Pathogenesis, diagnosis and treatment of the acute complications of Diabetes Mellitus
Signs, symptoms, pre-disposing factors and features of the various kinds of acute diabetic complications
















INTRODUCTION
Hello everyone and welcome to the second edition of disease cases been clinically analyzed and treated here in my internet hospital. Today's case would be on the acute complications of Diabetes mellitus closely following the first case we treated, which is Diabetes Mellitus itself. You may want to go through it first before reading this, it would be very great if you do so, but if you want to have a glance and a view of what diabetes is all about, I suggest, you go to this link and have a short glance to prepare your mind on what is to come from this hub
Diabetes Mellitus in simple plain language
Then come back here and read the detailed clinical explanations of the acute complications of Diabetes Mellitus. Most of the literals on the street just see diabetes as a simple illness involving an increased level of glucose in blood. In fact some see it as a sugar-related disease not even knowing what sugar is involved. But if will blow your mind to see how devastating, vast, broad and complicating diabetes is. If you'd followed us from the previous hub about diabetes, you will see the effects and long term complications of Diabetes which also includes sexual complications both to men and women. Diabetes is a disease worth knowing so that each and every one of us can apply adequate preventive measures in order not to acquire it. A link of my previous hub on diabetes will be shown at the end of this hub, so that you may read it if you please to.
Classification of acute complications of DM
1. Diabetic coma:
1) diabetic ketoacidisis (DKA);
2) nonketonic hyperglycemic-hyperosmolar coma (NKHHC);
3) lactoacidosis (LA).
2. Hypoglycemic coma (HC).
DIABETIC KETOACIDISIS (DKA)
DKA is the most frequent endocrine emergency seen by the primary care physician. Mortality rates from 6 – 10 % have been reported. All the abnormalities associated with DKA can be traced to an absolute or relative insulin lack, which develops over the period of several hours or days.
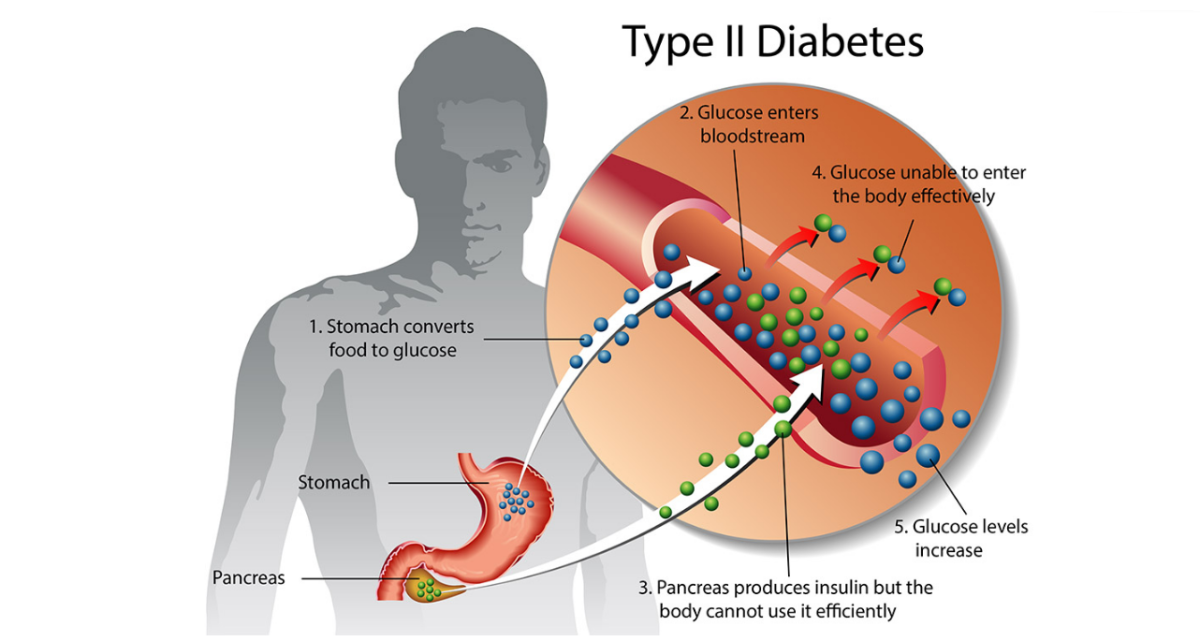
DKA results from grossly deficient insulin modulation of glucose and lipid metabolism.
Major components of the pathogenesis of diabetic ketoacidosis are reductions in effective concentrations of circulating insulin and concomitant elevations of counterregulatory hormones (catecholamines, glucagon, growth hormone and cortisol).
