- HubPages»
- Health»
- Women's Health»
- Pregnancy
Umbilical Cord Blood Banking: What to Know When Pregnant to Prepare for Baby

What to Know When Pregnant to Prepare for Baby
The tough decisions of parenting begin during pregnancy. To prepare for baby, one important decision to make is whether saving baby's umbilical cord blood, placental blood or cord blood tissue is right for your family. To make an informed decision, parents first need to understand the scope of the issue: what cord blood stem cells are, their limitations, diseases cured, clinical trials, experimental studies, public versus private cord blood banks, questions to ask cord blood banks, warnings, and finding reliable resources. Newborn stem cells can be collected after either a vaginal birth or c-section birth, and can be used in stem cell transplants to cure many blood diseases.
Copyright © 2020 Melis Ann
- Cord Blood: To Save Or Not? - CBS News
CBS Evening News: Cord Blood: To Save Or Not? - Stem Cells From Umbilical Cords Can Treat Diseases, But Should Parents Invest In Keeping Them?
The Decision to Bank or Not to Bank
As a soon-to-be parent, it can be overwhelming to consider cryogenically freezing your baby's umbilical cord blood for possible future use to treat disease. Some look at the decision as another insurance policy, others feel guilty unless they choose to store cord blood and some regret that they didn't invest in private storage when their baby or a later sibling ends up with a treatable disease. The same decision is not right for everyone.
As opposed to embryonic stem cells, cord blood stem cells are not controversial in that there are no political or religious issues associated with these type of stem cells.
Factors to begin exploring this decision include cost, medical history and recommendations by medical agencies.
Recommendations by the American Academy of Pediatrics
- The AAP does not recommend storing baby's umbilical cord in a private bank for potential future personal or family use. Their reason is that conditions that require stem cells as a treatment would need to be treated using donor stem cells since the genetics of that condition are already part of the cord blood at birth.
- The AAP does recommend storing umbilical cord blood for personal use if there is a sibling with a condition that is treatable with a stem cell transplant.
- Public donation of cord blood is recommended for the greater good of society to help those needing stem cell transplants as well as medical research to further understand the potential of cord blood stem cells.
These recommendations can be taken into account along with your personal feelings about your situation. Ask yourself how comfortable you are with the cost of private banking. Are you comfortable storing cord blood for a just-in-case situation? Do you have another child or family member with a treatable disease? How would you feel if you did not store the cord blood and then ended up needing it? Do you feel satisfied donating the cord blood to those in need of a stem cell transplant? Do you feel comfortable donating the cord blood to others that may need it, knowing that it will likely be unavailable to your family if needed? Are you deciding to save cord blood for the future possibilities that it may provide that are experimental right now? Are you ok with having the cord blood thrown away as medical waste? Asking these tough questions will help you discover the path that's right for you.

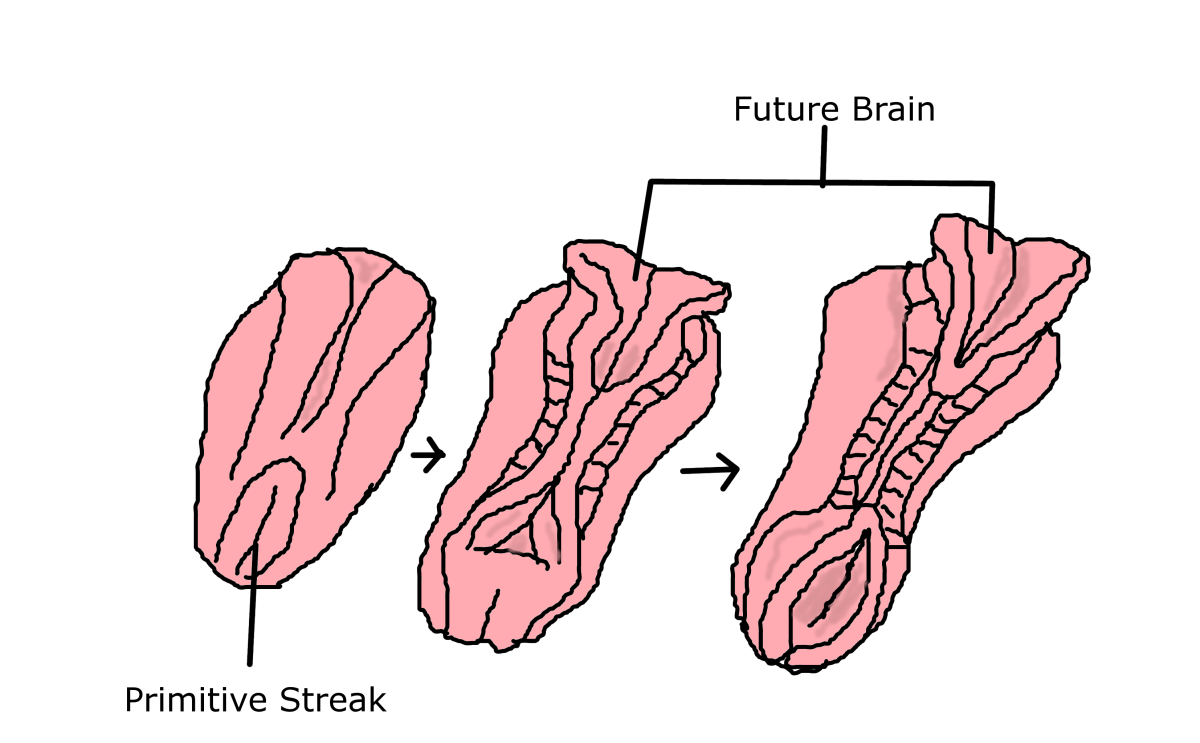
How is Umbilical Cord Blood Used?
