Does Your Loved One Need A Healthcare Advance Directive Or A Do Not Resuscitate (DNR) Order?
With more people in our society entering retirement relative to our population, more and more people are contemplating what "end of life" planning they should have in place. For many people, the thought of suffering from a debilitating illness or accident and becoming a burden on their loved ones is more than they can bear. Many of them have had a heart attack, stroke or suffer from some debilitating pain. For this reason, among others, everyone should take time to decide if an Advance Directive or a DNR order is right for them.
Below you will find an Advance Directive definition along with its benefits and risks. You will also learn the difference between an Advance Directive and a Do Not Resuscitate Order. Find out how having or not having these legal documents can affect you and your family should the worst happen.
Advance Directives: A Definition And Explanation
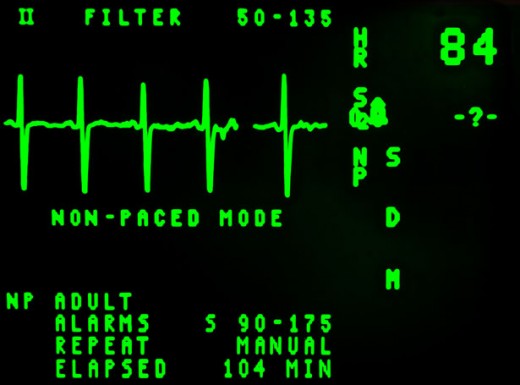
A healthcare Advance Directive, also called a Living Will, is a legal document that spells out to one's family and healthcare professionals what medical procedure or procedures not to do in the case of an emergency or at the end of one's life. Advance Directives allow medical professionals, in the hospital and in the ambulance, to know exactly what procedures they can or cannot perform on the individual.
Although there are some states that do not recognize Advance Directives, most states will recognize them, and even hand out penalties or legal responsibility to those who knowingly act outside of the confines of that Advance Directive. There is no consequence for those acting outside the confines of the directive if they do not physically see the document. If a person has a stroke, and family members say his Advance Directive says to not perform CPR, if the family cannot produce the directive for the ambulance personnel to see, they must perform as if there is no directive.
Living Will, DNR Advance Directive : What's The Difference?
What Is Advance Directive?
For many people who are struggling with some end of life choices, or those who are trying to make sure their families don't have to make the hard choices, the different medical legal terms can make your eyes cross. It can be difficult to know exactly what someone is referring to unless you have a basic grasp on what each of the terms mean.
For all intensive purposes, a living will and an Advance Directive are the same thing. Advance Directive is a legal term that defines what a person's living will is. In some states you may hear medical personnel use one term, and in other states you will hear the other term.
DNR, or a Do Not Resuscitate order, is a living will or an Advance Directive that specifically says the person does not wish to be resuscitated should they go into cardiac arrest or quit breathing, whether it be from trauma or a heart attack. This form must be kept available if the person is at home, and must be filed with a hospital everytime a person is admitted.
Limitations Of Advance Directive And DNR's
Advance Directive Poll
Do you or any of your close relatives have an Advance Directive or a DNR order?
As with any other legal document or action, there are limitations to the advance directive. As mentioned above, they must be present for medical personnel to abide by them. If the ambulance is called, the family must produce the document. If the patient is moved from one floor of the hospital to another, they document must be moved to the new floor.
With that said, humans are just that: human. Sometimes the document may get lost or may not be transferred to the new hospital floor. What makes it worse, you probably will not be able to ensure the document is where it needs to be if you are the one needing medical care.
Also, in certain states, certain medical procedures may not be able to be omitted and in most states, the directive must be renewed every so often, usually every year, and signed by your physician. Although these documents can be just as frustrating as any other legal documentation, it is important that we remember that there are definite benefits to Advance Directives.
Benefits Of Advance Directives And DNR's

The most obvious benefit of having an accurate and up to date Advance Directive or DNR is that your wishes will be carried out, even when you are not able to voice them. Many people do not wish to have CPR done or to be intubated and on a respirator, especially if they are past a certain age. They want to die without being confined to a hospital bed or a nursing home. However, often those same people have family members, be it children or not, that will want emergency personnel to do anything and everything to keep their relative alive.
Understand, the desire of the family member to have every effort given is no less important as the desire of the person to not have certain medical procedures implemented.
Another benefit of Advance Directives is that in most states you can spell out specific medical procedures to be omitted. Some people choose to allow CPR, but only allow a respirator for a certain amount of time. Others will allow oxygen delivery up to, and including intubation, but do not allow CPR once they have gone into cardiac arrest. Still others do not allow any medical intervention once they have lost consciousness.
These legal documents are flexible in what they allow the patient to choose to disallow. Most states have printable Advance Directive forms on their website for their Department of Health or equivalent. Be sure to consult your Primary Care Physician about the benefits of disallowing certain medical procedure.
Other Health Hubs
- Signs And Symptoms: Emergency Management Of Your Hypertensive Crisis
Hypertensive Crisis affects many Americans every year and leads to thousands of hospital visits and in some cases can even lead to death. Learn how to deal with Hypertensive Crisis, what causes Hypertensive Crisis, and how to avoid Hypertensive Crisi - Do You Need To Have A Gallbladder Removal Surgery Due To Gall Bladder Stone?
Many people in the United States experience Gallbladder Pain due to Gallbladder stone, especially late in life. Find out more about the Gallbladder, what causes Gall Stones, Gallbladder Symptoms in Women, and more. - What Are Complications Of Diabetes?
Learn about Diabetes Mellitus and how it can affect your life and overall health.