These hormonal alterations bring about three major metabolic events:
(1) hyperglycemia (high level of glucose in blood) resulting from accelerated gluconeogenesis ( the production of glucose by using new and different sources such as amino acids, fats etc) and decreased glucose utilization,
(2) increased proteolysis (the break down of proteins) and decreased protein synthesis (the production of proteins) and
(3) increased lipolysis (the breakdown of Lipids) and ketone production.
Hyperglycemia initially causes the movement of water out of cells, with subsequent intracellular dehydration, extracellular fluid expansion and hyponatremia (low level of sodium in blood). It also leads to a diuresis in which water losses exceed sodium chloride losses. Urinary losses then lead to progressive dehydration and volume depletion, which causes diminished urine flow and greater retention of glucose in plasma. The net result of all these alterations is hyperglycemia with metabolic acidosis and an increased plasma anion gap.
Precipitating factors:
1) newly diagnosed diabetes (presenting manifestation);
2) inadequate administration of exogenous insulin;
3) increased requirements for insulin caused by the presence of an underlying stressful condition:
- an intercurrent infection (pneumonia, cholecyctite);
- a vascular disorder (myocardial infarction, stroke);
- an endocrine disorder(hyperthyroidism, pheochromocytoma);
- trauma;
- pregnancy;
- surgery.
Factors Most Often Associated with the Development of Diabetic Ketoacidosis
Factor
Approximate frequency (%)
Infection: 35
Omission of insulin or inadequate insulin: 30
Initial presentation of diabetes mellitus: 20
Medical illness: 10
Unknown: 5
Clinical presentation
Diabetic ketosis
It is status which is characterized by increased level of ketones in blood, without clinical signs of dehydration and can be corrected by diet (fat restriction) and regular insulin injection.
DKA develops over a period of days or weeks.
Signs and symptoms
1. Polydipsia (Increased appetite), polyurea (increased and frequent Urination) and weakness are the most common presenting complaints.
2. Anorexia (eating disorder), nausea (Sensation of unease and discomfort in the upper stomach with an urge to vomit), vomiting, and abdominal pain may be present and mimic an abdominal emergency.
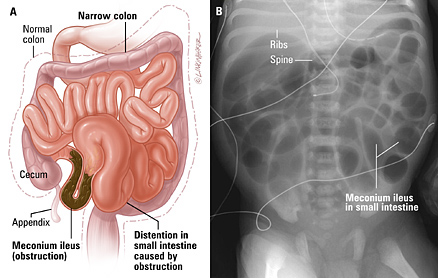
3. Ileus and gastric dilatation may occur and predispose to aspiration.
4. Kussmaul breathing (deep, sighing respiration) is present as respiratory compensation for the metabolic acidosis and is obvious when the pH is less than 7.2.
5. Symptoms of central-nervous-system involvement include headaches, drowsiness, lassitude, stupor and coma (only 10 % patients are unconscious).
Physical examination
1. Hypotermia is common in DKA. A fever should be taken as strong evidence of infection.
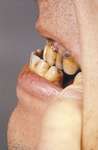
2. Hyperpnea or Kussmaul respiration are present and related to degree of acidosis, acetone may be detected on the breath (musty (fruity) odor to the breath).
3. Tachycardia (Increased heart rate which exceeds the normal range) frequently is present, but blood pressure is usually normal unless profound dehydration is present.
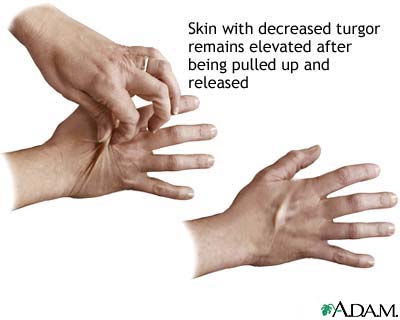
4. Poor skin tugor (an abnormality in the skin’s ability to change shape and return to normal elasticity) may be prominent depending on the degree of hydration.
5. Hyporeflexia (associated with low serum potassium- a condition of below-normal or absent reflexes which can be tested for by using a reflex hammer) can be elicited.
6. Signs consistent with a “surgical abdomen” but which follow severe ketonemia (presence of Ketone bodies in blood) can confuse the clinical picture.
7. In extreme cases of DKA one can see hypotonia (a state of low muscle tone) stupor (the lack of critical cognitive function and level of consciousness where in a sufferer is almost entirely unresponsive and only responds to base stimuli such as pain), coma, in-coordination of ocular movements, field dilated pupils, and finally death.
8. Other signs from a precipitating illness can be present.
Although usually straightforward, the diagnosis of diabetic ketoacidosis is occasionally missed in unusual situations, such as when it is the initial presentation of diabetes in infants or elderly patients or when patients present with sepsis or infarction of the brain, bowel or myocardium. These presentations can distract the physician from the underlying diagnosis of diabetic ketoacidosis.