The stem cells in umbilical cord blood can be used in transplantation. A transplant replaces unhealthy blood-forming cells with healthy blood-forming cells. Before cord blood was used as a source of stem cells, the only options for a stem cell source were bone marrow or circulating (peripheral) blood, both of which have their disadvantages.
What is Special About Cord Blood?
The blood remaining in the umbilical cord and placenta after childbirth contains stem cells which can be used in a stem cell transplant to treat blood diseases such as leukemia. Like bone marrow, umbilical cord blood is a rich source of stem cells, or blood-forming cells.
What Is A Stem Cell Transplant?
Patients with leukemia, aplastic anemia and other blood disorders or cancers can be cured with a stem cell transplant. In the case of leukemia, chemotherapy and/or radiation treatment destroys the existing stem cells after which new stem cells are introduced into the body. After the body circulates these new stem cells, the cells begin multiplying in the bone marrow. From this point, the new stem cells begin to build back health.
For diseases where stem cell transplants are standard therapy, cord blood is an accepted source of stem cells. For children that receive transplants, cord blood is the most common source of stem cells. Although the most common source of stem cells for adult transplants is donated bone marrow, the use of cord blood as a source of stem cells is becoming more common.
The first stem cell transplant using cord blood was done in 1988 to cure an infant with severe anemia syndrome.
Advantages of Stem Cells from Cord Blood Compared to Bone Marrow
According to the National Cord Blood Program, there are several advantages of using stem cells from cord blood compared to stem cells from bone marrow or peripheral blood.
- Collecting stem cells from cord blood is easy and painless compared to collecting from bone marrow. To extract cells from bone marrow, the patient undergoes a surgical procedure, risking infection and complications.
- Cord blood is less likely to contain viruses than bone marrow.
- Stem cells are available more quickly for transplants from cord blood. A cord blood unit is available immediately from storage whereas the bone marrow donor has to be contacted, have surgery and the sample has to be processed.
- Patients can more easily find a match with cord blood than with bone marrow. The tissue proteins, human leukocyte antigens (HLAs), only have to be a partial match between donor and recipient with cord blood, but must be a full match for a bone marrow transplant to be successful.
- More matches are available to non-white ethnic and racial groups through cord blood registries because there are more cord blood samples collected from individuals in these groups compared to the number of individuals registered to donate bone marrow (genes that determine matching are inherited and thus patients have a better chance of finding a match within their own racial group).
- Less risk of GvHD (graft vs. host disease) with cord blood stem cells. With GvHD, donor cells attack cells in the patient. This is a severe reaction which can be fatal. Since cord blood stem cells are less mature blood cells, GvHD is less severe, less frequent and easier to treat.
