instead of 3 main meals. Just like with breakfast, a carb-heavy late dinner should help your liver out overnight.
IV glucose is often used for patients during bad attacks, when you have significant diarrhea and vomiting. During those attacks, your intestinal tract isn't able to absorb glucose well, so you need it by IV.
If your attack isn't that bad and you're keeping food down okay, then liquid glucose shots and chewable tablets or even high-sugar foods are ideal. Stay away from HFCS (High Fructose Corn Syrup) because fructose makes your liver produce heme and porphyrins in order to process it into usable types of sugar.
How Much Glucose Will Stop an Attack?
During an attack, you need about 500 grams of carbohydrates, including a good amount of glucose, each day. Those will often be provided by IV in the form of D10, or 10 percent dextrose. If you are not hospitalized, you can use liquid shots and tablets to get to 500 grams in combination with your normal diet. Some people use applications like iPhone “Lose It” to keep track of their diet and make sure they are getting enough but not too much carbohydrate. This can also let you calculate how many glucose tablets you need to make up the difference if you're short.
Benefits of Glucose Treatment
Fasting, extreme diets and strenuous activity without enough carbs are all very bad ideas with porphyria.
IV glucose also provides enough hydration when you're losing liquids through vomiting and diarrhea.
Glucose is safe during pregnancy. The drug Hemetin has not been studied enough to know if it harms pregnant women or their unborn. Also, glucose is widely available, while hemetin must often be flown in to more rural areas.
Glucose Treatment Side Effects
Excessive sweets in your diet and possibly frequent IV glucose could cause Type 2 diabetes. However, a Swedish study of AIP patients demonstrated that those who developed Type 2 diabetes actually were nearly 'cured' of their porphyria symptoms.
Some patients have a hard time getting emergency department personnel to actually give glucose IV without making the patient re-take many of the tests and differential diagnoses.