The laboratory tests needed to confirm the presence of diabetic ketoacidosis and to screen for precipitating events.
Laboratory findings
1. The hallmark of DKA is the finding of:
- hyperglycemia;
- ketonemia;
- metabolic acidosis (plasma pH and bicarbonates are decreased.
2. A presumptive bedside diagnosis is justified if the urine is strongly positive for both glucose and ketones.
3. Different changes of electrolyte levels in the blood can be observed and does not reflect the actual total body deficits.
4. Serum amylase and transaminases can be elevated.
5. Leucocytosis (Production of white blood cells) occurs frequently in DKA and therefore cannot be used as a sole indication of infectious process.
Types of DKA:
- abdominal;
- vascular collapse;
- cerebral (encephalopathic);
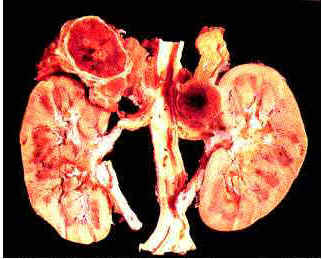
- renal;
- mixed.
Treatment
The management of patients may be difficult because of problems in achieving of normal glucose control. Because there is good evidence that hyperglycemia conveys risks for all of the common long-term complications of DM, which are the major cases of excess morbidity and mortality in diabetics.
Patients with type 1 DM usually start treatment at the hospital. They require close monitoring during efforts to develop an appropriate insulin treatment regimen, and the patients or their care givers require detailed education in their responsibilities and proficiency in them before home management is safe.
Most patients with type 2 DM who are not acutely ill can be safety started on the insulin (if they need it) on an outpatient basis with adequate patient education and close physician follow-up.
An effort to maintain persistently normal serum glucose fluctuations in diabetics entail significant risk of causing frequent or severe hypoglycemic episodes, particularly in type 1 DM patients. Treatment regimens differ in the priorities assigned to keeping the risks for hypoglycemia minimal and to keeping serum glucose fluctuations in a normal to near-normal range.
The therapeutic goals for diabetic ketoacidosis consist of improving circulatory volume and tissue perfusion, reducing blood glucose and serum osmolality toward normal levels, clearing ketones from serum and urine at a steady rate, correcting electrolyte imbalances and identifying precipitating factors.
The goals of therapy include:
1. Rehydratation.
2. Reduction of hyperglycemia.
3. Correction of: a) acid-base and b) electrolyte imbalance.
4. Investigation of precipitating factors, treatment of complications.
The most important factor to emphasize is the frequent monitoring of the patient both clinically and chemically. Initially, laboratory data should be obtained every 1 – 3 hours and less frequently once clinical improvement is noted. If the patient is in shock, stupor or coma, a nasogastric tube, especially if vomiting, and urinary catheter are recommended.
Frequent assessment of potassium status is vital. A lead II electrocardiogram (ECG) can be provide a rapid assessment of hyperkalemia (peaked T waves) and hypokalemia (flat T waves and presence of U waves). Hyporeflexia and ileus are clinical indications of potassium deficiency.
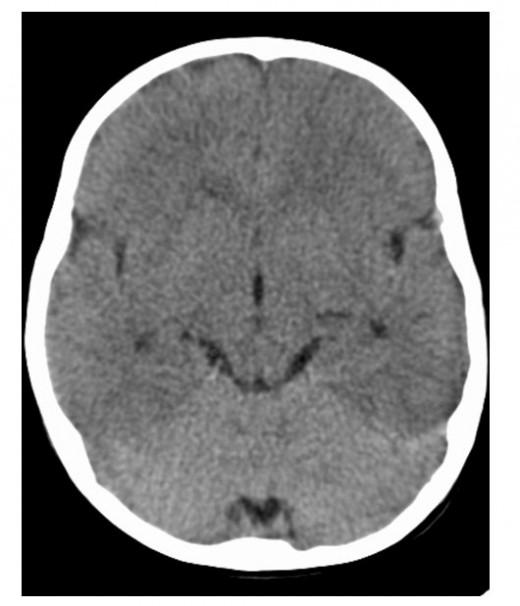
Careful observation of neurological status is vital to detect the infrequent but devastating presence of cerebral edema.
Rehydration(Fluid Replacement)
The severity of fluid and sodium deficits is determined primarily by the duration of hyperglycemia, the level of renal function and the patient's fluid intake.
The average fluid deficit in adults with DKA is 3 to 5 l.
Dehydration can be estimated by clinical examination and by calculating total serum osmolality and the corrected serum sodium concentration.