Cord Blood Statistics
- 4000 cord blood transplants performed each year globally
- 7 out of 10 people needing a transplant need to find a match outside the family
- only 9% of the 10,000 - 15,000 people in the U.S. who need a stem cell transplant are able to find a suitable match; for minority groups there is even less success in finding a match (data from 2002)
- siblings have a 25% chance of being a perfect HLA match to use cord blood and a 50% chance of being a partial HLA match
- 21% of transplants use publicly donated cord blood
- 30% of patients needing a stem cell transplant have a relative that is a match with bone marrow as the stem cell source
- U.S. FDA licensed cord blood transplants in 2011 for diseases that have been using cord blood for transplants for many years, making health insurance coverage available for many patients
- difficult to calculate the likelihood of needing your own stem cells; one estimate is that the lifetime probability could be as much as 1 in 400; the likelihood that a newborn or other family member may benefit from cord blood stem cells is as much as 1 in 200, not including future uses of stem cells beyond which are currently approved
- other studies show odds of needing stem cell transplant from donor by age 10 is 1 in 5,000 (for approved standard list of conditions); odds of needing stem cell transplant from own cord blood by age 10 is 1 in 10,000 (for approved standard list of conditions)
- older studies pointed to a higher survival rate for patients that used sibling cord blood stem cells for transplant compared to an unrelated donor, however, more recent studies show that survival rates are almost equivalent
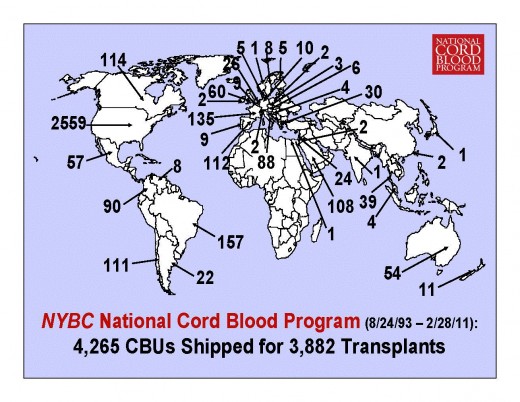
International Reach of National Cord Blood Program
What Diseases Can Be Cured With Cord Blood Stem Cells?
Patients with immunodeficiencies, bone marrow failure syndromes, certain cancers, hemoglobinopathies, and inborn errors of metabolism can benefit from stem cell transplants. Some examples of specific diseases are leukemia, sickle cell disease, thalassemia and Hodgkin's lymphoma.
An umbilical cord blood stem cell transplant is considered a standard treatment for these conditions.
Depending on the disease being treated, doctors will decide if using the patient's own cord blood (autologous) or if donated cells (allogeneic) are the best method for treatment. It is standard that all blood diseases are treated with donor stem cells, except for solid tumors that are unrelated to the blood or immune system. However, there are many clinical trials using autologous stem cells.
Take Caution With Cord Blood Cure Claims
Keep in mind that the only proven use for cord blood stem cells is a transplant to cure genetic diseases of the blood with the exception of solid tumors.
Dr. George Daley, Director of the Stem Cell Transplantation Program at Children's Hospital of Boston, warns that families need to be cautious of claims that cord blood can be used to treat other conditions such as spinal cord injuries and Cerebral Palsy.
Clinics that offer treatments beyond blood diseases are operating in locations outside the regulatory umbrella of the Food and Drug Administration (FDA) or the European Medicine Agency (EMA).
There are studies taking place to understand further benefits of cord blood. The process takes time and needs to occur under regulatory agencies to ensure safety and efficacy.
A Warning on Cure Claims

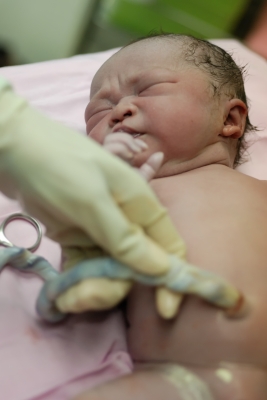
Cord Blood, Placental Blood and Cord Tissue Collection
There are several different types of collection packages to purchase through private banks.
- Cord Blood
There are a couple of standard methods for collecting cord blood once the umbilical cord is clamped after birth. The procedure is non-invasive and painless. The volume collected is important in addition to making sure that the instructions are followed carefully. - Placental Blood
This additional sample would likely double the volume of blood collected from the cord alone. Usually this is an additional collection cost. - Cord Tissue
For another additional fee, a small piece of the umbilical cord is stored. There is no currently approved use for umbilical cord tissue. Research is ongoing to find out if it's feasible to use cord tissue stem cells to repair the spinal cord, for example. If needed in the future, cells could be extracted from the cord tissue being stored.
Cord blood banks should be accredited by FACT (Foundation for the Accreditation of Cellular Therapy). FACT regulates collection and banking of cord blood using an international standard. Their website lists accredited organizations.
Choices for Cord Blood Banking
There are three choices for baby's cord blood: private banking, public donation or disposal. In the U.S., cord blood is stored in about 5% of births. It is very expensive to collect and process the blood, whether the cost is incurred by an individual family or institution that sponsors blood donation.
