Is There a Cure for HIV and AIDS?
Finding the Cure to HIV
Acquired Immunodeficiency Syndrome, a disease characterized by a weakened immune system, was first officially recognized in 1981 when five men in Los Angeles were found to have Pneumocystis pneumonia – a type of pneumonia caused by clusters of a yeast-like fungus called Pneumocystis jirovecii. Since then, scientists have set out to erase it, but with no success, they settled on finding treatments and learning how to prevent it from spreading. While new treatments and methods of prevention are, of course, beneficial ways to help the growing population of people with AIDS, it has not made a significant impact in eradicating the disease. Millions of people still suffer from AIDS and thousands of people catch the disease each year. The only solution can be found in a cure. (For more information about treatment options, see my other article.)
And so, scientists are for a cure, but nothing has been successful in curing HIV/AIDS until recently. A man, who has been dubbed the “berlin patient”, has been officially declared cured of HIV. Suffering from both AIDS and Leukemia, Timothy Ray Brown, was offered a drastic suggestion by his doctor. He was to undergo a bone marrow transplant. Transplants of this sort are often used to treat Leukemia, but Mr. Brown was to receive a special type of transplant from a special donor that would hopefully treat his HIV as well. His donor had what is referred to as CCR5 – Delta 32. It is a deletion mutation of the CCR5 gene. The deletion of that portion of the gene actually has a negative effect on T cells that function as part of the immune system. However, it also has a positive effect: it provides protection against HIV.
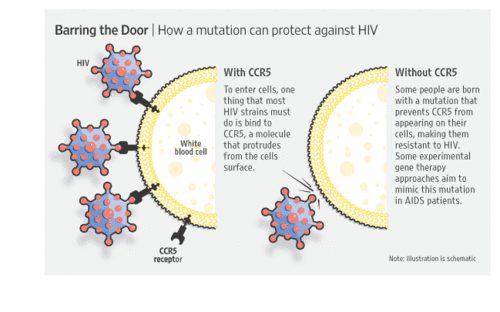
The CCR5 gene codes for a CCR5 protein that serves as a receptor on T cells. HIV uses the CCR5 receptor to enter into the cells. While CCR5 has a deletion mutation of the 32 segment, the receptor does not function. This prohibits HIV from using that receptor to enter the cell. Thus, it prevents HIV from replicating and destroying T cells. In essence, it provides immunity against HIV.
CCR5 – Delta 32 is found in around 10% of people from Northern Europe, and also in people from Northern European descent, but is almost nonexistent in people from other countries around the world. Scientists believe that the Delta 32 mutation might have been perpetuated by natural selection during the reign of Smallpox. The Delta 32 mutation also protects against Smallpox.
With the bone marrow transplant of stem cells containing CCR5 - Delta 32, Mr. Brown also developed resistance to HIV. The donor’s cells reproduced inside of Mr. Brown, replacing his cells with cells that were resistant to HIV. He has now been declared cured and three years later remains unaffected. And while most people and scientists accept the fact that providing bone marrow transplants with the rare CCR5 – Delta 32 mutation to the 35 million people with HIV is not plausible, there is one common thought: HIV can be cured.
Bone marrow transplants are costly, they required specific donors for specific people, and are extremely dangerous; as a mismatched transplant can result in death as the body will reject it. However, scientists are harnessing the information provided by the CCR5 – Delta 32 mutation and using it in gene therapy. Their ultimate goal is to make CD4+ T cells resistant to HIV. Through gene therapy, scientists have been able to extract CD4+ cells, delete segment 32, and reinsert the cells back into the patients where they replicate. A recent study done earlier this year showed that these genetically modified cells lasted for several months inside the body. Therefore, modified CD4+ cells, through the process of natural selection, will overtake and outlive normal, unmodified CD4+ cells when presented with HIV. The virus will kill off the unmodified version, leaving only the resistant cells behind.
Along with this group of people who resist HIV comes another group just as special. These people, known as “elite controllers”, become infected by HIV, but keep the virus in check, never allowing it to progress to AIDS. They may live their whole lives and never know they even have HIV. Some, however, may develop AIDS eventually, but the progression of HIV into AIDS is extremely slower than non-controllers because their immune system is more effective at battling it. After many tests, these controllers were found to have something in common. There were single nucleotide polymorphisms, or SNPs, in over 300 base pairs on chromosome 6 in the region that coded for a protein called human leukocyte antigen, or HLA. This HLA protein is a vehicle that, when a person is infected with HIV, attaches itself to the viral peptide. It then carries the virus to the surface to signal the immune system that it has found an infection. The body’s Killer T cells them come and destroy the infected cell and B cells begin to make antibodies against those peptides. The difference between the controllers and the rest of the human population is in the amino acid makeup of the HLAs. Controllers have been found to have three different amino acids that change the “binding pockets” of their HLAs. The binding pocket is the location where the HLA protein attaches to the viral peptide. This difference allows the HLA to attach to other kinds of binding pockets, and their HLAs will even recognize and attach to mutant forms of HIV. In addition, Killer T cells are trained, in their creation process, to recognize certain types of peptides. The more peptides they are presented to during the training process, the more specific their range is. In order words, the Killer T cell will only recognize a few specific peptides. Likewise, if the Killer T cell is only presented with a few peptides in training, its scope will be broader and more general. This is both good and bad. Killer T cells are trained to recognize foreign, dangerous cells. If the T cell’s range is broad, it might erroneously target the body’s good cells and destroy them. For that reason, the body naturally makes the T cell’s range more specific. However, in the case of HIV, it is good for the T cell’s range to be more general because this allows them to target all forms of HIV, even the mutant forms. In this way, elite controllers are able to mount an attack on HIV as soon as they are affected. Non-controllers do not begin to form resistances until it is too late and HIV is able to over take their T cells.
This recent information has changed scientists reasoning when it comes to HIV. Most had usually said that looking for a cure was irresponsible and a waste of time. Some still consider that to be true, but the opinion has changed for the most part. Finding a cure is the better solution, and is now even seen to be possible. Treatments are getting better and better, but are too costly and still leave millions of people affected with HIV, while millions more join the group each year. Scientists hope that by using this new information about gene mutations that cause resistance to HIV, they may be able to find a vaccine or cure, in this way, and only in this way, will they be able to actually end the pandemic.
*If you live in Albuquerque, New Mexico and need help with STD testing or treatment*