A rapid infusion of 0,9 % sodium chloride (e.g., 1 l/h for the first 1 to 2 hours) is given and then reduced to about 0,5 – 0,3 l/h if the blood pressure is stable and the urine follow is adequate. After the initial infusion, intravenous fluid therapy must be adjusted individually on the basis of urine output, clinical assessments of hydration and circulation, determination of plasma electrolytes and glucose. When serum glucose level is about 11 – 13 mmoll/ (approximately 250 mg per dL )l administration of 5 % glucose with insulin can be performed (1 to 2 unites of insulin on each 100 ml of 5 % glucose solution). The addition of glucose to the intravenous solution is necessary for correction of tissue lipolysis and acidosis. This allows continued insulin administration until ketonemia is controlled and also helps to avoid iatrogenic hypoglycemia.
Another important aspect of rehydration therapy in patients with diabetic ketoacidosis is the replacement of ongoing urinary losses.
Insulin treatment
Modern management of diabetic ketoacidosis has emphasized the use of lower doses of insulin.
This has been shown to be the most efficacious treatment in both children and adults with diabetic ketoacidosis. The current recommendation is to give low-dose (short-acting regular) insulin after the diagnosis of diabetic ketoacidosis has been confirmed by laboratory tests and fluid replacement has been initiated.
It is prudent to withhold insulin therapy until the serum potassium concentration has been determined. In the rare patient who presents with hypokalemia, insulin therapy may worsen the hypokalemia and precipitate life-threatening cardiac arrhythmias.
E.g., initial intravenous administration of 10 to 20 units of regular insulin followed by continuous intravenous infusion of 0,1 unit/kg/hour in 0,9 % sodium chloride infusion. (50 units of insulin can be added to a 500 ml bottle of 0,9 % sodium chloride solution to give 1 insulin unite/10 ml of solution.)
In clinical situations in which continuous intravenous insulin cannot be administered, the recommended initial insulin dose is 0.3 unit per kg, with one half of the dose given as an intravenous bolus and the remainder given subcutaneously or intramuscularly Subsequently, regular insulin should be given in a dosage of 0.1 unit per kg per hour until the blood glucose level is approximately 11 – 13 mmoll/L (250 mg per dL).
If the blood glucose concentration does not fall by 2.8 to 3.9 mmol per L (50 to 70 mg per dL) in the first hour, the intravenous infusion rate should be doubled or additional intravenous 10-unit boluses of insulin should be given every hour Either of these treatments should be continued until the blood glucose level falls by 2.8 to 3.9 mmol per L (50 to 70 mg per dL) Low-dose insulin therapy typically produces a linear fall in the glucose concentration of 2.8 to 3.9 mmol per L (50 to 70 mg per dL).
More rapid correction of hyperglycemia should be avoided because it may increase the risk of cerebral edema. This dreaded treatment complication occurs in approximately 1 percent of children with diabetic ketoacidosis. The typical presentation is onset of headache and decreased mental status occurring several hours after the start of treatment. Cerebral edema is associated with a mortality rate of up to 70 percent.
But if there is a tendency for decreasing the level of glucose we have to decrease the dose of insulin in two times.
When the serum glucose concentration reaches 11-13 mmoll/l, hourly insulin dosage can be reduced to 0.05 unit per kg per hour or insulin can be given subcutaneously (if plasma and urine persistently negative for ketones). Blood glucose level should be maintained at about 11 mmoll/l during intravenous therapy.
Improvement usually is noted in 8 – 24 hours. Following stabilization of the clinical condition, patients are placed in insulin regimen consisting of five injections of regular insulin.
Treatment of electrolyte disorders.
As a rule, potassium should never be given until the state of renal function is known and until the serum potassium concentration is available.
Although the typical potassium deficit in diabetic ketoacidosis is 500 to 700 mEq (500 to 700 mmol), most patients are hyperkalemic at the time of diagnosis because of the effects of insulinopenia, hyperosmolality and acidemia. During rehydration and insulin therapies for diabetic ketoacidosis, the serum potassium concentration typically declines rapidly as potassium reenters the intracellular compartment.
The initiation of K replacement (20 to 40 mmoll/h) usually can be deferred for 2 hours, using hourly serum measurements as a guide.Potassium would be to infuse at a rate of ml of 1,5 g/h during 3 – 5 hours.
The goal is to maintain the serum potassium concentration in the range of 4 to 5 mEq per L (4 to 5 mmol per L).
Correction of metabolic acidosis.
The metabolic acidosis occurs due to insulin deficiency and dehydration. So ketone bodies are themselves metabolized to bicarbonate once proper therapy is begun (fluids, electrolytes, insulin) and exogenous administration of bicarbonate can overcorrect to alkalosis.
The use of bicarbonate can be recommended only in the following cases:
- if life-threatening hyperkalemia;
- when severe lactic acidosis complicates DKA;
- with severe acidosis (pH<7), especially when complicated by shock that is not responsive to appropriate fluid resuscitative measures in an attempt to improve cardiac output.