Private Banking
Families can store their baby's cord blood in a private bank for use by the child or child's family. The average initial costs of cord blood banking are $1500 which include collection and processing. Thereafter, the storage fee for the cord blood unit is approximately $100 per year. Health insurance is not likely to cover this optional service.
- Find a list of private cord blood banks by country, then compare banks by features such as cost.
- When blood is processed in a private bank, the processing involves a degree of testing to ensure the sample is eligible to be stored.
Public Donation
When cord blood units are donated to a public bank, the bank then owns the unit. It becomes available to those needing a match, although if still available, it is possible to use your donation in the future. If the quality or quantity of cord blood collected is not transplant quality, the unit may still be able to be used in research. The number of hospitals or facilities that have the capability to accept cord blood donations is limited based on the funding they receive to pay for the cost.
- Find out if you are eligible to donate cord blood. The National Marrow Donor Program defines parameters to protect the health of those that would receive donor cord blood. Some limitations relate to diabetes, tattoos, malaria, hepatitis, cancer, AIDS, and sexually transmitted diseases.
- Find a location for either a hospital that offers cord blood donation or a mail-in donation program.
- The more donations the blood banks receive and can share with other banks internationally, the more successful the program can become. It is a chance to save a life.
- Cord blood samples donated to a public bank go through more rigorous testing criteria to ensure the safety of future recipients.
Free Cord Blood Banking for Families in Need
Cord blood banking is available to families for free or a discount if there is a medical need. In cases where stem cells are used as a standard therapy, families can apply under one of several programs.
Private Banks
Several private cord blood banks provide free collection, processing and storage for families that have an eligible medical need. As opposed to public banks, the private bank may have an expanded definition of eligible situations. There is a list of banks that provide this charity service on the Parent's Guide to Cord Blood Foundation website. See the list under the section Family Banks - Related Donor Programs. Calling each for the most current information is advised.
Public Banks
Although cord blood storage through a public bank typically becomes anonymous, the donation can be directed to a sibling in the Sibling Directed Donation Program. Cord blood storage kits are provided for free to bring to the hospital where cord blood is collected at birth and then sent to the public bank for free processing and storage.
Choosing a Private Cord Blood Bank
The differences between private cord blood banks are subtle.
A few points to consider:
- Are storage fees fixed or can they increase over time?
- How does the bank ensure that the cord blood unit collected is of transplant quality?
- Are you still required to pay for collection and processing if the cord blood unit is not transplant quality or not enough sample is collected?
- What are your options if the cord blood bank goes out of business?
- Find out the privacy policy of each bank and what is in the consent forms you will be required to sign. For example, testing may be required of the mother's blood to check for certain infectious diseases and genetic conditions. You will be notified of findings in addition to public health officials depending on local laws.
- What happens to your cord blood unit if you decide to stop paying storage fees?
- How is the cord blood stored? Is the unit separated into multiple vials for access to a portion of the unit if not all of it needs to be extracted from storage at the same time?
Parent's Guide to Cord Blood Foundation
The Parent's Guide to Cord Blood Foundation is a non-profit organization formed to educate parents about cord blood uses and cord blood storage. This group is run by an expert advisory panel made up of physicians and scientists from around the world. Their website is the only cord blood website accredited by the Health on the Net Foundation (HON) under the United Nations, which ensures that they provide accurate health advice and information.
Parent's Guide is also involved in promoting public policy to support education of the public; getting states to adopt laws requiring physicians and hospitals to educate parents about their child's cord blood.
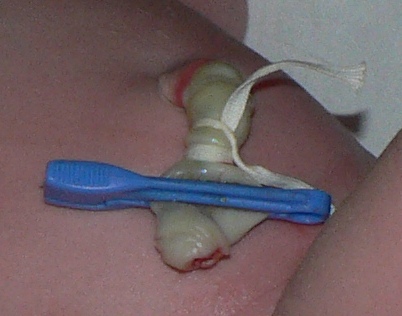
Delayed Clamping of Umbilical Cord
There is concern over early clamping of the umbilical cord in order to collect cord blood as opposed to giving the baby more time to receive blood from the cord, known as placental transfusion. The concern is that the infant will not receive the blood volume from the cord that would naturally occur without the interruption to collect cord blood, possibly up to 40% less blood volume. Thus, the infant could be more at risk for developing anemia in addition to breathing problems or possibly long-term brain development effects.
In theory, there is generally enough blood left in a discarded placenta and umbilical cord after birth to provide a sufficient cord blood sample. After the cord is cut, it is discarded as medical waste. Therefore, collecting cord blood should not be a problem for baby if done with appropriate timing.
This is an area where some doctors dismiss the idea that this is a concern whereas other doctors are proactive in considering these potentially negative effects. There is interest in a method which involves collecting the cord blood without clamping the umbilical cord which would, in theory, allow enough blood for both placental transfusion and blood collection. Another possibility is waiting until the birth of the placenta to collect cord blood from different parts of the cord and placenta until enough volume is extracted.
The American Academy of Pediatrics formally recommended, in 2007, that cord blood collection should not alter the timing of normal umbilical cord clamping. According to the Parent's Guide to Cord Blood Foundation, studies show that there is no need to wait beyond a two minute delay in clamping the umbilical cord. Another study published in the British Medical Journal showed that early clamping leads to iron deficiency in infants. Since iron deficiency is related to impaired brain development the study recommends delayed cord clamping.
There are other factors to consider in delayed cord clamping:
- Delayed clamping can lead to heavy bleeding by the mother. A decision of when best to clamp may have to be made based on the mother's health.
- Too long of a delay can make cord blood collection fail based on volume. The blood in the cord naturally begins to clot, making collection difficult.
Discussing your concerns about early clamping and cord blood collection with your physician is your best strategy. Help them understand what your goals are so you can work together.
Dr. Fogelson Making A Case for Delayed Cord Clamping
Limitations of Cord Blood
- Volume ~ Even if the volume collected at birth is sufficient, this amount of blood may not be enough to perform a successful transplant for an older child or adult.
- One chance ~ Cord blood stem cells cannot be used in a transplant more than once whereas with bone marrow, additional samples can be taken from a donor.
- Longer time to produce cells ~ Compared to bone marrow stem cells, cord blood cells may take longer to start producing healthy cells after transplant which can leave the patient vulnerable to infection.
- Plan ahead ~ The decision to bank cord blood has to be made well in advance of delivery.
- Complicated deliveries ~ The plan to collect cord blood may be changed based on developments during delivery. It may not be possible to collect a sample even if you make plans in advance.
- Expiration date ~ There is currently no expiration date on cord blood that is stored in liquid nitrogen. Duke Health states that cord blood stem cells are considered usable for several decades. The National Cord Blood Program has units of blood designated for research that they have been testing for long term viability. Samples that are sixteen years old have maintained their quality thus far.
Current Research on Cord Blood Stem Cells
Current research is helping us learn more about stem cells from cord blood. At Children's Hospital Boston, a top rated Children's Hospital in the U.S., there are many research projects underway that study diseases using stem cells.
To address one of the limitations of cord blood - volume of blood collected - researchers at Children's are trying to find a way to expand the number of cells in a unit before the unit is used in a transplant. This would enable a sample from an umbilical cord to be usable by an older child or adult.
Research studies and clinical trials are currently under way to discover further applications for cord blood including regenerative applications (finding out if these stem cells can develop into other cells other than blood cells). This breakthrough could potentially benefit those with Alzheimer's disease, Parkinson's disease, diabetes, multiple sclerosis, heart defects or spinal cord injuries.
Resource:
Find a Clinical Trial
for Cord Blood
Access to stem cell therapy for many conditions is limited to clinical trials. There are literally hundreds of ongoing trials using cord blood. The U.S. National Institute of Health website has a search tool for clinical trials by location and condition.
Clinical Trials Using Stem Cells
Currently, there are many clinical trials studying the effects of using stem cells to benefit patients with various conditions. At this stage, use of cord blood appears to be beneficial even if only to slow disease progression. These developments are exciting because they potentially treat common conditions and would likely require smaller amounts of cord blood compared to the quantity needed for a transplant.