Bicarbonate would be to infuse at a rate of 100 to 300 ml of 2,5 % solution.
Other therapeutic consideration:
- since infection is one of the leading precipitating events of DKA, it should be looked for and, if found, treated appropriately;
- vascular thrombosis (it is secondary to severe dehydration, high serum viscosity, and low cardiac output) – heparin (5000 unites 4 times a day);
- vascular collapse can be treated by mesatone (1 – 2 ml); glucocorticoides (dexametasone 4 mg two times a day). You must remember that development of vascular collapse after initiation of therapy should suggest the presence of gram-negative sepsis or silent myocardial infarction;
- cerebral edema (It is a rare and frequently fatal complication. Some physicians believe that rapid osmotic reduction of plasma glucose should be avoided to minimize rapid osmotic changes. Some patients have premonitory symptoms (e.g., sudden headache, rapid decrease in the level of consciousness), but in others acute respiratory arrest is the initial manifestation. If cerebral edema is diagnosed, therapeutic maneuvers might include the use of : mannitol (1 – 2 g/kg intravenous over 20 min), dexametasone (0,25 – 0,50 mg/kg/day divided q 4 – 6 h). But they are usually ineffective after the onset of respiratory arrest.
Immediate Posthyperglycemic Care
In patients who are unable to eat, 5 percent dextrose in hypotonic saline solution is continued at a rate of 100 to 200 mL per hour. Blood glucose levels are monitored every four hours, and regular insulin is given subcutaneously every four hours using a sliding scale. When patients are able to eat, multidose subcutaneous therapy with both regular (short-acting) and intermediate-acting insulin may be given.
In patients with newly diagnosed diabetes, an initial total insulin dosage of 0.6 to 0.7 unit per kg per day is usually adequate to achieve metabolic control. A typical regimen is two thirds of the total daily dosage before breakfast and one third of the total daily dosage before dinner, with the insulin doses consisting of two-thirds NPH (intermediate-acting) insulin and one-third regular (short-acting) insulin.
Patients with known diabetes can typically be given the dosage they were receiving before the onset of diabetic ketoacidosis.
Complications of Therapy
Symptomatic cerebral edema occurs primarily in pediatric patients, particularly those with newly diagnosed diabetes. No single factor predictive for cerebral edema has yet been identified. As noted previously, however, overly rapid rehydration or overcorrection of hyperglycemia appears to increase the risk of cerebral edema. Onset of headache or mental status changes during therapy should lead to consideration of this complication. Intravenous mannitol in a dosage of 1 to 2 g per kg given over 15 minutes is the mainstay of therapy. Prompt involvement of a critical care specialist is prudent.
Adult respiratory distress syndrome (ARDS) is a rare but potentially fatal complication of the treatment of diabetic ketoacidosis. Excessive crystalloid infusion favors the development of pulmonary edema, even in the presence of normal cardiac function. Patients with an increased alveolar to arterial oxygen gradient (AaO2) and patients with pulmonary rales on physical examination may be at increased risk for ARDS. Monitoring of oxygen saturation with pulse oximetry may assist in the management of such patients.
Hyperchloremic metabolic acidosis with a normal anion gap typically persists after the resolution of ketonemia. This acidosis has no adverse clinical effects and is gradually corrected over the subsequent 24 to 48 hours by enhanced renal acid excretion. The severity of hyperchloremia can be aggravated by excessive chloride administration in hydration fluids.
NONKETONIC HYPERGLYCEMIC-HYPEROSMOLAR COMA (NKHHC OR HNC)
HNC is a syndrome characterized by impaired consciousness, sometimes accompanied by seizures, extreme dehydration, , and extreme hyperglycemia that is not accompanied by ketoacidosis.
The syndrome usually occurs in patients with type II DM, who are treated with a diet or oral hypoglycemic agents, sometimes it is a complication of previously undiagnosed or medically neglected DM (type II).
In contrast to ketoacidosis, mortality in patients with HNC has been very high (50 %) in most series. Mortality has been associated with convulsions, deep vein thrombosis, pulmonary embolus, pancreatitis and renal failure. Death is usually due to an associated severe medical condition and not to the hyperosmolality.
The pathophysiology of HNC is similar to that of ketoacidosis, except that ketoacids do not accumulate in the blood. The reason of this phenomenon is unclear. Initially it was thought that patients with HNC produced enough insulin to prevent lipolysis and ketogenesis but not enough to prevent hyperglycemia. The concept was invalidated by finding similar inappropriately low plasma insulin concentrations in patients with the two syndromes. The finding of lower plasma free fatty acids, as well as cortisol and growth-hormone concentrations, in patients with ketoacidosis has raised the possibility that the absence of ketosis may be the result of decreased cortisol and growth-hormone effects on lipolysis. Suppression of lipolysis by hyperosmolality also has been proposed.