The following are conditions where emerging therapies are being studied using cord blood as a source of stem cells:
- Cerebral Palsy
- Neonatal Oxygen Deprivation
- Traumatic Brain Injury
- Type I Diabetes
- Crohn's Disease
- Lupus
- Hypoplastic Left Heart Syndrome (HLHS)
Experimental Treatments: Regenerative Medicine
Treatments that have not yet reached clinical trial phase are considered experimental. These treatments using cord blood are first being analyzed in cell cultures or animal studies. Possible future uses of stem cells in the form of regenerative medicine may include:
- growth of cardiac muscle cells
- liver cell growth
- cure for Alzheimer's Disease
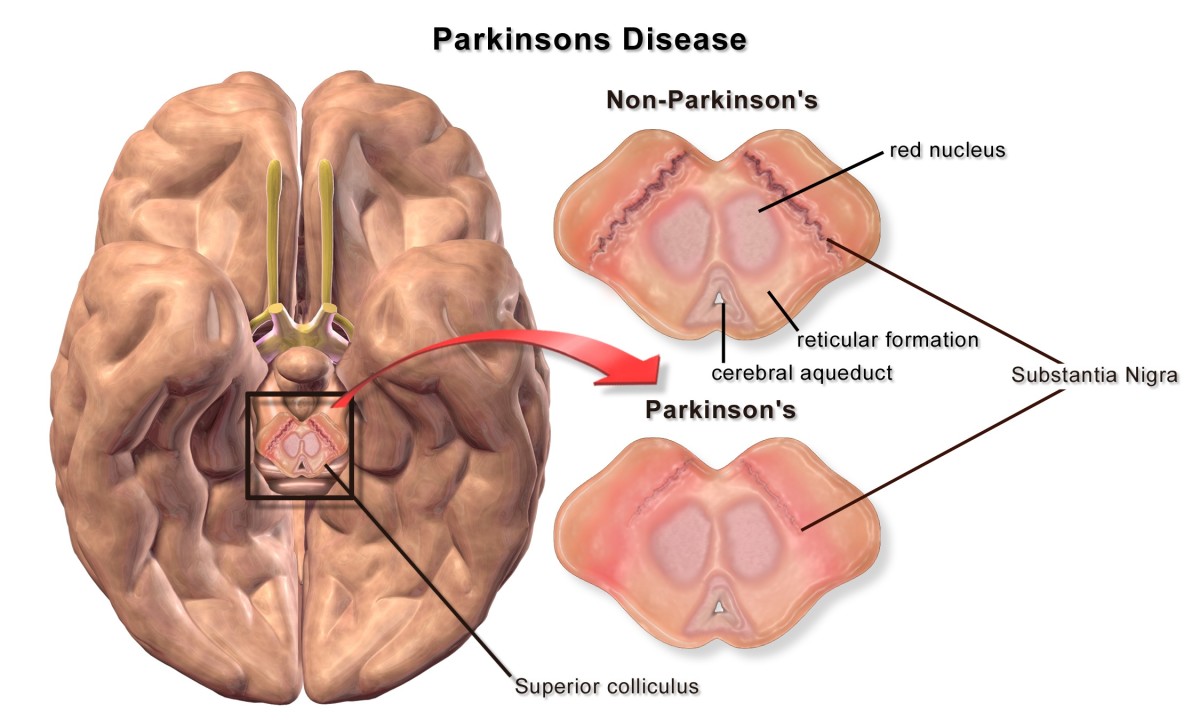
- cure for Parkinson's Disease
For the first time, a child received stem cells to grow a vascular graft to treat a congenital heart defect. Congenital heart defects are the most common birth defect, thus making advancements in this area very exciting.
Disclaimer: Note that this website portrays my opinion. I want to help others consider a new or different view. Any action taken based on these opinions is the responsibility of the reader.
Copyright © 2020 Melis Ann
Original content written by Melis Ann published only on HubPages at the following web address: http://melisann.hubpages.com/hub/Umbilical-Cord-Blood-Banking-Research-Benefits-and-Disadvantages-What-to-Know-When-Pregnant-to-Prepare-for-Baby
My Personal Experience With Cord Blood Banking
If you've already read my article about the importance of hospital NICU levels, then you've read about my oldest son who was born with multiple congenital heart defects.
Storing cord blood was not as mainstream when he was born as it is now, but it certainly was an option. We opted, based on the low probability of needing it, not to store his umbilical cord blood. After seeing him struggling to survive open heart surgeries and other horrific procedures, our perspective changed about cord blood.
For our next two children, the decision to store cord blood was a given. Although there are still not approved uses related to cardiac repair, we decided that we wanted to bank for the just-in-case situation. We still wish we had cord blood for all three children.
Since banking for our kids, public donation of cord blood is a new option. It's exciting to be able to donate to help those in need. It's also heartening to know that there is a public bank out there with thousands of cord blood units to find a potential match for your child to use if needed in the future. For families that have a definite medical need, private banking is a great option. And for the fortunate families that do not have to deal with medical problems, public donation is a wonderful option.
Making a Decision on Cord Blood Banking
What's Your Choice?
After reading this information on cord blood, which way are you leaning?
© 2012 Melis Ann