HNC usually develops after a period of symptomatic hyperglycemia in which fluid intake is inadequate to prevent extreme dehydration from the hyperglycemia-induced osmotic diuresis.
Predisposing factors.
1. HNC seems to occur spontaneously in about 5 – 7 % of patients.
2. In 90 % of patients some degree of renal insufficiency seems to coexist.
3. Infection (e.g., pneumonia, urinary tract infection, gram-negative sepsis) is underlying frequent precipitating cause.
4. Use of certain drugs has been associated with this condition:
- steroids increase glucogenesis and antagonize the action of insulin;
- potassium-wasting diuretics (hypokalemia decreases insulin secretion), e.g., thiazides, furosemide;
- other drugs, e.g., propranolol, azathioprine, diazoxide.
5. Other medical conditions such as cerebrovascular accident, subdural hematoma, acute pancreatitis, and severe burns have been associated with HNC.
6. Use of concentrated glucose solutions, such as used in peripheral hyperalimentation or renal dialysis, has been associated with HNC.
7. HNC can be induced by peritoneal or hemodialysis, tube feeding.
8. Endocrine disorders such as acromegaly, Cushing disease, and thyrotoxicosis have also been associated with HNC.
Clinical presentation
Signs and symptoms.
1. Polyuria, polydipsia, weight loss, weakness and progressive changes in state of consciousness from mental cloudiness to coma (present in 50 % of patients) occur over a number of days to weeks.
2. Because other underlying conditions (such as cerebrovascular accident and subdural hematoma) can coexist, other causes of coma should be kept in mind, especially in the elderly.
3. Seizures occur in 5 % of patients and may be either focal or generalized.
Physical examination.
1. Severe dehydration is invariably present.
2. Various neurologic deficits (such as coma, transient hemiparesis, hyperreflexia, and generalized areflexia- absence of neurologic reflexes such as the knee jerk reaction) are commonly present. Altered states of consciousness from lethargy ( a state of being lazy, sluggish, or indifferent) to coma are observed.
3. Findings associated with coexisting medical problems (e.g., renal disease, cardiovascular disease) may be evident.
Laboratory findings.
1. Extreme hyperglycemia (blood glucose levels from 30 mmoll/l and over are common.
2. A markedly elevated serum osmolality is present, usually in excess of 350 mOsm/l. (Normal = 290 mOsm/l). The osmolality can be calculated by the following formula: mOsm/l = 2(Na + K) = blood glucose/18 + BUN/2.8.
3. The initial plasma bicarbonate averaged.
4. Serum ketones are usually not detectable, and patients are not acidic.
5. Serum sodium may be high (if severe degree of dehydration is present), normal, or high (when the marked shift of water from the intracellular to the extracellular space due to the marked hyperglycemia is present).
6. Serum potassium levels may be high (secondary to the effects of hyperosmolality as it draws potassium from the cells), normal, or low (from marked urinary losses from the osmotic diuresis). But potassium deficiency exists.
Treatment
This condition is a medical emergency and the patient should be placed in an intensive care unit.
Many of the management techniques recommended for a patient with DKA are applicable here as well.
The goals of therapy include:
- rehydration;
- reduction of hyperglycemia;
- electrolytes replacement;
- investigation of precipitating factors, treatment of complications.
Rehydration.
The average fluid deficit is 10 liters, and acute circulatory collapse is a common terminal event in HNC. The immediate aims of treatment are to rapidly expand the contracted intravascular volume in order to stabilize the blood pressure, improve the circulation, and improve the rate of urine production. It is important to remember that it is the severe hyperglycemia and the concomitant obligatory shift of water from the intracellular to the intravascular compartment that prevents this latter space from collapsing at the time of severe fluid depletion. With too rapid a correction of hyperglycemia, potential hypovolimic shock (as fluid moves from the extracellular space back into the intracellular space) may occur.
Treatment is starting by infusion 1 to 3 liters of 0,9 % sodium chloride over 1 to 2 hours; if this suffices to stabilize the blood pressure, circulation and restore good urine flow, the intravenous fluid can be changed to 0,45 % sodium chloride to provide some free water. 0,45 % sodium chloride is used at a rate of 150 to 500 ml/hour depending on the state of hydration, previous clinical response and the balance between fluid input and output. The aim of this phase of intravenous fluid therapy is not to attempt to rapidly correct the total fluid deficit or the hyperosmolality, but rather to maintain stable circulation and renal function and to progressively replenish water and sodium at rates that do not threaten or cause acute fluid overload.
Generally, half of the loss is replaced in the first 12 hours and the rest in the subsequent 24 hours.
Insulin therapy.
Insulin treatment in HNC is started by 10 to 20 unites of regular insulin intravenously as a bolus dose prior to starting the insulin infusion and then giving intravenously regular insulin in a dose of 0,05 – 0,10 unites/kg/hour (many authorities routinely use the same insulin treatment regimens as for treating DKA, other authorities recommend smaller doses of insulin, because they believe that patients with type II DM are offer very sensitive to insulin, but this view is not universally accepted, and many obese type II diabetics with NHC require larger insulin doses to induce a progressive decrease in their marked hyperglycemia. It is important to remember that because of insulin therapy causes blood glucose levels to fall, water shifts into the cells and existing hypotension and oliguria can further aggravated. Thus, initially some advocate delaying insulin therapy while infusion normal saline until vital signs have improved.
When the plasma glucose reaches the range 11 to 13 mmoll/l, 5 % glucose should be added to the intravenous fluids to avoid the risk of hypoglycemia. Following recovery the acute episode, patients are usually switched to adjusted doses of subcutaneous regular insulin at 4 to 6-hour intervals. When they are able to eat, this is changed to a 1 or 2 injection regimen.
Treatment of electrolyte disorders.
Once urine flow has been reestablished, potassium should be added to begin repletion of the total body deficits.
Potassium replacement is usually started by adding 20 mmoll/l to the initial liter of the intravenously-infused 0,45 % sodium chloride with careful serum potassium and ECG monitoring.
Contributors And acknowledgements














LACTIC ACIDOSIS (LA)
DM is one of the major causes of LA, a serious condition characterized by excessive accumulation of lactic acid and metabolic acidosis.
Pyruvic acid Lactic acid
NADH NAD
Acetoacetic Beta-hydroxybutyric
The hallmark of LA is the presence of tissue hypoxemia (reduced concentration of oxygen in blood), which leads to enhanced anaerobic glycolysis and to increased lactic acid formation.
Pyruvic acid is converted into lactic acid by lactic dehydrogenase (LDH) in the presence of reduced nicotinamide adenine dinucleotide (NADH), which, in turn, is converted into NAD. The reaction is reversible and involves LDH in both directions. The conversion of acetoacetic acid into beta-hydroxybutyric acid also requires the oxidation of NADH. LA results from decreased availability of NAD caused by lack of oxygen. Likewise, the deficiency of NAD impairs the conversion of beta-hydroxybutyric into acetoacetic acid. Thus, LA predisposes to accumulation of beta-hydroxybutyric acid, which does not react with acetest tablet, so, the reaction for ketone bodies may be negative or slightly positive. The normal blood lactic acid concentration is 1mmol/l, and the pyruvic to lactic ratio is 10:1. An increase in lactic acid without concomitant rise in pyruvate leads to LA of clinical importance.
Predisposing factors
1. Heart and pulmonary failure (which leads to hypoxia).
2. Usage of biguanids, pheformin therapy.
3. Alcohol intoxication.
4. Ketoacidosis (it is important to have a very high index of suspection with respect to presence of LA).
Clinical presentation
Signs and symptoms.
1. Kussmaul breathing (deep, sighing respiration) is present as respiratory compensation for the metabolic acidosis and is obvious when the pH is less than 7.2.
2. Symptoms of central-nervous-system involvement include headaches, drowsiness, lassitude (weariness of body or mind from strain, oppression climate; exhaustion, lethargy etc).
3. Anorexia, nausea, vomiting, and abdominal pain may be present.
4. Myalgia (Muscle pain) is common.
Physical examination.
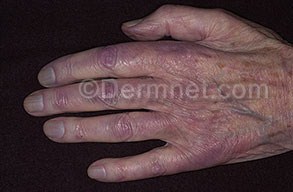
1. Acrocyanosis (perisistent blue or cyanotic discoloration of the digits, ost commonly seen in the hands, although also occurring in the face and feet as well) is common.
2. Tachycardia frequently is present, blood pressure is decreased.
3. Poor skin tugor and dry skin may be prominent.
4. Hypothermia (when the normal body temperature for body metabolism is dropped, usually to 35 degrees Celsius) is common in LA.
5. Hyperpnea (increased depth of breathing when required to meet demand, as during or following exercise or when the body lacks oxygen- hypoxia) or Kussmaul respiration is present and related to degree of acidosis.
4. Findings associated with coexisting medical problems (e.g., renal disease, cardiovascular disease) may be evident.
Laboratory findings
1. Blood glucose level is not high
2. Glucosurea (Glucose in Urine) is absent.
3. Blood lactic acid is high.
Treatment
LA is treated by correcting the underlying cause.
In severe cases, bicarbonate therapy should be used (intravenously-infused 2,5 % sodium bicarbonates 1 to 2 l/day).
LA can be treated with low dose insulin regimens with 5 % glucose solution infusion.
Volume expanders and oxygen therapy are helpful treatment as well.
Comparison of DCA, HNC and LA.
DKA
1. Age: Below 40 years
2. Type of DM: Type I
3. Predisposing factor: Insulin Deficiency
4. prodromes: Several days duration or less than 1 day
5. Underlying renal, Cardiovascular or Pulmonary disease: About 15%
6. General: More acidic and less dehydrated, hyperventilation
7. Neurologic symptoms and signs: rare
8. Laboratory findings: blood glucose- High (about 20-30 mmol/l)
9. Plasma Ketones: +
10. Serum bicarbonate: Low
11. Blood pH: Less than 7.35
12. Serum Osmolality: less than 330 mOsm?l
13. free fatty acids: elevated
14. serum sodium: Normal, elevated or low
15. Serum Potassium: Noraml, elevated or low
16. Complications-thrombosis: rare
17. Mortality rate: 1-10%
18. Diabetes treatment after recovery: Always Insulin
HNC
1. Age: Above 40
2. Type of DM: Type II
3. Predisposing factor: Dehydration
4. Prodromes: several days duration
5. Underlying renal, Cardiovascular or pulmonary diseases: 85%
6. General: More hydrated and less acidic, no hyperventilation
7. Neurologic symptoms: very common
8. Laboratory findings- blood glucose: very high (about 40-50 mmol/l)
9. Plasma Ketones: -
10. Serum sodium: Normal, elevated or low
11. Serum Potassium: Normal, elevated or low
12. Serum bicarbonate: Normal
13. Blood pH: Normal
14. Serum Osmolality: over 350 mOsm/l
15. free fatty acids: decreased or normal
16. complications (thrombosis): frequent
17. Mortality rate: 20-50%
18. Diabetes treatment after recovery: Diet alone or Oral agents and sometimes insulin.
LA
1. Age: Above 40
2. Type of DM: Type II
3. Predisposing factor: Hypoxia
4. Prodromes: Less than 1 day
5. Underlying renal, Cardiovascular or Pulmonary diseases: About 90%
6. General: More acidic and less dehydrated, hyperventilation
7. Neurologic symptoms and signs: Very common
8. Laboratory findings-blood glucose: Normal or about 10-11 mmol/l
9. Plasma ketones: -
10. Serum Sodium: Normal
11. Serum Potassium: Normal
12. Serum Bicarbonate: Low
13. Blood pH: Less than 7.35
14. Serum Osmolality: Normal
15. free fatty acids: Normal
16. Complications (thrombosis): very rare
17. Mortality rate: About 90%
18. Diabetes treatment: Diet alone or oral agents, sometimes insulin.
HYPOGLYCEMIA
It is a syndrome characterized by symptoms of sympathetic nervous system stimulation or central nervous system dysfunction that are provoked by an abnormally low plasma glucose level.
Hypoglycemia represents insulin excess and it can occur at any time.
Precipitating factors
- irregular ingestion of food;
- extreme activity;
- alcohol ingestion;
- drug interaction;
- liver or renal disease;
- hypopituitarism and adrenal insufficiency.
Clinical presentation
Signs and symptoms.
Two distinct patterns are distinguished:
1) adrenergic symptoms (they are attributed to increased sympathetic activity and epinephrine release): sweating, nervousness, tremulousness, faintness, palpitation, and sometimes hunger;
2) cerebral nervous system manifestations: confusion, inappropriate behavior (which can be mistaken for inebriation); visual disturbances, stupor, coma or seizures. (Improvement in the cerebral nervous system manifestations will be with a rise in blood glucose.)
A common symptom of hypoglycemia is the early morning headache, which is usually present when the patient awakes.
Patients should be familiar with the symptoms of the hypoglycemia but some of them are not heralded by symptoms.
Physical examination.
1. The skin is cold, moist.
2. Hyperreflexia can be elicited.
3. Hypoglycemic coma is commonly associated with abnormally low body temperature
4. Patient may be unconsciousness.
Laboratory findings
1. Low level of blood glucose
Treatment
Insulin–treated patients are advised to carry sugar lumps, candy, or glucose tablets at all time.
If the symptoms of hypoglycemia develop, the patients have to drink a glass of fruit juice or water with 3 tbsp. of table sugar added or to eat candy, and to teach their family members to give such treatment if they suddenly exhibit confusion or inappropriate behavior:
1) Glucagons 0,5 – 1 unit (0,5 – 1 ml) s/c, i/m or i/v. If the patient does not respond to 1 unit of glucagon within 25 minutes, further injections are unlikely to be effective, and are not recommended;
2) an i/v injection of 20 or 100 ml of 40 % glucose, followed by a continuous infusion of 5 % glucose (10 % glucose may be needed) until it clearly can be stopped safely;
3) glucocorticoids and adrenaline are helpful as well.
You can check out my previous hub on Diabetes mellitus here